Abstract
Background
Severe neonatal hyperbilirubinemia has been known to cause the clinical syndrome of kernicterus and a milder one the syndrome of bilirubin-induced neurologic dysfunction (BIND). BIND clinically manifests itself after the neonatal period as developmental delay, cognitive impairment, and related behavioral and psychiatric disorders. The complete picture of BIND is not clear.
Methods
The Gunn rat is a mutant strain of the Wistar rat with the BIND phenotype, and it demonstrates abnormal behavior. We investigated serotonergic dysfunction in Gunn rats by pharmacological analyses and ex vivo neurochemical analyses.
Results
Ketanserin, the 5-HT2AR antagonist, normalizes hyperlocomotion of Gunn rats. Both serotonin and its metabolites in the frontal cortex of Gunn rats were higher in concentrations than in control Wistar rats. The 5-HT2AR mRNA expression was downregulated without alteration of the protein abundance in the Gunn rat frontal cortex. The TPH2 protein level in the Gunn rat raphe region was significantly higher than that in the Wistar rat.
Conclusions
It would be of value to be able to postulate that a therapeutic strategy for BIND disorders would be the restoration of brain regions affected by the serotonergic dysfunction to normal operation to prevent before or to normalize after onset of BIND manifestations.
Impact
-
We demonstrated serotonergic dysregulation underlying hyperlocomotion in Gunn rats. This finding suggests that a therapeutic strategy for bilirubin-induced neurologic dysfunction (BIND) would be the restoration of brain regions affected by the serotonergic dysfunction to normal operation to prevent before or to normalize after the onset of the BIND manifestations.
-
Ketanserin normalizes hyperlocomotion of Gunn rats.
-
To our knowledge, this is the first study to demonstrate a hyperlocomotion link to serotonergic dysregulation in Gunn rats.
Similar content being viewed by others
Introduction
Delivery from in utero low-oxic condition into the oxygen-rich atmosphere lets newborn infants switch their oxygen carrying hemoglobin (Hb) from fetal-type HbF to adult-type HbA, where HbF and HbA are, respectively, hetero-tetramers α2γ2 and α2β2 of α-, β-, and γ-globin-chain subunits.1,31 we measured the concentrations of neurotransmitters and their metabolites in the frontal cortex and striatum of the Gunn rat without ketanserin treatment by ex vivo neurochemical analyses to determine whether or not 5-HT system dysfunction existed that could be subdued by ketanserin binding to 5-HT2Rs. Figure 2 shows the concentrations in the frontal cortices and striata of the (j/j) and control (+/+) rats of 5-HT, 5-HIAA, DA, DOPAC, and HVA and turnovers of 5-HT and DA, respectively, calculated by the ratios of 5-HIAA/5-HT and (DOPAC + HVA)/DA.
These figures show the concentrations of 5-HT, DA, and their metabolites in the frontal cortex and striatum as assayed by ex vivo neurochemical analysis (N = 6–8 each). a 5-HT: 5-hydroxytryptamine, b 5HIAA: 5-hydroxyindole acetic acid, c 5HIAA/5-HT ratio, d DA: dopamine, e DOPAC: 3,4-dihydroxyphenylacetic acid, f HVA: 3-methoxy-4-hydroxyphenyl acetic acid, g (DOPAC+HVA)/DA ratio. Gunn rats showed significantly higher concentrations of 5-HT (***P = 0.0014) and 5HIAA (**P = 0.0026) in the frontal cortex than Wistar rats. DA and its metabolites were not significantly different between Gunn rats and Wistar rats. Gunn rat: black bar (j/j), Wistar rat: white bar (+/+). All data indicate mean ± SEM. Statistical analysis of the data was performed by multiple Student’s t test. ***P < 0.001, **P < 0.01, *P < 0.05.
Figure 2a, b show that both 5-HT and 5-HTIAA concentrations were significantly higher in the frontal cortex but not in the striatum of the (j/j) rat compared to the control (+/+) rat, and Fig. 2c shows that 5-HT turnover did not differ significantly both in the frontal cortices and striata between the two rats. Figure 2d–g, on the other hand, show that DA and its metabolite concentrations in the frontal cortices and striata of the (j/j) and control (+/+) rats did not significantly differ from each other.
Ketanserin is a high-affinity antagonist toward 5-HT2 receptor families (5-HT2Rs) in rodent brain, having a subtype-dependent inhibition constant Ki toward 5-HT2 receptor subtypes A (5-HT2AR) and C (5-HT2CR).32 In order to determine whether either or both subtypes are involved in the ketanserin effect on Gunn rat hyperlocomotion, we compared the RT-PCR 5-HT2AR and 5-HT2CR expression levels in the frontal cortices and striata of the Gunn and control Wistar rats. As shown in Fig. 3a, 5-HT2AR expression was lower in the frontal cortex of the (j/j) rat, but not in the striatum, than that in the control (+/+) rat. Figure 3b illustrates that the 5-HT2CR expression was not significantly different in the two rats. We also investigated the 5HT2AR protein expression in the Gunn rat frontal cortex and striatum, and there was no significant difference compared with the control (+/+) rat (Supplementary Fig. 2).
Expression levels of 5-HT2AR- and 5-HT2C-mRNA were assayed by reverse transcription PCR (RT-PCR) using total RNA from the frontal cortex and striatum (N = 6 each). a Decreased expression of 5TH2AR mRNA in the Gunn rat frontal cortex compared with Wistar rat (*P = 0.015). b On the other hand, expression of 5TH2CR mRNA was not significantly different in the frontal cortex or striatum. Gunn rat: black bar (j/j), Wistar rat: white bar (+/+). All data indicate mean ± SEM. Statistical analysis of the data was performed by multiple Student’s t test. ***P < 0.001, **P < 0.01, *P < 0.05.
Augmentation of TPH2 in raphe region of Gunn rat
Serotonergic neurons project from the raphe nucleus to the forebrain in rat brains,33 and one of their marker proteins is TPH2, an enzyme involved in 5-HT synthesis in the brain. Figure 4 compares western blots (Fig. 4h) and IHC images (Fig. 4a, b–g) of TPH2 protein in the raphe region of the Gunn and control Wistar rats. The lower panel in Fig. 4h shows CCD-camera-captured 16-bit digital images of TPH2 and GAPDH western-blotted bands of the (+/+) and (j/j) rat samples, and the rectangular shapes surrounding the respective bands were registered in Image J as “regions of interest” (ROIs). Image J analyzed the respective ROIs and reported integrated densities of the TPH2 and GAPDH bands of the (+/+) and (j/j) rats, followed by normalization of the former by the latter in the respective lanes. The lower bar graph in Fig. 4h shows normalized TPH2 integrated densities that show about 2.3 times augmentation in the (j/j) samples over the (+/+) ones. Comparison of TPH2-stained IHC images of the DRN (Fig. 4b, c), PDR (Fig. 4d, e), and MnR (Fig. 4f, g), where the left and right columns indicate the (+/+) and (j/j) sample images, respectively, proved that TPH2-positive cells in the (j/j) raphe regions showed no obviously different distributions from the (+/+) regions.
TPH2-positive cells mainly expressed in three parts of raphe nucleus; DRN dorsal raphe nucleus, PDR posterodorsal raphe nucleus, MnR median raphe nucleus. a Whole image of raphe region. Scale bars = 200 μm. b–g Micrographs of TPH2-immune stained cells in DRV (b, c), PDR (d, e), and MnR (f, g) regions from Wistar rats (left column) and Gunn rats (right column). Scale bars = 100 μm. Serotonergic neuronal marker tryptophan hydroxylase 2 (TPH2) protein in raphe region were assayed by western blotting and immunohistochemistry (N = 6 each). h TPH2 western blot analysis of the raphe region. The upper four panels show western blots of TPH2 proteins together with GAPDH as controls in the raphe region of Wistar and Gunn samples. TPH2- and GAPDH-specific bands were at 56k and 38k, respectively, on SDS-PAGE gel. The TPH2 levels were normalized by GAPDH level. Western blot analysis also showed significantly higher TPH2 protein levels in the Gunn rat raphe region compared with Wistar rat (**P = 0.0029). Gunn rat: black bar (j/j), Wistar rat: white bar (+/+). All data indicate mean ± SEM. Statistical analysis of the data was performed by multiple Student’s t test or Student’s t test. **P < 0.01.
While TPH2 is one of the serotonergic neuron markers, TH itself is one of the dopaminergic neuron markers in the central nervous system. Supplementary Fig. 1 shows TH-stained IHC images of the ventral tegmental area (VTA) and substantia nigra, a compact part (SNc) of the (+/+) and (j/j) samples, from which we can see that the dopaminergic neurons in VTA and SNc of the (j/j) rat had no clear differences in distribution from those in the control (+/+) rat. Dopaminergic neurons project from VTA to the frontal cortex and from nigra to the striatum in rat brain,34 and Supplementary Fig. 1 suggests that no abnormalities were found in the upstream regions of the dopaminergic system in the Gunn rat brain.
Discussion
To our knowledge, this is the first study to demonstrate a hyperactive link to serotonergic dysfunction in Gunn rats. As for nuclear jaundice in humans, unconjugated bilirubin deposited in basal ganglia, in specific globus pallidus and subthalamic nucleus, as well as in other nerve nuclei has not been revealed.35
In summary, 9–10-week-old Gunn rats having been s.c. injected with ketanserin 30 min before open field tests normalized their hyperlocomotion and serotonergic dysfunction. Ketanserin is a quinazoline derivative and 5-HT2AR antagonist, and we compared the concentrations of 5-HT and 5-HIAA in the frontal cortices and striata of Gunn and control Wistar rats by ex vivo neurochemical analyses. In the frontal cortex of Gunn rats, both 5-HT and 5-HIAA were higher in concentrations than in control Wistar rats, but in striata of the two rat types they were not statistically different from each other. The 5-HT2AR mRNA expression and protein abundance were studied by RT-PCR and western blotting, respectively, to reveal the downregulation of the mRNA expression without alteration of the protein abundance in the frontal cortex, but not in the striatum, of the Gunn rats compared with the control Wistar rats. Of note was that serotonergic dysfunction was not found in the striatum, but it was observed in the frontal cortex of the Gunn rats. On the other hand, our study showed that the Gunn rat dopaminergic system was intact.
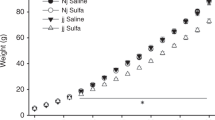
Figure 1 shows that Gunn rats displayed hyperactivity, frequent grooming and rearing during open field tests, behaviors that seemed agitation-like. These abnormal behaviors in Gunn rats were ameliorated by 5-HT receptor antagonist, ketanserin, s.c. injection. 5-HT is associated with anxiety, agitation, mood, and aggression, and it is considered to be a main target among neurotransmitters regarding neuropsychiatric disorders.36 Especially, the pre-frontal cortex (PFC), which projects serotonergic neurons from median raphe nuclei, controls emotion and cognition. PFC has a rich expression of 5-HT2AR, and 5-HT works to increase the postsynaptic current and inhibition of GABAA receptor via its receptors.37,38 It has also been reported that 5HT2AR antagonists improve hyperactivity and agitation-like behavior in such pharmacological rodent models.39,40 In vivo binding study of [3H]ketanserin showed that after [3H]ketanserin injection (i.v.), the highest labeling was found in the frontal cortex in rats.21 In our study, we found hyperlocomotion together with frontal cortical abnormal serotonergic transmission in Gunn rats. It is speculated that the effect of ketanserin on the Gunn rat abnormal behaviors may be due to the result of inhibiting the excess 5-HT transmission via the 5HT2A receptor in the frontal cortex.
Figure 4, on the other hand, shows augmentation of TPH2 protein without clear differences in distribution of TPH2-positive serotonergic cells in the raphe region of the Gunn rat. It is well known that, while cell bodies of most serotonergic neurons are found largely within the boundaries of the raphe nuclei, their axonal projections innervate nearly every area of the central nervous system.33 It seems plausible that increased 5-HT production in the raphe region of the Gunn rat, as shown in Fig. 4, led to hyper serotonergic transmission in the frontal cortex of Gunn rats, as shown in Fig. 2. The downregulation of 5-HT2AR mRNA, as shown in Fig. 3, might be caused by the hyper serotonergic transmission in the Gunn rat frontal cortex.
The locomotor circuitry in vertebrate animals is well understood.41 The basal ganglia and striatal projection neurons of the direct pathway initiate locomotor activity. The indirect pathway suppressed movement via globus pallidus externa and the subthalamic nucleus. The output from the basal ganglia activates the mesencephalic locomotor region, which in turn im**es on the lateral paragigantocellular nucleus that controls the spinal cords. The basal ganglia receive input from the cortex, thalamus, and SNc. Serotonergic neurons are located in the brainstem and innervate several levels of the locomotor circuitry. The rostral group of 5-HT nuclei largely project to the forebrain, and the caudal group of 5-HT nuclei largely project to the spinal cord. Moreover, the 5-HT nuclei also project to the brainstem (midbrain, pons, and medulla).42 The dopaminergic neurons in SNc also contribute to locomotor activity. The neurons project from SNc to the basal ganglia and brainstem.43 Based on these findings, other brain regions (i.e., thalamus, basal ganglia, brainstem, etc.) are also considered to be important for locomotion, so it may be worth investigating these brain regions in Gunn rats.
Previous studies have shown some abnormal behaviors of Gunn rats, such as hyperactivity,19,44 increased aggression,16 and attention and learning impairments.45 Gunn rats after sulfa injection show a clinical course and neuropathological findings similar to bilirubin encephalopathy, such as nuclear jaundice.15 Severe neurological abnormalities of Gunn rats after sulfa injection are clinical symptoms such as opisthotonos, seizures, ataxia, and dystonia,15 and characteristic neuropathological findings are cell death or gliosis in auditory nuclei, oculomotor nuclei, cerebellum, hippocampus, and basal ganglia.46 As for neurotransmitters of Gunn rats, one study reported elevated catecholamine levels in basal ganglia and cerebellum.45 Our group reported that some cognitive impairment of Gunn rats was likely to be caused by highly activated microglia.17,47,48,49 Recently, interneuronal loss in the Gunn rat hippocampus was reported.30 While those studies suggested associations of central neural dysfunction with the abnormal behaviors of Gunn rats, their mechanisms have not yet been sufficiently revealed.
The results suggest the presence of agitation underlying the hyperactivity of Gunn rats. The relationship between agitation and 5-HT is widely known as “serotonin syndrome.” Serotonin syndrome is an adverse phenomenon that is caused by an excess of 5-HT secreted by psychoactive drugs such as selective 5-HT reuptake inhibitors,50 and its clinical symptoms are remarkable agitation, psychomotor excitation, confusion, autonomic symptoms, etc. Agitation is one main psychological symptom that also accompanies schizophrenia, neurodevelopmental disorder, and dementia, not just serotonin syndrome. Patients with prolonged agitation feel strong suffering, and treatment of agitation has profound significance in the clinical picture.
Neonatal jaundice, including physiological jaundice, occurs in about 90% of Japanese, and we have not recognized the clinical risk of neonatal jaundice since phototherapy became an established therapy for pathological jaundice. However, together with results in the progress of neonatal care, several pediatricians have suggested to the rediscovery of the problems concerning neonatal jaundice particularly in premature babies. Recent studies have suggested that there is a significant correlation between neonatal jaundice and neurodevelopmental disorders.8,51 One epidemiological study conducted in Denmark for about 10 years reported a significantly increased risk for infantile autism in infants who showed hyperbilirubinemia after birth.7 The mechanisms associating neonatal jaundice and neurodevelopmental disorders remain poorly understood, so this clinical problem has been left largely unexplored.
ADHD is a common psychiatric disorder characterized by hyperlocomotion that affects 8–12% of children worldwide.52 The pathogenesis of ADHD is multifactorial, such as genetic and environmental factors as well as others not yet identified. Previous genetic studies concerning ADHD have focused mainly on the dysfunction of the dopaminergic system and discussed the defective function of DA and noradrenaline, so a central nervous system stimulant is a typical drug for ADHD. However, previous studies have suggested the important role of the 5-HT system in ADHD.53 Children diagnosed with ADHD and suffering from hyperlocomotion, and particularly with a history of BIND, may receive benefits from treatment by 5HT2A antagonist.
Other significant behavioral alterations in Gunn rats were social deficits as reported in our previous studies, which were demonstrated by social interaction tests.16 Social deficits are one of the characteristic symptoms of ASD. Recent studies suggested a relationship between ASD and 5-HT system dysfunction such as high levels of 5-HT in the brain in ASD model mice.54,55 We can find a similarity between ASD and BIND in certain aspects of their clinical symptoms and pathological background. From the above, 5HT2A antagonist treatment may be effective for the treatment of social deficits with a history of BIND.
The use of ketanserin has also been reported for the treatment of neurological disorder (Tourette’s syndrome) in children (9–16 years of age).56 The report showed that ketanserin was given at an initial dose of 20 mg/day to 7 children with Tourette’s syndrome. Six children showed dramatic improvement within a few days. Total disappearance of tics was obtained with doses up to 240 mg/day (mean = 120 mg/day). The report also showed that ketanserin was stopped in 1 child after 4 months because of orthostatic hypotension. The case report suggests that ketanserin may be given to children as long as blood pressure is controlled.
We examined the cause of hyperactivity in Gunn rats showing congenital hyperbilirubinemia, and our data demonstrate that hyperactivities in Gunn rat result in serotonergic dysfunction mainly in PFC. Our findings may help in the prevention and treatment of neurodevelopmental disorders with a post-birth history of hyperbilirubinemia.
In terms of psychiatric objectives, the pathophysiological mechanism of neuropsychiatric disorders, such as schizophrenia and neurodevelopmental disorder, has yet to be defined. Previous studies suggested that there are many clinical cases of neuropsychiatric disorders complicated by idiopathic unconjugated hyperbilirubinemia (Gilbert’s syndrome (GS)).10,57 In particular, schizophrenia accompanied by GS (20.6%) is significantly increased compared with other mental disorders (mood disorders: 2.8%, neurosis: 4.2%).10 These data indicate that we can discuss these issues in relation to the role of hyperbilirubinemia in the pathophysiological mechanism of schizophrenia. In this study, we demonstrated the effect of ketanserin on hyperactivity in model rats of congenital hyperbilirubinemia. It is expected that 5-HT2AR antagonists will treat clinical symptoms observed in schizophrenia, and most notably when complicated by hyperbilirubinemia.
Our study has some limitations. (1) We did not experiment with the use of ketanserin by local injection approach. Therefore, it is unclear whether the frontal cortex is a responsible focus for the behavioral abnormality in Gunn rats. (2) The molecular mechanism by which hyperbilirubinemia adversely affects the serotonergic system has not been clarified. Further studies will lead to understanding of the basic mechanism of the neurological dysfunction triggered by hyperbilirubinemia.
Our results suggest that higher serotonergic transmission voided the downregulation of 5-HT2AR mRNA expression and left the 5-HT2AR protein abundance unchanged in the frontal cortex of the Gunn rat, from which then developed the hyperactive phenotype of the rat. Although our experimental observations were limited to the frontal cortices and striata of 9–10-week-old Gunn and Wistar rats, it would be of value to be able to postulate that a therapeutic strategy for the BIND disorders would include restoration of the brain regions affected by serotonergic dysfunction to normal operation to prevent before or to normalize after onset of the BIND manifestations.
References
Richard, J., Avroy, A. & Michele, C. Fanaroff and Martin’s Neonatal-Perinatal Medicine 2-Volume Set 11th edn (Elsevier, 2019).
Wu, X. J., Zhong, D. N., **e, X. Z., Ye, D. Z. & Gao, Z. Y. UGT1A1 gene mutations and neonatal hyperbilirubinemia in Guangxi Heiyi Zhuang and Han populations. Pediatr. Res. 78, 585–588 (2015).
Nguyen, T. T., Zhao, W., Yang, X. & Zhong, D. N. The relationship between hyperbilirubinemia and the promoter region and first exon of UGT1A1 gene polymorphisms in Vietnamese newborns. Pediatr. Res. 88, 940–944 (2020).
Wang, J., Yin, J., Xue, M., Lyu, J. & Wan, Y. Roles of UGT1A1 Gly71Arg and TATA promoter polymorphisms in neonatal hyperbilirubinemia: a meta-analysis. Gene 736, 144409 (2020).
Long, J., Zhang, S., Fang, X., Luo, Y. & Liu, J. Neonatal hyperbilirubinemia and Gly71Arg mutation of UGT1A1 gene: a Chinese case-control study followed by systematic review of existing evidence. Acta Paediatr. 100, 966–971 (2011).
Dalman, C. & Cullberg, J. Neonatal hyperbilirubinaemia-a vulnerability factor for mental disorder? Acta Psychiatr. Scand. 100, 469–471 (1999).
Maimburg, R. D. et al. Neonatal jaundice: a risk factor for infantile autism? Paediatr. Perinat. Epidemiol. 22, 562–568 (2008).
Wei, C. C. et al. Neonatal jaundice and increased risk of attention-deficit hyperactivity disorder: a population-based cohort study. J. Child Psychol. Psychiatry 56, 460–467 (2015).
Miyaoka, T., Seno, H., Maeda, T., Itoga, M. & Horiguchi, J. Schizophrenia-associated idiopathic unconjugated hyperbilirubinemia (Gilbert’s syndrome): 3 case reports. J. Clin. Psychiatry 61, 299–300 (2000).
Miyaoka, T. et al. Schizophrenia-associated idiopathic unconjugated hyperbilirubinemia (Gilbert’s syndrome). J. Clin. Psychiatry 61, 868–871 (2000).
Amin, S. B., Smith, T. & Timler, G. Developmental influence of unconjugated hyperbilirubinemia and neurobehavioral disorders. Pediatr. Res. 85, 191–197 (2019).
Schutta, H. S. & Johnson, L. Bilirubin encephalopathy in the Gunn rat: a fine structure study of the cerebellar cortex. J. Neuropathol. Exp. Neurol. 26, 377–396 (1967).
Gunn, C. K. Hereditary acholuric jaundice in the rat. Can. Med. Assoc. J. 50, 230–237 (1944).
Daood, M. J., Hoyson, M. & Watchko, J. F. Lipid peroxidation is not the primary mechanism of bilirubin-induced neurologic dysfunction in jaundiced Gunn rat pups. Pediatr. Res. 72, 455–459 (2012).
Schutta, H. S. & Johnson, L. Clinical signs and morphologic abnormalities in Gunn rats treated with sulfadimethoxine. J. Pediatr. 75, 1070–1079 (1969).
Hayashida, M. et al. Hyperbilirubinemia-related behavioral and neuropathological changes in rats: a possible schizophrenia animal model. Prog. Neuropsychopharmacol. Biol. Psychiatry 33, 581–588 (2009).
Liaury, K. et al. Minocycline improves recognition memory and attenuates microglial activation in Gunn rat: a possible hyperbilirubinemia-induced animal model of schizophrenia. Prog. Neuropsychopharmacol. Biol. Psychiatry 50, 184–190 (2014).
Tsuchie, K. et al. The effects of antipsychotics on behavioral abnormalities of the Gunn rat (unconjugated hyperbilirubinemia rat), a rat model of schizophrenia. Asian J. Psychiatr. 6, 119–123 (2013).
Stanford, J. A. et al. Hyperactivity in the Gunn rat model of neonatal jaundice: age-related attenuation and emergence of gait deficits. Pediatr. Res. 77, 434–439 (2015).
Leysen, J. E. et al. Biochemical profile of risperidone, a new antipsychotic. J. Pharmacol. Exp. Ther. 247, 661–670 (1988).
Laduron, P. M., Janssen, P. F. & Leysen, J. E. In vivo binding of [3H]ketanserin on serotonin S2-receptors in rat brain. Eur. J. Pharmacol. 81, 43–48 (1982).
Oh-Nishi, A., Saji, M., Furudate, S. I. & Suzuki, N. Dopamine D(2)-like receptor function is converted from excitatory to inhibitory by thyroxine in the developmental hippocampus. J. Neuroendocrinol. 17, 836–845 (2005).
Oh-Nishi, A., Obayashi, S., Sugihara, I., Minamimoto, T. & Suhara, T. Maternal immune activation by polyriboinosinic-polyribocytidilic acid injection produces synaptic dysfunction but not neuronal loss in the hippocampus of juvenile rat offspring. Brain Res. 1363, 170–179 (2010).
Iyanagi, T., Watanabe, T. & Uchiyama, Y. The 3-methylcholanthrene-inducible UDP-glucuronosyltransferase deficiency in the hyperbilirubinemic rat (Gunn rat) is caused by a -1 frameshift mutation. J. Biol. Chem. 264, 21302–21307 (1989).
Malkova, N. V., Gallagher, J. J., Yu, C. Z., Jacobs, R. E. & Patterson, P. H. Manganese-enhanced magnetic resonance imaging reveals increased DOI-induced brain activity in a mouse model of schizophrenia. Proc. Natl Acad. Sci. USA 111, E2492–E2500 (2014).
Ogata, M., Akita, H. & Ishibashi, H. Behavioral responses to anxiogenic tasks in young adult rats with neonatal dopamine depletion. Physiol. Behav. 204, 10–19 (2019).
Kalueff, A. V. & Tuohimaa, P. Grooming analysis algorithm for neurobehavioural stress research. Brain Res. Brain Res. Protoc. 13, 151–158 (2004).
Paxinos, G. & Watson, C. The Rat Brain IN Stereotaxic Coordinates 6th edn (Elsevier, 2007).
Shimoyama, M. et al. The Rat Genome Database 2015: genomic, phenotypic and environmental variations and disease. Nucleic Acids Res. 43, D743–D750 (2015).
Hayashida, M. et al. Parvalbumin-positive GABAergic interneurons deficit in the hippocampus in Gunn rats: a possible hyperbilirubinemia-induced animal model of schizophrenia. Heliyon 5, e02037 (2019).
Pazos, A., Cortes, R. & Palacios, J. M. Quantitative autoradiographic map** of serotonin receptors in the rat brain. II. Serotonin-2 receptors. Brain Res. 346, 231–249 (1985).
NIMH. NIMH Psychoactive Drug Screening Program. https://pdsp.unc.edu/ (2017).
Hensler, J. G. Serotonergic modulation of the limbic system. Neurosci. Biobehav. Rev. 30, 203–214 (2006).
Bjorklund, A. & Dunnett, S. B. Dopamine neuron systems in the brain: an update. Trends Neurosci. 30, 194–202 (2007).
Shapiro, S. M. Definition of the clinical spectrum of kernicterus and bilirubin-induced neurologic dysfunction (BIND). J. Perinatol. 25, 54–59 (2005).
Puig, M. V. & Gulledge, A. T. Serotonin and prefrontal cortex function: neurons, networks, and circuits. Mol. Neurobiol. 44, 449–464 (2011).
Aghajanian, G. K. & Marek, G. J. Serotonin induces excitatory postsynaptic potentials in apical dendrites of neocortical pyramidal cells. Neuropharmacology 36, 589–599 (1997).
Aghajanian, G. K. & Marek, G. J. Serotonin, via 5-HT2A receptors, increases EPSCs in layer V pyramidal cells of prefrontal cortex by an asynchronous mode of glutamate release. Brain Res. 825, 161–171 (1999).
Kanno, H. et al. Effect of yokukansan, a traditional Japanese medicine, on social and aggressive behaviour of para-chloroamphetamine-injected rats. J. Pharm. Pharmacol. 61, 1249–1256 (2009).
Ninan, I. & Kulkarni, S. K. 5-HT2A receptor antagonists block MK-801-induced stereotypy and hyperlocomotion. Eur. J. Pharmacol. 358, 111–116 (1998).
Grillner, S., & El Manira, A. Current principles of motor control, with special reference to vertebrate locomotion. Physiol. Rev. 100, 271–320 (2020).
Flaive, A., Fougere, M., van der Zouwen, C. I. & Ryczko, D. Serotonergic modulation of locomotor activity from basal vertebrates to mammals. Front. Neural Circuits 14, 590299 (2020).
Ryczko, D. & Dubuc, R. Dopamine and the brainstem locomotor networks: from lamprey to human. Front. Neurosci. 11, 295 (2017).
Butcher, R. E., Stutz, R. M. & Berry, H. K. Behavioral abnormalities in rats with neonatal jaundice. Am. J. Ment. Defic. 75, 755–759 (1971).
Swenson, R. M. & Jew, J. Y. Learning deficits and brain monoamines in rats with congenital hyperbilirubinemia. Exp. Neurol. 76, 447–456 (1982).
Jew, J. Y. & Sandquist, D. CNS changes in hyperbilirubinemia. Functional implications. Arch. Neurol. 36, 149–154 (1979).
Furuya, M. et al. Yokukansan promotes hippocampal neurogenesis associated with the suppression of activated microglia in Gunn rat. J. Neuroinflammation 10, 145 (2013).
Limoa, E. et al. Electroconvulsive shock attenuated microgliosis and astrogliosis in the hippocampus and ameliorated schizophrenia-like behavior of Gunn rat. J. Neuroinflammation 13, 230 (2016).
Arauchi, R. et al. Gunn rats with glial activation in the hippocampus show prolonged immobility time in the forced swimming test and tail suspension test. Brain Behav. 8, e01028 (2018).
Scotton, W. J., Hill, L. J., Williams, A. C. & Barnes, N. M. Serotonin syndrome: pathophysiology, clinical features, management, and potential future directions. Int. J. Tryptophan Res. 12, 1178646919873925 (2019).
Lozada, L. E. et al. Association of autism spectrum disorders with neonatal hyperbilirubinemia. Glob. Pediatr. Health 2, 2333794X15596518 (2015).
Biederman, J. & Faraone, S. V. Attention-deficit hyperactivity disorder. Lancet 366, 237–248 (2005).
Ribases, M. et al. Exploration of 19 serotoninergic candidate genes in adults and children with attention-deficit/hyperactivity disorder identifies association for 5HT2A, DDC and MAOB. Mol. Psychiatry 14, 71–85 (2009).
Tanaka, M. et al. Brain hyperserotonemia causes autism-relevant social deficits in mice. Mol. Autism 9, 60 (2018).
Shen, H. W. et al. Regional differences in extracellular dopamine and serotonin assessed by in vivo microdialysis in mice lacking dopamine and/or serotonin transporters. Neuropsychopharmacology 29, 1790–1799 (2004).
Bonnier, C., Nassogne, M. C. & Evrard, P. Ketanserin treatment of Tourette’s syndrome in children. Am. J. Psychiatry 156, 1122–1123 (1999).
Muller, N., Schiller, P. & Ackenheil, M. Coincidence of schizophrenia and hyperbilirubinemia. Pharmacopsychiatry 24, 225–228 (1991).
Acknowledgements
We are grateful to Professor emeritus Tadakazu Maeda (Kitasato Univ.) and Dr. Nobuyuki Suzuki (neuroscientist) for giving us advice and to Riho Murai (Shimane Univ.), Kohei Ueda (Shimane Univ.), and Ayumi Fujiwara (Shimane Univ.) for research assistances. Funding came from KAKENHI 19K17363 (to S.M.), from the Ministry of Education, Culture, Sports, Science and Technology (MEXT).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: S.M. and A.O.-N. Performed the experiments: S.M., K.T., M.F., R.A., T.T., and A.O.-N. Discussed the data: T.T., K.O., M.H., S.H., R.W., T.M., and M.I. Wrote the paper: all authors contributed. A.O.-N. supervised this study.
Corresponding author
Ethics declarations
Competing interests
Shimane University has submitted a patent application (PCT/JP2020/017552) for the use of the compound described in this paper. M.I. has received grants from Research for Promotion of Cancer Control Programs during the conduct of the study. He has received lecture fees from Technomics, Fuji Keizai, Novartis, Yoshitomiyakuhin, Pfizer, MSD, Meiji Seika Pharma, Eisai, Otsuka, Sumitomo Dainippon Pharma, Mochida, Janssen, Takeda, and Eli Lilly. The institution of M.I. received grants or research support from Otsuka, Eisai, Daiichi-Sankyo, Pfizer, Astellas, MSD, Takeda, Fujifilm, Shionogi, and Mochida. A.O.-N. is listed as an inventor of this patent. A.O.-N. is CEO & CTO of RESVO Inc. and has >5% of RESVO Inc. shares but had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript. This does not alter our adherence to Pediatric Research publication policy. Other authors have no competing interests to declare.
Patient consent
Patient consent was not required.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
About this article
Cite this article
Miura, S., Tsuchie, K., Fukushima, M. et al. Normalizing hyperactivity of the Gunn rat with bilirubin-induced neurological disorders via ketanserin. Pediatr Res 91, 556–564 (2022). https://doi.org/10.1038/s41390-021-01446-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-021-01446-1
- Springer Nature America, Inc.