Abstract
Background
Sexual function may be harmed after treatment for rectal cancer. This study aimed to evaluate prospectively the incidence of sexual dysfunction after rectal cancer treatment and to compare the effects of laparoscopic and traditional open approaches in terms of postoperative sexual function.
Methods
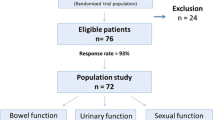
Baseline and 3-, 6-, and 12-month assessments of sexual dysfunction using the International Index of Erectile Function (IIEF) and its specific domains prospectively took place for 56 patients who underwent rectal cancer surgery (38 open vs. 18 laparoscopic procedures, 38 low anterior vs. 18 abdominoperineal resections). The preliminary results are presented.
Results
The average total IIEF and isolated IIEF response domain scores were significantly decreased after surgery (p < 0.01) except for the intercourse satisfaction and overall satisfaction scores at 12 months. An improvement in IIEF scores was observed between the 3- and 6-month assessment points (p < 0.01) except for the erectile function and orgasmic function scores. No significant differences were observed between the open and laparoscopic groups in the total IIEF and domain scores preoperatively and at the 3- and 6-month assessment points. The rates of sexual dysfunction did not differ significantly preoperatively or at 3 months postoperatively when open and laparoscopic procedures were compared, although there was a trend in favor of laparoscopic surgery at 6 months (p = 0.076). The baseline IIEF score and the baseline, 3-, and 6-month sexual desire scores were better (p = 0.035, 0.004, 0.017, and 0.061, respectively) in the low anterior resection group than in the abdominoperineal resection group.
Conclusions
Rectal cancer resections were postoperatively associated with a significant reduction in IIEF scores and high rates of sexual dysfunction at 3 and 6 months. The IIEF and domain scores at different assessment points were comparable between the laparoscopic and open surgery groups. Extending the monitoring period and adding more patients in this ongoing prospective study will further elucidate postoperative sexual dysfunction after rectal cancer surgery.


Similar content being viewed by others
References
Heald RJ, Moran BJ, Ryall RD, Sexton R, MacFarlane JK (1998) Rectal cancer: the Basingstoke experience of total mesorectal excision, 1978–1997. Arch Surg 133:894–899
ASCO (1996) Outcomes of cancer treatment for technology assessment and cancer treatment guidelines. J Clin Oncol 14:671–679
Cammilleri-Brennan J, Steele RJC (1998) Quality of life after treatment for rectal cancer. Br J Surg 85:1036–1043
Hendren SK, O’Connor IB, Liu M, Asano T, Cohenn Z, Swallow JC, MacRae MH, Gryfe R, McLeod SR (2005) Prevalence of male and female sexual dysfunction is high following surgery for rectal cancer. Ann Surg 242:212–223
Chang PL, Fan HA (1983) Urodynamic studies before and/or after abdominoperineal resection of the rectum for carcinoma. J Urol 130:948–951
Kinn AC, Ohman U (1986) Bladder and sexual function after surgery for rectal cancer. Dis Colon Rectum 29:43–48
Santangelo ML, Romano G, Sassaroli C (1987) Sexual function after resection for rectal cancer. Am J Surg 154:502–504
Fazio VW, Fletcher J, Montague D (1980) Prospective study of the effect of resection of the rectum on male sexual function. World J Surg 4:149–152
Havenga K, Enker WE, McDermott K, Cohen AM, Minsky BD, Guillem J (1996) Male and female sexual and urinary function after total mesorectal excision with autonomic nerve preservation for carcinoma of the rectum. J Am Coll Surg 182:495–502
Enker WE, Havenga K, Polyak T, Thaler H, Cranor M (1997) Abdominoperineal resection via total mesorectal excision and autonomic nerve preservation for low rectal cancer. World J Surg 21:715–720
Masui H, Ike H, Yamaguchi S, Oki S, Shimada H (1996) Male sexual function after autonomic nerve-preserving operation for rectal cancer. Dis Colon Rectum 39:1140–1145
Maas CP, Moriya Y, Steup WH, Kiebert GM, Kranenbarg WM, van de Velde CJ (1998) Radical and nerve-preserving surgery for rectal cancer in the Netherlands: a prospective study on morbidity and functional outcome. Br J Surg 85:92–97
Nesbakken A, Nygaard K, Bull Njaa T, Carlsen E, Eri LM (2000) Bladder and sexual dysfunction after mesorectal excision for rectal cancer. Br J Surg 87:206–210
Kim NK, Aahn TW, Park JK, Lee KY, Lee WH, Sohn SK, Min JS (2002) Assessment of sexual and voiding function after total mesorectal excision with pelvic autonomic nerve preservation in males with rectal cancer. Dis Colon Rectum 45:1178–1185
Jayne DG, Brown JM, Thorpe H, Walker J, Quirke P, Guillou PJ (2005) Bladder and sexual function following resection for rectal cancer in a randomized clinical trial of laparoscopic versus open technique. Br J Surg 92:1124–1132
Cöl C, Hasdemir O, Yalçin E, Yandakçi K, Tunç G, Kuçukpinar T (2006) Sexual dysfunction after curative radical resection of rectal cancer in men: the role of extended systematic lymph-node dissection. Med Sci Monit 12:CR70–CR74
Asoglu O, Matlim T, Karanlik H, Atar M, Muslumanoglu M, Kapran Y, Igci A, Ozmen V, Kecer M, Parlak M (2008) Impact of laparoscopic surgery on bladder and sexual function after total mesorectal excision for rectal cancer. Surg Endosc [Epub ahead of print]
Breukink SO, van Driel MF, Pierie JP, Dobbins C, Wiggers T, Meijerink WJ (2008) Male sexual function and lower urinary tract symptoms after laparoscopic total mesorectal excision. Int J Colorectal Dis [Epub ahead of print]
Lacy AM, García-Valdecasas JC, Piqué JM, Delgado S, Campo E, Bordas JM, Taurá P, Grande L, Fuster J, Pacheco JL et al (1995) Short-term outcome analysis of a randomized study comparing laparoscopic vs. open colectomy for colon cancer. Surg Endosc 9:1101–1105
Weeks JC, Nelson H, Gelber S, Sargent D, Schroeder G (2002) Short-term quality-of-life outcomes following laparoscopic-assisted colectomy vs. open colectomy for colon cancer: a randomized trial. JAMA 287:321–328
Breukink SO, Pierie JP, Grond AJ, Hoff C, Wiggers T, Meijerink WJ (2005) Laparoscopic versus open total mesorectal excision: a case-control study. Int J Colorectal Dis 20:428–433
Quah HM, Jayne DG, Eu KW, Seow-Choen F (2002) Bladder and sexual dysfunction following laparoscopically assisted and conventional open mesorectal resection for cancer. Br J Surg 89:1551–1556
Yang L, Yu YY, Zhou ZG, Li Y, Xu B, Song JM, Liu HY, Jiang X (2007) Quality-of-life outcomes following laparoscopic total mesorectal excision for low rectal cancers: a clinical control study. Eur J Surg Oncol 33:575–579
Tsang WW, Chung CC, Kwok SY, Li MK (2006) Laparoscopic sphincter-preserving total mesorectal excision with colonic J-pouch reconstruction: five-year results. Ann Surg 243:353–358
Liang JT, Lai HS, Lee PH (2007) Laparoscopic pelvic autonomic nerve-preserving surgery for patients with lower rectal cancer after chemoradiation therapy. Ann Surg Oncol 14:1285–1287
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 49:822–830
Hojo K, Vernava AMIII, Sugihara K, Katumata K (1991) Preservation of urine voiding and sexual functions after rectal cancer surgery. Dis Colon Rectum 34:532–539
Enker WE, Thaler HT, Cranor ML, Polyak T (1995) Total mesorectal excision in the operative treatment of carcinoma of the rectum. J Am Coll Surg 181:335–346
Havenga K, Maas CP, DeRuiter MC, Welvaart K, Trimbos JB (2000) Avoiding long-term disturbance to bladder and sexual function in pelvic surgery, particularly with rectal cancer. Semin Surg Oncol 18:235–243
Wu CJ, Hsieh JT, Lin JS, Hwang TI, Jiann BP, Huang ST, Wang CJ, Lee SS, Chiang HS, Chen KK, Lin HD (2007) Comparison of prevalence between self-reported erectile dysfunction and erectile dysfunction as defined by five-item International Index of Erectile Function in Taiwanese men older than 40 years. Urology 69:743–747
Canadian Male Sexual Health Council (2004) Prevalence of erectile dysfunction. Canadian Male Sexual Health Council, Toronto, ON, Canada
Moriya Y, Hojo K, Sawada T, Koyama Y (1989) Significance of lateral node dissection for advanced rectal carcinoma at or below the peritoneal reflection. Dis Colon Rectum 32:307–315
Leroy J, Jamali F, Forbes L, Smith M, Rubino F, Mutter D, Marescaux J (2004) Laparoscopic total mesorectal excision (TME) for rectal cancer surgery: long-term outcomes. Surg Endosc 18:281–289
Breukink SO, van der Zaag-Loonen HJ, Bouma EM, Pierie JP, Hoff C, Wiggers T, Meijerink WJ (2007) Prospective evaluation of quality of life and sexual functioning after laparoscopic total mesorectal excision. Dis Colon Rectum 50:147–155
Schmidt CE, Bestmann B, Küchler T, Longo WE, Kremer B (2005) Prospective evaluation of quality of life of patients receiving either abdominoperineal resection or sphincter-preserving procedure for rectal cancer. Ann Surg Oncol 12:117–123
Engel J, Kerr J, Schlesinger-Raab A, Eckel R, Sauer H, Hölzel D (2003) Quality of life in rectal cancer patients: a four-year prospective study. Ann Surg 238:203–213
Zippe CD, Jhaveri FM, Klein EA, Kedia S, Pasqualotto FF, Kedia A, Agarwal A, Montague DK, Lakin MM (2000) Role of Viagra after radical prostatectomy. Urology 55:241–245
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stamopoulos, P., Theodoropoulos, G.E., Papailiou, J. et al. Prospective evaluation of sexual function after open and laparoscopic surgery for rectal cancer. Surg Endosc 23, 2665–2674 (2009). https://doi.org/10.1007/s00464-009-0507-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0507-2