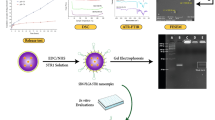
Abstract
Background
Medical fraternity are continuously pitching toward the development of novel mechanisms to combat the menace of cancer and to enhance the efficacy of prevailing molecules. During the drug development phase, majority of new molecular entity pose a threat due to hydrophobic nature, that compromises its bioavailability upon administration. These suboptimal accumulation and low drug loading hampers the clinical translation in cancer therapy.
Main body of abstract
Nanotechnology with valuable advantages create possibilities to accelerate the efficacy of treatment. Compared to matrix-based formulations, drug nanocrystals (NCs) with smaller size, high drug loading, high active targeting, extended circulation, great structural stability, tailored dissolution, and being carrier free have sparked a lot of interest in drug delivery. Many hydrophobic drugs were explored as drug NCs such as—doxorubicin, paclitaxel, campothecin and so on. However, premature leakage and clearance by mononuclear phagocytosis system lead to some great obstacles in the clinical applications of drug NCs.
Conclusion
In the recent years, strategies leading to surface modification are applied to improve uncontrolled drug release and targeting efficiency to tumor cells. The current review sheds light on various properties of drug nanocrystals, brief insights on its fabricating techniques, approaches for tumor targeting with NCs, and their applications in cancer imaging and therapeutics.
Similar content being viewed by others
Background
The field of medicine faces challenges for effectively addressing the complexities of cancer, a multifaceted group of diseases characterized by uncontrolled growth and spread of abnormal cells. Unlike normal cells, which follow a regulated life cycle, cancer cells disrupt this balance and undergo uncontrolled division, leading to the formation of tumor masses[1]. Many factors contribute to development of cancer, like—genetic predisposition, food habits, lifestyle changes, infection caused by harmful microorganisms, and environmental factors [2]. Cancer has become a global burden with approximately 10 million deaths in the year 2022 [3,4,5]. The conventional therapies include radiation therapy, chemotherapy or combination therapy, while immuno-therapy, gene therapy, cell therapy, photodynamic therapy, and antibody therapy have also gained momentum, however, there effectiveness is still under debate as it lacks site specificity and low build-up inside the tumor cells [6, 7]. As a consequence, cancer treatment has now turned toward tailoring approaches which are patient specific depending on the profiles and characteristic of the disease. In this era, nanotechnology being a blend of technology, biomedicine and biomaterials, has been growing as a plausible approach to overcome the current shortfalls. Of them, NCs have sparked a lot of interest in the field of cancer therapeutics, offering unique advantages over conventional drug delivery systems. These nanoscale particles possess the ability to precisely target tumor tissues, stimulate drug solubility, and enhance therapeutic efficacy, revolutionizing the landscape of cancer treatment. The application of NCs in cancer therapy is driven by their small size, large surface area, and unique physicochemical characteristics. These attributes enable efficient drug loading and controlled release, facilitate targeted drug delivery with minimizing side effects on healthy tissues. They have also shown potential to overcome biological barriers, penetrating deep into tumor tissues by both active and passive pathways, and reaching intracellular targets, thereby maximizing treatment outcomes [8, 9]. In addition to drug delivery, NCs play a pivotal role in cancer imaging techniques. Their unique optical and magnetic properties have transformed cancer imaging, providing high-resolution and sensitive modalities. NCs in the form of semiconductor quantum dots, exhibit size-dependent fluorescence emission and high photo-stability, making them exceptional candidates for precise tumor visualization. Similarly, surface modifications with targeting ligands, NCs can be used as contrast agents for imaging, enabling accurate diagnosis, staging, and real-time monitoring of treatment responses [10, 11]. The integration of NCs with imaging techniques allows for multimodal approaches, facilitating comprehensive cancer diagnosis and personalized treatment regimens. Furthermore, NCs offer a versatile platform for combining different therapeutic agents within a single system, enabling synergistic effects, improved drug ratio, and targeted release. This approach enhances therapeutic efficacy while minimizing systemic toxicity. Further by engineering NCs to respond to external stimuli, controlled drug activation and spatiotemporal release can be achieved, paving the way for treatment tailored to individual patient profiles [12, 13].
Despite their immense potential, the full utilization of NCs in cancer treatment requires addressing challenges associated with formulation stability, scalability, and establishing reliable quality control measures. Thus, the current review comprehensively focuses on unveiling the potential of NCs as targeted delivery for the management of cancer.
Main text
Brief insights on nanocrystals and their fabricating method
NCs are nanometer-sized particles consisting purely of drug substances stabilized using suitable stabilizers [14]. The term "nanocrystals" is specifically used to refer to these crystalline nanoparticles or liquid crystalline nanoparticles. Comparing NCs to other carrier-based nanoparticles (NPs), nanocrystals exhibit a high drug loading which allows for a reduction in dose while still enhancing bioavailability and drug safety. Also, for formulating NCs, there is practically no use of organic solvents, making NCs devoid of residual solvents and solvent associated toxicity concerns. Additionally, improved solubility and dissolution rate will promote the pharmacokinetics and bio-distribution of drugs as suggested by Peltonen et al. [15].
The main excipient in fabricating NCs include a stabilizer. The primary function of a stabilizer is to prevent ostwald ripening or aggregation of intrinsically diminuted drug nanoparticles and to preserve them in nano-crystalline form [16]. The selection of stabilizer and its concentration form one of the critical process parameter [17]. Now-a-days, researchers have a wide list of stabilizer starting from non-ionic, ionic, amphoteric to polymeric. Polymeric stabilizers have gained an edge over the others due to their enhanced wetting and steric stabilization property. These stabilizers impart stability to NCs via electrostatic repulsion, van der Waals forces, steric stabilization, surface coating, reducing interfacial tension, etc., [18].
Production techniques of NCs are categorized as top-down, bottom-up and combination technologies (details briefed in Table 1), subsequent section describes briefly the different sub-types of these technologies explored by researchers across the globe.
Top-down techniques diminute the drug substances in micron size state to nanometer size. Different approaches include—media milling, high-pressure homogenization (HPH) (diagrammatically described in Fig. 1), and ultrasonication. Media milling, a mechanical technique used for size reduction, has demonstrated considerable efficiency in the production of NCs. This method employs milling media to fragment drug particles into smaller dimensions, milling agent such as beads/coated balls made of—glass, zirconium oxide, chromium, agate or some special polymers for grinding of drug particles and a stabilizer to ensure the stability of formulation. The main principle of media milling includes impact and attrition [23,24,25,26]. HPH is another top-down technique used for NC formulation. It involves subjecting the drug suspension to high pressure (ranging from 100 to 2000 bar)/ultra-sonication, forcing it through a narrow nozzle or valve. During this process, the particles under-go high shear stress resulting in generation of nano-sized crystalline particles [27, 28]. Dissocubes, Nanopure and Nanoedge are few patented technologies based on use of HPH [29]. Another approach, utilizes ultra-sonication as a means to reduce the particle size. Probe sonicator is a tool to transmit high and low power ultrasound cycles through the drug suspension. These cycles create alternative low and high pressure respectively in the suspension, causing formation of bubbles in low pressure cycle, which break during high pressure cycle. These results in cavitation effect causing reduction in particle size [30, 31].
An alternative strategy for develo** NCs is through a "bottom-up" approach, where drug substances are precipitated to form nanoparticles with accurate control on particle growth. The critical aspect with this approach is controlling the size of re-crystallized particles, as uncontrolled growth might result in Oswald ripening. Some of the technologies using these approach include- high gravity controlled precipitation, sono-crystallization, liquid jet precipitation, rapid expansion of supercritical solution, super critical anti-solvent, multi-inlet vortex mixing, evaporative precipitation into aqueous solution, etc. All these approaches have their own applications, however, major limitation lies in the use of organic solvents [20, 32, 33]. Some of these techniques have been modified by using supercritical fluids instead of organic solvents. Rapid expansion of supercritical solutions (RESS) and supercritical solvent/anti-solvent (SAS) methods of fabricating drug NC are based on the solubility of drugs in supercritical fluids [34, 35]. Hydrosol® and Nanomorph® are the patented technologies to produce drug NCs with size less than 100 nm. An innovative work reported by Han et al., revealed fabrication of paclitaxel nanocrystals (PNC) using a novel approach of evaporation and precipitation technique. The PNC were coated with tannic acid and ferric chloride to enable them for dual therapy—photothermal-chemotherapy. The in-vivo results exhibited mild photothermal activity along with strong tumor inhibition [36]. Through such innovative approach, advancements in the field of cancer treatment are being made, offering the potential for more effective and targeted therapies.
The combination technologies comprise of a two-step process—pre-treatment followed by processing. The pre-process step might be- pre-milling or precipitation, with a high-energy top-down process, such as milling or HPH, while the processing step includes evaporation, lyophilisation, etc. [37]. NANOEDGE®, was developed by Baxter, Inc., USA which involved precipitation of crystals as pre-treatment step and later the processing involved HPH to control the particle size and morphology [38]. More recent advancements have introduced- Nanopure® and SmartCrystal® technology into the market. Later technology integrated high-pressure homogenization with various pre-processes—like H42 (spray-drying pre-process), H69 (precipitation pre-process), H96 (lyophilization pre-process), and CT (media milling pre-process) [39, 40]. Hence, it could be summarized that all the different technologies are efficient enough for fabrication of different and stable NCs.
Role of nanocrystal technology in tumor targeting
Nanotechnology has sparked a lot of possibilities for effective delivery of poorly soluble drugs [41, 42]. They have emerged as a promising tool in the field of cancer therapy, offering unique properties and versatility to revolutionize treatment approaches [8]. One of the key advantage is their ability to serve as carriers for chemotherapy drugs by addressing crucial challenges of poor solubility, limited bioavailability, and systemic toxicity, thereby enhancing drug stability and solubility while enabling their efficient delivery to the tumor site. By modifying the surface of NCs with specific ligands, such as antibodies or peptides, they can be engineered to selectively recognize and bind to cancer cells. These targeted approach facilitates the direct delivery of therapeutic agents to the tumor site while minimizing exposure to healthy tissues [107].
Oral administration
NCs when administered via oral route enter into the GIT. A part of the NCs are absorbed via villi in the intestine, the remaining amount enters the blood stream while some still get excreted via feces. In the intestinal lumen they form complex with the bile acid, which later go across the mucus layer, epithelial layer and finally reach the blood capillary. In the blood stream, enzymes cause metabolism of the NCs in liver and spleen, a part of it is excreted via kidney and a fraction reaches the target site. In a study, PTX-NCs were administered orally to BALB/c tumor-bearing mice with two doses 80 mg/kg and 60 mg/kg. The tumor volume measured after day 6 of the treatment revealed reduction to one third volume when treated with NCs as compared to free PTX [108]. In another study PTX-NCs were coated with N-((2-hydroxy-3-trimethylammonium) propyl) chitosan chloride (HTCC) maintaining the average particle size around 130 nm, were observed to be localized in GIT within 3 h of oral administration. Eventually after 24 h, fluorescence signals showed their preferential accumulation in the tumor. The control group treated with taxol, also inhibited the tumor growth, however, the NCs had long residence time in tumor resulting in remarkable inhibition. The medial survival rates were lengthened even after discontinuation of the treatment [8, 109]. Thereby, such studies have unveiled the path traveled by NC after oral administration.
Parenteral administration
Upon i.v. administration the NCs enter the blood stream and bruit around in the body. During this journey they encounter interactions with different proteins and other elements present in the blood stream. While circulating, they stumble on with the mononuclear phagocytic system (MPS), the larger size NCs are taken up by these MPS present in organs. The smaller size NCs, take a french leave across the MPS and show prolong circulation in the blood. Upon reaching the tumor site, they penetrate through the leaky vasculature of the tumor cells and undergo the EPR effect resulting in accumulation of NCs. Some of NCs enter the lymphatic system via the lymph nodes of the tumor tissue and go efferent into the blood stream. The extended circulation of NCs ensure their extended residence in the tumor, resulting in better efficacy and lower toxicity to healthy tissues [110, 111].
Diving into the fate, NCs are recognized and rapidly taken up by the phagocytic cells of macrophages. At this time, they are also labeled by opsonins, and immunoglobulins. They will be docked onto the receptors present on the macrophages, monocytes, and neutrophils, causing catastrophe of NCs via phagocytosis. The in-vivo fate is influenced by many factors- particle size, surface charge, surface hydrophilicity/hydrophobicity, morphology, dissolution rate, as well as concentration. Among these factors surface morphology influence the most [112]. Many anticancer drugs are delivered in the form of NCs—methoxyestradiol (2-ME), puerarin, and oridonin via i.v. injection [113, 114]. In a recent study consisting of PTX and campothecin NCs stabilized using pluronic-F127, significant inhibition of growth of human cancer and murine breast cancer, was observed [115, 116]. Similarly, PTX-NCs having nearly spheroid shape and hydrodynamic diameter of 419.9 ± 80.9 nm, were surface coated with polydopamine to form a reaction platform for effective PEGylation and RGD peptide conjugation. Cellular uptake and growth inhibition studies over A549 lung cells demonstrated superior activity over non-PEGylated NCs. The results suggest intratumor accumulation and retarded tumor growth, giving a hope toward coating being effective in functionalization of NCs for enhanced anti-cancer activity [117]. In another study, tocopheryl polyethylene glycol succinate (TPGS) stabilized PTX-NCs showed better therapeutic effect in taxol-resistant ovarian cancer both in-vivo and in-vitro [118]. Similarly, campothecin NCs were studied over lung metastasis of MDA-MB-231 and MCF-7 tumors. The results supported with the confocal images of the tumor sections revealed a better inhibition of tumor metastasis and apoptosis with NCs compared to campothecin salt solution and control group [116]. Such study reports supply glimpse of information depicting the in-vivo fate of NCs upon parenteral administration.
Applications of NC in cancer diagnostics and bio-imaging
NCs have also garnered significant attention in the field of bio-imaging offering promising prospects toward unambiguous detection. Cellulose NCs (CNCs) conjugated with fluorescent agents (rhodamine-B-isothiocyanate and FITC) have been explored for therapeutic imaging of tumors by measuring the acoustic signals. Similarly, non-conjugated CNCs were used for photoacoustic imaging of ovarian cancer in mouse models. The peak photoacoustic signal was reported at 700 nm with doses below 1.2 mg/mL in carcinomatous cells. For efficient bioimaging the NCs were conjugated fluorescent agent to passively trigger cell internalization with insignificant toxicity [119]. Mahmoud et al. proved the capability of fluorescent CNCs to penetrate the cancerous cells without a sign of toxicity and no effect on integrity of cell membrane. They also provided evidence of intake of positively charged CNC-RBITCs within the membranes of Spodoptera frugiperda (Sf9) and human embryonic kidney 293 (HEK 293) cells, while CNC-FITC were not taken-up owing to their negative charge. These reports suggest the relevance of surface charge of NCs with their uptake [120]. Magnetic-NCs in the form of magnetic probes have opened new avenues for bio-imaging with its signal enhancement capabilities. Although magnetic resonance imagining (MRI) is widely accepted diagnostic tool, its non-invasive nature, tomographic compatibilities and low-signal sensitivity hinders its applications. Iron-oxide-based magnetic NCs including superparamagnetic iron oxide (SPIO) are being used for enhancing the signal for better tomographic imaging. Recently, a water soluble magnetic iron-oxide NCs was fabricated with tunable MR signaling effect. The magnetic NC probes were successful in diagnosis of breast cancer tested over SK-BK-3 cell lines. Similar study was tested in breast cancer induce mice and the results suggest that the magnetic NC-antibody probe was able to signal the diagnosis of cancer with magnetic-field of 1.5 and 9.4 T. At higher magnetic-field Yong et al. [121] reported the detailed monitoring of cancer cells with complex vasculature and tumor tissues, thus suggesting the enlightening potential of magnetic NCs for diagnostics purposes.
Gold-NCs with different size and shapes have potential to extend the resonance from visible to near infrared range where light can infiltrate into the tissues. At resonance wavelength gold can absorb and scatter the light, this property enables a distinct color to gold which is sensitive to be detected by naked eye, making gold NCs excellent for biomedical diagnostics. Typically, such gold NCs have been extensively used for immunogenic strip test. The surface electrons on the gold NCs can amplify Raman scattering signals, thus AuNCs with immune probes/antibodies significantly enhance sensitivity and contrast of detection which are stable with repetitive analysis, making it an important candidate as imaging agent for cancer cell identification and diagnosis [122]. In a study conducted with fabrication of Eu/Gd codo** HAP-NCs using co-precipitation technique possess a luminescence property, which enabled successful cell labeling and in-vivo imaging [149]. For the therapeutic purpose, researchers developed ZnO-nanoparticles loaded with DOX. This co-administration caused synergistic effect and enhanced cytotoxicity [150]. Additionally, ZnO can be used for biosensing, which enables the early identification of malignancy [151]. Moreover, the effect of zinc nanostructures on living cells, in particular cancer cells, is still under debate.
Gold nanoparticles (Au-NCs)
Over the period of time, novel delivery carriers resulted in reduction in dose dependent toxicity in comparison to conventional products. These lead to increase in research on exploring metallic materials for targeted delivery and diagnosis. Au-NC are aggregates of Au atoms ranging between 10 to 400 nm in size. The amount of gold, material of inorganic substrates, pH of medium, temperature and mechanical forces used during the synthesis governs the shaper of Au-NCs. The Au-NCs when conjugated with stimuli-responsive polymers, are found to be used for targeted delivery to specific organs of human body [152]. Various reports have successfully loaded anticancer drugs—campothecin, thymectacin, busulfan and cyclosporine using Au-NCs [8].
A study to treat metastatic breast cancer was carried out by Wang et al., using DOX decorated Au-nanorods. With irradiation of near-infrared light over these decorated Au-nanorods, caused increase in temperature along with release of DOX within the tumor as Au-NCs show a sharp absorption peak around 500–550 nm due to excitation of surface plasmons. These combination was observed to be more toxic in 4T1 breast cancer cells [153, 154]. A similar study was conducted over 4T1 breast cancer cells with Au-NCs loaded with 10-hydroxycampothecin. The AuNCs possessed average size of 130 nm with 75% drug loading, when administered i.v, showed a sustain drug release pattern and enhanced cytotoxicity [155]. A study conducted by Shen et al., revealed the use of Au-NCs for inhibition of retinal angiogenesis. The Au-NCs with average size of 26.2 nm and potential of 24.9 mV, were able to inhibit the cell proliferation to an extent of 50–72% and 54–83% inhibition of cell migration at concentration 10 µg/mL and 20 µg/mL, respectively [156]. Li et al., carried out a study to test Au-NCs as potential antiangiogenic agents. In this investigation, Au-NCs were used to target human recombinant endostatin (angiogenesis inhibitor). The results showed promising effects with tumor vascular normalization and strengthened blood vessel [157]. Au-NCs fabricated in conjugation with hydroxylcampothecin and polydopamine, when injected i.v. into the mice, showed accumulation and cytotoxicity in the tumor [162].
According to Muhammad et al., AgNCs functionalized with PTX boost the anticancer activity in human cells. The PTX-NCs were surfaced with polydopamine, later the AgNPs and tumor targeting peptide NR1 was decorated onto the PDA. This grafted Ag-PTX-NC system dramatically enhanced the cellular absorption during in-vitro anticancer models. Additionally, the Ag-PTX-NCs showed synergistic influence causing cell membrane lysis, nucleus damage, mitochondrial dysfunction, ROS over production, and breakage of DNA. Such observations linked the potential application of NR1/Ag-NC decorated PTX for targeted therapy of anticancer drugs [163]. Liang et al., demonstrated the anticancer effect of camptothecin (CPT)/Ag-NCs. Silver exhibit excellent inhibitory effect on drug resistance related p-glycoprotein (Pgp) while CPT has proven data of being cytotoxic. The combination of both CPT/Ag-NCs was able to bypass the Pgp recognition resulting in indiscriminate cytotoxicity. In addition, the drastic release of CPT into the tumor triggered by cleavage of Ag-ions in acidic microenvironment led to chromatin structure breakage, DNA damage and apoptosis. Nevertheless, such exploration of molecular events needs support of in-vivo studies [164]. Kim et al. investigated the toxic effect of synthesized crystalline AgNPs on F9 cells. They identified the dose-dependent toxic effect of AgNPs was linked with leakage of lactate dehydrogenase, ROS, and mitochondrial dysfunctioning. At high concentration DNA fragmentation, neuronal differentiation, increased expression of apoptotic genes, and decreased expression of anti-apoptotic genes was reported. The results support the use of crystalline AgNPs for differentiation therapy in amalgamation with chemotherapeutic agents [165]. In a report published by Paul et al., the crystalline AgNPs were biosynthesized using ethanolic leaf powder extract of Premna serratifolia L. and possessed 22.97 nm size. Anticancer effect of the synthesized AgNPs was evaluated on Swiss albino mice induced with liver cancer. The results revealed AgNPs were non-toxic with protective effects of other organs while they sustained control over the cancer progression. Such studies open up ways toward cost-effective economic alternatives for anticancer therapy, however certain understanding of molecular mechanism restrain the use of synthesized Ag-NPs of P. serratifolia [166]. Nima et al. developed Ag–Au nanorods functionalized with certain molecules and antibodies improved photothermal contrast and surface-enhanced Raman scattering (SERS) for the diagnosis of breast cancer [167]. Thus, AgNCs embark great potential to be explored for diagnostic and therapeutic purposes. A brief list of metal based drug delivery explored for cancer therapeutics is reported in Table 5.
Regulatory challenges toward formulation of drug NCs
In addition to opportunities and challenges, hurdles pertaining to approval of NCs by the regulatory bodies are one of the major obstacle in its commercialization. A bridge needs to be build-up with validation, toxicity, reproducibility and stability of NCs produced in academic setting to enable collaboration with industries. A hel** hand with adopting minimal standards for conducting pre-clinical studies was offered by US-FDA and European medical agency (EMA), to promote clinical translation of academic-industry collaboration. On the other hand, following good manufacturing practice (GMP) becomes crucial while demonstrating the promise of technology for effective drug delivery and diagnostics. However, following GLP might increase the overall cost, but with previously demonstrated proof of concept, the collaborators may seek funding from different organization for the said purpose. Pre-clinical studies might also need placebo controlled treatment regimens for appropriate evaluation of safety and efficacy. In these context, FDA has initiated the Nanotechnology Regulatory Science Research Plan. The plan aims to address the gap in scientific knowledge required to make regulatory assessment of NCs hassle free. The plan includes major criteria- physio-chemical characterization, preclinical models, risk characterization, risk assessment, and risk communication open for discussion with collaborators [177]. A fruitful outcome of the plan is the establishment of Nanotechnology Characterization Lab, that performs characterization of the different nanoparticles received from government funded research labs, academia, and industry. These platform integrates academic-industry collaborations to gather relevant data for filing Investigational New Drug application. Thus, such resource utilization enables academic-industry collaborations for effective translation of the NC-based therapeutics established by academic to reach market [178].
A part from these, a significant consideration must also be given to selection of demographics for performing clinical trials. Recently, a phase 2 clinical study failed to achieve its primary end point for treating lung cancer, and prostate cancer using BIND-014 (PSMA-targeted docetaxel nanocrystals). This results reflect the need for designing clinical trials, considering selection of patients based on EPR, tumor heterogeneity, presence of target receptors, ability of NCs to bind to receptors, and the simultaneous need for diagnostics during the study are some of the crucial parameters for achieving better outcomes [175]. Another NC-based product called as Panzem Nanocrystal Colloidal Dispersion is currently under phase 2 clinical trials, being explored for its potential effect on prostrate and ovarian cancer. Some of the NC-based formulation approved for commercialization by FDA are listed in Table 6. A pioneering effort in this direction was adopted by Merrimack Pharmaceuticals, to determine the accumulation of ferumoxytol iron nanoparticles (FMX) using quantitative MRI and may predict the response to nanoliposomal-irinotecan. The study concluded that the tumors with high accumulation of FMX were more responsive to nano-liposomes [176]. This study was based on simultaneous quantitative estimation using MRI, and we believe that such initiatives along with pre-selection of patients will turn out to be a bridging bench-bed gap. Thereby promoting the commercialization of highly potent NCs with detailed safety and efficacy profiles along with backbone of clinical data.
Conclusion and future prospects
Delivery of BCS class II and IV is challenging yet a promising pitch for research. NC-based drug delivery has emerged with incomparable drug loading over other carrier-based drug delivery systems for poorly soluble drug substances. Over the last two decades, NC technology have shown useful and prevailing role in the treatment of cancer providing improved drug targeting and delivery. Current research on these drug substances deals with strategies to improve their absorption and selective delivery to tumor cells, leading to emergence of surface functionalization and usage of novel excipients. To add cherry on the top, their functionalization with targeting ligands offers excellent dynamism to control the growth of tumors. With the on-going research, different new techniques have also evolved for the production of NCs. These techniques involve combination of top-down and bottom-up approaches to effectively rationalize their advantages. Nevertheless, the clinical efficacy of drug NCs depends on number of factors. The present review highlighted multifaceted applications of different types of NCs in the management of cancer. Metal based NCs have offered simultaneous application in diagnostic and therapy with targeted drug delivery, thereby revolutionizing cancer management and therapy. The drug-metal NC complex enable tracking within the body owing to their interaction with light, thus offer an efficient therapy in addition to chemotherapy. Despite these facts, their clinical translation and market authorization is challenging due to certain bottlenecks. Toxic effects are possible due to their tiny size and large surface area which boosts reactivity with the biological targets. Numerous problems with respect to long-term sustainability and safety of nanoparticles has always remained unresolved. Inflammation, genotoxicity, and organelle failure in cells are few dose dependent toxic effects of nanocrystalline particles. Also, the activation of oxidative enzymes results in increase in concentration of free radicals and in-turn increase oxidative stress and cell damage. Moreover, they have a great potential if the risks and toxicity are controlled from production to treatment. Certain ways including coating with polymers and with the concept of green synthesis, a relatively safe way for the use of metallic nanoparticles can be en-routed.
As far as biological challenges are concerned, the bridge between the disease pathology and human heterogeneity is required. Also, the physicochemical properties of drug NCs should primarily focus on overcoming biological barriers to achieve target and reduce build-up in nonspecific organs. Unfortunately, lack of attention toward these aspects, cause failure observed during the translation of promising NCs in clinical trials. These factors could be deterrent for pharmaceutical industries for investing on commercialization of NC-based products. To cope with this challenge, there is a dire need for inclusive evaluation of preclinical data with special emphasis on efficacy, safety, pharmacokinetics (ADME profile), targeting efficiency and stability with appropriate tumor induced animal models. Also, reproducibility of the results must be validated using different animal models, such practise will boost the reliability toward the anticancer therapy. For most of commercialized products, EPR-mediated accumulation has been reported in most of the animal models. Moreover, the tumors are heterogeneous and may possess inter and intra patient variability. With NC-based products, the amount of cellular uptake and drug release kinetics inside the target sites can be tailored, moving away from the traditional concept of one-size-fits all.
Although most of the research about drug NCs on cancer therapy are still in preclinical development, the motivation arises from those products which have reached the market, with enhanced circulation time, site specific cellular uptake, long retention in tumor environment and reduction in dose-dependent toxicity. Also, decorated NCs with targeting ligands have generated a ray of hope for cancer therapy. Even, NCs can be labeled with dyes/contrast agents to further augment visualization and theranostic applications. In nutshell, NC technology has profound opportunities to mitigate cancer therapy and with gradual maturation of drug NCs, commercialization of NC-based products will emerge like a boon for cancer therapeutics.
Availability of data and materials
Not applicable.
Abbreviations
- NCs:
-
Nanocrystals
- HPH:
-
High-pressure homogenization
- RESS:
-
Rapid expansion of supercritical solutions
- PNC:
-
Paclitaxel nanocrystals
- EPR:
-
Enhanced permeability and retention
- PTX:
-
Paclitaxel
- MTO NCs:
-
Mitoxantrone nanocrystals
- RES:
-
Reticuloendothelial system
- PEG:
-
Polyethylene glycol
- PLGA-PEG:
-
Polylactide-co-glycolide-Polyethylene glycol
- MMP:
-
Matrix metallo-proteinases
- TNF:
-
Tumor necrosis factor
- PSMA:
-
Prostate-specific membrane antigen
- FA:
-
Folic acid
- I.V.:
-
Intravenous
- GIT:
-
Gastrointestinal tract
- MPS:
-
Mononuclear phagocytic system
- TPGS:
-
D-a-tocopheryl polyethylene glycol 1000 succinate
- CNCs:
-
Cellulose nanocrystals
- FITC:
-
Fluorescein isothiocyanate
- RBITC:
-
Rhodamine-b-isothiocyanate
- MRI:
-
Magnetic resonance imaging
- AuNCs:
-
Gold nanocrystals
- DNA:
-
Deoxy ribonucleic acid
- Fe-NCs:
-
Iron nanocrystals
- Zn-NCs:
-
Zinc nanocrystals
- Ag-NCs:
-
Silver nanocrystals
- SPIONs:
-
Superparamagnetic iron nanocrystals
- ROS:
-
Reactive oxygen species
- DOX:
-
Doxorubicin
- mPEG:
-
Methoxypolyethene glycol
- TAT:
-
Trans-activator of transcription
- UV:
-
Ultra violet
- ZnO:
-
Zinc oxide
- Pgp:
-
P-glycoprotein
- CPT:
-
Camptothecin
- US-FDA:
-
United States Food and Drug Administration
- EMA:
-
European medical agency
- GMP:
-
Good manufacturing practice
- BCS:
-
Biopharmaceutical classification system
- MOA:
-
Mechanism of action
References
Compton C, Compton C (2020) Cancer initiation, promotion, and progression and the acquisition of key behavioral traits. Cancer: The Enemy from Within. Springer
Boubertakh B, Silvestri C, Di Marzo V (2022) Obesity: the fat tissue disease version of cancer. Cells 11(12):1872
Mattiuzzi C, Lippi G (2019) Current cancer epidemiology. J Epidemiol Glob Health 9(4):217
Loeffen EA, Knops RR, Boerhof J, Feijen EL, Merks JH, Reedijk AM et al (2019) Treatment-related mortality in children with cancer: prevalence and risk factors. European J Cancer 121:113–122
Miller KD, Nogueira L, Devasia T, Mariotto AB, Yabroff KR, Jemal A et al (2022) Cancer treatment and survivorship statistics, 2022. CA Cancer J Clin 72(5):409–436
Miller KD, Nogueira L, Mariotto AB, Rowland JH, Yabroff KR, Alfano CM et al (2019) Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin 69(5):363–385
** S, Sun Y, Liang X, Gu X, Ning J, Xu Y et al (2022) Emerging new therapeutic antibody derivatives for cancer treatment. Signal Transduct Target Ther 7(1):39
Miao X, Yang W, Feng T, Lin J, Huang P (2018) Drug nanocrystals for cancer therapy. Wiley Interdiscip Rev Nanomed Nanobiotechnology 10(3):e1499
Navya P, Kaphle A, Srinivas S, Bhargava SK, Rotello VM, Daima HK (2019) Current trends and challenges in cancer management and therapy using designer nanomaterials. Nano Convergence 6(1):1–30
Joseph E, Singhvi G (2019) Multifunctional nanocrystals for cancer therapy: a potential nanocarrier. Nanomater Drug Deliv Ther 91–116
Desai N, Momin M, Khan T, Gharat S, Ningthoujam RS, Omri A (2021) Metallic nanoparticles as drug delivery system for the treatment of cancer. J Expert Opinion Drug Deliv 18(9):1261–1290
Yenurkar D, Nayak M, Mukherjee S (2023) Recent advances of Nanocrystals in Cancer theranostics. Nanoscale Adv
Lu L, Xu Q, Wang J, Wu S, Luo Z, Lu L (2022) Drug nanocrystals for active tumor-targeted drug delivery. Pharmaceutics 14(4):797
Sharma OP, Patel V, Mehta T (2016) Nanocrystal for ocular drug delivery: hope or hype. Drug Deliv Transl Res 6:399–413
Peltonen L, Hirvonen J (2018) Drug nanocrystals–versatile option for formulation of poorly soluble materials. Int J Pharm 537(1–2):73–83
Al-Kassas R, Bansal M, Shaw J (2017) Nanosizing techniques for improving bioavailability of drugs. J Control Release 260:202–212
Fontana F, Figueiredo P, Zhang P, Hirvonen JT, Liu D, Santos HA (2018) Production of pure drug nanocrystals and nano co-crystals by confinement methods. Adv Drug Deliv Rev 131:3–21
Sharma OP, Patel V, Mehta T (2016) Design of experiment approach in development of febuxostat nanocrystal: application of Soluplus® as stabilizer. Powder Technol 302:396–405
Patel V, Sharma OP, Mehta T (2018) Nanocrystal: a novel approach to overcome skin barriers for improved topical drug delivery. Expert Opin Drug Deliv 15(4):351–368
Sinha B, Müller RH, Möschwitzer JP (2013) Bottom-up approaches for preparing drug nanocrystals: formulations and factors affecting particle size. Int J Pharm 453(1):126–141
Malamatari M, Taylor KM, Malamataris S, Douroumis D, Kachrimanis K (2018) Pharmaceutical nanocrystals: production by wet milling and applications. Drug Discov Today 23(3):534–547
Mohammad IS, Hu H, Yin L, He W (2019) Drug nanocrystals: Fabrication methods and promising therapeutic applications. Int J Pharm 562:187–202
Patel V, Sharma OP, Mehta TA (2019) Impact of process parameters on particle size involved in media milling technique used for preparing clotrimazole nanocrystals for the management of cutaneous candidiasis. AAPS PharmSciTech 20:1–15
Chogale M, Gite S, Patravale V (2020) Comparison of media milling and microfluidization methods for engineering of nanocrystals: a case study. Drug Dev Ind Pharm 46(11):1763–1775
Junyaprasert VB, Morakul B (2015) Nanocrystals for enhancement of oral bioavailability of poorly water-soluble drugs. Asian J Pharm Sci 10(1):13–23
Parveen N, Abourehab MA, Thanikachalam PV, Khar RK, Kesharwani P (2023) Nanocrystals as an emerging nanocarrier for the management of dermatological diseases. Colloids and Surf B Biointerf. 113231
Romero GB, Keck CM, Müller RH (2016) Simple low-cost miniaturization approach for pharmaceutical nanocrystals production. Int J Pharm 501(1–2):236–244
Pawar VK, Singh Y, Meher JG, Gupta S, Chourasia MK (2014) Engineered nanocrystal technology: in-vivo fate, targeting and applications in drug delivery. J Control Release 183:51–66
Jarvis M, Krishnan V, Mitragotri S (2019) Nanocrystals: a perspective on translational research and clinical studies. Bioeng Transl Med 4(1):5–16
Shojaeiarani J, Bajwa D, Holt G (2020) Sonication amplitude and processing time influence the cellulose nanocrystals morphology and dispersion. Nanocomposites 6(1):41–46
Sohn JS, Yoon DS, Sohn JY, Park JS, Choi JS (2017) Development and evaluation of targeting ligands surface modified paclitaxel nanocrystals. Mater Sci Eng C 72:228–237
Asimakidou T, Makridis A, Veintemillas-Verdaguer S, Morales M, Kellartzis I, Mitrakas M et al (2020) Continuous production of magnetic iron oxide nanocrystals by oxidative precipitation. Chem Eng J 393:124593
Shah PS, Husain S, Johnston KP, Korgel BA (2001) Nanocrystal arrested precipitation in supercritical carbon dioxide. J Phys Chem B 105(39):9433–9440
Padrela L, Rodrigues MA, Duarte A, Dias AM, Braga ME, de Sousa HC (2018) Supercritical carbon dioxide-based technologies for the production of drug nanoparticles/nanocrystals–a comprehensive review. Adv Drug Deliv Rev 131:22–78
Aymonier C, Philippot G, Erriguible A, Marre S (2018) Playing with chemistry in supercritical solvents and the associated technologies for advanced materials by design. J Supercritic Fluids 134:184–196
Huang X, Shi Q, Du S, Lu Y, Han N (2021) Poly-tannic acid coated paclitaxel nanocrystals for combinational photothermal-chemotherapy. Colloids Surf B 197:111377
Salazar J, Ghanem A, Müller RH, Möschwitzer JP (2012) Nanocrystals: comparison of the size reduction effectiveness of a novel combinative method with conventional top-down approaches. European J Pharm Biopharm 81(1):82–90
Trivedi V, Ajiboye AL (2023) Supercritical fluids: a promising technique in pharmaceutics. Nano-and microfabrication techniques in drug delivery: recent developments and future prospects. Springer, p 295–320
Kalaydina RV, Bajwa K, Qorri B, Decarlo A, Szewczuk MR (2018) Recent advances in “smart” delivery systems for extended drug release in cancer therapy. Int J Nanomed. 4727–4745
Lu Y, Lv Y, Li T (2019) Hybrid drug nanocrystals. Adv Drug Deliv Rev 143:115–133
Bae KH, Chung HJ, Park TG (2011) Nanomaterials for cancer therapy and imaging. Mol Cells 31:295–302
Kumari P, Ghosh B, Biswas S (2016) Nanocarriers for cancer-targeted drug delivery. J Drug Targeting 24(3):179–191
**ang H, Xu S, Li J, Li Y, Xue X, Liu Y, et al (2022) Functional drug nanocrystals for cancer-target delivery. J Drug Deliv Sci Technol 103807
Morales-Cruz M, Delgado Y, Castillo B, Figueroa CM, Molina AM, Torres A, et al (2019) Smart targeting to improve cancer therapeutics. Drug Des Develop Therapy. 3753–3772
Kumar M, Jha A, Dr M, Mishra B (2020) Targeted drug nanocrystals for pulmonary delivery: a potential strategy for lung cancer therapy. Expert Opin Drug Deliv 17(10):1459–1472
Ren X, Qi J, Wu W, Yin Z, Li T, Lu Y (2019) Development of carrier-free nanocrystals of poorly water-soluble drugs by exploring metastable zone of nucleation. Acta Pharm Sinica B 9(1):118–127
Luo Z, Lu L, Xu W, Meng N, Wu S, Zhou J et al (2022) In vivo self-assembled drug nanocrystals for metastatic breast cancer all-stage targeted therapy. J Control Release 346:32–42
Sultana S, Khan MR, Kumar M, Kumar S, Ali M (2013) Nanoparticles-mediated drug delivery approaches for cancer targeting: a review. J Drug Target 21(2):107–125
Zhang M, Gao S, Yang D, Fang Y, Lin X, ** X et al (2021) Influencing factors and strategies of enhancing nanoparticles into tumors in vivo. Pharmaceutica Sinica B 11(8):2265–2285
Wang Y, Rong J, Zhang J, Liu Y, Meng X, Guo H et al (2017) Morphology, in vivo distribution and antitumor activity of bexarotene nanocrystals in lung cancer. Drug Dev Ind Pharm 43(1):132–141
Zhang C, Long L, **ong Y, Wang C, Peng C, Yuan Y et al (2019) Facile engineering of indomethacin-induced paclitaxel nanocrystal aggregates as carrier-free nanomedicine with improved synergetic antitumor activity. ACS Appl Mater Interf 11(10):9872–9883
Bai M, Yang M, Gong J, Xu H, Wei ZJAP (2021) Progress and principle of drug nanocrystals for tumor targeted delivery. AAPS PharmSciTech 23(1):41
Calzoni E, Cesaretti A, Polchi A, Di Michele A, Tancini B, Emiliani C (2019) Biocompatible polymer nanoparticles for drug delivery applications in cancer and neurodegenerative disorder therapies. J Funct Biomater 10(1):4
Yetisgin AA, Cetinel S, Zuvin M, Kosar A, Kutlu O (2020) Therapeutic nanoparticles and their targeted delivery applications. Mol Cells 25(9):2193
Liu Y, Wang Y, Zhao J (2019) Design, optimization and in vitro-in vivo evaluation of smart nanocaged carrier delivery of multifunctional PEG-chitosan stabilized silybin nanocrystals. Int J Biol Macromol 124:667–680
Mao Y, Liu J, Shi T, Chen G, Wang S (2019) A novel self-assembly nanocrystal as lymph node-targeting delivery system: higher activity of lymph node targeting and longer efficacy against lymphatic metastasis. AAPS PharmSciTech 20:1–11
Alfaifi MY, Shati AA, Elbehairi SEI, Fahmy UA, Alhakamy NA, Md S (2020) Anti-tumor effect of PEG-coated PLGA nanoparticles of febuxostat on A549 non-small cell lung cancer cells. Biotech 10:1–10
**n Y, Huang Q, Tang J-Q, Hou X-Y, Zhang P, Zhang LZ et al (2016) Nanoscale drug delivery for targeted chemotherapy. Cancer Lett 379(1):24–31
He J, Li C, Ding L, Huang Y, Yin X, Zhang J et al (2019) Tumor targeting strategies of smart fluorescent nanoparticles and their applications in cancer diagnosis and treatment. Adv Mater 31(40):1902409
Danhier F, Feron O, Préat V (2010) To exploit the tumor microenvironment: passive and active tumor targeting of nanocarriers for anti-cancer drug delivery. J Control Release 148(2):135–146
Dutta B, Barick K, Hassan P (2021) Recent advances in active targeting of nanomaterials for anticancer drug delivery. Adv Coll Interf Sci 296:102509
Wang H, Liu Y, He R, Xu D, Zang J, Weeranoppanant N et al (2020) Cell membrane biomimetic nanoparticles for inflammation and cancer targeting in drug delivery. Biomaterials Sci 8(2):552–568
Kesharwani P, Chadar R, Sheikh A, Rizg WY, Safhi AY (2022) CD44-targeted nanocarrier for cancer therapy. Front Pharmacol 12:800481
Danhier F, Pourcelle V, Marchand-Brynaert J, Jérôme C, Feron O, Préat V (2012) Targeting of tumor endothelium by RGD-grafted PLGA-nanoparticles. Methods in enzymology. Elsevier, p 157–75.
Amreddy N, Babu A, Muralidharan R, Munshi A, Ramesh R (2018) Polymeric nanoparticle-mediated gene delivery for lung cancer treatment. Polymeric Gene Deliv Syst 233–255
Parakh S, Parslow AC, Gan HK, Scott AM (2016) Antibody-mediated delivery of therapeutics for cancer therapy. Expert Opin Drug Deliv 13(3):401–419
Rothdiener M, Beuttler J, Messerschmidt SK, Kontermann RE (2010) Antibody targeting of nanoparticles to tumor-specific receptors: immunoliposomes. Cancer Nanotechnol Methods Protocols. 295–308
Lee YT, Tan YJ, Oon CE (2018) Molecular targeted therapy: treating cancer with specificity. European J Pharmacol 834:188–196
Behrens LM, van den Berg TK, van Egmond M (2022) Targeting the CD47-SIRPα innate immune checkpoint to potentiate antibody therapy in cancer by neutrophils. Cancers 14(14):3366
Sarda S, Iafisco M, Pascaud-Mathieu P, Adamiano A, Montesi M, Panseri S et al (2018) Interaction of folic acid with nanocrystalline apatites and extension to methotrexate (antifolate) in view of anticancer applications. Langmuir 34(40):12036–12048
Steinhauser I, Spänkuch B, Strebhardt K, Langer K (2006) Trastuzumab-modified nanoparticles: optimisation of preparation and uptake in cancer cells. Biomaterials 27(28):4975–4983
Zhi D, Yang T, Yang J, Fu S, Zhang S (2020) Targeting strategies for superparamagnetic iron oxide nanoparticles in cancer therapy. Acta Biomater 102:13–34
Yang Z, Ma Y, Zhao H, Yuan Y, Kim BY (2020) Nanotechnology platforms for cancer immunotherapy. Wiley Interdiscip Rev Nanomed Nanobiotechnol 12(2):e1590
Jovčevska I, Muyldermans S (2020) The therapeutic potential of nanobodies. BioDrugs 34(1):11–26
Kunjiappan S, Pavadai P, Vellaichamy S, Ram Kumar Pandian S, Ravishankar V, Palanisamy P et al (2021) Surface receptor-mediated targeted drug delivery systems for enhanced cancer treatment: a state-of-the-art review. Drug Develop Res 82(3):309–340
Large DE, Soucy JR, Hebert J, Auguste DT (2019) Advances in receptor-mediated, tumor-targeted drug delivery. Adv Therapeut 2(1):1800091
Yousefi H, Vatanmakanian M, Mahdiannasser M, Mashouri L, Alahari NV, Monjezi MR et al (2021) Understanding the role of integrins in breast cancer invasion, metastasis, angiogenesis, and drug resistance. Oncogene 40(6):1043–1063
Kularatne SA, Low PS (2010) Targeting of nanoparticles: folate receptor. Cancer Nanotechnol Methods Protocols. 249–265
Yao VJ, D’Angelo S, Butler KS, Theron C, Smith TL, Marchiò S et al (2016) Ligand-targeted theranostic nanomedicines against cancer. J Control Release 240:267–286
Bae YH, Park K (2011) Targeted drug delivery to tumors: myths, reality and possibility. J Control Release 153(3):198–205
Li L, Liu Y, Wang J, Chen L, Zhang W, Yan X (2016) Preparation, in vitro and in vivo evaluation of bexarotene nanocrystals with surface modification by folate-chitosan conjugates. J Drug Deliv 23(1):79–87
Yusefi M, Soon MLK, Teow SY, Monchouguy EI, Neerooa BNHM, Izadiyan Z et al (2022) Fabrication of cellulose nanocrystals as potential anticancer drug delivery systems for colorectal cancer treatment. Int J Biol Macromol 199:372–385
Ančić D, Oršolić N, Odeh D, Tomašević M, Pepić I, Ramić S (2022) Resveratrol and its nanocrystals: a promising approach for cancer therapy? J Toxicology Appl Pharmacol 435:115851
Noh JK, Naeem M, Cao J, Lee EH, Kim M-S, Jung Y et al (2016) Herceptin-functionalized pure paclitaxel nanocrystals for enhanced delivery to HER2-postive breast cancer cells. Int J Pharm 513(1–2):543–553
Zhao J, Du J, Wang J, An N, Zhou K, Hu X et al (2021) Folic acid and poly (ethylene glycol) decorated paclitaxel nanocrystals exhibit enhanced stability and breast cancer-targeting capability. J ACS Appl Mater 13(12):14577–14586
Moghaddam AS, Khonakdar HA, Sarikhani E, Jafari SH, Javadi A, Shamsi M et al (2020) Fabrication of carboxymethyl chitosan nanoparticles to deliver paclitaxel for melanoma treatment. J ChemNanoMat 6(9):1373–1385
Haddad R, Alrabadi N, Altaani B, Li T (2022) Paclitaxel drug delivery systems: focus on nanocrystals’ surface modifications. J Polym 14(4):658
Sohn JS, Yoon DS, Sohn JY, Park JS, Choi JS (2017) Development and evaluation of targeting ligands surface modified paclitaxel nanocrystals. J Mater Sci Eng C 72:228–237
Park J, Sun B, Yeo Y (2017) Albumin-coated nanocrystals for carrier-free delivery of paclitaxel. J Control Release 263:90–101
Wang D, Wang Y, Zhao G, Zhuang J, Wu W (2019) Improving systemic circulation of paclitaxel nanocrystals by surface hybridization of DSPE-PEG2000. J Colloids Surf B Biointerf 182:110337
Gad SF, Park J, Park JE, Fetih GN, Tous SS, Lee W et al (2018) Enhancing docetaxel delivery to multidrug-resistant cancer cells with albumin-coated nanocrystals. J Mol Pharm 15(3):871–881
Cheng M, Liu Q, Gan T, Fang Y, Yue P, Sun Y et al (2021) Nanocrystal-loaded micelles for the enhanced in vivo circulation of docetaxel. J Mol 26(15):4481
Choi JS, Park JS (2017) Surface modification of docetaxel nanocrystals with HER2 antibody to enhance cell growth inhibition in breast cancer cells. J Colloids Surf B Biointerf 159:139–150
Wang J, Muhammad N, Li T, Wang H, Liu Y, Liu B et al (2020) Hyaluronic acid-coated camptothecin nanocrystals for targeted drug delivery to enhance anticancer efficacy. J Mol Pharm 17(7):2411–2425
Zhan H, Jagtiani T, Liang JF (2017) Biopharmaceutics. A new targeted delivery approach by functionalizing drug nanocrystals through polydopamine coating. European J Pharm Biopharm. 114:221–9.
Wang Z, Feng T, Zhou L, Jiang D, Zhang Y, He G et al (2020) Salinomycin nanocrystals for colorectal cancer treatment through inhibition of Wnt/β-catenin signaling. J Nanoscale 12(38):19931–19938
Hao L, Luan J, Zhang D, Li C, Guo H, Qi L et al (2014) Research on the in vitro anticancer activity and in vivo tissue distribution of Amoitone B nanocrystals. J Colloids Surf B Biointerf 117:258–266
Luo M, Sun H, Jiang Q, Chai Y, Li C, Yang B et al (2021) Novel nanocrystal injection of insoluble drug anlotinib and its antitumor effects on hepatocellular carcinoma. J Front Oncol 11:777356
Zhu Y, Fu Y, Zhang A, Wang X, Zhao Z, Zhang Y et al (2022) Rod-shaped nintedanib nanocrystals improved oral bioavailability through multiple intestinal absorption pathways. J European J Pharm Sci 168:106047
Ji P, Wang L, Chen Y, Wang S, Wu Z, Qi X (2020) Hyaluronic acid hydrophilic surface rehabilitating curcumin nanocrystals for targeted breast cancer treatment with prolonged biodistribution. J Biomater Sci 8(1):462–472
de Souza GD, Yukuyama MN, Miyagi MYS, Silva TJV, Lameu C, Bou-Chacra NA et al (2023) Revisiting flubendazole through nanocrystal technology: statistical design, characterization and its potential inhibitory effect on xenografted lung tumor progression in mice. J Cluster Sci 34(1):261–272
Park JE, Park J, Jun Y, Oh Y, Ryoo G, Jeong Y-S et al (2019) Expanding therapeutic utility of carfilzomib for breast cancer therapy by novel albumin-coated nanocrystal formulation. J Control Release 302:148–159
Liang P, Wu H, Zhang Z, Jiang S, Lv H (2020) Preparation and characterization of parthenolide nanocrystals for enhancing therapeutic effects of sorafenib against advanced hepatocellular carcinoma. Int J Pharm 583:119375
Lu Y, Qi J, Dong X, Zhao W, Wu W (2017) The in vivo fate of nanocrystals. Drug Discov Today 22(4):744–750
Baek M, Chung HE, Yu J, Lee JA, Kim TH, Oh JM, et al (2012) Pharmacokinetics, tissue distribution, and excretion of zinc oxide nanoparticles. Int J Nanomed. 3081–97.
Raj S, Khurana S, Choudhari R, Kesari KK, Kamal MA, Garg N, et al (2021) Specific targeting cancer cells with nanoparticles and drug delivery in cancer therapy. Seminars in cancer biology: Elsevier, p 166–77.
Lu Y, Chen Y, Gemeinhart RA, Wu W, Li T (2015) Develo** nanocrystals for cancer treatment. Nanomedicine 10(16):2537–2552
Sharma S, Verma A, Teja BV, Shukla P, Mishra PR (2015) Development of stabilized Paclitaxel nanocrystals: In-vitro and in-vivo efficacy studies. European J Pharmaceut Sci 69:51–60
Lv PP, Wei W, Yue H, Yang TY, Wang LY, Ma GH (2011) Porous quaternized chitosan nanoparticles containing paclitaxel nanocrystals improved therapeutic efficacy in non-small-cell lung cancer after oral administration. Biomacromol 12(12):4230–4239
Dong D, Wang X, Wang H, Zhang X, Wang Y, Wu B. Elucidating the in vivo fate of nanocrystals using a physiologically based pharmacokinetic model: a case study with the anticancer agent SNX-2112. Int J Nanomedicine. 2015:2521–35.
Ahire E, Thakkar S, Darshanwad M, Misra M (2018) Parenteral nanosuspensions: a brief review from solubility enhancement to more novel and specific applications. Acta Pharmaceutica Sinica B 8(5):733–755
McGuckin MB, Wang J, Ghanma R, Qin N, Palma SD, Donnelly RF et al (2022) Nanocrystals as a master key to deliver hydrophobic drugs via multiple administration routes. J Controlled Release 345:334–353
Bruce JY, Eickhoff J, Pili R, Logan T, Carducci M, Arnott J et al (2012) A phase II study of 2-methoxyestradiol nanocrystal colloidal dispersion alone and in combination with sunitinib malate in patients with metastatic renal cell carcinoma progressing on sunitinib malate. Invest New Drugs 30:794–802
Wang Y, Ma Y, Ma Y, Du Y, Liu Z, Zhang D et al (2012) Formulation and pharmacokinetics evaluation of puerarin nanocrystals for intravenous delivery. J Nanosci Nanotechnol 12(8):6176–6184
Lu Y, Wang ZH, Li T, McNally H, Park K, Sturek M (2014) Development and evaluation of transferrin-stabilized paclitaxel nanocrystal formulation. J Controlled Release;176:76–85.
Zhang H, Wang X, Dai W, Gemeinhart RA, Zhang Q, Li T (2014) Pharmacokinetics and treatment efficacy of camptothecin nanocrystals on lung metastasis. Mol Pharm 11(1):226–233
Huang ZG, Lv FM, Wang J, Cao SJ, Liu ZP, Liu Y et al (2019) RGD-modified PEGylated paclitaxel nanocrystals with enhanced stability and tumor-targeting capability. Int J Pharmaceut 556:217–225
Liu H, Ma Y, Liu D, Fallon JK, Liu F (2016) The effect of surfactant on paclitaxel nanocrystals: an in vitro and in vivo study. J Biomed Nanotechnol 12(1):147–153
Lugoloobi I, Maniriho H, Jia L, Namulinda T, Shi X, Zhao Y (2021) Cellulose nanocrystals in cancer diagnostics and treatment. J Controlled Release 336:207–232
Mahmoud KA, Mena JA, Male KB, Hrapovic S, Kamen A, Luong JH (2010) Effect of surface charge on the cellular uptake and cytotoxicity of fluorescent labeled cellulose nanocrystals. ACS Appl Mater Interf 2(10):2924–2932
Huh YM, Jun YW, Song HT, Kim S, Choi JS, Lee JH et al (2005) In vivo magnetic resonance detection of cancer by using multifunctional magnetic nanocrystals. J Am Chem Soc 127(35):12387–12391
Atapour A, Khajehzadeh H, Shafie M, Abbasi M, Mosleh-Shirazi S, Kasaee SR et al (2022) Gold nanoparticle-based aptasensors: a promising perspective for early-stage detection of cancer biomarkers. J Mater Today Commun 30:103181
**e Y, He W, Li F, Perera TSH, Gan L, Han Y et al (2016) Luminescence enhanced Eu3+/Gd3+ co-doped hydroxyapatite nanocrystals as imaging agents in vitro and in vivo. J ACS Appl Mater Interf 8(16):10212–10219
Sharma H, Mishra PK, Talegaonkar S, Vaidya B (2015) Metal nanoparticles: a theranostic nanotool against cancer. J Drug Discov Today 20(9):1143–1151
Wu L, Qu X (2015) Cancer biomarker detection: recent achievements and challenges. J Chem Soc Rev 44(10):2963–2997
Jun YW, Huh YM, Choi JS, Lee JH, Song HT, Kim S et al (2005) Nanoscale size effect of magnetic nanocrystals and their utilization for cancer diagnosis via magnetic resonance imaging. J Am Chem Soc 127(16):5732–5733
Cole AJ, Yang VC, David AE (2011) Cancer theranostics: the rise of targeted magnetic nanoparticles. J Trends Biotechnol 29(7):323–332
Xu JJ, Zhang WC, Guo YW, Chen XY, Zhang YN (2022) Metal nanoparticles as a promising technology in targeted cancer treatment. J Drug Deliv 29(1):664–678
Khursheed R, Dua K, Vishwas S, Gulati M, Jha NK, Aldhafeeri GM et al (2022) Biomedical applications of metallic nanoparticles in cancer: current status and future perspectives. J Biomed Pharmacother 150:112951
Farinha P, Coelho JM, Reis CP, Gaspar MM (2021) A comprehensive updated review on magnetic nanoparticles in diagnostics. J Nanomater 11(12):3432
Lorkowski ME, Atukorale PU, Ghaghada KB, Karathanasis E (2021) Stimuli-Responsive iron oxide nanotheranostics: a versatile and powerful approach for cancer therapy. J Adv Healthcare Mater 10(5):2001044
**ao L, Mertens M, Wortmann L, Kremer S, Valldor M, Lammers T et al (2015) Enhanced in vitro and in vivo cellular imaging with green tea coated water-soluble iron oxide nanocrystals. J ACS Appl Mater Interf 7(12):6530–6540
Gu L, Fang RH, Sailor MJ, Park J-H (2012) In vivo clearance and toxicity of monodisperse iron oxide nanocrystals. J ACS Nano 6(6):4947–4954
Ma X, Gong A, Chen B, Zheng J, Chen T, Shen Z et al (2015) Exploring a new SPION-based MRI contrast agent with excellent water-dispersibility, high specificity to cancer cells and strong MR imaging efficacy. J Colloids Surf B Biointerf 126:44–49
Shahbazi-Gahrouei D, Abdolahi M (2013) Detection of MUC1-expressing ovarian cancer by C595 monoclonal antibody-conjugated SPIONs using MR imaging. J Sci World J
Vellingiri S, Rejeeth C, Varukattu NB, Sharma A, Kumar RS, Almansour AI et al (2022) In vivo delivery of nuclear targeted drugs for lung cancer using novel synthesis and functionalization of iron oxide nanocrystals. New J Chem 46(26):12488–12499
Sreevani V, Shanthi K, Kannan S (2013) Goat red blood cells as precursor for iron oxide nanocrystal synthesis to develop nuclear targeted lung cancer therapy. J Mater Res Bulletin 48(9):3164–3171
Armijo LM, Brandt YI, Mathew D, Yadav S, Maestas S, Rivera AC et al (2012) Iron oxide nanocrystals for magnetic hyperthermia applications. J Nanomater 2(2):134–146
Li Y, Ma X, Liu X, Yue Y, Cheng K, Zhang Q et al (2022) Redox-responsive functional iron oxide nanocrystals for magnetic resonance imaging-guided tumor hyperthermia therapy and heat-mediated immune activation. J ACS Appl Nano Mater 5(3):4537–4549
Lin G, Zhu W, Yang L, Wu J, Lin B, Xu Y et al (2014) Delivery of siRNA by MRI-visible nanovehicles to overcome drug resistance in MCF-7/ADR human breast cancer cells. J Biomater 35(35):9495–9507
Wiesmann N, Tremel W, Brieger J (2020) Zinc oxide nanoparticles for therapeutic purposes in cancer medicine. J Mater Chem B 8(23):4973–4989
Pandurangan M, Kim DH (2015) In vitro toxicity of zinc oxide nanoparticles: a review. J Nanopart Res 17:1–8
Mishra PK, Mishra H, Ekielski A, Talegaonkar S, Vaidya B (2017) Zinc oxide nanoparticles: a promising nanomaterial for biomedical applications. J Drug Discovery Today 22(12):1825–1834
Racca L, Limongi T, Vighetto V, Dumontel B, Ancona A, Canta M et al (2020) Zinc oxide nanocrystals and high-energy shock waves: a new synergy for the treatment of cancer cells. J Front Bioeng Biotechnol 8:577
Garino N, Limongi T, Dumontel B, Canta M, Racca L, Laurenti M et al (2019) A microwave-assisted synthesis of zinc oxide nanocrystals finely tuned for biological applications. J Nanomater 9(2):212
Dumontel B, Canta M, Engelke H, Chiodoni A, Racca L, Ancona A et al (2017) Enhanced biostability and cellular uptake of zinc oxide nanocrystals shielded with a phospholipid bilayer. J Mater Chem B 5(44):8799–8813
Dumontel B, Susa F, Limongi T, Canta M, Racca L, Chiodoni A et al (2019) ZnO nanocrystals shuttled by extracellular vesicles as effective Trojan nano-horses against cancer cells. J Nanomed 14(21):2815–2833
Sasidharan A, Chandran P, Menon D, Raman S, Nair S, Koyakutty M (2011) Rapid dissolution of ZnO nanocrystals in acidic cancer microenvironment leading to preferential apoptosis. J Nanoscale 3(9):3657–3669
Gu B, Pliss A, Kuzmin AN, Baev A, Ohulchanskyy TY, Damasco JA et al (2016) In-situ second harmonic generation by cancer cell targeting ZnO nanocrystals to effect photodynamic action in subcellular space. J Biomater 104:78–86
Sharma H, Kumar K, Choudhary C, Mishra PK, Vaidya B (2016) Development and characterization of metal oxide nanoparticles for the delivery of anticancer drug. J Artif Cells Nanomed Biotechnol 44(2):672–679
Anjum S, Hashim M, Malik SA, Khan M, Lorenzo JM, Abbasi BH et al (2021) Recent advances in zinc oxide nanoparticles (ZnO NPs) for cancer diagnosis, target drug delivery, and treatment. J Cancers 13(18):4570
Patra JK, Das G, Fraceto LF, Campos EVR, Rodriguez-Torres MdP, Acosta-Torres LS et al (2018) Nano based drug delivery systems: recent developments and future prospects. J Nanobiotechnol 16(1):1–33
Wang D, Xu Z, Yu H, Chen X, Feng B, Cui Z et al (2014) Treatment of metastatic breast cancer by combination of chemotherapy and photothermal ablation using doxorubicin-loaded DNA wrapped gold nanorods. J Biomater 35(29):8374–8384
Al-Sagheer L, Alshahrie A, Mahmoud WE (2021) Facile approach for develo** gold nanorods with various aspect ratios for an efficient photothermal treatment of cancer. Colloids Surf, A 618:126394
Yang X, Liu Y, Zhao Y, Han M, Guo Y, Kuang H, et al (2016) A stabilizer-free and organic solvent-free method to prepare 10-hydroxycamptothecin nanocrystals: in vitro and in vivo evaluation. Int J Nanomed 2979–2994
Shen N, Zhang R, Zhang H-R, Luo H-Y, Shen W, Gao X et al (2018) Inhibition of retinal angiogenesis by gold nanoparticles via inducing autophagy. Int J Ophthalmol 11(8):1269
Li W, Zhao X, Du B, Li X, Liu S, Yang X-Y et al (2016) Gold nanoparticle–mediated targeted delivery of recombinant human endostatin normalizes tumour vasculature and improves cancer therapy. J Sci Rep 6(1):30619
Wang H, Zhu W, Huang Y, Li Z, Jiang Y, **e Q (2017) Facile encapsulation of hydroxycamptothecin nanocrystals into zein-based nanocomplexes for active targeting in drug delivery and cell imaging. J Acta Biomaterialia 61:88–100
Chanda N, Upendran A, Boote EJ, Zambre A, Axiak S, Selting K et al (2014) Gold nanoparticle based X-ray contrast agent for tumor imaging in mice and dog: a potential nanoplatform for computer tomography theranostics. J Biomed Nanotechnol 10(3):383–392
Menon D, Basanth A, Retnakumari A, Manzoor K, Nair SV (2012) Green synthesis of biocompatible gold nanocrystals with tunable surface plasmon resonance using garlic phytochemicals. J Biomed Nanotechnol 8(6):901–911
Lee SH, Jun B-H (2019) Silver nanoparticles: synthesis and application for nanomedicine. Int J Mol Sci 20(4):865
Chugh H, Sood D, Chandra I, Tomar V, Dhawan G, Chandra R (2018) Role of gold and silver nanoparticles in cancer nano-medicine. J Artif Cells Nanomed Biotechnol 46(sup1):1210–1220
Muhammad N, Zhao H, Song W, Gu M, Li Q, Liu Y et al (2020) Silver nanoparticles functionalized Paclitaxel nanocrystals enhance overall anti-cancer effect on human cancer cells. J Nanotechnol 32(8):085105
Zhan H, Zhou X, Cao Y, Jagtiani T, Chang T-L, Liang JF (2017) Anti-cancer activity of camptothecin nanocrystals decorated by silver nanoparticles. J Mater Chem B 5(14):2692–2701
Han JW, Gurunathan S, Choi YJ, Kim JH (2017) Dual functions of silver nanoparticles in F9 teratocarcinoma stem cells, a suitable model for evaluating cytotoxicity-and differentiation-mediated cancer therapy. Int J Nanomed. 7529–7549
Arockia John Paul J, Karunai Selvi B, Karmegam N (2015) Biosynthesis of silver nanoparticles from Premna serratifolia L. leaf and its anticancer activity in CCl 4-induced hepato-cancerous Swiss albino mice. J Appl Nanosci 5:937–944
Nima ZA, Mahmood M, Xu Y, Mustafa T, Watanabe F, Nedosekin DA et al (2014) Circulating tumor cell identification by functionalized silver-gold nanorods with multicolor, super-enhanced SERS and photothermal resonances. J Sci Rep 4(1):4752
Thambiraj S, Shruthi S, Vijayalakshmi R, Shankaran DR (2019) Evaluation of cytotoxic activity of docetaxel loaded gold nanoparticles for lung cancer drug delivery. J Cancer Treat Res Commun 21:100157
Ding J, Chen G, Chen G, Guo M (2019) One-pot synthesis of epirubicin-capped silver nanoparticles and their anticancer activity against hep G2 cells. J Pharm 11(3):123
Chen W, Yang W, Chen P, Huang Y, Li F (2018) Disulfiram copper nanoparticles prepared with a stabilized metal ion ligand complex method for treating drug-resistant prostate cancers. J ACS Appl Mater Interf 10(48):41118–41128
Pan UN, Khandelia R, Sanpui P, Das S, Paul A, Chattopadhyay A (2017) Protein-based multifunctional nanocarriers for imaging, photothermal therapy, and anticancer drug delivery. J ACS Appl Mater Interf 9(23):19495–19501
Muhammad Z, Raza A, Ghafoor S, Naeem A, Naz SS, Riaz S et al (2016) PEG capped methotrexate silver nanoparticles for efficient anticancer activity and biocompatibility. J European J Pharm Sci 91:251–255
Ahmed KBA, Mahapatra SK, Raja MRC, Subramaniam S, Sengan M, Rajendran N et al (2016) Jacalin-capped silver nanoparticles minimize the dosage use of the anticancer drug, shikonin derivatives, against human chronic myeloid leukemia. J RSC Adv 6(23):18980–18989
Mohanty RK, Thennarasu S, Mandal AB (2014) Resveratrol stabilized gold nanoparticles enable surface loading of doxorubicin and anticancer activity. J Colloids Surf B Biointerf 114:138–143
Autio KA, Dreicer R, Anderson J, Garcia JA, Alva A, Hart LL et al (2018) Safety and efficacy of BIND-014, a docetaxel nanoparticle targeting prostate-specific membrane antigen for patients with metastatic castration-resistant prostate cancer: a phase 2 clinical trial. J JAMA Oncol 4(10):1344–1351
Ramanathan RK, Korn RL, Raghunand N, Sachdev JC, Newbold RG, Jameson G et al (2017) Correlation between ferumoxytol uptake in tumor lesions by MRI and response to nanoliposomal irinotecan in patients with advanced solid tumors: a pilot study. J Clin Cancer Res 23(14):3638–3648
Malik R, Patil S (2020) Nanotechnology: regulatory outlook on nanomaterials and nanomedicines in United States, Europe and India. Appl Clin Res Clin Trials Regul Aff 7(3):225–236
Mühlebach S (2018) Regulatory challenges of nanomedicines and their follow-on versions: a generic or similar approach? Adv Drug Deliv Rev 131:122–131
Acknowledgements
The authors would like to acknowledge Charotar University of Science and Technology (CHARUSAT) for the support.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
VP conceptualized the work; AP, KP and VP wrote the manuscript; MSR and RP critiqued the manuscript; AR formatted the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Authors provide consent for publication in Future Journal of Pharmaceutical Sciences.
Competing interests
Authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Patel, A., Patel, K., Patel, V. et al. Nanocrystals: an emerging paradigm for cancer therapeutics. Futur J Pharm Sci 10, 4 (2024). https://doi.org/10.1186/s43094-024-00579-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43094-024-00579-4