Abstract
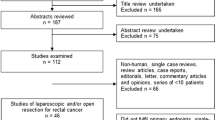
Several studies have reported high rates of urogenital dysfunction after open and laparoscopic surgery for rectal cancer. Robotic surgery has several features that could facilitate identification and preservation of autonomic nerves. This manuscript aims to summarize the literature regarding urogenital function after robotic rectal cancer surgery and focus on technical aspects of nerve-sparing total mesorectal excision. Comprehensive searches were conducted through online databases. Selection criteria included: original articles assessing urinary and sexual function after robotic surgery of males and/or females with standardized questionnaires. A total of 16 articles were included in the review. Seven of the nine cohort studies evaluating male sexual function showed earlier recovery or better outcomes in patients operated with robotic techniques. Two studies did not find any statistically significant difference. Three out of four case series found no difference in sexual function scores measured preoperatively and after 1 year. Female sexual function was assessed in seven studies: two case series show no deterioration of at 1 year. Three comparative studies showed no difference between robotic and laparoscopic groups. Two randomized control trials showed different results in terms of male and female sexual functions with better preservation at 1 year in the robotic group in one and no difference in another. Urinary functions assessed in males and/or females in the 16 studies showed no statistically significant differences at long-term follow-up. At present, there is no evidence of superiority of robotic surgery for performing nerve-sparing rectal cancer surgery.

Similar content being viewed by others
References
Edwards BK, Ward E, Kohler BA, Eheman C, Zauber AG, Anderson RN, Ries LA (2010) Annual report to the nation on the status of cancer, 1975–2006, featuring colorectal cancer trends and impact of interventions (risk factors, screening, and treatment) to reduce future rates. Cancer 116(3):544–573
Kapiteijn E, Velde CV (2002) The role of total mesorectal excision in the management of rectal cancer. Surg Clin North Am 82(5):995–1007. https://doi.org/10.1016/s0039-6109(02)00040-3
Siegel RL, Jemal A, Ward EM (2009) Increase in incidence of colorectal cancer among young men and women in the United States. Cancer Epidemiol Biomark Prev 18(6):1695–1698
Lindsey I, Guy RJ, Warren BF, Mortensen NJ (2000) Anatomy of Denonvilliers fascia and pelvic nerves, impotence, and implications for the colorectal surgeon. Br J Surg 87(10):1288–1299
Lange M, Marijnen C, Maas C, Putter H, Rutten H, Stiggelbout A, Velde CV (2009) Risk factors for sexual dysfunction after rectal cancer treatment. Eur J Cancer 45(9):1578–1588
Banerjee AK (1999) Sexual dysfunction after surgery for rectal cancers. Lancet 353(9168):1900–1902
Hendren SK, O’Connor BI, Liu M, Asano T, Cohen Z, Swallow CJ, Mcleod RS (2005) Prevalence of male and female sexual dysfunction is high following surgery for rectal cancer. Ann Surg 242(2):212–223
Stamopoulos P, Theodoropoulos GE, Papailiou J, Savidis D, Golemati C, Bramis K, Leandros E (2009) Prospective evaluation of sexual function after open and laparoscopic surgery for rectal cancer. Surg Endosc 23(12):2665–2674
Quah HM et al (2002) Bladder and sexual dysfunction following laparoscopically assisted and conventional open mesorectal resection for cancer. Br J Surg 89(12):1551–1556
Nitori N, Hasegawa H, Ishii Y, Endo T, Kitajima M, Kitagawa Y (2008) Sexual function in men with rectal and rectosigmoid cancer after laparoscopic and open surgery. Hepatogastroenterology 55(85):1304–1307
Morino M, Parini U, Allaix ME, Monasterolo G, Contul RB, Garrone C (2008) Male sexual and urinary function after laparoscopic total mesorectal excision. Surg Endosc 23(6):1233–1240
Hur H, Bae SU, Kim NK, Min BS, Baik SH, Lee KY, Choi YD (2013) Comparative study of voiding and male sexual function following open and laparoscopic total mesorectal excision in patients with rectal cancer. J Surg Oncol 108(8):572–578
Schmidt C, Daun A, Malchow B, Küchler T (2010) Sexual impairment and its effects on quality of life in patients with rectal Cancer. Dtsch Arztebl Int 107(8):123–130
Hassan I, Cima RR (2007) Quality of life after rectal resection and multimodality therapy. J Surg Oncol 96(8):684–692
Kim JY, Kim N, Lee KY, Hur H, Min BS, Kim JH (2012) A comparative study of voiding and sexual function after total mesorectal excision with autonomic nerve preservation for rectal cancer: laparoscopic versus robotic surgery. Ann Surg Oncol 19(8):2485–2493
D’Annibale A, Pernazza G, Monsellato I, Pende V, Lucandri G, Mazzocchi P, Alfano G (2013) Total mesorectal excision: a comparison of oncological and functional outcomes between robotic and laparoscopic surgery for rectal cancer. Surg Endosc 27(6):1887–1895
Kenawadekar RD, Dhange RZ, Pandit A, Bandawar MS, Joshi S, Agarwal G, Puntambekar S (2012) Robot-assisted low anterior resection in fifty-three consecutive patients: an Indian experience. J Robot Surg 7(4):311–316
Leung AL, Chan W, Cheung HY, Lui GK, Fung JT, Li MK (2013) Initial experience on the urogenital outcomes after robotic rectal cancer surgery. Surg Pract 17(1):13–17
Luca F, Valvo M, Ghezzi TL, Zuccaro M, Cenciarelli S, Trovato C, Biffi R (2013) Impact of robotic surgery on sexual and urinary functions after fully robotic nerve-sparing total mesorectal excision for rectal cancer. Ann Surg 257(4):672–678
Park SY, Choi G, Park JS, Kim HJ, Ryuk J (2012) Short-term clinical outcome of robot-assisted intersphincteric resection for low rectal cancer: a retrospective comparison with conventional laparoscopy. Surg Endosc 27(1):48–55
Park SY, Choi G, Park JS, Kim HJ, Ryuk J, Yun S (2013) Urinary and erectile function in men after total mesorectal excision by laparoscopic or robot-assisted methods for the treatment of rectal cancer: a case-matched comparison. World J Surg 38(7):1834–1842
Stãnciulea O, Eftimie M, David L, Tomulescu V, Popescu I (2013) Robotic surgery for rectal cancer: a single center experience of 100 consecutive cases. Chirurgia 108(2):143–151
Morelli L, Ceccarelli C, Franco GD, Guadagni S, Palmeri M, Caprili G, Mosca F (2015) Sexual and urinary functions after robot-assisted versus pure laparoscopic total mesorectal excision for rectal cancer. Int J Colorectal Dis 31(4):913–915
Ozeki S, Maeda K, Hanai T, Masumori K, Katsuno H, Takahashi H (2015) Effects of robotic rectal surgery on sexual and urinary functions in male patients. Surg Today 46(4):491–500
Panteleimonitis S, Ahmed J, Ramachandra M, Farooq M, Harper M, Parvaiz A (2017) Urogenital function in robotic vs laparoscopic rectal cancer surgery: a comparative study. Int J Colorectal Dis 32(2):241–248
Schmiegelow AF, Broholm M, Gögenur I, Fode M (2016) Evaluation of sexual and urinary function after implementation of robot-assisted surgery for rectal cancer. Surg Laparosc Endosc Percutan Tech 26(2):141–145
Jayne D, Pigazzi A, Marshall H, Croft J, Corrigan N, Copeland J, Brown J (2017) Effect of robotic-assisted vs conventional laparoscopic surgery on risk of conversion to open laparotomy among patients undergoing resection for rectal cancer. JAMA 318(16):1569
Wang G, Wang Z, Jiang Z, Liu J, Zhao J, Li J (2016) Male urinary and sexual function after robotic pelvic autonomic nerve-preserving surgery for rectal cancer. Int J Med Robot Computer Assisted Surg 13(1):e1725
Kim HJ, Choi G, Park JS, Park SY, Yang CS, Lee HJ (2018) The impact of robotic surgery on quality of life, urinary and sexual function following total mesorectal excision for rectal cancer: a propensity score-matched analysis with laparoscopic surgery. Colorectal Dis 20(5):O103–O113
Kim MJ, Park SC, Park JW, Chang HJ, Kim DY, Nam B, Oh JH (2018) Robot-assisted versus laparoscopic surgery for rectal cancer. Ann Surg 267(2):243–251
Kandeel FR (2001) Male sexual function and its disorders: physiology, pathophysiology, clinical investigation, and treatment. Endocr Rev 22(3):342–388
Panjari M, Bell RJ, Burney S, Bell S, Mcmurrick PJ, Davis SR (2012) Sexual function, incontinence, and wellbeing in women after rectal cancer—a review of the evidence. J Sex Med 9(11):2749–2758
Calpista A, Lai S, Agostini A, Mancini M, Artibani W (2007) Functional urological complications after colorectal cancer surgery. Pelviperineology 26(1):38–40
Campbell WW (2008) Evaluation and management of peripheral nerve injury. Clin Neurophysiol 119(9):1951–1965
Graziottin A, Giraldi A (2006) Anatomy and physiology of womens sexual function. Int Soc Sex Med 1:289–304
Sterk P, Shekarriz B, Günter S, Nolde J, Keller R, Bruch H, Shekarriz H (2005) Voiding and sexual dysfunction after deep rectal resection and total mesorectal excision. Int J Colorectal Dis 20(5):423–427
Luca F, Valvo M (2017) Nerve preservation in robotic rectal surgery. In: Obias V (ed) Robotic colon and rectal surgery. Springer, Heidelberg
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 69(10):613–616
Jacobs M, Verdeja JC, Goldstein HS (1991) Minimally invasive colon resection (laparoscopic colectomy). Surg Laparosc Endosc 1(3):144–150
Ballantyne GH, Merola P, Weber A, Wasielewski A (2001) Robotic solutions to the pitfalls of laparoscopic colectomy. Osp Ital Chir 7(405):405–412
Jayne DG, Brown JM, Thorpe H, Walker J, Quirke P, Guillou PJ (2005) Bladder and sexual function following resection for rectal cancer in a randomized clinical trial of laparoscopic versus open technique. Br J Surg 92(9):1124–1132
Andersson J, Abis G, Gellerstedt M, Angenete E, Angerås U, Cuesta MA, Haglind E (2014) Patient-reported genitourinary dysfunction after laparoscopic and open rectal cancer surgery in a randomized trial (COLOR II). Br J Surg 101(10):1272–1279
Jamali FR, Soweid AM, Dimassi H, Bailey C, Leroy J, Marescaux J (2008) Evaluating the degree of difficulty of laparoscopic colorectal surgery. Arch Surg 143(8):762–767
Marusch F, Gastinger I, Schneider C, Scheidbach H, Konradt J, Bruch HP, Köckerling F (2001) Experience as a factor influencing the indications for laparoscopic colorectal surgery and the results. Surg Endosc 15(2):116–120
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human or animal subjects performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Luca, F., Craigg, D.K., Senthil, M. et al. Sexual and urinary outcomes in robotic rectal surgery: review of the literature and technical considerations. Updates Surg 70, 415–421 (2018). https://doi.org/10.1007/s13304-018-0581-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-018-0581-x