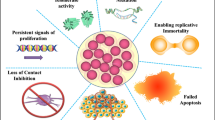
Abstract
Ginsenosides, the main components isolated from Panax ginseng, can play a therapeutic role by inducing tumor cell apoptosis and reducing proliferation, invasion, metastasis; by enhancing immune regulation; and by reversing tumor cell multidrug resistance. However, clinical applications have been limited because of ginsenosides’ physical and chemical properties such as low solubility and poor stability, as well as their short half-life, easy elimination, degradation, and other pharmacokinetic properties in vivo. In recent years, develo** a ginsenoside delivery system for bifunctional drugs or carriers has attracted much attention from researchers. To create a precise treatment strategy for cancer, a variety of nano delivery systems and preparation technologies based on ginsenosides have been conducted (e.g., polymer nanoparticles [NPs], liposomes, micelles, microemulsions, protein NPs, metals and inorganic NPs, biomimetic NPs). It is desirable to design a targeted delivery system to achieve antitumor efficacy that can not only cross various barriers but also can enhance immune regulation, eventually converting to a clinical application. Therefore, this review focused on the latest research about delivery systems encapsulated or modified with ginsenosides, and unification of medicines and excipients based on ginsenosides for improving drug bioavailability and targeting ability. In addition, challenges and new treatment methods were discussed to support the development of these new tumor therapeutic agents for use in clinical treatment.

Similar content being viewed by others
Introduction
Drug delivery systems (DDSs) for cancer treatment, which have been explored for many years, have been developed rapidly for their solubility, bioavailability, and targeting with their high drugloading rates, large specific surface areas and diverse surface functions [1,2,3]. However, further work has been hindered by low drug-loading rates, drug resistance, toxicity and immune responses induced by nanocarriers [4, 5]. Because most DDSs acted only as excipients with no direct effects, short and long-term toxicity can appear with their metabolites.
In addition, therapeutic effects can be reduced for the phagocytosis and clearance of nanoparticles (NPs) by the reticuloendothelial system (RES). Furthermore, DDSs can interact with cell surface-specific receptors resulting in adverse immune reactions. Nevertheless, natural products such as ginsenosides have been studied widely for the treatment of cancer and other diseases because of their chemical and biological properties including chemical diversity, specificity, and low toxicity, making them conducive to the development of DDSs [6].
Ginsenosides are a group of bioactive compounds extracted from Panax ginseng [7] (Fig. 1). As small-molecule substances, ginsenosides can resist diabetes, depression and cancer, offering better protective effects for cerebral ischemia, endothelial cell injury, and cardiovascular disease (CVD) [8,9,10,11]. Currently, ginsenoside Rg3 has been launched as a new drug in traditional Chinese medicine (TCM, Shenyi capsule) for the treatment of lung, breast, gastrointestinal (GI) cancers [12]. Researches have reported that the human body can develop resistance after multiple administrations of cancer therapy. Ginsenosides combined with cisplatin [13], adriamycin [14], vincristine [15] or other chemotherapy drugs can reverse multidrug resistance and improve the antitumor effects for lung and liver cancers. Ginsenosides have been proved to exhibit good anticancer activity and targeting ability, both as a drug and as an excipient compound simultaneously [190,191,192]. These NPs are usually sensitive to tiny changes related to tumor cells and TME (e.g., pH, redox state, enzymes) to release drugs, which also can be activated by external stimuli (e.g., light, heat, magnetic field, ultrasound) [193]. According to TME characteristics, conditionally sensitive NPs can achieve controlled drug release, only releasing drugs at tumor sites and stabilizing themselves under certain physiological conditions. pH-sensitive NPs (Rg3-loaded mPEG-b-P (Glu-co-Phe)) achieved CRC tumor targeting and Ph-stimulated drug release, as well as a longer circulation time in the blood, resulting in an increased tumor therapy and decreased side effects to other tissues or organs [88].
In addition, targeting NPs and microenvironment-sensitive NPs can reduce the toxicity and side-effects of ginsenoside nanomedicines. Hypoxia around the tumor tissue is caused by the lack of blood flowing through that tissue resulting from the exuberant metabolism [194]. Hypoxia-sensitive NPs can be designed to know the difference between the hypoxia environment of tumor tissue and the normoxic environment of healthy tissue. For example, although ~ 150-nm NPs exhibited good serum stability and passive tumor targeting, their weak tissue permeability can limit drug efficacy. In contrast, reducing particle size can increase tissue permeability while also reducing the stability of NPs in the blood circulation. Therefore, Designing NPs to achieve superior serum stability and permeability simultaneously is necessary.
A strategy based on the dissociation of tumor site NPs is worth pondering, which can not only increase the stability of NPs in the blood but also can enhance the tissue permeability [195]. Importantly, a human serum albumin anticancer drug modified by a hypoxia-sensitive azobenzene group has been fabricated, with a particle size of 100–150 nm. After reaching the tumor site, the azobenzene NPs groups disintegrated the NPs to < 10 nm, enhancing the role of tumor permeability and the curative effect.
Codelivery strategy
Combination drug therapy has synergistic therapeutic effects as compared with single chemotherapy drugs. Although it is common for multiple drugs to be applied for various diseases in the clinic, differences in physicochemical properties and pharmacokinetics may cause the drugs to fail to reach the same site at the same time, thus not achieving the optimum synergy. Therefore, it is necessary to determine the optimal ratio of drugs, which is complicated to investigate in vivo. Drug codelivery strategy provides a new possibility for the treatment of drug resistance in tumor cells.
Currently, codelivery systems including liposomes, micelles, and inorganic NPs with same pharmacokinetics have overcome multiple drug resistance, providing a new possibility for the treatment of this resistance in tumor cells. Synergistic anticancer effects produced by codelivery are of significance for DDSs..
Liposomes embedded with ginsenoside and other drugs such as curcumin, PTX, and betulinic acid can significantly inhibit tumor growth [19]. Liposomes containing parthenolide, betulinic acid, honokiol and ginsenoside Rh2 have been found to be safer than cisplatin for the treatment of tumors [98]. In addition, it has been reported that ginsenosides, as chemotherapy adjuvant and membrane stabilizer combined with PTX, could inhibit the proliferation of gastric cancer cells and reduce side-effects, thus further improving the therapeutic effect for gastric cancer. The silanol hydroxyl group on the surface and adjustable pore size of MS are beneficial to the combination of ginsenoside CK and Rh2, which exerted excellent biocompatibility with normal hacaT skin cells and anticancer effect on HepG2, A549 and HT-29 colon cancer cells [111]. Furthermore, combination therapies have displayed potential applications for reducing side-effects and metastasis and for overcoming drug resistance. Multicomponent MEs consisting of etoposide, coix seed oil and ginsenoside Rh2 have been utilized to regulate a variety of signaling pathways to overcome drug resistance by inhibiting P-gp. Furthermore, Rh2 can relieve the inflammatory response and immune suppression caused by etoposide [122]. Thus, combination therapies of ginsenosides to overcome drug resistance and metastasis require further research.
Photodynamic and photothermal therapy enhancement
Much attention has been focused on PDT and PTT because of their advantages of being a noninvasive, precise treatment with strong specificity and high tumor destruction efficiency [196,197,215].
For example, fluorescent signal probes including NIR fluorescent dye ICG [216], up-conversion nanomaterials NaYF4: Yb/Er/Tm [217], GNP clusters (AuNCs) with a particle size of < 2 nm [218], and quantum dots recently have been designed for cancer imaging and therapy due to their biocompatibility and low toxicity [219]. In addition, NPs with iron, manganese, or gadolinium ions or iron oxide NPs for MRI imaging have been applied clinically [220]. Furthermore, acoustic waves from the contrast agents for photoacoustic imaging have been shown to be much safer than those of CT or PET [221]. More complex multimodal imaging for diagnosis and designing a treatment platform are needed. Therefore, the development of ginsenosides based on an integrated imaging and therapy delivery system must be explored further.
Multifunction as nanocarriers
Ginsenosides, as nanocarriers, have also shown multiple pharmacological functions, which are shown in Fig. 14 including antitumor effect improvement, side-effect attenuation, self-targeting delivery, biomimetic delivery, and immunomodulation.
Antitumor effect improvement and attenuation of side-effects
Most drug delivery carriers’ act only as excipients with no direct effects on the main drugs; however, short- or long-term toxicity may appear with their metabolites [108]. Ginsenosides have a potential application for being both adjuvant drugs and excipients simultaneously.
liposomes have been utilized to replace cholesterol for stabilizing the phospholipid bilayer. The liposome preparation formulations were simple without adding PEG or targeting ligand, which greatly simplified the technological production. Liposomes exerted a significant synergistic anticancer pharmacological activity with the chemotherapeutic drug PXT by targeting the GLUT on the surface of tumors [25,26,27].
Self-targeting delivery
Rh2, Rg3, and Rg5 ginsenoside liposomes can be accumulated in tumors for recognizing the GLUT receptor on the tumor cell membrane with stronger toxicities and targeting abilities. The curative effects of Rg5-PTX-liposomes have been confirmed with HGC-27, A549, and MCF-7 subcutaneous tumor models [27]. In addition, PTX-Rh2-lipo achieved excellent tumor targeting and anti-tumor activity of mouse breast cancer [25]. Rg3-PTX-liposomes inhibited tumor proliferation by activating the C6 glioma immune microenvironment via inducing the transformation of M2 TAMs into M1 in the TME [28].
Biomimetic delivery
The adsorption of opsonin proteins such as Ig and other complex proteins can enable NPs to be recognized and cleared easily by the mononuclear phagocytes. It has been demonstrated that the inhibited uptake of phagocytes by reducing the adsorption of these proteins can enhance the stealth effect of NPs [222].
PEGylated NPs can form steric hindrance on their surface through their hydrophilicity and spatial repulsion, thus decreasing protein adsorption and avoiding being removed by the monocyte phagocytic system [223]. Nevertheless, the increased blood circulation cycle of ginsenoside-embedded liposomes is achieved because Rh2, Rg3 and Rg5 can prevent the activation of the monocyte phagocytic system. It has been verified that the amount of Rh2 liposomes coated by protein corona was significantly lower than that of traditional liposomes [25]. The long circulating liposome fabricated with ginsenosides can reduce the adsorption of opsonins on their surface, thus exhibiting the stealth effect of ginsenoside and increasing the adsorption of apolipoprotein E, which can retard the absorption of macrophages to liposomes.
Immunomodulation
TME gradually has become the target of tumor treatment due to its important role in tumor development, diffusion, metastasis, and drug resistance. As compared to targeted tumor cells, one benefit of targeting nontumor cells in TME is that they are genetically more stable and, therefore, are less likely to form drug resistance. However, the difficulty of targeting nontumor cells to obtain good therapeutic effects involves reducing the toxicity to normal cells. Interfering with the TME of primary tumor cells or the premetastatic microenvironment of tumor cells can be effective for the treatment of malignant tumors prone to metastasis [224, 225].
The immunotherapeutic activities of ginsenoside liposomes have been reflected in improving the TME structure to enhance the drug permeability by reducing tumor vascular density. Some researchers have focused on transporting drugs to blood vessels with Rh2, Rh3 or Rg5 liposomes, which is important for tumor growth and metastasis [25, 26, 28]. Targeted stromal cells including cancer-associated fibroblasts and TAMs also have been utilized for cancer treatment [174]. Ginsenosides liposomes changed the immune-deficiency TME mainly through reducing the heterogeneous cells in the TME and enhancing the immune function by increasing the infiltration of CD8+ T cells. As a targeted stromal cells, TAMs easily differentiate into M2 phenotypes, which often have been associated with tumor metastasis and poor outcomes. Ginsenoside liposomes have played a role in reconstructing the TME by transforming TAM2 into TAM1 to promote the role of T cells by inhibiting the activities of signal transducers and transcription activators [25].
Multifunction as both drug and nanocarrier
Ginsenosides as a drug are commonly encapsulated into the core of NPs or modified on their surface. Ginsenoside Rg3, Rg5, and Rh2 have acted as carriers of nano lipid structures, substituting cholesterol for the similar structure. Therefore, ginsenoside DDSs not only can exhibit their multifunctionality as a drug but also can display their merits as carriers.
It has been verified that ginsenoside nanomedicines can increase anticancer efficacy and can exhibit synergistic anticancer effects with other chemotherapy drugs while decreasing the side-effects caused by these drugs, NPs, or cholesterol. In addition, the ligand-targeting ability of ginsenoside DDS for specific sites or their self-targeting ability for recognizing the GLUT receptor on the tumor cell membrane enable ginsenosides to be potential delivery systems. Furthermore, ginsenosides themselves are endowed with the delivery system’s stealth effect for the inhibition of the uptake of phagocytes and immune function by increasing the infiltration of CD8+ T cells and reconstructing the TME, strengthening tumor treatment.
Clinical application and translation
Ginsenoside nanomedicines have shown great application value and development prospects. Certain tumor therapeutic nanomedicines are in clinical trials, such as a G-PTX liposome loaded with ginsenoside and PTX, and have exhibited advantages for drug loading, tumor targeting, stability, and biological safety [27]. However, much remains to be explored before these therapies are truly mature. Several challenges must be solved before applying ginsenoside DDSs in clinical practice [226,227,228], including the synthesis and large-scale production of controllable and repeatable nanodrugs, the development of a safety evaluation, and the undertaking of clinical research.
Nanodrug synthesis and large-scale production
Repeatable synthesis methods and controllable quality are prerequisites for drug clinical transformation. Some multifunctional nanodrugs (e.g., layer-by-layer, self-assembly NPs) involve multiple or complex synthesis steps. Therefore, it is difficult to synthesize nanodrugs with the same qualities quickly, accurately and repeatedly. Microfluidic technology might help solve the problem of inconsistent effects from laboratory research to clinical experiments given its high-speed self-assembly, narrow size distribution, and good repeatability [229].
In addition, monodisperse NPs with highly controllable size, shape, chemical composition, surface properties, and drug loading capacity can be synthesized using a nonwetting template complex method [230]. To carry out a comprehensive quality control for nanodrugs and carrier materials, more research on their formulation technology and stability are necessary. Furthermore, corresponding quality control methods must be established, optimized, and verified. The research and development of a GMP-compliant preparation process and equipment for the large-scale production of nanodrugs will be required.
Safety evaluation and clinical research
As compared with traditional small-molecule or biological macromolecular drugs, ginsenoside nanodrugs are different in their variety and physical and chemical properties. Hence, to achieve a clinical transformation, we must focus on evaluating the biocompatibility and safety of NPs in vivo. Safety assessment first requires the completion of high-throughput cytotoxicity testing, including for oxidative stress, surface membrane, and mitochondrial damage, lysosomes, autophagy, and inflammatory corpuscles. Animal models with different species are needed to study the pharmacokinetics, biodistribution, efficacy, and safety of nanomedicines [226]. It will be necessary to carry out preclinical studies on ADME, toxicokinetics, acute toxicity, immunology, and drug-specific toxicity of drugs in vivo, as well as to design standard operating procedures for safety evaluation method.
Certain correlations and differences exist between the toxicological results of experimental animals and the adverse reactions of the human body. Although animal models are commonly used to evaluate safety, the safety responses of animals and humans are different and can be affected by many factors, such as the differences of cytochrome P450 and enzymes. There also are differences among the animal models themselves. For example, the rat model is more sensitive than is the mouse model for predicting the GI toxicity of chemotherapy and targeted therapy. Some models, such as the genetically engineered and patient-derived xenotransplantation mouse model, can accurately simulate the heterogeneity of human tumors [231, 232].
Another challenge is clinical trials. After the completion of a preclinical safety assessment, it will be necessary to evaluate and manage patient side-effects and adverse events to evaluate toxicity in the human body, so as to facilitate the successful clinical transformation of the drugs.
Conclusion and prospects
The ideal DDS maintains a drug concentration in a certain range or specifically delivers a drug to target organs and tissues after a single administration while minimizing the drug’s concentration in other regions and reducing the immune response in vivo. Ginsenosides have been an important component of cancer drugs for a long time. The research on and development of ginsenoside DDSs have provided a certain prospect for tumor treatment, but the antitumor mechanisms of some nanodrugs require further research. Only with a reasonable research strategy, comprehensive preclinical evaluation and strict clinical trials can more antitumor drugs be developed.
The antitumor effects of a ginsenoside DDS for lung, colon, and liver cancer cells, as well as the inhibitory effects on tumor xenografts in mice, have been investigated. Although the nano-delivery systems can increase drug concentration in the blood, only a few studies have explored in depth the distribution of ginsenosides or their metabolites in tumor tissues or organs. The research on ginsenoside DDSs is still in the preclinical stage, and no DDS has been launched successfully. Although NPs have achieved progress, the clinical transformation of nanodrugs for cancer treatment remains a focus.
To simulate the real clinical environment as much as possible, it is necessary to further explore the mechanism and pharmacokinetics of a ginsenoside DDS in vivo to inhibit cancer metastasis and to combine chemical sensitizers to eliminate the resistance of the body to ginsenosides. Furthermore, the therapeutic effects can be maintained by a combination of ginsenosides and classical chemotherapy drugs, the dosage of which can be reduced. Although still in the early stages of research and development, a multifunctional DDS for diagnosis, treatment, and prognosis will require evaluating its efficacy in vivo, which is worthwhile research. The development and improvement of new dosage forms show a great potential in cancer treatment.
Availability of data and materials
Not applicable.
References
Song X, Liu C, Wang N, Huang H, He S, Gong C, et al. Delivery of CRISPR/Cas systems for cancer gene therapy and immunotherapy. Adv Drug Deliv Rev. 2021;168:158–80.
He L, Qin X, Fan D, Feng C, Wang Q, Fang J. Dual-stimuli responsive polymeric micelles for the effective treatment of rheumatoid arthritis. ACS Appl Mater Interfaces. 2021;13(18):21076–86.
Javed R, Zia M, Naz S, Aisida SO, Ul Ain N, Ao Q. Role of cap** agents in the application of nanoparticles in biomedicine and environmental remediation: recent trends and future prospects. J Nanobiotechnol. 2020;18:172.
Duncan R. Polymer conjugates as anticancer nanomedicines. Nat Rev Cancer. 2006;6(9):688–701.
Zolnik BS, Gonzalez-Fernandez A, Sadrieh N, Dobrovolskaia MA. Minireview: Nanoparticles and the Immune System. Endocrinology. 2010;151(2):458–65.
Patra JK, Das G, Fraceto LF, Campos EVR, Rodriguez-Torres MDP, Acosta-Torres LS, et al. Nano based drug delivery systems: recent developments and future prospects. J Nanobiotechnol. 2018;16:17.
Guo M, Shao S, Wang D, Zhao D, Wang M. Recent progress in polysaccharides from Panax ginseng C. A Meyer Food Funct. 2021;12(2):494–518.
Shibata S. Chemistry and cancer preventing activities of ginseng saponins and some related triterpenoid compounds. J Korean Med Sci. 2001;16:S28–37.
Yang FF, Zhou J, Hu X, Yu SK, Liu CY, Pan RL, et al. Preparation and evaluation of self-microemulsions for improved bioavailability of ginsenoside-Rh1 and Rh2. Drug Deliv Transl Res. 2017;7(5):731–7.
Zhang EY, Shi HL, Yang L, Wu XJ, Wang ZT. Ginsenoside Rd regulates the Akt/mTOR/p70S6K signaling cascade and suppresses angiogenesis and breast tumor growth. Oncol Rep. 2017;38(1):359–67.
Paek IP, Moon Y, Kim J, Ji HY, Kim SA, Sohn DH, et al. Pharmacokinetics of a ginseng saponin metabolite compound K in rats. Biopharm Drug Dispos. 2006;27(1):39–45.
Pan LL, Zhang TT, Sun HY, Liu GR. Ginsenoside Rg3 (Shenyi Capsule) combined with chemotherapy for digestive system cancer in china: a meta-analysis and systematic review. Evid-based Complement Altern Med. 2019;2019:2417418.
** L, Xu M, Luo XH, Zhu XF. Stephania Tetrandra and Ginseng-containing chinese herbal formulation NSENL reverses cisplatin resistance in lung cancer xenografts. Am J Chin Med. 2017;45(2):385–401.
Zhang JW, Zhou F, Wu XL, Zhang XX, Chen YC, Zha BS, et al. Cellular pharmacokinetic mechanisms of adriamycin resistance and its modulation by 20 (S)-ginsenoside Rh2 in MCF-7/Adr cells. Br J Pharmacol. 2012;165(1):120–34.
Park JD, Rhee DK, Lee YH. Biological Activities and Chemistry of Saponins from Panax ginseng C. A Meyer Phytochem Rev. 2005;4(2–3):159–75.
Chen JX, Peng HM, ** OY, He XY. Research on the antitumor effect of ginsenoside Rg3 in B16 melanoma cells. Melanoma Res. 2008;18(5):322–9.
Gu Y, Wang GJ, Sun JG, Jia YW, Wang W, Xu MJ, et al. Pharmacokinetic characterization of ginsenoside Rh2, an anticancer nutrient from ginseng, in rats and dogs. Food Chem Toxicol. 2009;47(9):2257–68.
He BC, Gao JL, Luo XJ, Luo JY, Shen JK, Wang LY, et al. Ginsenoside Rg3 inhibits colorectal tumor growth through the down-regulation of Wnt/beta-catenin signaling. Int J Oncol. 2011;38(2):437–45.
Vijayakumar A, Baskaran R, Maeng HJ, Yoo BK. Ginsenoside improves physicochemical properties and bioavailability of curcumin-loaded nanostructured lipid carrier. Arch Pharm Res. 2017;40(7):864–74.
Selvaraj K, Yoo BK. Curcumin-loaded nanostructured lipid carrier modified with partially hydrolyzed ginsenoside. AAPS PharmSciTech. 2019;20:252.
Tao C, Zhang JJ, Wang JX, Le Y. Ginsenoside drug nanocomposites prepared by the aerosol solvent extraction system for enhancing drug solubility and stability. Pharmaceutics. 2018;10(3):95.
Zhang W, Wang XY, Zhang M, Xu M, Tang WY, Zhang Y, et al. Intranasal delivery of microspheres loaded with 20 (R)-ginsenoside Rg3 enhances anti-fatigue effect in mice. Curr Drug Deliv. 2017;14(6):867–74.
Kim H, Lee JH, Kim JE, Kim YS, Ryu CH, Lee HJ, et al. Micro-/nano-sized delivery systems of ginsenosides for improved systemic bioavailability. J Ginseng Res. 2018;42(3):361–9.
Lu JM, Yao QZ, Chen CY. Ginseng compounds: an update on their molecular mechanisms and medical applications. Curr Vasc Pharmacol. 2009;7(3):293–302.
Hong C, Liang JM, **a JX, Zhu Y, Guo YZ, Wang AN, et al. One stone four birds: a novel liposomal delivery system multi-functionalized with ginsenoside Rh2 for tumor targeting therapy. Nano-Micro Lett. 2020;12:129.
Hong C, Wang D, Liang JM, Guo YZ, Zhu Y, **a JX, et al. Novel ginsenoside-based multifunctional liposomal delivery system for combination therapy of gastric cancer. Theranostics. 2019;9(15):4437–49.
Wang X, Zheng WW, Shen Q, Wang YH, Tseng YJ, Luo ZG, et al. Identification and construction of a novel biomimetic delivery system of paclitaxel and its targeting therapy for cancer. Signal Transduct Tar. 2021;6:33.
Zhu Y, Liang JM, Gao CF, Wang AN, **a JX, Hong C, et al. Multifunctional ginsenoside Rg3-based liposomes for glioma targeting therapy. J Control Release. 2021;330:641–57.
Nag SA, Qin JJ, Wang W, Wang MH, Wang H, Zhang RW. Ginsenosides as anticancer agents: in vitro and in vivo activities, structure-activity relationships, and molecular mechanisms of action. Front Pharmacol. 2012;3:25.
Hasegawa H, Sung JH, Matsumiya S, Uchiyama M. Main Ginseng saponin metabolites formed by intestinal bacteria. Planta Med. 1996;62(5):453–7.
Tang W, Zhang Y, Gao J, Ding X, Gao S. The Anti-fatigue Effect of 20 (R)-Ginsenoside Rg3 in Mice by Intranasally Administration. Biol Pharm Bull. 2008;31(11):2024–7.
Hurh J, Markus J, Kim YJ, Ahn S, Castro-Aceituno V, Mathiyalagan R, et al. Facile reduction and stabilization of ginsenoside-functionalized gold nanoparticles: optimization, characterization, and in vitro cytotoxicity studies. J Nanopart Res. 2017;19(9):313.
Jeon JH, Lee J, Choi MK, Song IS. Pharmacokinetics of ginsenosides following repeated oral administration of red ginseng extract significantly differ between species of experimental animals. Arch Pharm Res. 2020;43(12):1335–46.
Piao XM, Zhang H, Kang JP, Yang DU, Li YL, Pang SF, et al. Advances in Saponin Diversity ofPanax ginseng. Molecules. 2020;25(15):3452.
Xu QF, Fang XL, Chen DF. Pharmacokinetics and bioavailability of ginsenoside Rb-1 and Rg (1) from Panax notoginseng in rats. J Ethnopharmacol. 2003;84(2–3):187–92.
**e HT, Wang GJ, Sun JG, Tucker I, Zhao XC, **e YY, et al. High performance liquid chromatographic-mass spectrometric determination of ginsenoside Rg3 and its metabolites in rat plasma using solid-phase extraction for pharmacokinetic studies. J Chromatogr B. 2005;818(2):167–73.
Li XY, Sun JG, Wang GJ, Hao HP, Liang Y, Zheng YT, et al. Simultaneous determination of panax notoginsenoside R1, ginsenoside Rg1, Rd, Re and Rb1 in rat plasma by HPLC/ESI/MS: platform for the pharmacokinetic evaluation of total panax notoginsenoside, a typical kind of multiple constituent traditional Chinese medicine. Biomed Chromatogr. 2007;21(7):735–46.
Han M, Fang XL. Difference in oral absorption of ginsenoside Rg (1) between in vitro and in vivo models. Acta Pharmacol Sin. 2006;27(4):499–505.
Lai L, Hao HP, Liu YT, Zheng CN, Wang Q, Wang GJ, et al. Characterization of Pharmacokinetic Profiles and Metabolic Pathways of 20 (S)-Ginsenoside Rh1 in vivo and in vitro. Planta Med. 2009;75(8):797–802.
Li BQ, Qu GF. Inhibition of the hypoxia-induced factor-1 alpha and vascular endothelial growth factor expression through ginsenoside Rg3 in human gastric cancer cells. J Cancer Res Ther. 2019;15(7):1642–6.
Meng LB, Ji R, Dong XM, Xu XC, **n Y, Jiang X. Antitumor activity of ginsenoside Rg3 in melanoma through downregulation of the ERK and Akt pathways. Int J Oncol. 2019;54(6):2069–79.
Chen JM, Zhang XJ, Liu XX, Zhang C, Shang WY, Xue J, et al. Ginsenoside Rg1 promotes cerebral angiogenesis via the PI3K/Akt/mTOR signaling pathway in ischemic mice. Eur J Pharmacol. 2019;856:172418.
Zhao M, **e J, Shen H, Wang X, Wu Q, **a L. Role of endothelial-microparticles and the tissue factor pathway in ginsenoside Rb1-mediated prevention of umbilical vein endothelial cell injury. Biomed Rep. 2021;14(1):8.
Liu HB, Lu XY, Hu Y, Fan XH. Chemical constituents of Panax ginseng and Panax notoginseng explain why they differ in therapeutic efficacy. Pharmacol Res. 2020;161:105263.
Chen YY, Zhang YQ, Song W, Zhang Y, Dong X, Tan MQ. Ginsenoside Rh2 Improves the Cisplatin Anti-tumor Effect in Lung Adenocarcinoma A549 Cells via Superoxide and PD-L1. Anti-Cancer Agent Me. 2020;20(4):495–503.
Lu S, Zhang YB, Li HJ, Zhang J, Ci YQ, Han M. Ginsenoside Rb1 can ameliorate the key inflammatory cytokines TNF-alpha and IL-6 in a cancer cachexia mouse model. Bmc Complement Med. 2020;20:11.
Yang XL, Zou J, Cai HY, Huang XL, Yang XF, Guo DX, et al. Ginsenoside Rg3 inhibits colorectal tumor growth via down-regulation of C/EBP beta/NF-kappa B signaling. Biomed Pharmacother. 2017;96:1240–5.
Li JL, Qi YX. Ginsenoside Rg3 inhibits cell growth, migration and invasion in Caco-2 cells by downregulation of lncRNA CCAT1. Exp Mol Pathol. 2019;106:131–8.
Kim AD, Kang KA, Kim HS, Kim DH, Choi YH, Lee SJ, et al. A ginseng metabolite, compound K, induces autophagy and apoptosis via generation of reactive oxygen species and activation of JNK in human colon cancer cells. Cell Death Dis. 2013;4:e750.
Kang KA, Piao MJ, Kim KC, Zheng J, Yao CW, Cha JW, et al. Compound K, a metabolite of ginseng saponin, inhibits colorectal cancer cell growth and induces apoptosis through inhibition of histone deacetylase activity. Int J Oncol. 2013;43(6):1907–14.
Lee IK, Kang KA, Lim CM, Kim KC, Kim HS, Kim DH, et al. Compound K, a Metabolite of Ginseng Saponin, Induces Mitochondria-Dependent and Caspase-Dependent Apoptosis via the Generation of Reactive Oxygen Species in Human Colon Cancer Cells. Int J Mol Sci. 2010;11(12):4916–31.
Han S, Jeong AJ, Yang H, Bin Kang K, Lee H, Yi EH, et al. Ginsenoside 20 (S)-Rh2 exerts anti-cancer activity through targeting IL-6-induced JAK2/STAT3 pathway in human colorectal cancer cells. J Ethnopharmacol. 2016;194:83–90.
Liu GW, Liu YH, Jiang GS, Ren WD. The reversal effect of Ginsenoside Rh2 on drug resistance in human colorectal carcinoma cells and its mechanism. Hum Cell. 2018;31(3):189–98.
Jang HJ, Han IH, Kim YJ, Yamabe N, Lee D, Hwang GS, et al. Anticarcinogenic effects of products of heat-processed ginsenoside re, a major constituent of ginseng berry, on human gastric cancer cells. J Agr Food Chem. 2014;62(13):2830–6.
Lyu X, Xu XD, Song AL, Guo JY, Zhang YW, Zhang YC. Ginsenoside Rh1 inhibits colorectal cancer cell migration and invasion in vitro and tumor growth in vivo. Oncol Lett. 2019;18(4):4160–6.
Liu YN, Fan DD. Ginsenoside Rg5 induces G2/M phase arrest, apoptosis and autophagy via regulating ROS-mediated MAPK pathways against human gastric cancer. Biochem Pharmacol. 2019;168:285–304.
Yuan ZG, Jiang H, Zhu XH, Liu XG, Li JH. Ginsenoside Rg3 promotes cytotoxicity of Paclitaxel through inhibiting NF-kappa B signaling and regulating Bax/Bcl-2 expression on triple-negative breast cancer. Biomed Pharmacother. 2017;89:227–32.
Choi S, Kim TW, Singh SV. Ginsenoside Rh2-mediated G (1) phase cell cycle arrest in human breast cancer cells is caused by p15 (Ink4B) and p27 (Kip1)-dependent Inhibition of Cyclin-dependent Kinases. Pharm Res-Dordr. 2009;26(10):2280–8.
** Y, Huynh DTN, Nguyen TLL, Jeon H, Heo KS. Therapeutic effects of ginsenosides on breast cancer growth and metastasis. Arch Pharm Res. 2020;43(8):773–87.
Liu YN, Fan DD. The Preparation of Ginsenoside Rg5, its antitumor activity against breast cancer cells and its targeting of PI3K. Nutrients. 2020;12(1):246.
Liu YN, Fan DD. Ginsenoside Rg5 induces apoptosis and autophagy via the inhibition of the PI3K/Akt pathway against breast cancer in a mouse model. Food Funct. 2018;9(11):5513–27.
Zhang GD, He LX, Chen JH, Xu BT, Mao ZJ. Ginsenoside Rh2 activates alpha-catenin phosphorylation to inhibit lung cancer cell proliferation and invasion. Exp Ther Med. 2020;19(4):2913–22.
Song LX, Yang F, Wang ZT, Yang L, Zhou Y. Ginsenoside Rg5 inhibits cancer cell migration by inhibiting the nuclear factor-kappa B and erythropoietin-producing hepatocellular receptor A2 signaling pathways. Oncol Lett. 2021;21(6):452.
Wang M, Yan SJ, Zhang HT, Li N, Liu T, Zhang YL, et al. Ginsenoside Rh2 enhances the antitumor immunological response of a melanoma mice model. Oncol Lett. 2017;13(2):681–5.
Wang CZ, Aung HH, Ni M, Wu JA, Tong RB, Wicks S, et al. Red American ginseng: Ginsenoside constituents and antiproliferative activities of heat-processed Panax quinquefolius roots. Planta Med. 2007;73(7):669–74.
Liu WK, Xu SX, Che CT. Anti-proliferative effect of ginseng saponins on human prostate cancer cell line. Life Sci. 2000;67(11):1297–306.
Oh M, Choi YH, Choi SH, Chung YH, Kim KW, Kim SI, et al. Anti-proliferating effects of ginsenoside Rh2 on MCF-7 human breast cancer cells. Int J Oncol. 1999;14(5):869–75.
Kang KA, Kim YW, Kim SU, Chae S, Koh YS, Kim HS, et al. G (1) phase arrest of the cell cycle by a ginseng metabolite, compound K, in U937 human monocytic leukamia cells. Arch Pharm Res. 2005;28(6):685–90.
Wu WS, Zhou Q, Zhao WJ, Gong YP, Su AP, Liu F, et al. Ginsenoside Rg3 inhibition of thyroid cancer metastasis is associated with alternation of actin skeleton. J Med Food. 2018;21(9):849–57.
Li HL, Huang N, Zhu WK, Wu JC, Yang XH, Teng WJ, et al. Modulation the crosstalk between tumor-associated macrophages and non-small cell lung cancer to inhibit tumor migration and invasion by ginsenoside Rh2. BMC Cancer. 2018;18:579.
Park EK, Lee EJ, Lee SH, Koo KH, Sung JY, Hwang EH, et al. Induction of apoptosis by the ginsenoside Rh2 by internalization of lipid rafts and caveolae and inactivation of Akt. Brit J Pharmacol. 2010;160(5):1212–23.
Bian S, Zhao Y, Li FY, Lu SY, Wang SM, Bai XY, et al. 20 (S)-Ginsenoside Rg3 Promotes HeLa cell apoptosis by regulating autophagy. Molecules. 2019;24(20):3655.
Li C, Dong YC, Wang LB, Xu GB, Yang Q, Tang XF, et al. Ginsenoside metabolite compound K induces apoptosis and autophagy in non-small cell lung cancer cells via AMPK-mTOR and JNK pathways. Biochem Cell Biol. 2019;97(4):406–14.
Liu X, Zhang ZJ, Liu JH, Wang Y, Zhou Q, Wang SW, et al. Ginsenoside Rg3 improves cyclophosphamide-induced immunocompetence in Balb/c mice. Int Immunopharmacol. 2019;72:98–111.
Szebeni J, Baranyi L, Savay S, Bodo M, Morse DS, Basta M, et al. Liposome-induced pulmonary hypertension: properties and mechanism of a complement-mediated pseudoallergic reaction. Am J Physiol-Heart C. 2000;279(3):H1319–28.
Wu QQ, Wang QT, Fu JF, Ren RD. Polysaccharides derived from natural sources regulate triglyceride and cholesterol metabolism: a review of the mechanisms. Food Funct. 2019;10(5):2330–9.
Yang Z, Gao S, Wang JR, Yin TJ, Teng Y, Wu BJ, et al. Enhancement of Oral Bioavailability of 20 (S)-Ginsenoside Rh2 through improved understanding of its absorption and efflux mechanisms. Drug Metab Dispos. 2011;39(10):1866–72.
Baek JS, Yeon WG, Lee CA, Hwang SJ, Park JS, Kim DC, et al. Preparation and characterization of mucoadhesive enteric-coating ginsenoside-loaded microparticles. Arch Pharm Res. 2015;38(5):761–8.
Zhou M, Li X, Li YY, Yao QE, Ming Y, Li ZW, et al. Ascorbyl palmitate-incorporated paclitaxel-loaded composite nanoparticles for synergistic anti-tumoral therapy. Drug Deliv. 2017;24(1):1230–42.
Mathiyalagan R, Subramaniyam S, Kim YJ, Kim YC, Yang DC. Ginsenoside compound K-bearing glycol chitosan conjugates: Synthesis, physicochemical characterization, and in vitro biological studies. Carbohydr Polym. 2014;112:359–66.
Yang L, **n J, Zhang ZH, Yan HM, Wang J, Sun E, et al. TPGS-modified liposomes for the delivery of ginsenoside compound K against non-small cell lung cancer: formulation design and its evaluation in vitro and in vivo. J Pharm Pharmacol. 2016;68(9):1109–18.
Soppimath KS, Aminabhavi TM, Kulkarni AR, Rudzinski WE. Biodegradable polymeric nanoparticles as drug delivery devices. J Control Release. 2001;70(1–2):1–20.
Owens DE, Peppas NA. Opsonization, biodistribution, and pharmacokinetics of polymeric nanoparticles. Int J Pharm. 2006;307(1):93–102.
Alexis F, Pridgen E, Molnar LK, Farokhzad OC. Factors affecting the clearance and biodistribution of polymeric nanoparticles. Mol Pharm. 2008;5(4):505–15.
Otsuka H, Nagasaki Y, Kataoka K. PEGylated nanoparticles for biological and pharmaceutical applications. Adv Drug Deliv Rev. 2003;55(3):403–19.
Sahay G, Alakhova DY, Kabanov AV. Endocytosis of nanomedicines. J Control Release. 2010;145(3):182–95.
Mathiyalagan R, Wang C, Kim YJ, Castro-Aceituno V, Ahn S, Subramaniyam S, et al. Preparation of Polyethylene Glycol-Ginsenoside Rh1 and Rh2 Conjugates and Their Efficacy against Lung Cancer and Inflammation. Molecules. 2019;24(23):4367.
Qiu RN, Qian F, Wang XF, Li HJ, Wang LZ. Targeted delivery of 20 (S)-ginsenoside Rg3-based polypeptide nanoparticles to treat colon cancer. Biomed Microdevices. 2019;21:18.
Su XM, Zhang DS, Zhang HW, Zhao KY, Hou WS. Preparation and characterization of angiopep-2 functionalized Ginsenoside-Rg3 loaded nanoparticles and the effect on C6 Glioma cells. Pharm Dev Technol. 2020;25(3):385–95.
Wang XH, Zhang X, Fan LL, He H, Zhang XF, Zhang YY, et al. Influence of polymeric carrier on the disposition and retention of 20 (R)-ginsenoside-rg3-loaded swellable microparticles in the lung. Drug Deliv Transl Re. 2018;8(1):252–65.
Torchilin VP. Recent advances with liposomes as pharmaceutical carriers. Nat Rev Drug Discov. 2005;4(2):145–60.
da Rocha MCO, da Silva PB, Radicchi MA, Andrade BYG, de Oliveira JV, Venus T, et al. Docetaxel-loaded solid lipid nanoparticles prevent tumor growth and lung metastasis of 4T1 murine mammary carcinoma cells. J Nanobiotechnol. 2020;18:43.
Sharma A, Sharma US. Liposomes in drug delivery: progress and limitations. Int J Pharm. 1997;154(2):123–40.
Bozzuto G, Molinari A. Liposomes as nanomedical devices. Int J Nanomed. 2015;10:975–99.
Al-Jamal WT, Kostarelos K. Liposomes: from a clinically established drug delivery system to a nanoparticle platform for theranostic nanomedicine. Accounts Chem Res. 2011;44(10):1094–104.
Cui YQ, Yang P, Sun P, Yan YD, ** GY, Quan JS. Preparation of PEGylated liposomal ginsenoside; formulation design and in vitro evaluation. Indian J Pharm Sci. 2020;82(1):149–56.
Yu H, Teng LR, Meng QF, Li YH, Sun XC, Lu JH, et al. Development of liposomal Ginsenoside Rg3: formulation optimization and evaluation of its anticancer effects. Int J Pharmaceut. 2013;450(1–2):250–8.
** X, Yang Q, Cai N, Zhang ZH. A cocktail of betulinic acid, parthenolide, honokiol and ginsenoside Rh2 in liposome systems for lung cancer treatment. Nanomedicine. 2020;15(1):41–54.
Zalipsky S, Hansen CB, deMenezes DEL, Allen TM. Long-circulating, polyethylene glycol-grafted immunoliposomes. J Control Release. 1996;39(2–3):153–61.
Xu LQ, Yu H, Yin SP, Zhang RX, Zhou YD, Li J. Liposome-based delivery systems for ginsenoside Rh2: in vitro and in vivo comparisons. J Nanopart Res. 2015;17:415.
** X, Zhou JP, Zhang ZH, Lv HX. The combined administration of parthenolide and ginsenoside CK in long circulation liposomes with targeted tLyp-1 ligand induce mitochondria-mediated lung cancer apoptosis. Artif Cell Nanomed B. 2018;46:S931–42.
Samimi R, Salarian M, Xu WZ, Lui EMK, Charpentier PA. Encapsulation of Acetyl Ginsenoside Rb-1 within Monodisperse Poly (DL-lactide-co-glycolide) microspheres using a microfluidic device. Ind Eng Chem Res. 2014;53(28):11333–44.
Lahiani MH, Eassa S, Parnell C, Nima Z, Ghosh A, Biris AS, et al. Carbon nanotubes as carriers of Panax ginseng metabolites and enhancers of ginsenosides Rb1 and Rg1 anti-cancer activity. Nanotechnology. 2017;28:015101.
Liu CB, Zhang D, Li DG, Jiang D, Chen X. Preparation and Characterization of Biodegradable Polylactide (PLA) Microspheres Encapsulating Ginsenoside Rg3. Chem Res Chin Univ. 2008;24(5):588–91.
Zhang JM, Wang YJ, Jiang YY, Liu TW, Luo YY, Diao EJ, et al. Enhanced cytotoxic and apoptotic potential in hepatic carcinoma cells of chitosan nanoparticles loaded with ginsenoside compound K. Carbohydr Polym. 2018;198:537–45.
Yang L, Zhang ZH, Hou J, ** X, Ke ZC, Liu D, et al. Targeted delivery of ginsenoside compound K using TPGS/PEG-PCL mixed micelles for effective treatment of lung cancer. Int J Nanomed. 2017;12:7653–67.
** X, Yang Q, Cai N. Preparation of ginsenoside compound-K mixed micelles with improved retention and antitumor efficacy. Int J Nanomed. 2018;13:3827–38.
Zhan JM, Jiang YY, Li YP, Li WB, Zhou J, Chen JW, et al. Micelles modified with a chitosan-derived homing peptide for targeted intracellular delivery of ginsenoside compound K to liver cancer cells. Carbohyd Polym. 2020;230:115576.
Zhang YW, Tong DY, Che DB, Pei B, **a XD, Yuan GF, et al. Ascorbyl palmitate/D-alpha-tocopheryl polyethylene glycol 1000 succinate monoester mixed micelles for prolonged circulation and targeted delivery of compound K for antilung cancer therapy in vitro and in vivo. Int J Nanomed. 2017;12:605–14.
Kim YJ, Perumalsamy H, Markus J, Balusamy R, Wang C, Kang SH, et al. Development of Lactobacillus kimchicus DCY51 (T)-mediated gold nanoparticles for delivery of ginsenoside compound K: in vitro photothermal effects and apoptosis detection in cancer cells. Artif Cell Nanomed B. 2019;47(1):30–44.
Singh P, Singh H, Castro-Aceituno V, Ahn S, Kim YJ, Farh ME, et al. Engineering of mesoporous silica nanoparticles for release of ginsenoside CK and Rh2 to enhance their anticancer and anti-inflammatory efficacy: in vitro studies. J Nanopart Res. 2017;19:257.
**a XJ, Tao J, Ji ZW, Long CC, Hu Y, Zhao ZY. Increased antitumor efficacy of ginsenoside Rh-2 via mixed micelles: in vivo and in vitro evaluation. Drug Deliv. 2020;27(1):1369–77.
Li P, Zhou XY, Qu D, Guo MF, Fan CY, Zhou T, et al. Preliminary study on fabrication, characterization and synergistic anti-lung cancer effects of self-assembled micelles of covalently conjugated celastrol-polyethylene glycol-ginsenoside Rh2. Drug Deliv. 2017;24(1):834–45.
Qu D, Wang L, Liu M, Shen S, Li T, Liu Y, et al. Oral nanomedicine based on multicomponent microemulsions for drug-resistant breast cancer treatment. Biomacromol. 2017;18(4):1268–80.
Singh P, Kim YJ, Singh H, Ahn S, Castro-Aceituno V, Yang DC. In situ preparation of water-soluble ginsenoside Rh2-entrapped bovine serum albumin nanoparticles: in vitro cytocompatibility studies. Int J Nanomed. 2017;12:4073–84.
Zare-Zardini H, Taheri-Kafrani A, Amiri A, Bordbar AK. New generation of drug delivery systems based on ginsenoside Rh2-, Lysine- and Arginine-treated highly porous graphene for improving anticancer activity. Sci Rep-Uk. 2018;8:586.
Yao H, Li J, Song YB, Zhao H, Wei ZH, Li XY, et al. Synthesis of ginsenoside Re-based carbon dots applied for bioimaging and effective inhibition o f cancer cells. Int J Nanomed. 2018;13:6249–64.
Dong YN, Fu RZ, Yang J, Ma P, Liang LH, Mi Y, et al. Folic acid-modified ginsenoside Rg5-loaded bovine serum albumin nanoparticles for targeted cancer therapy in vitro and in vivo. Int J Nanomed. 2019;14:6971–88.
Gaucher G, Dufresne MH, Sant VP, Kang N, Maysinger D, Leroux JC. Block copolymer micelles: preparation, characterization and application in drug delivery. J Control Release. 2005;109(1–3):169–88.
Nasongkla N, Bey E, Ren JM, Ai H, Khemtong C, Guthi JS, et al. Multifunctional polymeric micelles as cancer-targeted MRI-ultrasensitive drug delivery systems. Nano Lett. 2006;6(11):2427–30.
Vijayakumar A, Baskaran R, Baek JH, Sundaramoorthy P, Yoo BK. In Vitro cytotoxicity and bioavailability of ginsenoside-modified nanostructured lipid carrier containing curcumin. AAPS PharmSciTech. 2019;20:88.
Qu D, Guo MF, Qin Y, Wang LX, Zong B, Chen YY, et al. A multicomponent microemulsion using rational combination strategy improves lung cancer treatment through synergistic effects and deep tumor penetration. Drug Deliv. 2017;24(1):1179–90.
Salarian M, Samimi R, Xu WZ, Wang ZQ, Sham TK, Lui EMK, et al. Microfluidic Synthesis and Angiogenic Activity of Ginsenoside Rg (1)-Loaded PPF Microspheres. Acs Biomater Sci Eng. 2016;2(11):1872–82.
Hou PP, Pu FL, Zou HY, Diao MX, Zhao CH, ** CY, et al. Whey protein stabilized nanoemulsion: A potential delivery system for ginsenoside Rg3 whey protein stabilized nanoemulsion: Potential Rg3 delivery system. Food Biosci. 2019;31:100427.
Kunjiappan S, Govindaraj S, Parasuraman P, Sankaranarayanan M, Arunachalam S, Palanisamy P, et al. Design, in silico modelling and functionality theory of folate-receptor-targeted myricetin-loaded bovine serum albumin nanoparticle formulation for cancer treatment. Nanotechnology. 2020;31:155102.
Bhuchar N, Sunasee R, Ishihara K, Thundat T, Narain R. Degradable Thermoresponsive Nanogels for Protein Encapsulation and Controlled Release. Bioconjugate Chem. 2012;23(1):75–83.
Teran-Saavedra NG, Sarabia-Sainz JAI, Silva-Campa E, Burgara-Estrella AJ, Guzman-Partida AM, Montfort GRC, et al. Lactosylated albumin nanoparticles: potential drug nanovehicles with selective targeting toward an in vitro model of hepatocellular carcinoma. Molecules. 2019;24(7):1382.
Low PS, Henne WA, Doorneweerd DD. Discovery and development of folic-acid-based receptor targeting for Imaging and therapy of cancer and inflammatory diseases. Accounts Chem Res. 2008;41(1):120–9.
Zhou CC, Song X, Guo CQ, Tan YL, Zhao J, Yang Q, et al. Alternative and injectable preformed albumin-bound anticancer drug delivery system for anticancer and antimetastasis treatment. Acs Appl Mater Inter. 2019;11(45):42534–48.
Ruan CH, Liu LS, Lu YF, Zhang Y, He X, Chen XL, et al. Substance P-modified human serum albumin nanoparticles loaded with paclitaxel for targeted therapy of glioma. Acta Pharm Sin B. 2018;8(1):85–96.
Saha A, Pradhan N, Chatterjee S, Singh RK, Trivedi V, Bhattacharyya A, et al. Fatty-amine-conjugated cationic bovine serum albumin nanoparticles for target-specific hydrophobic drug delivery. Acs Appl Nano Mater. 2019;2(6):3671–83.
Ghosh P, Han G, De M, Kim CK, Rotello VM. Gold nanoparticles in delivery applications. Adv Drug Deliv Rev. 2008;60(11):1307–15.
Giljohann DA, Seferos DS, Daniel WL, Massich MD, Patel PC, Mirkin CA. Gold Nanoparticles for Biology and Medicine. Angew Chem-Int Edit. 2010;49(19):3280–94.
Liong M, Lu J, Kovochich M, **a T, Ruehm SG, Nel AE, et al. Multifunctional inorganic nanoparticles for imaging, targeting, and drug delivery. ACS Nano. 2008;2(5):889–96.
Li ZX, Barnes JC, Bosoy A, Stoddart JF, Zink JI. Mesoporous silica nanoparticles in biomedical applications. Chem Soc Rev. 2012;41(7):2590–605.
Park JH, Gu L, von Maltzahn G, Ruoslahti E, Bhatia SN, Sailor MJ. Biodegradable luminescent porous silicon nanoparticles for in vivo applications. Nat Mater. 2009;8(4):331–6.
Paciotti GF, Myer L, Weinreich D, Goia D, Pavel N, McLaughlin RE, et al. Colloidal gold: A novel nanoparticle vector for tumor directed drug delivery. Drug Deliv. 2004;11(3):169–83.
D’Acunto M, Cioni P, Gabellieri E, Presciuttini G. Exploiting gold nanoparticles for diagnosis and cancer treatments. Nanotechnology. 2021;32:192001.
Datsyuk V, Kalyva M, Papagelis K, Parthenios J, Tasis D, Siokou A, et al. Chemical oxidation of multiwalled carbon nanotubes. Carbon. 2008;46(6):833–40.
Hola K, Zhang Y, Wang Y, Giannelis EP, Zboril R, Rogach AL. Carbon dots-Emerging light emitters for bioimaging, cancer therapy and optoelectronics. Nano Today. 2014;9(5):590–603.
Bianco A, Kostarelos K, Prato M. Applications of carbon nanotubes in drug delivery. Curr Opin Chem Biol. 2005;9(6):674–9.
Sun XM, Liu Z, Welsher K, Robinson JT, Goodwin A, Zaric S, et al. Nano-graphene oxide for cellular imaging and drug delivery. Nano Res. 2008;1(3):203–12.
Kam NWS, O’Connell M, Wisdom JA, Dai HJ. Carbon nanotubes as multifunctional biological transporters and near-infrared agents for selective cancer cell destruction. Proc Natl Acad Sci U S A. 2005;102(33):11600–5.
Liu Z, Sun XM, Nakayama-Ratchford N, Dai HJ. Supramolecular chemistry on water-soluble carbon nanotubes for drug loading and delivery. ACS Nano. 2007;1(1):50–6.
Zhang LM, **a JG, Zhao QH, Liu LW, Zhang ZJ. Functional graphene oxide as a nanocarrier for controlled loading and targeted delivery of mixed anticancer drugs. Small. 2010;6(4):537–44.
Chung C, Kim YK, Shin D, Ryoo SR, Hong BH, Min DH. Biomedical applications of graphene and graphene oxide. Accounts Chem Res. 2013;46(10):2211–24.
Liu JQ, Cui L, Losic D. Graphene and graphene oxide as new nanocarriers for drug delivery applications. Acta Biomater. 2013;9(12):9243–57.
Zare-Zardini H, Taheri-Kafrani A, Ordooei M, Amiri A, Karimi-Zarchi M. Evaluation of toxicity of functionalized graphene oxide with ginsenoside Rh2, lysine and arginine on blood cancer cells (K562), red blood cells, blood coagulation and cardiovascular tissue: In vitro and in vivo studies. J Taiwan Inst Chem E. 2018;93:70–8.
Markovic ZM, Harhaji-Trajkovic LM, Todorovic-Markovic BM, Kepic DP, Arsikin KM, Jovanovic SP, et al. In vitro comparison of the photothermal anticancer activity of graphene nanoparticles and carbon nanotubes. Biomaterials. 2011;32(4):1121–9.
Slowing II, Vivero-Escoto JL, Wu CW, Lin VSY. Mesoporous silica nanoparticles as controlled release drug delivery and gene transfection carriers. Adv Drug Deliv Rev. 2008;60(11):1278–88.
Tang FQ, Li LL, Chen D. Mesoporous silica nanoparticles: synthesis, biocompatibility and drug delivery. Adv Mater. 2012;24(12):1504–34.
Poscher V, Salinas Y. Trends in degradable mesoporous organosilica-based nanomaterials for controlling drug delivery: a mini review. Materials. 2020;13(17):3668.
Peer D, Karp JM, Hong S, FaroKHzad OC, Margalit R, Langer R. Nanocarriers as an emerging platform for cancer therapy. Nat Nanotechnol. 2007;2(12):751–60.
Chapman AP. PEGylated antibodies and antibody fragments for improved therapy: a review. Adv Drug Deliv Rev. 2002;54(4):531–45.
Li RX, He YW, Zhang SY, Qin J, Wang JX. Cell membrane-based nanoparticles: a new biomimetic platform for tumor diagnosis and treatment. Acta Pharm Sin B. 2018;8(1):14–22.
Chen ZW, Wang ZJ, Gu Z. Bioinspired and Biomimetic Nanomedicines. Accounts Chem Res. 2019;52(5):1255–64.
Chen ZW, Wen D, Gu Z. Cargo-encapsulated cells for drug delivery. Sci China Life Sci. 2020;63(4):599–601.
Sun Z, Jiang Y, Stenzel M. Manipulating endogenous exosome biodistribution for therapy. SmartMat. 2021;2(2):127–30.
Briuglia ML, Rotella C, McFarlane A, Lamprou DA. Influence of cholesterol on liposome stability and on in vitro drug release. Drug Deliv Transl Res. 2015;5(3):231–42.
Chaudhury A, Das S, Lee RFS, Tan KB, Ng WK, Tan RBH, et al. Lyophilization of cholesterol-free PEGylated liposomes and its impact on drug loading by passive equilibration. Int J Pharm. 2012;430(1–2):167–75.
Barenholz Y. Doxil (R) - The first FDA-approved nano-drug: Lessons learned. J Control Release. 2012;160(2):117–34.
Wei XH, Cohen R, Barenholz Y. Insights into composition/structure/function relationships of Doxil (R) gained from “high-sensitivity” differential scanning calorimetry. Eur J Pharm Biopharm. 2016;104:260–70.
Shah NN, Merchant MS, Cole DE, Jayaprakash N, Bernstein D, Delbrook C, et al. Vincristine Sulfate Liposomes Injection (VSLI, Marqibo (R)): Results From a Phase I Study in Children, Adolescents, and Young Adults With Refractory Solid Tumors or Leukemias. Pediatr Blood Cancer. 2016;63(6):997–1005.
Shah NN, Merchant M, Cole D, Richards K, Delbrook C, Widemann BC, et al. Vincristine Sulfate Liposomes Injection (VSLI, Marqibo): interim results from a phase i study in children and adolescents with refractory cancer. Blood. 2012;120(21):1497.
Zhang HJ. Onivyde for the therapy of multiple solid tumors. Oncotargets Ther. 2016;9:3001–7.
Qian TX, Cai ZW, Wong RNS, Mak NK, Jiang ZH. In vivo rat metabolism and pharmacokinetic studies of ginsenoside Rg (3). J Chromatogr B. 2005;816(1–2):223–32.
Li T, Shu YJ, Cheng JY, Liang RC, Dian SN, Lv XX, et al. Pharmacokinetics and efficiency of brain targeting of ginsenosides Rg1 and Rb1 given as Nao-Qing microemulsion. Drug Dev Ind Pharm. 2015;41(2):224–31.
Zhao LY, Wang L, Chang LP, Hou YL, Wei C, Wu YL. Ginsenoside CK-loaded self-nanomicellizing solid dispersion with enhanced solubility and oral bioavailability. Pharm Dev Technol. 2020;25(9):1127–38.
**ong J, Guo JX, Huang LS, Meng BY, ** QN. The use of lipid-based formulations to increase the oral bioavailability of panax notoginseng saponins following a single oral gavage to rats. Drug Dev Ind Pharm. 2008;34(1):65–72.
Knop K, Hoogenboom R, Fischer D, Schubert US. Poly (ethylene glycol) in drug delivery: pros and cons as well as potential alternatives. Angew Chem Int Edit. 2010;49(36):6288–308.
Zhou XL, Hao Y, Yuan LP, Pradhan S, Shrestha K, Pradhan O, et al. Nano-formulations for transdermal drug delivery: a review. Chinese Chem Lett. 2018;29(12):1713–24.
Moghimi SM, Hunter AC, Murray JC. Long-circulating and target-specific nanoparticles: theory to practice. Pharmacol Rev. 2001;53(2):283–318.
Kataoka K, Harada A, Nagasaki Y. Block copolymer micelles for drug delivery: design, characterization and biological significance. Adv Drug Deliver Rev. 2012;64:37–48.
Zhao PF, Wang YH, Kang XJ, Wu AH, Yin WM, Tang YS, et al. Dual-targeting biomimetic delivery for anti-glioma activity via remodeling the tumor microenvironment and directing macrophagemediated immunotherapy. Chem Sci. 2018;9(10):2674–89.
Gupta B, Levchenko TS, Torchilin VP. Intracellular delivery of large molecules and small particles by cell-penetrating proteins and peptides. Adv Drug Deliv Rev. 2005;57(4):637–51.
Hu Y, Yu D, Zhang XX. 9-amino acid cyclic peptide-decorated sorafenib polymeric nanoparticles for the efficient in vitro nursing care analysis of hepatocellular carcinoma. Process Biochem. 2021;100:140–8.
Cho HJ, Lee SJ, Park SJ, Paik CH, Lee SM, Kim S, et al. Activatable iRGD-based peptide monolith: Targeting, internalization, and fluorescence activation for precise tumor imaging. J Control Release. 2016;237:177–84.
Liu N, Tang M, Ding JD. The interaction between nanoparticles-protein corona complex and cells and its toxic effect on cells. Chemosphere. 2020;245:125624.
Liu N, Tang M. Toxic effects and involved molecular pathways of nanoparticles on cells and subcellular organelles. J Appl Toxicol. 2020;40(1):16–36.
Pandey RK, Prajapati VK. Molecular and immunological toxic effects of nanoparticles. Int J Biol Macromol. 2018;107:1278–93.
Li L, Ni JY, Li M, Chen JR, Han LF, Zhu Y, et al. Ginsenoside Rg3 micelles mitigate doxorubicin-induced cardiotoxicity and enhance its anticancer efficacy. Drug Deliv. 2017;24(1):1617–30.
Etrych T, Kovar L, Strohalm J, Chytil P, Rihova B, Ulbrich K. Biodegradable star HPMA polymer-drug conjugates: Biodegradability, distribution and anti-tumor efficacy. J Control Release. 2011;154(3):241–8.
Sudimack J, Lee RJ. Targeted drug delivery via the folate receptor. Adv Drug Deliver Rev. 2000;41(2):147–62.
Cabral H, Kataoka K. Progress of drug-loaded polymeric micelles into clinical studies. J Control Release. 2014;190:465–76.
Florczak A, Deptuch T, Lewandowska A, Penderecka K, Kramer E, Marszalek A, et al. Functionalized silk spheres selectively and effectively deliver a cytotoxic drug to targeted cancer cells in vivo. J Nanobiotechnol. 2020;18:177.
de Araujo JTC, Duarte JL, Di Filippo LD, Araujo VHS, Carvalho GC, Chorilli M. Nanosystem functionalization strategies for prostate cancer treatment: a review. J Drug Target. 2021;29(8):808–21.
Sanadgol N, Wackerlig J. Developments of smart drug-delivery systems based on magnetic molecularly imprinted polymers for targeted cancer therapy: a short review. Pharmaceutics. 2020;12(9):831.
Li C, Wang JC, Wang YG, Gao HL, Wei G, Huang YZ, et al. Recent progress in drug delivery. Acta Pharm Sin B. 2019;9(6):1145–62.
Sempkowski M, Zhu C, Menzenski MZ, Kevrekidis IG, Bruchertseifer F, Morgenstern A, et al. Sticky patches on lipid nanoparticles enable the selective targeting and killing of untargetable cancer cells. Langmuir. 2016;32(33):8329–38.
Li YM, Zhi XL, Lin JT, You X, Yuan J. Preparation and characterization of DOX loaded keratin nanoparticles for pH/GSH dual responsive release. Mat Sci Eng C-Mater. 2017;73:189–97.
Ganta S, Devalapally H, Shahiwala A, Amiji M. A review of stimuli-responsive nanocarriers for drug and gene delivery. J Control Release. 2008;126(3):187–204.
Xu ZG, Wang DD, Xu S, Liu XY, Zhang XY, Zhang HX. Preparation of a camptothecin prodrug with glutathione-responsive disulfide linker for anticancer drug delivery. Chem-Asian J. 2014;9(1):199–205.
Fang ZZ, Shen YF, Gao DQ. Stimulus-responsive nanocarriers for targeted drug delivery. New J Chem. 2021;45(10):4534–44.
Harris AL. Hypoxia - A key regulatory factor in tumour growth. Nat Rev Cancer. 2002;2(1):38–47.
Yang GB, Phua SZF, Lim WQ, Zhang R, Feng LZ, Liu GF, et al. A hypoxia-responsive albumin-based nanosystem for deep tumor penetration and excellent therapeutic efficacy. Adv Mater. 2019;31(25):1901513.
Dykman L, Khlebtsov N. Gold nanoparticles in biomedical applications: recent advances and perspectives. Chem Soc Rev. 2012;41(6):2256–82.
Robinson JT, Tabakman SM, Liang YY, Wang HL, Casalongue HS, Vinh D, et al. Ultrasmall reduced graphene oxide with high near-infrared absorbance for photothermal therapy. J Am Chem Soc. 2011;133(17):6825–31.
Wang XY, Xuan ZL, Zhu XF, Sun HT, Li JC, **e ZY. Near-infrared photoresponsive drug delivery nanosystems for cancer photo-chemotherapy. J Nanobiotechnol. 2020;18:108.
Zheng HQ, Zhang YN, Liu LF, Wan W, Guo P, Nystrom AM, et al. One-pot synthesis of metal organic frameworks with encapsulated target molecules and their applications for controlled drug delivery. J Am Chem Soc. 2016;138(3):962–8.
Park J, Jiang Q, Feng DW, Mao LQ, Zhou HC. Size-controlled synthesis of porphyrinic metal-organic framework and functionalization for targeted photodynamic therapy. J Am Chem Soc. 2016;138(10):3518–25.
Furukawa H, Cordova KE, O’Keeffe M, Yaghi OM. The Chemistry and Applications of Metal-Organic Frameworks. Science. 2013;341(6149):974.
Montaseri H, Kruger CA, Abrahamse H. Inorganic nanoparticles applied for active targeted photodynamic therapy of breast cancer. Pharmaceutics. 2021;13(3):296.
Wang F, Banerjee D, Liu YS, Chen XY, Liu XG. Upconversion nanoparticles in biological labeling, imaging, and therapy. Analyst. 2010;135(8):1839–54.
Ma YF, Huang J, Song SJ, Chen HB, Zhang ZJ. Cancer-targeted nanotheranostics: recent advances and perspectives. Small. 2016;12(36):4936–54.
Loo C, Lowery A, Halas NJ, West J, Drezek R. Immunotargeted nanoshells for integrated cancer imaging and therapy. Nano Lett. 2005;5(4):709–11.
Jokerst JV, Lobovkina T, Zare RN, Gambhir SS. Nanoparticle PEGylation for imaging and therapy. Nanomedicine-Uk. 2011;6(4):715–28.
Ming Y, Li YY, **ng HY, Luo MH, Li ZW, Chen JH, et al. Circulating tumor cells: from theory to nanotechnology-based detection. Front Pharmacol. 2017;8:35.
Luo ZT, Yuan X, Yu Y, Zhang QB, Leong DT, Lee JY, et al. From Aggregation-Induced Emission of Au (I)-Thiolate Complexes to Ultrabright Au (0)@Au (I)-Thiolate Core-Shell Nanoclusters. J Am Chem Soc. 2012;134(40):16662–70.
Bhuniya S, Maiti S, Kim EJ, Lee H, Sessler JL, Hong KS, et al. An activatable theranostic for targeted cancer therapy and imaging**. Angew Chem Int Edit. 2014;53(17):4469–74.
Baker SN, Baker GA. Luminescent Carbon nanodots: emergent nanolights. Angew Chem Int Edit. 2010;49(38):6726–44.
Cai WB, Chen XY. Nanoplatforms for targeted molecular imaging in living subjects. Small. 2007;3(11):1840–54.
Wang D, Lin BB, Ai H. Theranostic nanoparticles for cancer and cardiovascular applications. Pharm Res-Dordr. 2014;31(6):1390–406.
Lee HY, Li Z, Chen K, Hsu AR, Xu CJ, **e J, et al. PET/MRI dual-modality tumor imaging using arginine-glycine-aspartic (RGD) - Conjugated radiolabeled iron oxide nanoparticles. J Nucl Med. 2008;49(8):1371–9.
Zhao ZL, Fan HH, Zhou GF, Bai HR, Liang H, Wang RW, et al. Activatable Fluorescence/MRI Bimodal Platform for Tumor Cell Imaging via MnO2 Nanosheet-Aptamer Nanoprobe. J Am Chem Soc. 2014;136(32):11220–3.
Wang SG, Li X, Chen Y, Cai XJ, Yao HL, Gao W, et al. A facile one-pot synthesis of a two-dimensional MoS2/Bi2S3 Composite theranostic nanosystem for multi-modality tumor imaging and therapy. Adv Mater. 2015;27(17):2775.
Zheng MB, Yue CX, Ma YF, Gong P, Zhao PF, Zheng CF, et al. Single-Step Assembly of DOX/ICG loaded lipid-polymer nanoparticles for highly effective chemo-photothermal combination therapy. ACS Nano. 2013;7(3):2056–67.
Fan WP, Bu WB, Shen B, He QJ, Cui ZW, Liu YY, et al. Intelligent MnO2 Nanosheets Anchored with Upconversion Nanoprobes for Concurrent pH-/H2O2-Responsive UCL Imaging and Oxygen-Elevated Synergetic Therapy. Adv Mater. 2015;27(28):4155–61.
Liu JM, Chen JT, Yan XP. Near infrared fluorescent trypsin stabilized gold nanoclusters as surface plasmon enhanced energy transfer biosensor and in vivo cancer imaging bioprobe. Anal Chem. 2013;85(6):3238–45.
Gao XH, Cui YY, Levenson RM, Chung LWK, Nie SM. In vivo cancer targeting and imaging with semiconductor quantum dots. Nat Biotechnol. 2004;22(8):969–76.
Geszke M, Murias M, Balan L, Medjandi G, Korczynski J, Moritz M, et al. Folic acid-conjugated core/shell ZnS:Mn/ZnS quantum dots as targeted probes for two photon fluorescence imaging of cancer cells. Acta Biomater. 2011;7(3):1327–38.
Pramanik M, Ku G, Li CH, Wang LHV. Design and evaluation of a novel breast cancer detection system combining both thermoacoustic, (TA) and photoacoustic, (PA) tomography. Med Phys. 2008;35(6):2218–23.
Naik U, Nguyen QPH, Harrison RE. Binding and uptake of single and dual-opsonized targets by macrophages. J Cell Biochem. 2020;121(1):183–99.
Li SD, Huang L. Stealth nanoparticles: High density but sheddable PEG is a key for tumor targeting. J Control Release. 2010;145(3):178–81.
Yang MY, Li JP, Gu P, Fan XQ. The application of nanoparticles in cancer immunotherapy: Targeting tumor microenvironment. Bioact Mater. 2021;6(7):1973–87.
** J, Zhao QJ. Engineering nanoparticles to reprogram radiotherapy and immunotherapy: recent advances and future challenges. J Nanobiotechnol. 2020;18:75.
Liu XS, Tang IV, Wainberg ZA, Meng H. Safety considerations of cancer nanomedicine-a key step toward translation. Small. 2020;16(36):e2000673.
Chen FM, Wang YJ, Gao J, Saeed M, Li TL, Wang WQ, et al. Nanobiomaterial-based vaccination immunotherapy of cancer. Biomaterials. 2021;270:120709.
Murali VP, Holmes CA. Biomaterial-based extracellular vesicle delivery for therapeutic applications. Acta Biomater. 2021;124:88–107.
Lin L, Wang YF, Wang L, Pan JY, Xu YC, Li SY, et al. Injectable microfluidic hydrogel microspheres based on chitosan and poly (ethylene glycol) diacrylate (PEGDA) as chondrocyte carriers. Rsc Adv. 2020;10(65):39662–72.
Gratton SEA, PohhauS PD, Lee J, Guo I, Cho MJ, DeSimone JM. Nanofabricated particles for engineered drug therapies: A preliminary Biodistribution study of PRINT (TM) nanoparticles. J Control Release. 2007;121(1–2):10–8.
Mallya K, Gautam SK, Aithal A, Batra SK, Jain M. Modeling pancreatic cancer in mice for experimental therapeutics. Biochim Biophys Acta Rev Cancer. 2021;188:554.
Katsiampoura A, Raghav K, Jiang ZQ, Menter DG, Varkaris A, Morelli MP, et al. Modeling of patient-derived xenografts in colorectal cancer. Mol Cancer Ther. 2017;16(7):1435–42.
Acknowledgements
This study was supported by the National Science Foundation of China (No. 82003689, China), and the National Science and Technology Major Project (No. 2018ZX09303044, China).
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
We have included 9 figures (Figs. 1, 5, 6, 7, 8, 9, 10, 11, 12) from previously published literature with required copyright permission from the copyright holder. We have mentioned this in the manuscript with proper citation.
Competing interests
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Wang, H., Zheng, Y., Sun, Q. et al. Ginsenosides emerging as both bifunctional drugs and nanocarriers for enhanced antitumor therapies. J Nanobiotechnol 19, 322 (2021). https://doi.org/10.1186/s12951-021-01062-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12951-021-01062-5