Abstract
The use of nanomaterials in gene editing and synthetic biology has emerged as a pivotal strategy in the pursuit of refined treatment methodologies for pulmonary disorders. This review discusses the utilization of nanomaterial-assisted gene editing tools and synthetic biology techniques to promote the development of more precise and efficient treatments for pulmonary diseases. First, we briefly outline the characterization of the respiratory system and succinctly describe the principal applications of diverse nanomaterials in lung ailment treatment. Second, we elaborate on gene-editing tools, their configurations, and assorted delivery methods, while delving into the present state of nanomaterial-facilitated gene-editing interventions for a spectrum of pulmonary diseases. Subsequently, we briefly expound on synthetic biology and its deployment in biomedicine, focusing on research advances in the diagnosis and treatment of pulmonary conditions against the backdrop of the coronavirus disease 2019 pandemic. Finally, we summarize the extant lacunae in current research and delineate prospects for advancement in this domain. This holistic approach augments the development of pioneering solutions in lung disease treatment, thereby endowing patients with more efficacious and personalized therapeutic alternatives.

Similar content being viewed by others
Introduction
Pulmonary diseases have persistently presented formidable hurdles for public health and healthcare systems [1, 2]. The intricate physiology of the respiratory system renders the targeting of damaged lungs arduous in conventional therapies [3,4,5]. This underscores the urgent need for innovative strategies to manage lung disease. In this context, drug delivery using nanocarriers is a potentially effective way to avoid conventional therapeutic limitations. Simultaneously, the evolution of advanced biomedical technologies, namely gene editing and synthetic biology, has the potential to augment drug bio-dispersibility and efficacy within target organs, reduce undesired side effects, and unlock novel avenues for enhancing the spectrum of lung disease management [6, 7].
Nanotechnology, an interdisciplinary field spanning physics, chemistry, and biology, offers innovative pathways for addressing biomedical challenges by designing, controlling, and manipulating materials and structures at the nanoscale [8]. In lung disease treatment, nanomaterials are a flexible platform for precise administration of drugs and targeted administration of gene-editing tools, supporting cellular engineering [9,10,11]. Gene editing has become a focal point in precise genetic modification technology [12]. Notably, the Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR)/ associated protein (Cas)9 system has revolutionized the field of gene editing due to its remarkable efficacy and simplicity. It involves the knockout, insertion, and mutational target genes modification using the Cas9 nucleic acid endonuclease and a single-stranded guide RNA (sgRNA) that targets the gene of interest [13, 14]. With this technology, genome editing is performed with high precision, enabling the study of the relationship between genes and biological traits and treating diseases such as genetic disorders and cancer. Nevertheless, gene-editing tools require precise guidance to effectively modify lung cells, which poses considerable challenges. The emergence of nanomaterials presents a new methodology to address this challenge [15, 16], which involves the utilization of nano-delivery systems to correctly convey gene-editing tools to specific lung cells, consequently reducing unintended effects on the surrounding tissues [17].
Synthetic biology constitutes a design-centric discipline, with its core focus on conceiving novel biological functionalities by discovering, characterizing, and repurposing molecular components [18,19,20]. In this context, microorganisms can be systematically engineered and tailored through synthetic biological methodologies to enable the production of specific pharmaceutical compounds or serve as active therapeutic agents in the context of lung disease treatment [21,22,23]. Furthermore, based on the design principles and engineering framework intrinsic to synthetic biology, mammalian cells can be modified to manifest specific functionalities, including those relevant to organ transplantation, cell-based therapies, and vaccine production [24]. Synthetic biology provides broad applications, including vaccine development for lung diseases, molecular diagnostics, and cell-based therapeutic interventions. However, synthetic biology faces several technical and ethical challenges as a cutting-edge technology in life sciences while bringing benefits and visions to human society. Synthetic biology requires a very high level of understanding of biological fundamentals. Scientists need a comprehensive understanding of a biological system’s structure and function to accurately design and construct new biological systems [25]. At the same time, synthetic biology is concerned with the nature of life and the design of living organisms, raising discussions about bioethics and biodiversity conservation. In addition, the accidental release or deliberate misuse of synthetic organisms may lead to unknown biosafety risks [26]. Therefore, while encouraging its development, there is a need to strengthen relevant safety regulations and ethical constraints so that the potential of synthetic biology can be maximized while reducing the risks it poses.
Here, we highlight the potential of nanomaterials to enhance gene editing and synthetic biology, as well as present innovative approaches for lung disease treatment. Firstly, an overview of the respiratory system and limitations of present treatments for pulmonary disorders are briefly described. The application of nano-delivery systems in pulmonary diseases is also reviewed, along with insights into the rationale underlying the nano-delivery systems design for pulmonary therapy. Secondly, we outline the application of nanomaterial-assisted gene editing and synthetic biology in develo** novel therapies for pulmonary diseases. Finally, we propose the prospects for utilizing these techniques for lung disease treatment and their possible clinical applications.
Respiratory system overview
The efficacy of pulmonary therapy is hindered by respiratory physiology [27]. The upper respiratory system, which encompasses the nose, mouth, pharynx, and larynx, regulates lung-bound airflow and filters the incoming air [28]. The lower respiratory tract, which comprises the trachea and lungs, is a complicated network of branching airways characterized by a bronchial tree interlinked with the alveolar system. This intricate structure presents a multitude of barriers that shield the lungs from potential environmental hazards [29], particularly relevant are the airways host mucus and cilia, which constitute a physical barrier that intercepts particulate matter and microorganisms from lung entry [30]. While mucus traps irritants or inhaled substances, the coordinated motion of cilia propels mucus out of the lungs, maintaining lung hygiene [31]. Meanwhile, in obstructive lung diseases, the thickening of the mucus layer due to bronchoconstriction and increased mucus secretion disrupts the drug delivery mechanism [32].
When the delivered drug avoids mucosal ciliary clearance, it effectively engages with the target tissue; however, the intricate pulmonary environment, replete with various compounds, such as surfactants and protein hydrolases, presents obstacles, limits drug adsorption, and triggers its deactivation [33]. Alveolar surfactants comprise lipids and proteins that interact with drugs or particles [34]. Consequently, they can encase the drug with protein crowns, thwart adsorption, and expedite its elimination by alveolar macrophages. Furthermore, the pulmonary arena hosts an array of immune cells and molecules, including macrophages, lymphocytes, and immunoglobulins. These entities can phagocytose and degrade biological macromolecules and particles [35]. Notably, heightened macrophage activity is crucial in the pathogenesis of specific pulmonary diseases such as infection, acute lung injury, and chronic obstructive pulmonary disease (COPD) [36]. In summary, insights into the characterization of the lung barrier could promote the development of more effective lung therapies. Nanomaterial-based therapy is a promising alternative to traditional treatments with limited effectiveness in delivering drugs to the lungs [37, 38]. Nanomaterials have nanoscale dimensions and move more freely in the body. In addition, nano-delivery systems can enhance the stability of therapeutic agents, including DNA and RNA, to protect against early degradation and rapid clearance in vivo [39]. This allows the drug formulation to be delivered to the target region, enabling precise drug control, reducing toxic side effects, controlling biodistribution, and accelerating drug action or response. Several nanomaterials are available to deliver gene editing tools, offering potential solutions for treating lung diseases.
Nano-delivery system for pulmonary diseases treatment
Nano-delivery system
Nanotechnology in medicine offers new treatment strategies for lung disease [40]. Nanomedicine refers to the use of nanotechnology in healthcare and related research for supervising, regulating, constructing, repairing, protecting, and enhancing biological systems at the molecular level [41]. Nanotechnology has many unique physicochemical properties due to the quantum effects of materials at the nanoscale, which provide unlimited possibilities for the preparation, performance, improvement, and application of nanoscale products [42]. Within this framework, nano-delivery systems present a viable means of transporting drugs or messenger ribonucleic acid (mRNA) to a specific target [43, 44]. Nanomaterials can function as carriers to facilitate the delivery of diagnostic agents.
Nanomaterials offer a compelling avenue for develo** controlled-release delivery systems suitable for the pulmonary environment [45]. Their small scale of nanomaterials imparts novel functionalities to nanomedicine [46]. Specifically, nanocarriers enhance the stability of active agents during transport, safeguarding them from extracellular enzymes and evading scavenging systems [47]. These carriers facilitate the cellular uptake of active compounds and enable their controlled and targeted delivery with uniform distribution, thereby extending the retention time within the target tissue and mitigating adverse effects through protective shielding [48]. Collectively, these attributes synergistically enhance the pharmacokinetics and pharmacodynamics of active compounds. Furthermore, a diverse array of nanomaterials is already being used to overcome the limitations of lung therapies. The substantial absorption, extensive circulation, and permeability of the lungs promote nanoparticles (NPs) accumulation in the airways and lungs [49]. These unique characteristics make nanomaterials potential tools for lung therapy.
Types of nano-delivery systems
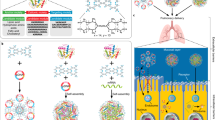
With the rapid advancements in biomaterials, nanocarriers designed for enhanced delivery, including lipids [50,51,52], polymers [53], inorganic NPs (INPs) [54], and other nanomaterials [55], have demonstrated substantial potential. The nanocarrier size is an key parameter that affects its deposition in the lungs (Fig. 1). The aerodynamic diameter (AD) represents the size of the atomized particles, which determines the region of the respiratory system where particle deposition occurs. Additionally, selecting delivery carrier strategies must consider three crucial aspects: biosafety, delivery efficiency, and target specificity [56]. To ensure biosafety, it is imperative to select carriers that exhibit biocompatibility and minimal immunogenicity [57]. Furthermore, the chosen carrier must be able to facilitate targeted therapy within the lungs while surmounting inherent biological and physical pulmonary barriers [58]. These include enhancing drug solubility and extending the duration of drug retention, thereby optimizing therapeutic outcomes.
Lipid-based nanomaterials
Lipid-based nanomaterials are nanoparticle carriers prepared using biodegradable synthetic lipid molecules that can carry, deliver, and release hydrophobic and lipophilic preparations [59]. Depending on their nanostructure and lipid source, these materials can be categorized into liposomes, lipid NPs (LNPs), and other carriers. Initially discovered by Bangham in 1965, liposomes exhibit biocompatibility and low toxicity as their composition resembles cell membranes and lung surfactants. Their lipid-like nature facilitates the traversal of biological barriers and enhances absorption [60, 61].
Liposomes come in different forms. Multilamellar vesicles have multiple lipid bilayers and are 500–5,000 nm in size [62]. Single lipid bilayer unilamellar vesicles ranging in size from 100 to 800 nm [63]. Long-circulating liposomes are strategically engineered with surface polymers to bolster their circulatory stability, whereas immunoliposomes equipped with antibody coatings attain precision in targeting specific cell types. The key advantages of liposomes over conventional therapies include drug protection against degradation, precise drug and macromolecule targeting, and reduced drug cytotoxicity [59, 64]. Notably, liposomes serve as prominent carriers in cancer therapy, and Doxil® was the first polyethylene glycol (PEG)-modified long-circulating liposome approved by the Food and Drug Administration (FDA) for cancer therapy in 1995 [42, 43, 65,66,67]. Liposomes encapsulate diverse drugs, including antibiotics, bronchodilators, immunosuppressants, anticancer agents, sex hormones, peptides, proteins, and oligonucleotides [68]. Despite their established application in clinical drug delivery, liposomes exhibit reduced delivery efficiency compared with viral vectors [69]. This phenomenon arises mainly from the multifaceted challenges that liposomes encounter upon interacting with cellular membranes, including factors such as membrane mass, charge, and liposome stability. Furthermore, efficient drug release from the liposomal interior is a potential compromise since the drug must traverse the lipid bilayer to access the cell. Researchers have consistently explored novel methodologies and techniques to augment the efficiency of liposomal delivery. Notably, enhancing liposome composition, dimensions, and surface characteristics enhances cellular interactions. Moreover, optimizing liposomal drug delivery efficacy can be further enhanced through strategic amalgamation with other modalities, such as targeted ligands and facilitated delivery systems.
Advances in nanotechnology have spurred the transformation of liposomes into versatile LNPs. Cationic liposomes are positively charged and can adsorb negatively charged nucleic acids or proteins through electrostatic interaction [70, 71]. Cellular internalization is expedited by endocytosis. This promotes the role of liposomes in the delivery of drugs, genes, and various biomolecules. Unlike viral vectors, cationic lipid liposomes offer distinct advantages such as mitigated off-target effects, reduced immunogenicity, enhanced biocompatibility, and elevated cargo capacity [72, 73]. Nevertheless, an overabundance of cationic lipids or imbalanced cation-nucleic acid ratios warrants attention, as these can precipitate cytotoxicity. Additionally, serum proteins may affect transfection efficiency, while the cationic lipid-deoxyribonucleic acid (DNA) complexes stability is diminished [74].
The emergence of ionizable lipids was a pivotal advancement in the develo** LNPs [75]. The polarity of ionizable liposomes undergoes pH-dependent alterations. Under acidic conditions, ionizable liposomes adopt a positive charge that enables the formation of mRNA complexes that serve as mRNA stabilizers but assume a neutral charge at physiological pH, which mitigates their potential toxicity [76]. Furthermore, the fusion of zwitterionic liposomes possessing low apparent charges with cationic liposomes can bolster the stabilization of the nanocarriers within the extra-cellular environment and heighten the load efficiency [77]. Miller et al. innovatively synthesized amphoteric amino lipids [163]. In addition, the stable presence of nanomaterials in circulation and their ability to accumulate at specific sites in vivo could enhance the therapeutic effects of CRISPR gene-edited drugs. Yan et al. used a complex of the cationic polymer poly(β-amino ester) (PBAE) with a plasmid encoding the CRISPR system at the core, combining targeted delivery and conditional activation of CRISPR-Cas9 for precision therapy of inflammatory bowel disease [Pneumonia Pneumonia is a pulmonary disease primarily triggered by pathogens including bacteria, viruses, fungi, and other microorganisms. Although antibiotics and antiviral agents play pivotal roles in its treatment, the generation of drug-resistant strains and intricacies of the disease underscore the need for novel therapeutic modalities [202, 203]. In recent years, the amalgamation of nanomaterials using gene editing technologies has ushered in novel prospects for pneumonia treatment. The outbreak of SARS-CoV-2 has expedited mRNA vaccine development by researchers worldwide, marking an important milestone in nanotechnology-based gene delivery from fundamental research to clinical applications. The FDA approved two mRNA vaccines from Moderna and BioNTech/Pfizer Pharmaceuticals for the prevention of coronavirus disease 2019 (COVID-19) [204]. Notably, both mRNA vaccines use LNPs as carriers for therapeutic genes [205]. However, although LNPs have achieved remarkable success as gene carriers [206], storing them for extended periods presents a challenging problem for clinical applications. Various long-term storage conditions for encapsulated mRNA LNPs have been investigated, and the stability of LNPs has been assessed by different cryoprotectant concentrations, such as mannitol, alginate, or sucrose. It was shown that adding alginate or sucrose (5%, w/v) to LNPs improves mRNA delivery efficiency for approximately three months [5A). The ability of SORT LNPs to co-deliver Cas9 mRNA and sgRNA as well as deliver Cas9 RNPs was experimentally verified, successfully realizing organ-selective gene editing. ReCode Therapeutics, a clinical-stage gene therapy company, announced that its inhaled mRNA therapeutic programs based on SORT LNPs technology, RCT1100 and RCT2100, had entered clinical trials for the treatment of primary ciliary dyskinesia (PCD) and cystic fibrosis (CF). In an efficacy validation study using a PCD model based on human bronchial epithelial (hBE) cells, SORT LNP-formulated DNAI1 mRNA delivered as an aerosol successfully rescued ciliary function for weeks after the last treatment. These data suggest that the SORT LNP delivery platform offers new approaches to gene therapy for rare and common genetic diseases. In addition, Dahlman et al. designed LNPs for effective drug delivery and effectively targeted delivery of therapeutic mRNAs to the lungs by nebulizing the LNPs [209]. The authors optimized the composition, molar ratio, and structure of LNPs made from lipids, helper lipids, and PEG, and investigated the in vivo workflow of LNPs for mRNA delivery to the lungs after nebulization (Fig. 5B). The optimal ratio of nebulized lung delivery 1 (NLD1) vectors was screened; they can be used to target mRNAs delivering a broad range of neutralizing antibodies to protect mice from the lethal challenge of H1N1 influenza. (A) SORT-LNP prepared by adding different SORT molecules to traditional LNP for targeting different organs [208]. (B) LNPs optimization for delivery of nebulized therapeutic mRNA to the lungs [209]. (a) Optimizing LNP-targeted lung delivery. (b) Mole ratio of NLD1 components. (c) Expression of NLD1 carrying AncNanoLuc mRNA in different tissues of mice. (d) Survival of H1V1-injected mice treated with NLD1 was 100%. Reprinted with permission from Ref [208, 209] Polymer NPs have been employed in gene therapy for lung diseases. For example, poly (β-amino ester) was combined with PEG-lipids to obtain an mRNA carrier with stability and good efficacy. By intravenous injection, the carrier was able to successfully deliver mRNA to the lungs of mice and the efficacy of degradable lipid polymer NPs for systemic mRNA delivery was confirmed [210, 211]. In addition, macrophage-specific gene editing was achieved using CRISPR/Cas9 components delivered by PEG-b-PLGA-based cationic lipid-assisted NPs [212, 213]. In addition to acting as gene carriers and targeting agents, NPs play a pivotal role in facilitating gene editing techniques to investigate resistance against pneumonia pathogens. Precise genetic modification of these pathogens can effectively mitigate or eliminate their resistance to antibiotics. Moreover, NPs are widely recognized as valuable tools for enhancing antimicrobial agents’ delivery. Specifically, NPs leverage two primary mechanisms to combat bacteria effectively: (i) the disruption of membrane potential and integrity and (ii) the induction of oxidative stress via nanoparticle-catalyzed reactive oxygen species production. These mechanisms operate both independently and synergistically [214]. CRISPR/Cas system is an effective tool to control antibiotic-resistance gene prevalence in bacteria and to eradicate pathogens with remarkable precision. For instance, Klebsiella pneumoniae often develops resistance to antibiotics, such as mucin and tigecycline, owing to chromosomal gene mutations [230]. Gene therapy has shown promise in clinical trials for treating CF [230]. Advances in gene therapy delivery mechanisms can provide valuable insights into the refinement of gene-editing delivery systems. For instance, Bao et al. developed an Au-based non-viral nanocarrier protamine sulfate stabilized Au NPs (AuPS)@pDNA for delivery of HGF pDNA into mesenchymal stem cells (MSCs) to improve the therapeutic efficacy of idiopathic pulmonary fibrosis (IPF). Meanwhile, as an effective CT contrast agent, it helps to elucidate the mechanism of transplanted MSCs for the treatment of IPF (Fig. 6A). This study synthesized PS-stabilized Au-based nano-delivery carriers (AuPS). HGF is a pleiotropic cytokine with promising anti-fibrotic effects and thus was delivered as a therapeutic gene into MSCs. Such engineered MSCs integrating therapy and visualization are expected to be used as novel therapeutic reagents in IPF treatment [231]. Bai et al. developed an inhalable NPs self-assembled from biodegradable PLGA-PEG copolymer and cationic lipid G0-C14, which could effectively deliver siIL11@PPGC NPs locally to the lungs of fibrotic mice, enabling the treatment of pulmonary fibrosis and significant improvement of lung function (Fig. 6B) [232]. Currently, gene manipulation techniques and molecular targets are being explored. The CRISPR/Cas9 technology for genome editing has substantial potential but remains in the nascent stages of development. In 2013, Schwank et al. achieved successful repair of the F508 mutation within the CFTR gene in intestinal stem cell-like organoids derived from CF patients through the utilization of the CRISPR/Cas9 system [233]. Subsequently, the viability of applying CRISPR/Cas9 technology to cystic fibrosis was firmly established. In summary, CRISPR/Cas9 systems offer significant potential as genome-editing strategies, demonstrating their ability to achieve specific and functional correction of mutant CFTRs in vitro [234]. Nevertheless, the translation of these strategies into clinical practice remains a distant goal, necessitating further research and optimization efforts.
Synthetic biology in the treatment of pulmonary diseases
Building new biological systems based on known biological systems to help humankind solve many problems in nature and social sciences has been a pursued goal. With the genomics revolution and the rise of systems biology in the 1990s, synthetic biology was developed to create, control, and program cellular behavior, and has become a major international scientific frontier [235]. As an avant-garde interdisciplinary domain, synthetic biology draws from numerous fields, including life sciences, engineering, genomics, informatics, mathematics, chemistry, and computer science [18]. Synthetic biology holds great promise for diverse applications in medicine, energy, materials, chemicals, and agriculture.
The development of synthetic biology
The origins of synthetic biology lie in the early 1960s when Jacob and Monod made groundbreaking discoveries on the regulation of lac operons in E. coli, an achievement that earned them the Nobel Prize [236]. The authors found that a protein known as a transcription factor can bind to the promoter region of a gene, thereby regulating its synthesis rate by activating or repressing it. This paves the way for viewing gene expression as a dynamic system with recognizable inputs and outputs. This concept holds promise for combining input and output systems to construct more intricate functionalities [237]. Since the late 1960s, progress in biotechnology has bestowed the scientific community with cost-effective and temporally efficient tools for DNA extraction, sequencing, amplification, and integration of exogenous DNA elements into cells. The advent of molecular cloning and polymerase chain reaction (PCR) techniques in the 1970s and the 1980s made genetic manipulation common in microbiological research. In recognition of their pioneering work on restriction endonucleases, pivotal components of DNA synthesis, Smith, Arber, and Nathans were awarded the Nobel Prize in 1978 [238]. This recognition began a new biotechnological era, allowing the description and analysis of existing genes as well as the construction and evaluation of novel gene arrangements. Nevertheless, in the pre-genomic period, research methods categorized as genetic engineering were primarily confined to cloning and recombinant gene expression. In essence, the field of genetic engineering lacked the requisite knowledge and tools to engineer biological systems that could exhibit the diversity and intricacy of regulatory behaviors inherent in microorganisms [239, 240].
By the mid-1990s, the emergence of automated DNA sequencing and improvements in computational tools have facilitated the sequencing of entire microbial genomes [241]. As biologists and computer scientists embarked on a collaborative journey to reverse engineer cellular networks, the expanding confluence of molecular biology gave birth to the field of systems biology. In 2016, a consortium of prominent scientists proposed an ambitious synthetic biology endeavor known as the Human Genome Writing Project. This initiative leverages synthetic biology tools encompassing standardized genes, whole-genome synthesis, and CRISPR/Cas9 gene editing to craft new genomes on a substantial scale. The proposal and the emergence of systems biology have catalyzed the rapid advancement of synthetic biotechnology [242].
Synthetic biotechnology is centered on an engineering-based approach that incorporates standardized experimental methods into the iterative process of designing, modifying, and constructing synthetic biological systems to achieve predetermined goals. This facilitates the systematic engineering of biology, emphasizing standardization, quantification, and universality. This methodology transcends the inherent constraints of biological evolution, enabling the precise and purposeful synthesis of novel compounds within the natural world.
Synthetic biology moving into biomedicine
Over the past two decades, synthetic biology has transitioned from its early role in engineering novel genetic circuits to being a pivotal component of 21st-century bioscience and biotechnology [243]. Simultaneously, the imperative to develop novel medical treatments has intensified. Synthetic biology extends the scope of traditional therapeutic interventions, offering the potential to fundamentally reshape the body’s maintenance of health and responses to diseases. CRISPR/Cas9 systems for genome engineering, gene regulatory grid analysis, and others offer a promising prospect for advanced cell-based therapies, microbiome reprogramming, and transformative disease diagnostics. The rational manipulation of bacteria through synthetic biology has given rise to the new concept of probiotics, designed to prevent and treat specific human diseases [244]. Chua et al. contended that engineered cells have the potential to address inherited or acquired metabolic disorders and target tumor cells for destruction [245]. In addition, bacterial programming may provide solutions for treating and preventing infectious diseases, offering alternatives to antibiotics and potential remedies for allergies and autoimmune disorders [240].
In summary, cells undergo modifications to produce pharmaceuticals and biofuels, the entire genome is synthesized de novo, and proteins and DNA molecules are endowed with non-native functionalities. Recent advances in synthetic biology have the potential to revolutionize biomedicine and biotechnology. These include the prospects of synthetic biology-based therapies to combat infectious diseases and cancer, innovations in vaccine development, microbiome manipulation, cellular therapies, and advances in regenerative medicine.
Synthetic biology for lung disease treatment
The COVID-19 pandemic disrupted the global socioeconomic landscape, compelling biologists to seek innovative solutions [246]. Synthetic biology, with its capability to detect pathogens, administer therapeutic agents, and regulate dosages to ensure safety compliance, has facilitated diagnostic and therapeutic research in the domain of lung diseases.
Synthetic biology-based diagnostics
Synthetic biology techniques have been employed to innovate diagnostic technologies aimed at detecting a range of pathogens and disease biomarkers or to fabricate novel diagnostic devices [247]. Typically, synthetic biology methodologies focus on the construction of innovative biosensing systems characterized by modular architectures that encompass sensors, signal processing components, and reporting modules, all equipped with quantifiable outputs. As the field of synthetic biology evolves, most constituent elements necessary for creating biosensing systems can be readily standardized and cataloged. Significant advancements have been made in synthetic biology to manage pulmonary disorders [248]. These advances encompass various in vitro diagnostic platforms, including biosensing systems that leverage CRISPR/Cas technology and synthetic RNAs designed for the efficient identification of biomarkers linked to lung diseases [249]. Consequently, these developments hold promise for enhancing patient well-being and health outcomes.
(A) Functionalized nano-delivery vector protamine sulfate stabilized Au NPs (AuPS)@pDNA for the treatment of IPF [231]. (a) Synthesis and therapeutic mechanism of AuPS@pDNA. (b) AuPS@pDNA-tagged hMSCs inhibit lung fibrosis in IPF cell model. (c) Three-dimensional computer tomography (CT) imaging of AuPS@pDNA-labeled hMSCs transplanted into the lungs of IPF mice. (B) Inhaled siIL11@PPGC NPs for the treatment of lung fibrosis [232]. (a) Inhaled siIL11@PPGC NPs into mouse lung fibroblasts for IPF treatment. (b) Inhalation therapy experimental design. (c-d) Lung tissue images (c) and immunofluorescence staining (d) of lung tissues of mice in different treatment groups. Reprinted with permission from Ref [231, 232]
CRISPR/Cas-based biosensors rely predominantly on the recognition of the disease-associated binding of specific pathogenic DNA or RNA target sequences and activate the nonspecific activity of Cas nucleases, leading to the cleavage of quenched fluorescent reporter RNAs. The cleaved RNA reporter genes subsequently emit easily detectable fluorescence signals [251]. For instance, during the identification of SARS-CoV-2 virus-specific mutations in envelope (E) and nucleoprotein (N) genes, the reporter molecule undergoes cleavage to generate a discernible viral signal [252]. To ensure reliable positive results, both genes must be detected to reduce the risk of false positives from related coronaviruses. Broughton et al. developed a CRISPR/Cas12 DETECTR technology with fast, accurate, and easy-to-use technique for the detection of SARS-CoV-2 in nasopharyngeal swab RNA extracts [250]. This method is based on the CRISPR/Cas12 lateral flow assay. The DETECTR system yielded positive results for both the E and N genes, improving the system’s accuracy in recognizing SARS-CoV-2 in the presence of other respiratory viral infections (Fig. 7A). Zhang et al. employed a cell-free, synthetic biology-driven biosensing strategy known as SHARK [249]. This approach regulates cell-free enzyme synthesis by utilizing activated Cas13a profiling to amplify RNA signals efficiently and accurately. Owing to its cascade amplification and enzyme output, SHARK offers broad compatibility in a wide range of situations. SHARK-based portable instruments have been successfully used for SARS-CoV-2 biosensing as shown in Fig. 7B, demonstrating extremely high sensitivity and selectivity, with results very close to the Ct value of quantitative reverse transcription polymerase chain reaction (qRT-PCR). Compared with existing detection methods, SHARK features precise identification, cascade amplification and customized signal output, and is promising for the development of next-generation RNA detection technologies.
(A) A CRISPR/Cas12-based assay for detection of SARS-CoV-2 [250]. (a) Primers, probes, and gRNA for genome. (b) SARS-CoV-2 DETECTR workflow. (B) SHARK-based RNA sensing for SARS-CoV-2 detection [249]. (a) SHARK workflow. (b) SARS-CoV-2 detection. (c) Optimization of crRNA types in SHARK. (d) SHARK assay for different concentrations of viral RNAs. (e) Results based on the SHARK device assay were consistent with the Ct values of qRT-PCR. Reprinted with permission from Ref [249, 250]
The synthetic RNA biosensor module comprises an RNA switch with sequences complementary to those of the target pathogen. The binding of the target RNA initiates the expression of a reporter gene, creating visually detectable product. The method enables rapid detection and reporting of SARS-CoV-2, is simple to develop, and is cost-effective. Nuclear regulators known as programmable riboregulator toehold switches have emerged as potential detection molecules. These riboregulators are constructed from codable RNA elements that can systematically generate reporter proteins in vivo or in vitro upon interaction with target nucleic acids. This interaction assesses the status of the endogenous RNA transcripts. Koksaldi et al. successfully devised a novel riboregulatory system using in vitro synthetic biology techniques [253]. This system was used to detect the specific genomic regions of SARS-CoV-2. The presence of SARS-CoV-2-related genes triggers the translation of sfGFP mRNA, resulting in green fluorescence emission. The design of this system also facilitates the visualization of the assay results when integrated with an immediate care device. The method is direct, cost-effective, and efficient, and offers the prospect of application to SARS-CoV-2 or other viral diagnostics.
Synthetic biology-based therapeutics
The concept of synthetic biology entails the deliberate reconstruction and redesign of biological systems for the purpose of attaining precise objectives [18]. Its application including gene editing and gene therapy, drug development and formulation, biosensor design, and enhancement of cellular therapies. Collectively, these applications hold substantial promise for the amelioration of lung diseases, potentially ushering in a new era of treatment for pulmonary disorders while simultaneously affording innovative therapeutic modalities and approaches.
Amidst the COVID-19 pandemic, extensive analyses of vast protein sequences have been made. This endeavor seeks to identify optimal candidate proteins for synthetic vaccine development and peptidomimetic therapeutic design, with the overarching goal of advancing drug and vaccine development. The intention behind these efforts aimed to curtail the propagation of the virus and mitigate the associated morbidity and mortality attributed to COVID-19. Several compounds have been engineered, designed, and tailored for use as therapeutic agents. Cao et al. designed a high-affinity miniprotein that competes with angiotensin converting enzyme 2 (ACE2) to bind to the SARS-CoV-2 spiking receptor-binding domain [254]. The authors demonstrated the ability of miniproteins to safeguard cultured human cells from SARS-CoV-2 infection by binding to the Spike protein and efficiently neutralizing the virus (Fig. 8A). Unlike antibodies, microproteins are not expressed in the mammalian cells. Their diminutive size and heightened stability render them amenable to direct delivery into the nasal cavity or respiratory system. This investigation not only holds promise for countering the COVID-19 pandemic but also exhibits potential efficacy against a range of respiratory viral infections. In addition, Schoof et al. devised nanosomes that disrupted the interactions between Spike protein and ACE2 [255]. This was achieved by screening a library of synthetic nanosome sequences on yeast surfaces. Notably, the nanobody 6 (Nb6) interacts with Spike in an entirely inactive conformation, with its receptor-binding structural domain locked in an inaccessible downstream state, preventing it from binding ACE2 (Fig. 8B). Further refinement through affinity maturation and structure-guided design culminated in the development of a trivalent nano-some, mNb6-tri, featuring femtomolar affinity for spikes and picomolar efficacy in neutralizing SARS-CoV-2 infection. mNb6-tri maintained its functionality after nebulization, lyophilization, and heat treatment, facilitating the aerosol-mediated delivery of this potent neutralizer directly to the airway epithelium. Stability, efficacy, and ability to bind to multiple epitopes make this anti-spiking protein NP a novel approach to potentially preventing and treating COVID-19.
(A) SARS-CoV-2 miniprotein inhibitors [254]. (a) Cryo–electron microscopy structures of SARS-CoV-2 S bound to LCB1. (b-c) Design of miniprotein inhibitors to neutralize live viruses. (B) A trivalent nano-some that neutralizes SARS-CoV-2 by stabilizing inactivated Spike [255]. (a) Cryo–electron microscopy structures of SpikeS2P-Nb6 complex. (b) mNb6-tri inhibits SARS-CoV-2 infection after lyophilization or heat treatment. Reprinted with permission frH
Although an effective antiviral drug to treat COVID-19 and other human coronavirus infections remains elusive, the FDA approved trials of Carrimycin, a synthetic biologic drug [256]. The drug is genetically engineered and modified with the incorporation of the heat-resistant Streptomyces 4-O-isopentyltransferase gene. This modification led to a notable enhancement of the antimicrobial activity of Carrimycin. In patients with severe COVID-19, Carrimycin impedes viral entry and subsequent replication events, particularly viral RNA synthesis. Studies have shown that carimycin has the highest antiviral potency and selectivity against HCoV-229E and HCoV-OC43 compared to those of acetylspiramycin and azithromycin. In addition, carimycin significantly inhibited the RNA synthesis of HCoV-OC43. However, it is not clear whether carimycin blocks viral protein synthesis, directly inhibits viral RNA synthesis, or regulates viral RNA synthesis by affecting host targets. Similar to other macrolides, carimycin can cause side effects such as adverse gastrointestinal reactions, but most are mildly tolerable.
Given the lack of potent antiviral drugs and effective therapeutic interventions for COVID-19, vaccination has emerged as the most effective control measure. Various strategies have been employed to develop SARS-CoV-2 vaccines such as DNA- and RNA-based [257]. Synthetic mRNA-based vaccines are particularly promising, being the first FDA-approved COVID-19 vaccine [258]. mRNA vaccines are lipid-based nanoparticle nucleotide-modified vaccines that employ viral proteins to induce immune responses during antigen presentation. SARS-CoV-2 involves viral spike proteins that bind to host cell ACE2 receptors and subsequently generate neutralizing antibodies in the presence of the virus [259]. Unlike traditional approaches, mRNA production facilitates large-scale vaccine manufacturing, thereby addressing the need for mass vaccination. This approach offers multiple advantages, including safety, cost-effectiveness, and the elicitation of both cell- and antibody-mediated immune responses.
In conclusion, since the 2019 epidemic, synthetic biotechnology has excelled in the development of diagnostics, therapeutics, and vaccines. However, it still has practical problems and technical challenges. For example, issues such as how to effectively avoid off-target effects, improve editing efficiency, and reduce immunogenicity limit the broad application of synthetic biotechnology in clinical diagnosis and treatment. In addition, targeted synthetic biotechnology can be used to design microorganisms or viruses with new functions. While these new organisms may have potential applications, they may also be misused or released into the environment with unpredictable consequences. Therefore, strict safety standards and regulatory mechanisms are therefore needed to ensure that the development of synthetic biology does not pose potential safety risks. In addition, synthetic biology designs and modifies organisms on a large scale, which may raise several ethical issues, such as the moral and social implications of human gene editing and the definition and boundaries of synthetic life. Hence, future research and applications of synthetic biology should pay attention to ethical considerations and sustainability to ensure that their development of synthetic biology technology is consistent with social values and environmental protection.
Summary and outlook
This review explored the use of nanomaterial-assisted gene editing and synthetic biology in diagnosing and treating lung diseases. The intricacies of the respiratory system often pose challenges to the management of lung diseases. Advances in nanotechnology have led to nanocarrier-based nano-delivery systems that can enhance lung biocarrier penetration through strategic considerations such as surface properties, particle size and shape. Consequently, the combination of nanotechnology and pulmonary drug delivery is a promising strategy for enhancing drug efficacy, release, and therapeutic effectiveness.
To enhance the efficacy of lung-targeted therapies, researchers have been actively exploring combining the unique properties of nanomaterials with gene editing techniques to achieve more precise and effective gene therapies. Among the gene editing systems, the emergence of the CRISPR/Cas9 system has greatly simplified the gene editing procedure and has had a profound impact on molecular biology and gene therapy. These proteins also function as nuclease enzymes to edit the genome of the target cell. Traditionally, delivery of the CRISPR/Cas9 gene-editing system relied on viral vectors. However, the immunogenicity, cytotoxicity, and potential infection risks associated with viral vectors limit their suitability as gene delivery vectors. Significantly, the rise of surface-modified or functionalized materials has propelled nanomaterials to the forefront as preferred carrier materials for non-viral CRISPR/Cas9 delivery systems. This is attributed to their high gene-editing efficiency, tissue/cell specificity, and low immunogenicity.
This review provides a comprehensive survey of nanomaterials as carriers for gene editing system delivery and their applications in lung disease therapy. The successful application of diverse biomaterials in CRISPR/Cas9 delivery systems underscores their versatility and adjustability, rendering them attractive solutions for addressing the various biological challenges associated with CRISPR/Cas9 delivery. Despite the advantages of biomaterial carriers, challenges remain in the delivery of CRISPR/Cas9 systems. Issues include achieving NP enrichment at precise locations, shielding the CRISPR/Cas9 system from detection and clearance by the reticuloendothelial system, and facilitating carrier penetration of a hydrophobic cell membrane. Furthermore, the immunological complications linked to biomaterial CRISPR/Cas9 systems pose significant concerns. With the advent of new biomaterial technologies and the intensive study of multiple extracellular and intracellular delivery systems, these limitations are expected to be progressively addressed by interdisciplinary researchers. The increasing efficiency of biomaterial delivery will bolster the clinical translation of CRISPR/Cas9 technology.
In the wake of the COVID-19 pandemic, it has become evident that traditional methods for detecting and diagnosing infectious pathogens have various limitations. These include dependence on well-established and comprehensive laboratories, the necessity for qualified personnel, the absence of standardized protocols, time-consuming processes, and increased susceptibility to false-negative and false-positive results. Consequently, these conventional analytical methods cannot provide reliable point-of-care testing solutions. Synthetic biology has emerged as a formidable asset in the medical field, in both industrialized and low-income countries. It excels in enhancing technology and point-of-care testing and addresses the drawbacks of traditional diagnostic approaches in the battle against deadly disease outbreaks. As an emerging interdisciplinary discipline, synthetic biology aims to realize the precision and modification of biological systems through in-depth research and engineering of organisms. This interdisciplinary approach enables the programming of microorganisms to provide swift, precise, specific, cost-effective, and non-invasive modalities in diagnosing and treating infectious diseases.
In the realms of nanomaterials, gene editing, and synthetic biology, advancements within a discipline have yielded novel tools and insights. The convergence of these two fields constitutes a prominent trend in their development, owing to the distinctive attributes and requirements of synthetic biology and nanobiology. With the continuous development of nanotechnology, arrays of nanoscale components can serve as catalysts, sensors, and delivery vehicles. This enables the intricate construction of gene circuits, precise regulation of gene circuit operation, and the execution of in vivo gene editing and modification. Synthetic biology can orchestrate specific biomolecules and ecosystems according to human design, autonomously produce nanomaterials, and yield nano-preparations, while simultaneously enhancing their efficiency and reducing toxicity.
Consequently, the interdisciplinary intersection and integration of nanotechnology, gene editing, and synthetic biology have emerged as significant focal points for the growth of these disciplines. Future advances in this convergence should focus primarily on achieving standardization and modularization. Standardization forms the cornerstone of the efficient construction and operation of nanodevices, while modularity of biological components is a fundamental feature of synthetic biology. Designing standardized, universally applicable interfaces and regulatory elements enables the targeted integration of functional modules, facilitating the scalability of synthetic biological systems. Moreover, the development of analytical techniques is imperative, encompassing multidisciplinary approaches, such as multimodal imaging techniques, fluorescence resonance energy transfer, and multi-omics analysis. These techniques are urgently needed for the in vivo monitoring and assessment of nanosynthesized biological systems. Furthermore, investigations into the biodistribution, effects on nontargeted tissues, and metabolic fate of synthetic nanobiosystems are essential to lay the groundwork for clinical translation and large-scale production applications.
Data availability
No datasets were generated or analysed during the current study.
References
Christenson SA, Smith BM, Bafadhel M, Putcha N. Chronic obstructive pulmonary disease. Lancet. 2022;399(10342):2227–42.
Stolz D, Mkorombindo T, Schumann DM, Agusti A, Ash SY, Bafadhel M, Bai C, Chalmers JD, Gerard JC, Dharmage SC, et al. Towards the elimination of chronic obstructive pulmonary disease: a Lancet Commission. Lancet. 2022;400(10356):921–72.
Celli BR, Wedzicha JA. Update on clinical aspects of chronic obstructive pulmonary disease. N Engl J Med. 2019;381(13):1257–66.
Burgel P-R, Burnet E, Regard L, Martin C. The changing epidemiology of cystic fibrosis the implications for adult care. Chest. 2023;163(1):89–99.
Kanne JP, Little BP, Schulte JJ, Haramati A, Haramati LB. Long-term lung abnormalities associated with covid-19 pneumonia. Radiology 2023, 306(2).
Zhang F, Zhuang J, Li Z, Gong H, de Avila BE-F, Duan Y, Zhang Q, Zhou J, Yin L, Karshalev E, et al. Nanoparticle-modified microrobots for in vivo antibiotic delivery to treat acute bacterial pneumonia. Nat Mater. 2022;21(11):1324.
Li B, Anderson DG. Lipid nanoparticle-enabled gene editing in the lung via inhalation. Nat Biotechnol. 2023;41(10):1394–5.
Sahu T, Ratre YK, Chauhan S, Bhaskar LVKS, Nair MP, Verma HK. Nanotechnology based drug delivery system: current strategies and emerging therapeutic potential for medical science. J Drug Deliv Sci Technol 2021, 63.
Woodman C, Vundu G, George A, Wilson CM. Applications and strategies in nanodiagnosis and nanotherapy in lung cancer. Sem Cancer Biol. 2021;69:349–64.
Chen J, Ye Z, Huang C, Qiu M, Song D, Li Y, Xu Q. Lipid nanoparticle-mediated lymph node-targeting delivery of mRNA cancer vaccine elicits robust CD8(+) T cell response. Proceedings of the National Academy of Sciences of the United States of America 2022, 119(34).
Milane L, Amiji M. Clinical approval of nanotechnology-based SARS-CoV-2 mRNA vaccines: impact on translational nanomedicine. Drug Delivery Translational Res. 2021;11(4):1309–15.
Liu G, Lin Q, ** S, Gao C. The CRISPR-Cas toolbox and gene editing technologies. Mol Cell. 2022;82(2):333–47.
Ghani MW, Iqbal A, Ghani H, Bibi S, Wang Z, Pei R. Recent advances in nanocomposite-based delivery systems for targeted CRISPR/Cas delivery and therapeutic genetic manipulation. J Mater Chem B. 2023;11(24):5251–71.
Taha EA, Lee J, Hotta A. Delivery of CRISPR-Cas tools for in vivo genome editing therapy: Trends and challenges. J Controlled Release. 2022;342:345–61.
Hu SW, Ding T, Tang H, Guo H, Cui W, Shu Y. Nanobiomaterial vectors for improving gene editing and gene therapy. Mater Today. 2023;66:114–36.
Sahel DK, Vora LK, Saraswat A, Sharma S, Monpara J, D’Souza AA, Mishra D, Tryphena KP, Kawakita S, Khan S et al. CRISPR/Cas9 genome editing for tissue-specific in vivo targeting: nanomaterials and translational perspective. Adv Sci 2023, 10(19).
Li T, Zhang L, Lu T, Zhu T, Feng C, Gao N, Liu F, Yu J, Chen K, Zhong J et al. Engineered extracellular vesicle-delivered CRISPR/CasRx as a novel RNA editing tool. Adv Sci 2023, 10(10).
Cubillos-Ruiz A, Guo T, Sokolovska A, Miller PF, Collins JJ, Lu TK, Lora JM. Engineering living therapeutics with synthetic biology. Nat Rev Drug Discovery. 2021;20(12):941–60.
Benner SA. Rethinking nucleic acids from their origins to their applications. Philosophical Trans Royal Soc B-Biological Sci 2023, 378(1871).
Matsuyama H, Suzuki HI. Systems and Synthetic microRNA Biology: from biogenesis to disease pathogenesis. Int J Mol Sci 2020, 21(1).
Marofi F, Abdul-Rasheed OF, Rahman HS, Budi HS, Jalil AT, Yumashev AV, Hassanzadeh A, Yazdanifar M, Motavalli R, Chartrand MS, et al. CAR-NK cell in cancer immunotherapy; a promising frontier. Cancer Sci. 2021;112(9):3427–36.
Hong M, Clubb JD, Chen YY. Engineering CAR-T cells for next-generation cancer therapy. Cancer Cell. 2020;38(4):473–88.
Wang Y, Zhang Z, Luo J, Han X, Wei Y, Wei X. mRNA vaccine: a potential therapeutic strategy. Mol Cancer 2021, 20(1).
Ma X, Zhang Y, Huang K, Zhu L, Xu W. Multifunctional rolling circle transcription-based nanomaterials for advanced drug delivery. Biomaterials. 2023;301:122241–122241.
Kim K, Choe D, Cho S, Palsson B, Cho B-K. Reduction-to-synthesis: the dominant approach to genome-scale synthetic biology. Trends Biotechnol 2024.
Wang M, Du L. Media representations of synthetic biology in China. Trends Biotechnol. 2023;41(12):1459–62.
** Z, Gao Q, Wu K, Ouyang J, Guo W, Liang X-J. Harnessing inhaled nanoparticles to overcome the pulmonary barrier for respiratory disease therapy. Adv Drug Deliv Rev. 2023;202:115111.
Lloyd CMM, Saglani S. Early-life respiratory infections and developmental immunity determine lifelong lung health. Nat Immunol 2023.
He Y, Liang Y, Han R, Lu W-L, Mak JCW, Zheng Y. Rational particle design to overcome pulmonary barriers for obstructive lung diseases therapy. J Controlled Release. 2019;314:48–61.
Munkholm M, Mortensen J. Mucociliary clearance: pathophysiological aspects. Clin Physiol Funct Imaging. 2014;34(3):171–7.
Ganesan S, Comstock AT, Sajjan US. Barrier function of airway tract epithelium. Tissue Barriers. 2013;1(4):24997.
Mikami Y, Grubb BR, Rogers TD, Dang H, Asakura T, Kota P, Gilmore RC, Okuda K, Morton LC, Sun L et al. Chronic airway epithelial hypoxia exacerbates injury in muco-obstructive lung disease through mucus hyperconcentration. Sci Transl Med 2023, 15(699).
Newman SP. Drug delivery to the lungs: challenges and opportunities. Therapeutic Delivery. 2017;8(8):647–61.
Lopez-Rodriguez E, Perez-Gil J. Structure-function relationships in pulmonary surfactant membranes: from biophysics to therapy. Biochim Et Biophys Acta-Biomembranes. 2014;1838(6):1568–85.
Khursheed R, Paudel KR, Gulati M, Vishwas S, Jha NK, Hansbro PM, Oliver BG, Dua K, Singh SK. Expanding the arsenal against pulmonary diseases using surface-functionalized polymeric micelles: breakthroughs and bottlenecks. Nanomedicine. 2022;17(12):881–911.
Garcia-Fernandez A, Sancenon F, Martinez-Manez R. Mesoporous silica nanoparticles for pulmonary drug delivery. Adv Drug Deliv Rev 2021, 177.
Doroudian M, Zanganeh S, Abbasgholinejad E, Donnelly SC. Nanomedicine in lung cancer immunotherapy. Front Bioeng Biotechnol. 2023;11:1144653.
Ajam-Hosseini M, Akhoondi F, Doroudian M. Nano based-oncolytic viruses for cancer therapy. Crit Rev Oncol/Hematol 2023:103980.
Hejabi F, Abbaszadeh MS, Taji S, O’Neill A, Farjadian F, Doroudian M. Nanocarriers: a novel strategy for the delivery of CRISPR/Cas systems. Front Chem 2022, 10.
Doroudian M, MacLoughlin R, Poynton F, Prina-Mello A, Donnelly SC. Nanotechnology based therapeutics for lung disease. Thorax. 2019;74(10):965–76.
Mirhadi E, Kesharwani P, Johnston TP, Sahebkar A. Nanomedicine-mediated therapeutic approaches for pulmonary arterial hypertension. Drug Discovery Today 2023, 28(6).
Forest V, Pourchez J. Nano-delivery to the lung- by inhalation or other routes and why nano when micro is largely sufficient? Adv Drug Deliv Rev 2022, 183.
Luo M-X, Hua S, Shang Q-Y. Application of nanotechnology in drug delivery systems for respiratory diseases. Mol Med Rep 2021, 23(5).
Ali ME, McConville JT, Lamprecht A. Pulmonary delivery of anti-inflammatory agents. Expert Opin Drug Deliv. 2015;12(6):929–45.
Joshi N. Nanotechnology enabled Inhalation of Bio-therapeutics for Pulmonary diseases: Design considerations and challenges. Curr Pathobiology Rep. 2018;6(4):225–31.
Wauthoz N, Rosiere R, Amighi K. Inhaled cytotoxic chemotherapy: clinical challenges, recent developments, and future prospects. Expert Opin Drug Deliv. 2021;18(3):333–54.
Osman N, Kaneko K, Carini V, Saleem I. Carriers for the targeted delivery of aerosolized macromolecules for pulmonary pathologies. Expert Opin Drug Deliv. 2018;15(8):821–34.
Tomak A, Cesmeli S, Hanoglu BD, Winkler D, Oksel Karakus C. Nanoparticle-protein corona complex: understanding multiple interactions between environmental factors, corona formation, and biological activity. Nanotoxicology. 2021;15(10):1331–57.
Shahrivar RY, Fakhr ZA, Abbasgholinejad E, Doroudian M. Smart lipid-based nanoparticles in lung cancer treatment: current status and future directions. Adv Ther. 2023;6(12):2300275.
Leong EWX, Ge R. Lipid nanoparticles as delivery vehicles for inhaled therapeutics. Biomedicines 2022, 10(9).
Thanki K, van Eetvelde D, Geyer A, Fraire J, Hendrix R, Van Eygen H, Putteman E, Sami H, Carvalho-Wodarz CS, Franzyk H, et al. Mechanistic profiling of the release kinetics of siRNA from lipidoid-polymer hybrid nanoparticles in vitro and in vivo after pulmonary administration. J Controlled Release. 2019;310:82–93.
Han H, Chen J, Li J, Correia A, Bartolo R, Shahbazi M-A, Teesalu T, Wang S, Cui W, Santos HA. Enhancing apoptosome assembly via mito-biomimetic lipid nanocarrier for cancer therapy. Adv Funct Mater 2023.
Souza FR, Fornasier F, Carvalho AS, Silva BM, Lima MC, Pimentel AS. Polymer-coated gold nanoparticles and polymeric nanoparticles as nanocarrier of the BP100 antimicrobial peptide through a lung surfactant model. J Mol Liq 2020, 314.
Pei Z, Lei H, Cheng L. Bioactive inorganic nanomaterials for cancer theranostics. Chem Soc Rev. 2023;52(6):2031–81.
Almeida SFF, Fonseca A, Sereno J, Ferreira HRS, Lapo-Pais M, Martins-Marques T, Rodrigues T, Oliveira RC, Miranda C, Almeida LP et al. Osteosarcoma-derived exosomes as potential PET imaging nanocarriers for lung metastasis. Small 2022, 18(49).
Wan M, Li T, Chen H, Mao C, Shen J. Biosafety, functionalities, and applications of biomedical micro/nanomotors. Angewandte Chemie-International Ed. 2021;60(24):13158–76.
Nguyen PHD, Jayasinghe MK, Le AH, Peng B, Le MTN. Advances in drug delivery systems based on red blood cells and their membrane-derived nanoparticles e. ACS Nano. 2023;17(6):5187–210.
Finbloom JA, Sousa F, Stevens MM, Desai TA. Engineering the drug carrier biointerface to overcome biological barriers to drug delivery. Adv Drug Deliv Rev. 2020;167:89–108.
Loira-Pastoriza C, Todoroff J, Vanbever R. Delivery strategies for sustained drug release in the lungs. Adv Drug Deliv Rev. 2014;75:81–91.
Torchilin VP. Recent advances with liposomes as pharmaceutical carriers. Nat Rev Drug Discovery. 2005;4(2):145–60.
Bangham AD, Standish MM, Watkins JC. Diffusion of univalent ions across lamellae of swollen phospholipids. J Mol Biol. 1965;13(1):238.
Sheikholeslami B, Lam NW, Dua K, Haghi M. Exploring the impact of physicochemical properties of liposomal formulations on their in vivo fate. Life Sci 2022, 300.
Ahmed KS, Hussein SA, Ali AH, Korma SA, Qiu L, Chen J. Liposome: composition, characterisation, preparation, and recent innovation in clinical applications. J Drug Target. 2019;27(7):742–61.
Mansour HM, Rhee Y-S, Wu X. Nanomedicine in pulmonary delivery. Int J Nanomed. 2009;4:299–319.
Barenholz Y. Doxil® - the first FDA-approved nano-drug: lessons learned. J Controlled Release. 2012;160(2):117–34.
Zhong W, Zhang X, Zeng Y, Lin D, Wu J. Recent applications and strategies in nanotechnology for lung diseases. Nano Res. 2021;14(7):2067–89.
Barenholz Y. Doxil (R) - the first FDA-approved nano-drug: lessons learned. J Controlled Release. 2012;160(2):117–34.
Chalmers JD, van Ingen J, van der Laan R, Herrmann J-L. Liposomal drug delivery to manage nontuberculous mycobacterial pulmonary disease and other chronic lung infections. Eur Respiratory Rev 2021, 30(161).
Wang C, Pan C, Yong H, Wang F, Bo T, Zhao Y, Ma B, He W, Li M. Emerging non-viral vectors for gene delivery. J Nanobiotechnol 2023, 21(1).
Kanasty R, Dorkin JR, Vegas A, Anderson D. Delivery materials for siRNA therapeutics. Nat Mater. 2013;12(11):967–77.
Anderson DM, Hall LL, Ayyalapu AR, Irion VR, Nantz MH, Hecker JG. Stability of mRNA/cationic lipid lipoplexes in human and rat cerebrospinal fluid: methods and evidence for nonviral mRNA gene delivery to the central nervous system. Hum Gene Ther. 2003;14(3):191–202.
Hamilton AG, Swingle KL, Mitchell MJ. Biotechnology: overcoming biological barriers to nucleic acid delivery using lipid nanoparticles. PLoS Biol 2023, 21(4).
Kumar K, Chatterjee N, Misra SK. Lipid based self-assembled nanostructures for therapeutic delivery applications. Chem Biology Lett 2022, 9(4).
Lv H, Zhang S, Wang B, Cui S, Yan J. Toxicity of cationic lipids and cationic polymers in gene delivery. J Controlled Release. 2006;114(1):100–9.
De A, Ko YT. A tale of nucleic acid-ionizable lipid nanoparticles: design and manufacturing technology and advancement. Expert Opin Drug Deliv. 2023;20(1):75–91.
Mendonca MCP, Kont A, Kowalski PS, O’Driscoll CM. Design of lipid-based nanoparticles for delivery of therapeutic nucleic acids. Drug Discovery Today. 2023;28(3):1–17.
Barba AA, Bochicchio S, Dalmoro A, Lamberti G. Lipid delivery systems for nucleic-acid-based-drugs: from production to clinical applications. Pharmaceutics 2019, 11(8).
Miller JB, Zhang S, Kos P, **ong H, Zhou K, Perelman SS, Zhu H, Siegwart DJ. Non-viral CRISPR/Cas gene editing in vitro and in vivo enabled by synthetic nanoparticle co-delivery of Cas9 mRNA and sgRNA. Angewandte Chemie-International Ed. 2017;56(4):1059–63.
Munir M, Zaman M, Waqar MA, Khan MA, Alvi MN. Solid lipid nanoparticles: a versatile approach for controlled release and targeted drug delivery. J Liposome Res 2023.
Salunkhe SA, Chitkara D, Mahato RI, Mittal A. Lipid based nanocarriers for effective drug delivery and treatment of diabetes associated liver fibrosis. Adv Drug Deliv Rev. 2021;173:394–415.
Sivadasan D, Ramakrishnan K, Mahendran J, Ranganathan H, Karuppaiah A, Rahman H. Solid lipid nanoparticles: applications and prospects in Cancer Treatment. Int J Mol Sci 2023, 24(7).
Yaghmur A, Mu H. Recent advances in drug delivery applications of cubosomes, hexosomes, and solid lipid nanoparticles. Acta Pharm Sinica B. 2021;11(4):871–85.
Liu J, Wu Z, Liu Y, Zhan Z, Yang L, Wang C, Jiang Q, Ran H, Li P, Wang Z. ROS-responsive liposomes as an inhaled drug delivery nanoplatform for idiopathic pulmonary fibrosis treatment via Nrf2 signaling. J Nanobiotechnol 2022, 20(1).
Tagami T, Ando Y, Ozeki T. Fabrication of liposomal doxorubicin exhibiting ultrasensitivity against phospholipase A(2) for efficient pulmonary drug delivery to lung cancers. Int J Pharm. 2017;517(1–2):35–41.
Bochicchio S, Lamberti G, Barba AA. Polymer-lipid Pharmaceutical Nanocarriers: innovations by New formulations and Production technologies. Pharmaceutics 2021, 13(2).
**e R, Wang X, Wang Y, Ye M, Zhao Y, Yandell BS, Gong S. pH-responsive polymer nanoparticles for efficient delivery of cas9 ribonucleoprotein with or without donor DNA. Adv Mater 2022, 34(23).
Rao JP, Geckeler KE. Polymer nanoparticles: Preparation techniques and size-control parameters. Prog Polym Sci. 2011;36(7):887–913.
Soppimath KS, Aminabhavi TM, Kulkarni AR, Rudzinski WE. Biodegradable polymeric nanoparticles as drug delivery devices. J Controlled Release. 2001;70(1–2):1–20.
Joshi G, Patel M, Chaudhary D, Sawant K. Preparation and surface modification of polymeric nanoparticles for drug delivery: state of the art. Recent Pat Drug Deliv Formul. 2020;14(3):201–13.
**ao Y, Tan A, Jackson AW, Boyd BJ. Nonspherical nanocapsules as long-circulating drug delivery systems. Chem Mater. 2022;34(6):2503–30.
Mora-Huertas CE, Fessi H, Elaissari A. Polymer-based nanocapsules for drug delivery. Int J Pharm. 2010;385(1–2):113–42.
Bu X, Ji N, Dai L, Dong X, Chen M, **ong L, Sun Q. Self-assembled micelles based on amphiphilic biopolymers for delivery of functional ingredients. Trends Food Sci Technol. 2021;114:386–98.
George A, Shah PA, Shrivastav PS. Natural biodegradable polymers based nano-formulations for drug delivery: a review. Int J Pharm. 2019;561:244–64.
Zacaron TM, Simoes e Silva ML, Costa MP, Mesquita e Silva D, Silva AC, Apolonio ACM, Fabri RL, Pittella F, Rocha HVA, Tavares GD. Advancements in chitosan-based nanoparticles for pulmonary drug delivery. Polymers 2023, 15(18).
Balde A, Kim S-K, Benjakul S, Nazeer RA. Pulmonary drug delivery applications of natural polysaccharide polymer derived nano/micro-carrier systems: a review. Int J Biol Macromol. 2022;220:1464–79.
Rahman Sabuj MZ, Islam N. Inhaled antibiotic-loaded polymeric nanoparticles for the management of lower respiratory tract infections. Nanoscale Adv. 2021;3(14):4005–18.
Tsung T-H, Tsai Y-C, Lee H-P, Chen Y-H, Lu D-W. Biodegradable polymer-based drug-delivery systems for ocular diseases. Int J Mol Sci 2023, 24(16).
Paranjpe M, Mueller-Goymann CC. Nanoparticle-mediated pulmonary drug delivery: a review. Int J Mol Sci. 2014;15(4):5852–73.
Menon JU, Ravikumar P, Pise A, Gyawali D, Hsia CCW, Nguyen KT. Polymeric nanoparticles for pulmonary protein and DNA delivery. Acta Biomater. 2014;10(6):2643–52.
Arora V, Abourehab MAS, Modi G, Kesharwani P. Dendrimers as prospective nanocarrier for targeted delivery against lung cancer. Eur Polymer J 2022, 180.
Gao Y, Dai W, Ouyang Z, Shen M, Shi X. Dendrimer-mediated intracellular delivery of fibronectin guides macrophage polarization to alleviate acute lung injury. Biomacromolecules 2023.
Inapagolla R, Guru BR, Kurtoglu YE, Gao X, Lieh-Lai M, Bassett DJP, Kannan RM. <i > in vivo efficacy of dendrimer-methylprednisolone conjugate formulation for the treatment of lung inflammation</i >. Int J Pharm. 2010;399(1–2):140–7.
Muddineti OS, Omri A. Current trends in PLGA based long-acting injectable products: the industry perspective. Expert Opin Drug Deliv. 2022;19(5):559–76.
Park K, Skidmore S, Hadar J, Garner J, Park H, Otte A, Soh BK, Yoon G, Yu D, Yun Y, et al. Injectable, long-acting PLGA formulations: analyzing PLGA and understanding microparticle formation. J Controlled Release. 2019;304:125–34.
Shi L-X, Liu X-R, Zhou L-Y, Zhu Z-Q, Yuan Q, Zou T. Nanocarriers for gene delivery to the cardiovascular system. Biomaterials Sci. 2023;11(24):7709–29.
Kango S, Kalia S, Celli A, Njuguna J, Habibi Y, Kumar R. Surface modification of inorganic nanoparticles for development of organic-inorganic nanocomposites-A review. Prog Polym Sci. 2013;38(8):1232–61.
Tsikourkitoudi V, Henriques-Normark B, Sotiriou GA. Inorganic nanoparticle engineering against bacterial infections. Curr Opin Chem Eng 2022, 38.
Lin G, Revia RA, Zhang M. Inorganic nanomaterial-mediated gene therapy in combination with other antitumor treatment modalities. Adv Funct Mater 2021, 31(5).
Hu X, Zhang Y, Ding T, Liu J, Zhao H. Multifunctional gold nanoparticles: a novel nanomaterial for various medical applications and biological activities. Front Bioeng Biotechnol 2020, 8.
Zheng Y, Zhao Y, Bai M, Gu H, Li X. Metal-organic frameworks as a therapeutic strategy for lung diseases. J Mater Chem B. 2022;10(30):5666–95.
Boisselier E, Astruc D. Gold nanoparticles in nanomedicine: preparations, imaging, diagnostics, therapies and toxicity. Chem Soc Rev. 2009;38(6):1759–82.
Gonzalez-Lopez MA, Gutierrez-Cardenas EM, Sanchez-Cruz C, Hernandez-Paz JF, Perez I, Olivares-Trejo JJ, Hernandez-Gonzalez O. Reducing the effective dose of cisplatin using gold nanoparticles as carriers. Cancer Nanotechnol 2020, 11(1).
Kankala RK, Han Y-H, Na J, Lee C-H, Sun Z, Wang S-B, Kimura T, Ok YS, Yamauchi Y, Chen A-Z et al. Nanoarchitectured structure and surface biofunctionality of mesoporous silica nanoparticles. Adv Mater 2020, 32(23).
Chen J, Wang Y, Wu C, **ao Y, Zhu Y. A coronavirus-mimic mesoporous silica nanosystem enables efficient targeted delivery of siRNA for anti-SARS-CoV-2. Appl Mater Today 2023, 35.
Subramaniam S, Thomas N, Gustafsson H, Jambhrunkar M, Kidd SP, Prestidge CA. Rifampicin-loaded mesoporous silica nanoparticles for the treatment of intracellular infections. Antibiotics-Basel 2019, 8(2).
Wang Z, Niu J, Zhao C, Wang X, Ren J, Qu X. A Bimetallic Metal-Organic Framework Encapsulated with DNAzyme for Intracellular Drug synthesis and self-sufficient gene therapy. Angewandte Chemie-International Ed. 2021;60(22):12431–7.
Cai G, Yan P, Zhang L, Zhou H-C, Jiang H-L. Metal-organic framework-based hierarchically porous materials: synthesis and applications. Chem Rev. 2021;121(20):12278–326.
Pan X, Wu N, Tian S, Guo J, Wang C, Sun Y, Huang Z, Chen F, Wu Q, **g Y et al. Inhalable MOF-Derived nanoparticles for Sonodynamic Therapy of Bacterial Pneumonia. Adv Funct Mater 2022, 32(25).
He S, Wu L, Li X, Sun H, **ong T, Liu J, Huang C, Xu H, Sun H, Chen W, et al. Metal-organic frameworks for advanced drug delivery. Acta Pharm Sinica B. 2021;11(8):2362–95.
El Andaloussi S, Maeger I, Breakefield XO, Wood MJA. Extracellular vesicles: biology and emerging therapeutic opportunities. Nat Rev Drug Discovery. 2013;12(5):348–58.
Rahimian S, Najafi H, Afzali B, Doroudian M. Extracellular vesicles and exosomes: novel insights and perspectives on lung cancer from early detection to targeted treatment. Biomedicines. 2024;12(1):123.
Woo H-K, Sunkara V, Park J, Kim T-H, Han J-R, Kim C-J, Choi H-I, Kim Y-K, Cho Y-K. Exodisc for rapid, size-selective, and efficient isolation and analysis of nanoscale extracellular vesicles from biological samples. ACS Nano. 2017;11(2):1360–70.
Li M, Liao L, Tian W. Extracellular vesicles derived from apoptotic cells: an essential link between death and regeneration. Front cell Dev Biology 2020, 8.
Miao C, Zhou W, Wang X, Fang J. The research progress of exosomes in osteoarthritis, with particular emphasis on the mediating roles of mirnas and lncrnas. Front Pharmacol 2021, 12.
Wu P, Zhang B, Ocansey DKW, Xu W, Qian H. Extracellular vesicles: a bright star of nanomedicine. Biomaterials 2021, 269.
Azhdari MH, Goodarzi N, Doroudian M, MacLoughlin R. Molecular insight into the therapeutic effects of stem cell-derived exosomes in respiratory diseases and the potential for pulmonary delivery. Int J Mol Sci. 2022;23(11):6273.
Hanjani NA, Esmaelizad N, Zanganeh S, Gharavi AT, Heidarizadeh P, Radfar M, Omidi F, MacLoughlin R, Doroudian M. Emerging role of exosomes as biomarkers in cancer treatment and diagnosis. Critical reviews in oncology/hematology 2022, 169:103565.
Duan L, Xu L, Xu X, Qin Z, Zhou X, **ao Y, Liang Y, **a J. Exosome-mediated delivery of gene vectors for gene therapy. Nanoscale 2021, 13(3).
Kim MS, Haney MJ, Zhao Y, Yuan D, Deygen I, Klyachko NL, Kabanov AV, Batrakova EV. Engineering macrophage-derived exosomes for targeted paclitaxel delivery to pulmonary metastases: <i > in vitro and < i > in vivo evaluations</i >. Nanomedicine-Nanotechnology Biology Med. 2018;14(1):195–204.
Liu B, Li Z, Huang S, Yan B, He S, Chen F, Liang Y. AAV-containing exosomes as a novel vector for improved gene delivery to lung cancer cells. Front cell Dev Biology 2021, 9.
Er S, Laraib U, Arshad R, Sargazi S, Rahdar A, Pandey S, Thakur VK, Diez-Pascual AM. Amino acids, peptides, and proteins: implications for nanotechnological applications in biosensing and drug/gene delivery. Nanomaterials 2021, 11(11).
Desale K, Kuche K, Jain S. Cell-penetrating peptides (CPPs): an overview of applications for improving the potential of nanotherapeutics. Biomaterials Sci. 2021;9(4):1153–88.
Shoari A, Tooyserkani R, Tahmasebi M, Lowik DWPM. Delivery of various cargos into cancer cells and tissues via cell-penetrating peptides: a review of the last decade. Pharmaceutics 2021, 13(9).
Shukla MK, Dubey A, Pandey S, Singh SK, Gupta G, Prasher P, Chellappan DK, Oliver BG, Kumar D, Dua K. Managing apoptosis in lung diseases using nano-assisted drug delivery system. Curr Pharm Design. 2022;28(39):3202–11.
Yang P, Lee AY-T, Xue J, Chou S-J, Lee C, Tseng P, Zhang TX, Zhu Y, Lee J, Chiou S-H et al. Nano-vectors for CRISPR/Cas9-mediated genome editing. Nano Today 2022, 44.
Liu J, Chang J, Jiang Y, Meng X, Sun T, Mao L, Xu Q, Wang M. Fast and efficient CRISPR/Cas9 genome editing in vivo enabled by bioreducible lipid and messenger rna nanoparticles. Adv Mater 2019, 31(33).
Chattopadhyay S, Sarkar SS, Saproo S, Yadav S, Antil D, Das B, Naidu S. Apoptosis-targeted gene therapy for non-small cell lung cancer using chitosan-poly-lactic-co-glycolic acid -based nano-delivery system and CASP8 and miRs 29A-B1 and 34A. Front Bioeng Biotechnol 2023, 11.
Gene editing. Nat Biotechnol. 2020;38(7):811–811.
Ferrari G, Thrasher AJ, Aiuti A. Gene therapy using haematopoietic stem and progenitor cells. Nat Rev Genet. 2021;22(4):216–34.
Fu Y, He X, Gao XD, Li F, Ge S, Yang Z, Fan X. Prime editing: current advances and therapeutic opportunities in human diseases. Sci Bull. 2023;68(24):3278–91.
Newby GA, Liu DR. In vivo somatic cell base editing and prime editing. Mol Ther. 2021;29(11):3107–24.
Su W, Li J, Ji C, Chen C, Wang Y, Dai H, Li F, Liu P. CRISPR/Cas systems for the detection of nucleic acid and non-nucleic acid targets. Nano Res. 2023;16(7):9940–53.
Gupta D, Bhattacharjee O, Mandal D, Sen MK, Dey D, Dasgupta A, Kazi TA, Gupta R, Sinharoy S, Acharya K et al. CRISPR-Cas9 system: a new-fangled dawn in gene editing. Life Sci 2019, 232.
Marraffini LA. CRISPR-Cas immunity in prokaryotes. Nature. 2015;526(7571):55–61.
Meng H, Nan M, Li Y, Ding Y, Yin Y, Zhang M. Application of CRISPR-Cas9 gene editing technology in basic research, diagnosis and treatment of colon cancer. Front Endocrinol 2023, 14.
Jiang F, Doudna JA. CRISPR-Cas9 Structures and Mechanisms. In: Annual Review of Biophysics, Vol 46 Edited by Dill KA, vol. 46; 2017: 505–529.
Liu C, Zhang L, Liu H, Cheng K. Delivery strategies of the CRISPR-Cas9 gene-editing system for therapeutic applications. J Controlled Release. 2017;266:17–26.
Zhao J, Fang H, Zhang D. Expanding application of CRISPR-Cas9 system in microorganisms. Synth Syst Biotechnol. 2020;5(4):269–76.
Nimkar S, Anand B. Casa3/I-C mediated target DNA recognition and cleavage during CRISPR interference are independent of the composition and architecture of Cascade surveillance complex. Nucleic Acids Res. 2020;48(5):2486–501.
Pausch P, Al-Shayeb B, Bisom-Rapp E, Tsuchida CA, Li Z, Cress BF, Knott GJ, Jacobsen SE, Banfield JF, Doudna JA. CRISPR-CasΦ from huge phages is a hypercompact genome editor. Science. 2020;369(6501):333–.
Lieber MR. The mechanism of double-strand DNA break repair by the nonhomologous DNA end-joining pathway. In: Annual Review of Biochemistry, Vol 79 Edited by Kornberg RD, Raetz CRH, Rothman JE, Thorner JW, vol. 79; 2010: 181–211.
Stinson BM, Loparo JJ. Repair of DNA double-strand breaks by the nonhomologous end joining pathway. In: Annual Review of Biochemistry, Vol 90, 2021. Edited by Kornberg RD, vol. 90; 2021: 137–164.
Ploessl D, Zhao Y, Cao M, Ghosh S, Lopez C, Sayadi M, Chudalayandi S, Severin A, Huang L, Gustafson M, et al. A repackaged CRISPR platform increases homology-directed repair for yeast engineering. Nat Chem Biol. 2022;18(1):38.
Wang H-X, Li M, Lee CM, Chakraborty S, Kim H-W, Bao G, Leong KW. CRISPR/Cas9-based genome editing for disease modeling and therapy: challenges and opportunities for nonviral delivery. Chem Rev. 2017;117(15):9874–906.
Zhang S, Shen J, Li D, Cheng Y. Strategies in the delivery of Cas9 ribonucleoprotein for CRISPR/Cas9 genome editing. Theranostics. 2021;11(2):614–48.
Lin Y-Q, Feng K-K, Lu J-Y, Le J-Q, Li W-L, Zhang B-C, Li C-L, Song X-H, Tong L-W, Shao J-W. CRISPR/Cas9-based application for cancer therapy: challenges and solutions for non-viral delivery. J Controlled Release. 2023;361:727–49.
Komor AC, Kim YB, Packer MS, Zuris JA, Liu DR. Programmable editing of a target base in genomic DNA without double-stranded DNA cleavage. Nature. 2016;533(7603):420–4.
Liang Y, Chen F, Wang K, Lai L. Base editors: development and applications in biomedicine. Front Med. 2023;17(3):359–87.
Neugebauer ME, Hsu A, Arbab M, Krasnow NA, McElroy AN, Pandey S, Doman JL, Huang TP, Raguram A, Banskota S. Evolution of an adenine base editor into a small, efficient cytosine base editor with low off-target activity. Nat Biotechnol. 2023;41(5):673–85.
Anzalone AV, Randolph PB, Davis JR, Sousa AA, Koblan LW, Levy JM, Chen PJ, Wilson C, Newby GA, Raguram A. Search-and-replace genome editing without double-strand breaks or donor DNA. Nature. 2019;576(7785):149–57.
Marzec M, Brąszewska-Zalewska A, Hensel G. Prime editing: a new way for genome editing. Trends Cell Biol. 2020;30(4):257–9.
Yang W, Yan J, Zhuang P, Ding T, Chen Y, Zhang Y, Zhang H, Cui W. Progress of delivery methods for CRISPR-Cas9. Expert Opin Drug Deliv. 2022;19(8):913–26.
Kreitz J, Friedrich MJ, Guru A, Lash B, Saito M, Macrae RK, Zhang F. Programmable protein delivery with a bacterial contractile injection system. Nature. 2023;616(7956):357–64.
Yan X, Pan Q, **n H, Chen Y, ** Y. Genome-editing prodrug: targeted delivery and conditional stabilization of CRISPR-Cas9 for precision therapy of inflammatory disease. Sci Adv. 2021;7(50):eabj0624.
Liang Y, Iqbal Z, Wang J, Xu L, Xu X, Ouyang K, Zhang H, Lu J, Duan L, **a J. Cell-derived extracellular vesicles for CRISPR/Cas9 delivery: engineering strategies for cargo packaging and loading. Biomaterials Sci. 2022;10(15):4095–106.
Dhaliwal HK, Fan Y, Kim J, Amiji MM. Intranasal delivery and transfection of mRNA therapeutics in the Brain using Cationic Liposomes. Mol Pharm. 2020;17(6):1996–2005.
Ho W, Gao M, Li F, Li Z, Zhang X-Q, Xu X. Next-generation vaccines: nanoparticle-mediated DNA and mRNA delivery. Adv Healthc Mater 2021, 10(8).
Yan J, Kang DD, Turnbull G, Dong Y. Delivery of CRISPR-Cas9 system for screening and editing RNA binding proteins in cancer. Adv Drug Deliv Rev 2022, 180.
Lohia A, Sahel DK, Salman M, Singh V, Mariappan I, Mittal A, Chitkara D. Delivery strategies for CRISPR/Cas genome editing tool for retinal dystrophies: challenges and opportunities. Asian J Pharm Sci. 2022;17(2):153–76.
Stadtmauer EA, Fraietta JA, Davis MM, Cohen AD, Weber KL, Lancaster E, Mangan PA, Kulikovskaya I, Gupta M, Chen F, et al. CRISPR-engineered T cells in patients with refractory cancer. Science. 2020;367(6481):1001–.
Huang L, Liao Z, Liu Z, Chen Y, Huang T, **ao H. Application and Prospect of CRISPR/Cas9 Technology in reversing Drug Resistance of Non-small Cell Lung Cancer. Front Pharmacol 2022, 13.
Schumann K, Lin S, Boyer E, Simeonov DR, Subramaniam M, Gate RE, Haliburton GE, Yee CJ, Bluestone JA, Doudna JA, et al. Generation of knock-in primary human T cells using Cas9 ribonucleoproteins. Proc Natl Acad Sci USA. 2015;112(33):10437–42.
Mandal PK, Ferreira LM, Collins R, Meissner TB, Boutwell CL, Friesen M, Vrbanac V, Garrison BS, Stortchevoi A, Bryder D. Efficient ablation of genes in human hematopoietic stem and effector cells using CRISPR/Cas9. Cell Stem Cell. 2014;15(5):643–52.
Rittiner JE, Moncalvo M, Chiba-Falek O, Kantor B. Gene-editing technologies paired with viral vectors for translational research into neurodegenerative diseases. Front Mol Neurosci 2020, 13.
Jena R, Vishwas S, Kumar R, Kaur J, Khursheed R, Gulati M, Singh TG, Vanathi BM, Alam A, Kumar B et al. Treatment strategies for HIV infection with emphasis on role of CRISPR/Cas9 gene: success so far and road ahead. Eur J Pharmacol 2022, 931.
Coughlan L. Factors which contribute to the immunogenicity of non-replicating adenoviral vectored vaccines. Front Immunol 2020, 11.
Bulcha JT, Wang Y, Ma H, Tai PWL, Gao G. Viral vector platforms within the gene therapy landscape. Signal Transduct Target Therapy 2021, 6(1).
Zalewska-Piatek B, Piatek R. Bacteriophages as potential tools for use in antimicrobial therapy and vaccine development. Pharmaceuticals 2021, 14(4).
Zanganeh S, Doroudian M, Nowzari ZR, Nasirmoghadas P, Nahand JS, Sepehrpour S, Moghoofei M. Viral nanoparticles-mediated delivery of therapeutic Cargo. Adv Ther. 2023;6(10):2300082.
Ren S, Wang M, Wang C, Wang Y, Sun C, Zeng Z, Cui H, Zhao X. Application of non-viral vectors in drug delivery and gene therapy. Polymers 2021, 13(19).
Li L, Hu S, Chen X. Non-viral delivery systems for CRISPR/Cas9-based genome editing: challenges and opportunities. Biomaterials. 2018;171:207–18.
Kashapov R, Ibragimova A, Pavlov R, Gabdrakhmanov D, Kashapova N, Burilova E, Zakharova L, Sinyashin O. Nanocarriers for biomedicine: from lipid formulations to inorganic and hybrid nanoparticles. Int J Mol Sci 2021, 22(13).
Yan J, Kang DD, Dong Y. Harnessing lipid nanoparticles for efficient CRISPR delivery. Biomaterials Sci. 2021;9(18):6001–11.
Hejabi F, Abbaszadeh MS, Taji S, O’Neill A, Farjadian F, Doroudian M. Nanocarriers: a novel strategy for the delivery of CRISPR/Cas systems. Front Chem. 2022;10:957572.
Wang M, Glass ZA, Xu Q. Non-viral delivery of genome-editing nucleases for gene therapy. Gene Ther. 2017;24(3):144–50.
Rui Y, Wilson DR, Green JJ. Non-viral delivery to enable genome editing. Trends Biotechnol. 2019;37(3):281–93.
Kang YK, Kwon K, Ryu JS, Lee HN, Park C, Chung HJ. Nonviral genome editing based on a polymer-derivatized CRISPR nanocomplex for targeting bacterial pathogens and antibiotic resistance. Bioconjug Chem. 2018;29(11):3936–3936.
Cong L, Ran FA, Cox D, Lin S, Barretto R, Habib N, Hsu PD, Wu X, Jiang W, Marraffini LA, et al. Multiplex genome engineering using CRISPR/Cas systems. Science. 2013;339(6121):819–23.
Xu C-F, Chen G-J, Luo Y-L, Zhang Y, Zhao G, Lu Z-D, Czarna A, Gu Z, Wang J. Rational designs of in vivo CRISPR-Cas delivery systems. Adv Drug Deliv Rev. 2021;168:3–29.
Xu X, Liu C, Wang Y, Koivisto O, Zhou J, Shu Y, Zhang H. Nanotechnology-based delivery of CRISPR/Cas9 for cancer treatment Advanced drug delivery reviews 2021, 176.
Zou Y, Sun X, Yang Q, Zheng M, Shimoni O, Ruan W, Wang Y, Zhang D, Yin J, Huang X. Blood-brain barrier–penetrating single CRISPR-Cas9 nanocapsules for effective and safe glioblastoma gene therapy. Sci Adv. 2022;8(16):eabm8011.
Doroudian M, O’Neill A, Mac Loughlin R, Prina-Mello A, Volkov Y, Donnelly SC. Nanotechnology in pulmonary medicine. Curr Opin Pharmacol. 2021;56:85–92.
Gersbach CA, Coyer SR, Le Doux JM, Garcia AJ. Biomaterial-mediated retroviral gene transfer using self-assembled monolayers. Biomaterials. 2007;28(34):5121–7.
Wang D, Nhu-An P, Tong J, Sakashita S, Allo G, Kim L, Yanagawa N, Raghavan V, Wei Y, To C, et al. Molecular heterogeneity of non-small cell lung carcinoma patient-derived xenografts closely reflect their primary tumors. Int J Cancer. 2017;140(3):662–73.
Han D, He X-Y, Huang Y, Gao M, Guo T, Ren X-H, Liao X-R, Chen X-S, Pang X, Cheng S-X. A multifunctional delivery system for remodulating cell behaviors of circulating malignant cells to prevent cell fusion. Adv Sci 2023, 10(29).
Liao Z-X, Kempson IM, Hsieh C-C, Tseng SJ, Yang P-C. Potential therapeutics using tumor-secreted lactate in nonsmall cell lung cancer. Drug Discovery Today. 2021;26(11):2508–14.
Doroudian M, Azhdari MH, Goodarzi N, O’Sullivan D, Donnelly SC. Smart nanotherapeutics and lung cancer. Pharmaceutics. 2021;13(11):1972.
Tseng SJ, Kempson IM, Liao Z-X, Ho Y-C, Yang P-C. An acid degradable, lactate oxidizing nanoparticle formulation for non-small cell lung cancer virotherapy. Nano Today 2022, 47.
Noureddine A, Maestas-Olguin A, Saada EA, LaBauve AE, Agola JO, Baty KE, Howard T, Sabo JK, Espinoza CRS, Doudna JA, et al. Engineering of monosized lipid-coated mesoporous silica nanoparticles for CRISPR delivery. Acta Biomater. 2020;114:358–68.
Kim SM, Shin SC, Kim EE, Kim S-H, Park K, Oh SJ, Jang M. Simple in vivo gene editing via direct self-assembly of Cas9 ribonucleoprotein complexes for cancer treatment. ACS Nano. 2018;12(8):7750–60.
Wang Y, Tang Y, Zhao X-m, Huang G, Gong J-h, Yang S-d, Li H, Wan W-j, Jia C-h, Chen G, et al. A multifunctional non-viral vector for the delivery of MTH1-targeted CRISPR/Cas9 system for non-small cell lung cancer therapy. Acta Biomater. 2022;153:481–93.
Long ME, Mallampalli RK, Horowitz JC. Pathogenesis of pneumonia and acute lung injury. Clin Sci. 2022;136(10):747–69.
Doroudian M, O’Neill A, O’Reilly C, Tynan A, Mawhinney L, McElroy A, Webster SS, MacLoughlin R, Volkov Y, Armstrong E. Aerosolized drug-loaded nanoparticles targeting migration inhibitory factors inhibit Pseudomonas aeruginosa-induced inflammation and biofilm formation. Nanomedicine. 2020;15(30):2933–53.
Meo SA, Bukhari IA, Akram J, Meo AS, Klonoff DC. COVID-19 vaccines: comparison of biological, pharmacological characteristics and adverse effects of Pfizer/BioNTech and Moderna Vaccines. Eur Rev Med Pharmacol Sci. 2021;25(3):1663–9.
Hajiaghapour Asr M, Dayani F, Saedi Segherloo F, Kamedi A, Neill AO, MacLoughlin R, Doroudian M. Lipid nanoparticles as promising carriers for mRNA vaccines for viral lung infections. Pharmaceutics. 2023;15(4):1127.
Schlich M, Palomba R, Costabile G, Mizrahy S, Pannuzzo M, Peer D, Decuzzi P. Cytosolic delivery of nucleic acids: the case of ionizable lipid nanoparticles. Bioeng Translational Med 2021, 6(2).
Zhao P, Hou X, Yan J, Du S, Xue Y, Li W, **ang G, Dong Y. Long-term storage of lipid-like nanoparticles for mRNA delivery. Bioactive Mater. 2020;5(2):358–63.
Cheng Q, Wei T, Farbiak L, Johnson LT, Dilliard SA, Siegwart DJ. Selective organ targeting (SORT) nanoparticles for tissue-specific mRNA delivery and CRISPR-Cas gene editing. Nat Nanotechnol. 2020;15(4):313.
Lokugamage MP, Vanover D, Beyersdorf J, Hatit MZC, Rotolo L, Echeverri ES, Peck HE, Ni H, Yoon J-K, Kim Y, et al. Optimization of lipid nanoparticles for the delivery of nebulized therapeutic mRNA to the lungs. Nat Biomedical Eng. 2021;5(9):1059–68.
Hassanzadeh P. The significance of bioengineered nanoplatforms against SARS-CoV-2: from detection to genome editing. Life Sci 2021, 274.
Kaczmarek JC, Patel AK, Kauffman KJ, Fenton OS, Webber MJ, Heartlein MW, DeRosa F, Anderson DG. Polymer-lipid nanoparticles for systemic delivery of mrna to the lungs. Angewandte Chemie-International Ed. 2016;55(44):13808–12.
Liu Y, Cao Z-T, Xu C-F, Lu Z-D, Luo Y-L, Wang J. Optimization of lipid-assisted nanoparticle for disturbing neutrophils-related inflammation. Biomaterials. 2018;172:92–104.
Wan F, Draz MS, Gu M, Yu W, Ruan Z, Luo Q. Novel strategy to combat antibiotic resistance: a sight into the combination of CRISPR/Cas9 and nanoparticles. Pharmaceutics 2021, 13(3).
Mba IE, Nweze EI. Nanoparticles as therapeutic options for treating multidrug-resistant bacteria: research progress, challenges, and prospects. World J Microbiol Biotechnol 2021, 37(6).
Wang G, Zhao G, Chao X, **e L, Wang H. The characteristic of virulence, biofilm and antibiotic resistance of klebsiella pneumoniae. Int J Environ Res Public Health 2020, 17(17).
Hao M, He Y, Zhang H, Liao X-P, Liu Y-H, Sun J, Du H, Kreiswirth BN, Chen L. CRISPR-Cas9-mediated carbapenemase gene and plasmid curing in carbapenem-resistant enterobacteriaceae. Antimicrob Agents Chemother 2020, 64(9).
Werder RB, Liu T, Abo KM, Lindstrom-Vautrin J, Villacorta-Martin C, Huang J, Hinds A, Boyer N, Bullitt E, Liesa M et al. CRISPR interference interrogation of COPD GWAS genes reveals the functional significance of desmoplakin in iPSC-derived alveolar epithelial cells. Science Advances 2022, 8(28).
Li Z, Luo G, Hu W-P, Hua J-L, Geng S, Chu PK, Zhang J, Wang H, Yu X-F. Mediated drug release from nanovehicles by black phosphorus quantum dots for efficient therapy of chronic obstructive pulmonary disease. Angewandte Chemie-International Ed. 2020;59(46):20568–76.
Mohamed A, Pekoz AY, Ross K, Hutcheon GA, Saleem IY. Pulmonary delivery of Nanocomposite Microparticles (NCMPs) incorporating miR-146a for treatment of COPD. Int J Pharm 2019, 569.
Lokras A, Thakur A, Wadhwa A, Thanki K, Franzyk H, Foged C. Optimizing the intracellular delivery of therapeutic anti-inflammatory tnf-α sirna to activated macrophages using lipidoid-polymer hybrid nanoparticles. Front Bioeng Biotechnol 2021, 8.
Frede A, Neuhaus B, Knuschke T, Wadwa M, Kollenda S, Klopfleisch R, Hansen W, Buer J, Bruder D, Epple M, et al. Local delivery of siRNA-loaded calcium phosphate nanoparticles abates pulmonary inflammation. Nanomedicine-Nanotechnology Biology Med. 2017;13(8):2395–403.
Song J, Cano-Rodriquez D, Winkle M, Gjaltema RAF, Goubert D, Jurkowski TP, Hei**k IH, Rots MG, Hylkema MN. Targeted epigenetic editing of SPDEF reduces mucus production in lung epithelial cells. Am J Physiology-Lung Cell Mol Physiol. 2017;312(3):1334–47.
Moses C, Kaur P. Applications of CRISPR systems in respiratory health: entering a new ‘red pen’ era in genome editing. Respirology. 2019;24(7):628–37.
Chen Q, Shen Y, Zheng J. A review of cystic fibrosis: Basic and clinical aspects. Anim Models Experimental Med. 2021;4(3):220–32.
Sui H, Xu X, Su Y, Gong Z, Yao M, Liu X, Zhang T, Jiang Z, Bai T, Wang J et al. Gene therapy for cystic fibrosis: challenges and prospects. Front Pharmacol 2022, 13.
Alton EWFW, Boyd AC, Cheng SH, Davies JC, Davies LA, Dayan A, Gill DR, Griesenbach U, Higgins T, Hyde SC, et al. Toxicology study assessing efficacy and safety of repeated administration of lipid/DNA complexes to mouse lung. Gene Ther. 2014;21(1):89–95.
Karmali PP, Chaudhuri A. Cationic Liposomes as non-viral carriers of gene medicines: resolved issues, open questions, and future promises. Med Res Rev. 2007;27(5):696–722.
Osman G, Rodriguez J, Chan SY, Chisholm J, Duncan G, Kim N, Tatler AL, Shakesheff KM, Hanes J, Suk JS, et al. PEGylated enhanced cell penetrating peptide nanoparticles for lung gene therapy. J Controlled Release. 2018;285:35–45.
van Meegen MA, Terheggen-Lagro SWJ, Koymans KJ, van der Ent CK, Beekman JM. Apical CFTR expression in human nasal epithelium correlates with lung disease in cystic fibrosis. PLoS ONE 2013, 8(3).
Villate-Beitia I, Zarate J, Puras G, Luis Pedraz J. Gene delivery to the lungs: pulmonary gene therapy for cystic fibrosis. Drug Dev Ind Pharm. 2017;43(7):1071–81.
Bao H, Cheng S, Li X, Li Y, Yu C, Huang J, Zhang Z. Functional au nanoparticles for engineering and long-term CT imaging tracking of mesenchymal stem cells in idiopathic pulmonary fibrosis treatment. Biomaterials 2022, 288.
Bai X, Zhao G, Chen Q, Li Z, Gao M, Ho W, Xu X, Zhang X-Q. Inhaled siRNA nanoparticles targeting IL11 inhibit lung fibrosis and improve pulmonary function post-bleomycin challenge. Sci Adv 2022, 8(25).
Schwank G, Koo B-K, Sasselli V, Dekkers JF, Heo I, Demircan T, Sasaki N, Boymans S, Cuppen E, van der Ent CK, et al. Functional repair of CFTR by CRISPR/Cas9 in intestinal stem cell organoids of cystic fibrosis patients. Cell Stem Cell. 2013;13(6):653–8.
Hodges CA, Conlon RA. Delivering on the promise of gene editing for cystic fibrosis. Genes Dis. 2019;6(2):97–108.
Simons M. Dreaming of a universal biology: synthetic biology and the origins of life. Hyle. 2021;27(1):91–116.
Jacob F, Monod J. Genetic regulatory mechanisms in synthesis of proteins. J Mol Biol. 1961;3(3):318.
Cameron DE, Bashor CJ, Collins JJ. A brief history of synthetic biology. Nat Rev Microbiol. 2014;12(5):381–90.
Szybalski W, Skalka A. Nobel-prizes and restriction enzymes. Gene. 1978;4(3):181–2.
Del Vecchio D, Qian Y, Murray RM, Sontag ED. Future systems and control research in synthetic biology. Annu Rev Control. 2018;45:5–17.
Jewett MC, Ellis T. Editorial overview: synthetic biology: frontiers in synthetic biology. Curr Opin Chem Biol. 2017;40:A1–3.
Ghosh M, Sharma N, Singh AK, Gera M, Pulicherla KK, Jeong DK. Transformation of animal genomics by next-generation sequencing technologies: a decade of challenges and their impact on genetic architecture. Crit Rev Biotechnol. 2018;38(8):1157–75.
Zhang X. From synthetic genome to creation of life. Protein Cell. 2010;1(6):501–2.
Schmidt TJN, Berarducci B, Konstantinidou S, Raffa V. CRISPR/Cas9 in the era of nanomedicine and synthetic biology. Drug Discovery Today. 2023;28(1):9–14.
Mayorga-Ramos A, Zuniga-Miranda J, Carrera-Pacheco SE, Barba-Ostria C, Guaman LP. CRISPR-Cas-based antimicrobials: design, challenges, and bacterial mechanisms of resistance. Acs Infect Dis. 2023;9(7):1283–302.
Chua KJ, Kwok WC, Aggarwal N, Sun T, Chang MW. Designer probiotics for the prevention and treatment of human diseases. Curr Opin Chem Biol. 2017;40:8–16.
Jiang Q, Xu Z, Ye G, Pahlow M, Hu M, Qu S. A systematic sco** review of environmental and socio-economic effects of COVID-19 on the global ocean-human system. Sci Total Environ 2022, 849.
Brooks SM, Alper HS. Applications, challenges, and needs for employing synthetic biology beyond the lab. Nat Commun 2021, 12(1).
Kabay G, DeCastro J, Altay A, Smith K, Lu H-W, Capossela AM, Moarefian M, Aran K, Dincer C. Emerging Biosensing Technologies for the Diagnostics of Viral Infectious Diseases. Advanced Materials 2022, 34(30).
Zhang C, Zhang P, Ren H, Jia P, Ji J, Cao L, Yang P, Li Y, Liu J, Li Z et al. Synthetic biology-powered biosensors based on CRISPR/Cas mediated cascade signal amplification for precise RNA detection. Chem Eng J 2022, 446.
Broughton JP, Deng X, Yu G, Fasching CL, Servellita V, Singh J, Miao X, Streithorst JA, Granados A, Sotomayor-Gonzalez A, et al. CRISPR-Cas12-based detection of SARS-CoV-2. Nat Biotechnol. 2020;38(7):870.
Li Y, Li S, Wang J, Liu G. CRISPR/Cas systems towards next-generation biosensing. Trends Biotechnol. 2019;37(7):730–43.
Krishnan S, Dusane A, Morajkar R, Venkat A, Vernekar AA. Deciphering the role of nanostructured materials in the point-of-care diagnostics for COVID-19: a comprehensive review. J Mater Chem B. 2021;9(30):5967–81.
Koksaldi IC, Kose S, Ahan RE, Haciosmanoglu N, Kehribar ES, Gungen MA, Bastug A, Dinc B, Bodur H, Ozkul A, et al. SARS-CoV-2 detection with de novo-designed synthetic riboregulators. Anal Chem. 2021;93(28):9719–27.
Cao L, Goreshnik I, Coventry B, Case JB, Miller L, Kozodoy L, Chen RE, Carter L, Walls AC, Park Y-J, et al. De novo design of picomolar SARS-CoV-2 miniprotein inhibitors. Science. 2020;370(6515):426.
Schoof M, Faust B, Saunders RA, Sangwan S, Rezelj V, Hoppe N, Boone M, Billesbolle CB, Puchades C, Azumaya CM, et al. An ultrapotent synthetic nanobody neutralizes SARS-CoV-2 by stabilizing inactive Spike. Science. 2020;370(6523):1473–9.
Iyer M, Jayaramayya K, Subramaniam MD, Lee SB, Dayem AA, Cho S-G, Vellingiri B. COVID-19: an update on diagnostic and therapeutic approaches. BMB Rep. 2020;53(4):191–205.
Peng X-L, Cheng J-S-Y, Gong H-L, Yuan M-D, Zhao X-H, Li Z. Wei D-X: advances in the design and development of SARS-CoV-2 vaccines. Military Med Res 2021, 8(1).
Shen C, Risk M, Schiopu E, Hayek SS, **e T, Holevinski L, Akin C, Freed G, Zhao L. Efficacy of COVID-19 vaccines in patients taking immunosuppressants. Ann Rheum Dis. 2022;81(6):875–80.
Yi C, Sun X, Ye J, Ding L, Liu M, Yang Z, Lu X, Zhang Y, Ma L, Gu W, et al. Key residues of the receptor binding motif in the spike protein of SARS-CoV-2 that interact with ACE2 and neutralizing antibodies. Cell Mol Immunol. 2020;17(6):621–30.
Funding
This work was supported by National Natural Scientific Funds (822770014 and 81991523), the National Key Research and Development Program Project (2018YFC1705900), and Zhejiang Shuren University research project (2023R053 and 2023KJ237).
Author information
Authors and Affiliations
Contributions
LJ.L., WJ.P. and LY.S. conceived the topic and drew up the outline. LJ.L. wrote and revised the original draft. WJ.P. and LY.S. reviewed and edited the draft. LJ.L. and LY.S. provided funding for the project. X.S., YY.S. and SX.Y performed the visualization of the manuscript. JF.Z. and N.K. performed project management and provided resources. All authors read and approved the final manuscript
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Lei, L., Pan, W., Shou, X. et al. Nanomaterials-assisted gene editing and synthetic biology for optimizing the treatment of pulmonary diseases. J Nanobiotechnol 22, 343 (2024). https://doi.org/10.1186/s12951-024-02627-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12951-024-02627-w