Abstract
Activity-dependent synaptic plasticity is a ubiquitous property of the nervous system that allows neurons to communicate and change their connections as a function of past experiences. Through reweighting of synaptic strengths, the nervous system can remodel itself, giving rise to durable memories that create the biological basis for mental function. In healthy individuals, synaptic plasticity undergoes characteristic developmental and aging trajectories. Dysfunctional plasticity, in turn, underlies a wide spectrum of neuropsychiatric disorders including depression, schizophrenia, addiction, and posttraumatic stress disorder. From a mechanistic standpoint, synaptic plasticity spans the gamut of spatial and temporal scales, from microseconds to the lifespan, from microns to the entire nervous system. With the numbers and strengths of synapses changing on such wide scales, there is an important need to develop measurement techniques with complimentary sensitivities and a growing number of approaches are now being harnessed for this purpose. Through hemodynamic measures, structural and tracer imaging, and noninvasive neuromodulation, it is possible to image structural and functional changes that underlie synaptic plasticity and associated behavioral learning. Here we review the mechanisms of neural plasticity and the historical and future trends in techniques that allow imaging of synaptic changes that accompany psychiatric disorders, highlighting emerging therapeutics and the challenges and opportunities accompanying this burgeoning area of study.
Similar content being viewed by others
Overview
Neuroplasticity has a profound impact on the manifestation and progression of clinical symptoms in many psychiatric illnesses. Understanding the multiscale role that plasticity has on neuropathology is critical to creating improved, targeted therapies. Through experiments that directly manipulate plasticity to create testable, causal changes over time, and through cross-sectional, retrospective, and postmortem analysis that reveal accumulated differences in plasticity that arise naturally, it is possible to obtain valuable information about the mechanism-of-action underlying healthy and disordered synaptic plasticity. While there has been considerable progress toward understanding these mechanisms, the impact of plasticity on behavior and the best approaches to induce neuroplastic change for therapeutic gains still remain open and important questions. This review seeks to provide a contemporary overview of the science elucidating the mechanisms of plasticity, the current state-of-the-art in methods used to image plasticity and promote therapeutic gains, and to provide suggestions for profitable future directions.
Mechanisms of neural plasticity
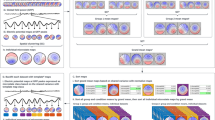
Neural plasticity refers to the possibility of altering the strength of connections within the nervous system through experience or injury. Plasticity can act to reorganize either the structure or the function of neurons and is necessary not only for neural networks to acquire new capabilities, but also for them to remain robust and stable over time. A key element of plasticity revolves around the temporal coincidence of activity. So-called, spike-timing-dependent plasticity (STDP) is a Hebbian learning rule in which the modification of synaptic strengths depends on the relative timing of action potentials [1]. Within monosynaptic pairs of neurons, it has been shown that if an input spike from the presynaptic neuron occurs immediately before the postsynaptic neuron’s output spike, then that input becomes stronger, creating long-term potentiation (LTP). If the input spike occurs immediately after an output spike, however, that input is made weaker, creating long-term depression [2, 3] (LTD) (While STDP generally involves molecular alterations at the synapse they rely on wide variety of distinct mechanisms that can differ in different brain regions (e.g., LTP induced during learning is different in the hippocampus and amygdala), among different neurons in the same brain region (e.g., endocannabinoid and non-endocannabinoid LTD in projections from the striatum to the basal ganglia), or within the same types of neurons (e.g., hippocampal CA3 pyramidal neurons that converge from different afferent inputs)). This critical window of timing-dependency spans tens of milliseconds and has profound functional implications on brain function, creating a means for activity-dependent bidirectional modification of synaptic strength, and ultimately forming the physiological basis for learning and memory. The mechanism underlying STDP has been attributed to two different glutamate receptors that are commonly co-expressed, the α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA) receptor and the N-methyl-D-aspartate (NMDA) receptor [4]. The NMDA is a glutamate receptor cation channel that is also widely referred to as a “coincidence detector”. Within this channel, coincidence is detected by the simultaneous presence of both membrane depolarization that vacates a channel-blocking magnesium ion, and the binding of its natural ligand, glutamate [4, 5]. The preexisting membrane depolarization of NMDA is in turn mediated through the coactivation of AMPA activation [6] to create reciprocal cellular mechanisms that enable long-term synaptic changes.
Beyond spike-timing-dependent plasticity that occurs rapidly at the synapses, other slower homeostatic processes occur over hours, days, or weeks to modify ion channel density, neurotransmitter release, or postsynaptic receptor sensitivity [7]. These processes are triggered in response to rapid activity-dependent changes and constitute a negative feedback loop, decreasing connectivity in response to high neuronal activity but increasing connectivity when activity drops [8]. Yet, another plasticity-based moderator of neuronal network communication is the growth of myelin, a multilayered membrane produced by oligodendrocytes that surrounds axons to increase the speed by which electrical signals propagate through the nervous system. While widely associated with critical developmental periods, there is also considerable evidence that activity-dependent myelination continues into adulthood [78]. CBT was found to yield decreases in both gray matter volume and BOLD responsivity in the amygdala, implying structural and functional level changes that decrease synaptic strength. The authors postulated that the diminished gray matter mediated the decreased responsivity and social anxiety in the CBT group, providing a specific mechanism by which plasticity may produce clinically meaningful effects in this treatment paradigm [78]. Conversely, a study of 13 patients with chronic pain who received CBT showed improved clinical measures as well as increased gray matter in the prefrontal and posterior parietal cortices as demonstrated through MRI VBM compared to 13 healthy controls [79]. These two studies taken together reinforce the premise for therapy-driven modulations of synaptic plasticity. Both studies led to clinical improvement, however through a decrease and increase in synaptic strength, respectively.
Prefrontal neural networks involved in motivation, cognition, social and emotional behavior exhibit learning-dependent plasticity. There has been considerable research on develo** engaging cognitive training to induce and maximize this plasticity, yielding several key takeaways. Namely, the mechanisms behind cognitive training induced neural plasticity are present throughout life and can impact higher-order cognition, but are also impacted by behavioral states and brain chemistry [80]. From a clinical perspective, data has demonstrated large, generalizable, and durable effects, with evidence of plasticity in frontal and sensory neural networks [80].
Individuals with schizophrenia are known to have accelerated cortical thinning, and by extension synapse loss, that is associated with illness severity. A recent study examined changes in cortical thickness in patients with recent onset schizophrenia randomly allocated to either targeted cognitive training or a computer game control intervention; whereas mean cortical thickness was not significantly changed in response to targeted cognitive training, individual increases in cortical thickness were predictive of increases in global cognition—an effect not seen in the control group [81]. Previous studies in patients with schizophrenia have established that cognitive training may impact structural and functional plasticity. Notably, 40 h of auditory and working memory targeted cognitive training were associated with changes in thalamic volume in patients with schizophrenia, suggestive of either a protective or enhancing effect on thalamic structure [82]. Of these two possibilities, a model for neural response to targeted cognitive training in patients with schizophrenia is one in which the training evokes general neuroprotection, as opposed to region-specific changes in neuroplasticity [81]. This is believed to be due to the increased cortical thickness, or prevented cortical thinning, seen in patients with schizophrenia who had undergone targeted cognitive training and exhibited corresponding increased global cognitive scores [81].
The left and right middle frontal gyri (MFG) of patients with schizophrenia are known to have signaling abnormalities, exhibiting both hyper and hypoactivation when performing working memory tasks [83, 84]. Intensive cognitive training in patients with schizophrenia increased fMRI signal efficiency of MFG compared to computer game control recipients with lasting effects present at 6 months post-intervention; notably, participants had improved working memory task performance, increased activation in the left MFG, and a significant association between improved task performance and right MFG signal [85]. Once more, changes in signaling efficacy seen in the cognitive training group lends itself to the idea that neural plasticity in humans can be induced in a measurable form via deliberate training.
Future research directions—challenges and opportunities
Understanding the roles of neuroplasticity in neuropsychiatric illnesses and their relationship to symptom development is critical to creating improved, targeted therapies. While there has been progress toward understanding the mechanisms of plasticity and innovations in therapies, there remain several challenges to studying this process. One of the major challenges is the multiscale nature in which the brain changes. Plasticity occurs on a spectrum from microscale changes at the synapse to morphological alterations that span the entire nervous system. They occur moment-to-moment and continually throughout the entire lifespan. Relating synaptic development to clinical improvement requires integration of multiple tools in conjunction, adding to the complexity of the evaluation, but creating new opportunities for discovery and development. Moreover, when comparing the brain before and after treatment, or even between healthy and diseased individuals, plasticity can depend on experience, time, and individual factors such as stress and genetics [15]. Interactions between these variables needs to be considered when attempting to delineate healthy and diseases brains. Therefore, this highly variable process complicates the generalizability of biomarkers and presents challenges to the field moving forward.
Although animal models can provide direct insight into neuronal alterations through invasive imaging and sampling, establishing valid animal models of psychiatric illnesses is difficult and means that findings remain speculative until validated in humans [86]. Animal models are also typically more homogenous in their symptomology and do not have co-morbid illnesses which tend to complicate disease etiology in humans. This is especially relevant when trying to correlate changes in plasticity to improvements in disease related behavior. On the other hand, most measures to assess plasticity in humans are noninvasive and are therefore not able to directly ascertain changes at a microscale, leaving open the possibility that they reflect indirect consequences of disordered plasticity and not the foundational pathology itself. In addition, due to the heterogenous nature of psychiatric illnesses and multiple factors influencing plasticity, establishing baseline healthy brain states, relative to disease states, is an important challenge. It is therefore challenging to assess the causes of maladaptive plasticity and distinguish these from their effects on behavior.
Despite these challenges, there is tremendous growth in the field with boundary-crossing innovations that allow greater resolution in space and time, and new approaches to link across multiple scales. In particular, there is a strong movement toward the development of predictive biomarkers of treatment efficacy that are critical for understanding not only how plasticity influences symptoms but determining who will benefit most from a given therapy. For example, by demonstrating correlations between specific markers of plasticity and individuals who respond to treatment, future clinical trials can use this information to predict whether a patient is likely to improve through changes in brain plasticity [87]. One example of a clinical biomarker currently in use is the presence of single nucleotide polymorphisms that correlate with greater efficacy of olanzapine in schizophrenia [88]. Epigenetic markers are also useful to predict drug efficacy such as the absence of methylated exon 4 of BDNF which is associated with reduced response to anti-depressants [89]. Not only would it be informative to have biomarkers of treatment response, but also of treatment progression [90]. To address some of the concerns with regards to disease heterogeneity and causes of dysregulation, it is crucial to have a better biological understanding of healthy neuroplasticity and how it can be dysregulated. Biomarkers would provide an objective measure of disease progression and pathogenesis, which could ultimately inform therapies.
Another profitable direction for future development is the individualization of treatment protocols to each patient with the goal of improving therapeutic gains. This is especially relevant to address the challenge of varied clinical profiles. For example, in most TMS protocols, patients are stimulated at the same brain region regardless of connectivity patterns or brain state during stimulation. Multiple studies, however, have shown that patients who respond best to TMS received stimulation at the node of the DLPFC most anti-correlated with the SGC [66]. Currently, there are investigations analyzing the difference between stimulating during resting-state, a more variable brain state between patients, versus during a task to create consistency or engage the network of interest [91]. Finally, combining therapies could provide another degree of personalization if patients respond better with just neurostimulation or with behavioral or pharmacological interventions as well. Biomarker development and improved therapeutic tools have the potential to transform patient outcomes through treatment personalization and objective measure of neuroplasticity.
Collectively, there is a profound need consistency in methodologies of interventions for psychiatric disorders. Currently response and remission rates remain low which may be due in part to the lack of proper controls, highly variable treatment parameters, and lack of consistency among clinical symptoms of patients [92]. By combining functional and structural imaging tools, therapies can be tailored to the individual. These and other innovations described in the preceding sections will continue to drive the field forward and to create more effective and efficient treatments
References
Caporale N, Dan Y. Spike timing-dependent plasticity: a Hebbian learning rule. Annu Rev Neurosci. 2008;31:25–46.
Markram H, Lübke J, Frotscher M, Sakmann B. Regulation of synaptic efficacy by coincidence of postsynaptic APs and EPSPs. Science. 1997;275:213–5.
Markram H, Gerstner W, Sjöström PJ. A history of spike-timing-dependent plasticity. Front Synaptic Neurosci. 2011;3:4.
Malenka RC, Bear MF. LTP and LTD: an embarrassment of riches. Neuron. 2004;44:5–21.
Li F, Tsien JZ. Memory and the NMDA receptors. N Engl J Med. 2009;361:302–3.
Chater TE & Goda Y. The role of AMPA receptors in postsynaptic mechanisms of synaptic plasticity. Front. Cell. Neurosci. 2014;8:401.
von Bernhardi R, Bernhardi LE, Eugenín J. What is neural plasticity? Adv Exp Med Biol. 2017;1015:1–15.
Fauth M, Tetzlaff C. Opposing effects of neuronal activity on structural plasticity. Front Neuroanat. 2016;10:75.
de Faria O, Gonsalvez DG, Nicholson M, **ao J. Activity-dependent central nervous system myelination throughout life. J Neurochem. 2019;148:447–61.
Haroutunian V, Katsel P, Roussos P, Davis KL, Altshuler LL, Bartzokis G. Myelination, oligodendrocytes, and serious mental illness. Glia. 2014;62:1856–77.
Bonetto G, Kamen Y, Evans KA, Káradóttir RT. Unraveling myelin plasticity. Front Cell Neurosci. 2020;14:156.
Grossman AW, Churchill JD, McKinney BC, Kodish IM, Otte SL, Greenough WT. Experience effects on brain development: possible contributions to psychopathology. J Child Psychol Psychiatry. 2003;44:33–63.
Fatori D, Bordin IA, Curto BM, de Paula CS. Influence of psychosocial risk factors on the trajectory of mental health problems from childhood to adolescence: a longitudinal study. BMC Psychiatry. 2013;13:31.
Green CA, Perrin NA, Leo MC, Janoff SL, Yarborough BJ, Paulson RI. Recovery from serious mental illness: trajectories, characteristics, and the role of mental health care. Psychiatr Serv. 2013;64:1203–10.
Cramer SC, Sur M, Dobkin BH, O’Brien C, Sanger TD, Trojanowski JQ, et al. Harnessing neuroplasticity for clinical applications. Brain. 2011;134:1591–609.
Goodkind M, Eickhoff SB, Oathes DJ, Jiang Y, Chang A, Jones-Hagata LB, et al. Identification of a common neurobiological substrate for mental illness. JAMA Psychiatry. 2015;72:305–15.
Duman RS, Aghajanian GK, Sanacora G, Krystal JH. Synaptic plasticity and depression: new insights from stress and rapid-acting antidepressants. Nat Med. 2016;22:238–49.
Price JL, Drevets WC. Neurocircuitry of mood disorders. Neuropsychopharmacology. 2010;35:192–216.
Bora E, Fornito A, Pantelis C, Yücel M. Gray matter abnormalities in major depressive disorder: a meta-analysis of voxel based morphometry studies. J Affect Disord. 2012;138:9–18.
Kühn S, Gallinat J. Gray matter correlates of posttraumatic stress disorder: a quantitative meta-analysis. Biol Psychiatry. 2013;73:70–4.
Kaiser RH, Andrews-Hanna JR, Wager TD, Pizzagalli DA. Large-scale network dysfunction in major depressive disorder: a meta-analysis of resting-state functional connectivity. JAMA Psychiatry. 2015;72:603–11.
Akiki TJ, Averill CL, Abdallah CG. A network-based neurobiological model of PTSD: evidence from structural and functional neuroimaging studies. Curr Psychiatry Rep. 2017;19:81.
Lewis DA, González-Burgos G. Neuroplasticity of neocortical circuits in schizophrenia. Neuropsychopharmacology. 2008;33:141–65.
Balu DT, Coyle JT. Neuroplasticity signaling pathways linked to the pathophysiology of schizophrenia. Neurosci Biobehav Rev. 2011;35:848–70.
Nestler EJ. Is there a common molecular pathway for addiction? Nat Neurosci. 2005;8:1445–9.
Kalivas PW, O’Brien C. Drug addiction as a pathology of staged neuroplasticity. Neuropsychopharmacology. 2008;33:166–80.
Chen WR, Lee S, Kato K, Spencer DD, Shepherd GM, Williamson A. Long-term modifications of synaptic efficacy in the human inferior and middle temporal cortex. Proc Natl Acad Sci USA. 1996;93:8011–5.
Citri A, Malenka RC. Synaptic plasticity: multiple forms, functions, and mechanisms. Neuropsychopharmacology. 2008;33:18–41.
Guerra-Carrillo B, Mackey AP, Bunge SA. Resting-state fMRI: a window into human brain plasticity. Neuroscientist. 2014;20:522–33.
Kanaan RA, Kim JS, Kaufmann WE, Pearlson GD, Barker GJ, McGuire PK. Diffusion tensor imaging in schizophrenia. Biol Psychiatry. 2005;58:921–9.
Kubicki M, Westin CF, McCarley RW, Shenton ME. The application of DTI to investigate white matter abnormalities in schizophrenia. Ann N Y Acad Sci. 2005;1064:134–48.
Tymofiyeva O, Gaschler R. Training-induced neural plasticity in youth: a systematic review of structural and functional MRI studies. Front Hum Neurosci. 2020;14:497245.
Nathan PJ, Cobb SR, Lu B, Bullmore ET, Davies CH. Studying synaptic plasticity in the human brain and opportunities for drug discovery. Curr Opin Pharm. 2011;11:540–8.
Shaw P, Lerch JP, Pruessner JC, Taylor KN, Rose AB, Greenstein D, et al. Cortical morphology in children and adolescents with different apolipoprotein E gene polymorphisms: an observational study. Lancet Neurol. 2007;6:494–500.
Finnema SJ, Nabulsi NB, Eid T, Detyniecki K, Lin SF, Chen MK, et al. Imaging synaptic density in the living human brain. Sci Transl Med. 2016;8:348ra96.
Cai Z, Li S, Matuskey D, Nabulsi N, Huang Y. PET imaging of synaptic density: a new tool for investigation of neuropsychiatric diseases. Neurosci Lett. 2019;691:44–50.
Onwordi EC, Halff EF, Whitehurst T, Mansur A, Cotel MC, Wells L, et al. Synaptic density marker SV2A is reduced in schizophrenia patients and unaffected by antipsychotics in rats. Nat Commun. 2020;11:246.
Holmes SE, Finnema SJ, Naganawa M, DellaGioia N, Holden D, Fowles K, et al. Imaging the effect of ketamine on synaptic density (SV2A) in the living brain. Mol Psychiatry. 2022;27:2273–2281.
Becker, G., Dammicco, S., Bahri, M. A., & Salmon, E. The rise of synaptic density PET imaging. Molecules. 2020;25:2303–23.
Mercier J, Provins L, Valade A. Discovery and development of SV2A PET tracers: potential for imaging synaptic density and clinical applications. Drug Disco Today Technol. 2017;25:45–52.
de Vos CMH, Mason NL, Kuypers KPC. Psychedelics and neuroplasticity: a systematic review unraveling the biological underpinnings of psychedelics. Front Psychiatry. 2021;12:724606.
Leal G, Afonso PM, Salazar IL, Duarte CB. Regulation of hippocampal synaptic plasticity by BDNF. Brain Res. 2015;1621:82–101.
Holmes SE, Scheinost D, Finnema SJ, Naganawa M, Davis MT, DellaGioia N, et al. Lower synaptic density is associated with depression severity and network alterations. Nat Commun. 2019;10:1529.
Gray JD, McEwen BS. Lithium’s role in neural plasticity and its implications for mood disorders. Acta Psychiatr Scand. 2013;128:347–61.
El Hayek L, Khalifeh M, Zibara V, Abi Assaad R, Emmanuel N, Karnib N, et al. Lactate mediates the effects of exercise on learning and memory through SIRT1-dependent activation of hippocampal brain-derived neurotrophic factor (BDNF). J Neurosci. 2019;39:2369–82.
Béïque JC, Imad M, Mladenovic L, Gingrich JA, Andrade R. Mechanism of the 5-hydroxytryptamine 2A receptor-mediated facilitation of synaptic activity in prefrontal cortex. Proc Natl Acad Sci USA. 2007;104:9870–5.
Andrade R. Serotonergic regulation of neuronal excitability in the prefrontal cortex. Neuropharmacology. 2011;61:382–6.
Aghajanian GK, Marek GJ. Serotonin and hallucinogens. Neuropsychopharmacology. 1999;21:16S–23S.
Pillai A, Kale A, Joshi S, Naphade N, Raju MS, Nasrallah H, et al. Decreased BDNF levels in CSF of drug-naive first-episode psychotic subjects: correlation with plasma BDNF and psychopathology. Int J Neuropsychopharmacol. 2010;13:535–9.
Pillai A, Bruno D, Sarreal AS, Hernando RT, Saint-Louis LA, Nierenberg J, et al. Plasma BDNF levels vary in relation to body weight in females. PLoS ONE. 2012;7:e39358.
Brunoni AR, Lopes M, Fregni F. A systematic review and meta-analysis of clinical studies on major depression and BDNF levels: implications for the role of neuroplasticity in depression. Int J Neuropsychopharmacol. 2008;11:1169–80.
Ferreri F, Pasqualetti P, Määttä S, Ponzo D, Ferrarelli F, Tononi G, et al. Human brain connectivity during single and paired pulse transcranial magnetic stimulation. Neuroimage. 2011;54:90–102.
Stefan K, Kunesch E, Benecke R, Cohen LG, Classen J. Mechanisms of enhancement of human motor cortex excitability induced by interventional paired associative stimulation. J Physiol. 2002;543:699–708.
Rajji TK, Sun Y, Zomorrodi-Moghaddam R, Farzan F, Blumberger DM, Mulsant BH, et al. PAS-induced potentiation of cortical-evoked activity in the dorsolateral prefrontal cortex. Neuropsychopharmacology. 2013;38:2545–52.
Hadas I, Sun Y, Lioumis P, Zomorrodi R, Jones B, Voineskos D, et al. Association of repetitive transcranial magnetic stimulation treatment with subgenual cingulate hyperactivity in patients with major depressive disorder: a secondary analysis of a randomized clinical trial. JAMA Netw Open. 2019;2:e195578.
Hadas I, Zomorrodi R, Hill AT, Sun Y, Fitzgerald PB, Blumberger DM, et al. Subgenual cingulate connectivity and hippocampal activation are related to MST therapeutic and adverse effects. Transl Psychiatry. 2020;10:392.
Bashir S, Mizrahi I, Weaver K, Fregni F, Pascual-Leone A. Assessment and modulation of neural plasticity in rehabilitation with transcranial magnetic stimulation. PM R. 2010;2:S253–68.
Blumberger DM, Vila-Rodriguez F, Thorpe KE, Feffer K, Noda Y, Giacobbe P, et al. Effectiveness of theta burst versus high-frequency repetitive transcranial magnetic stimulation in patients with depression (THREE-D): a randomised non-inferiority trial. Lancet. 2018;391:1683–92.
Philip NS, Barredo J, Aiken E, Larson V, Jones RN, Shea MT, et al. Theta-burst transcranial magnetic stimulation for posttraumatic stress disorder. Am J Psychiatry. 2019;176:939–48.
Vékony T, Németh VL, Holczer A, Kocsis K, Kincses ZT, Vécsei L, et al. Continuous theta-burst stimulation over the dorsolateral prefrontal cortex inhibits improvement on a working memory task. Sci Rep. 2018;8:14835.
Di Lazzaro V, Pilato F, Dileone M, Profice P, Oliviero A, Mazzone P, et al. Low-frequency repetitive transcranial magnetic stimulation suppresses specific excitatory circuits in the human motor cortex. J Physiol. 2008;586:4481–7.
Beynel L, Powers JP, Appelbaum LG. Effects of repetitive transcranial magnetic stimulation on resting-state connectivity: a systematic review. Neuroimage. 2020;211:116596.
Fox MD, Buckner RL, White MP, Greicius MD, Pascual-Leone A. Efficacy of transcranial magnetic stimulation targets for depression is related to intrinsic functional connectivity with the subgenual cingulate. Biol Psychiatry. 2012;72:595–603.
Fox MD, Liu H, Pascual-Leone A. Identification of reproducible individualized targets for treatment of depression with TMS based on intrinsic connectivity. Neuroimage. 2013;66:151–60.
Hoffman RE, Hampson M, Wu K, Anderson AW, Gore JC, Buchanan RJ, et al. Probing the pathophysiology of auditory/verbal hallucinations by combining functional magnetic resonance imaging and transcranial magnetic stimulation. Cereb Cortex. 2007;17:2733–43.
Cash RFH, Cocchi L, Lv J, Fitzgerald PB, Zalesky A. Functional magnetic resonance imaging-guided personalization of transcranial magnetic stimulation treatment for depression. JAMA Psychiatry. 2021;78:337–39.
Cappon D, den Boer T, Jordan C, Yu W, Metzger E, Pascual-Leone A. Transcranial magnetic stimulation (TMS) for geriatric depression. Ageing Res Rev. 2022;74:101531.
Young JR, Smani SA, Mischel NA, Kritzer MD, Appelbaum LG, Patkar AA. Non-invasive brain stimulation modalities for the treatment and prevention of opioid use disorder: a systematic review of the literature. J Addict Dis. 2020;38:186–99.
Addicott MA, Luber B, Nguyen D, Palmer H, Lisanby SH, Appelbaum LG. Low- and high-frequency repetitive transcranial magnetic stimulation effects on resting-state functional connectivity between the postcentral gyrus and the insula. Brain Connect. 2019;9:322–28.
Pascual-Leone A, Tormos JM, Keenan J, Tarazona F, Cañete C, Catalá MD. Study and modulation of human cortical excitability with transcranial magnetic stimulation. J Clin Neurophysiol. 1998;15:333–43.
Speer AM, Kimbrell TA, Wassermann EM, D Repella J, Willis MW, Herscovitch P, et al. Opposite effects of high and low frequency rTMS on regional brain activity in depressed patients. Biol Psychiatry. 2000;48:1133–41.
Eisenegger C, Herwig U, Jäncke L. The involvement of primary motor cortex in mental rotation revealed by transcranial magnetic stimulation. Eur J Neurosci. 2007;25:1240–4.
Baghai TC, Möller HJ. Electroconvulsive therapy and its different indications. Dialogues Clin Neurosci. 2008;10:105–17.
Singh A, Kar SK. How electroconvulsive therapy works?: understanding the neurobiological mechanisms. Clin Psychopharmacol Neurosci. 2017;15:210–21.
Ota M, Noda T, Sato N, Okazaki M, Ishikawa M, Hattori K, et al. Effect of electroconvulsive therapy on gray matter volume in major depressive disorder. J Affect Disord. 2015;186:186–91.
McClintock SM, Choi J, Deng ZD, Appelbaum LG, Krystal AD, Lisanby SH. Multifactorial determinants of the neurocognitive effects of electroconvulsive therapy. J ECT. 2014;30:165–76.
Sun Y, Blumberger DM, Mulsant BH, Rajji TK, Fitzgerald PB, Barr MS, et al. Magnetic seizure therapy reduces suicidal ideation and produces neuroplasticity in treatment-resistant depression. Transl Psychiatry. 2018;8:253.
Månsson KN, Salami A, Frick A, Carlbring P, Andersson G, Furmark T, et al. Neuroplasticity in response to cognitive behavior therapy for social anxiety disorder. Transl Psychiatry. 2016;6:e727.
Seminowicz DA, Shpaner M, Keaser ML, Krauthamer GM, Mantegna J, Dumas JA, et al. Cognitive-behavioral therapy increases prefrontal cortex gray matter in patients with chronic pain. J Pain. 2013;14:1573–84.
Vinogradov S, Fisher M, de Villers-Sidani E. Cognitive training for impaired neural systems in neuropsychiatric illness. Neuropsychopharmacology. 2012;37:43–76.
Ramsay IS, Fryer S, Roach BJ, Boos A, Fisher M, Loewy R, et al. Response to targeted cognitive training may be neuroprotective in patients with early schizophrenia. Psychiatry Res Neuroimaging. 2021;312:111285.
Ramsay IS, Fryer S, Boos A, Roach BJ, Fisher M, Loewy R, et al. Response to targeted cognitive training correlates with change in thalamic volume in a randomized trial for early schizophrenia. Neuropsychopharmacology. 2018;43:590–97.
Barch DM, Carter CS, Braver TS, Sabb FW, MacDonald A, Noll DC, et al. Selective deficits in prefrontal cortex function in medication-naive patients with schizophrenia. Arch Gen Psychiatry. 2001;58:280–8.
Carter CS, Perlstein W, Ganguli R, Brar J, Mintun M, Cohen JD. Functional hypofrontality and working memory dysfunction in schizophrenia. Am J Psychiatry. 1998;155:1285–7.
Subramaniam K, Luks TL, Garrett C, Chung C, Fisher M, Nagarajan S, et al. Intensive cognitive training in schizophrenia enhances working memory and associated prefrontal cortical efficiency in a manner that drives long-term functional gains. Neuroimage. 2014;99:281–92.
Salgado JV, Sandner G. A critical overview of animal models of psychiatric disorders: challenges and perspectives. Braz J Psychiatry. 2013;35:S77–81.
Fu CHY, Fan Y, Davatzikos C. Addressing heterogeneity (and homogeneity) in treatment mechanisms in depression and the potential to develop diagnostic and predictive biomarkers. Neuroimage Clin. 2019;24:101997.
Zhou W, Xu Y, Lv Q, Sheng YH, Chen L, Li M, et al. Genetic association of olanzapine treatment response in Han Chinese schizophrenia patients. Front Pharm. 2019;10:177.
Tadić A, Müller-Engling L, Schlicht KF, Kotsiari A, Dreimüller N, Kleimann A, et al. Methylation of the promoter of brain-derived neurotrophic factor exon IV and antidepressant response in major depression. Mol Psychiatry. 2014;19:281–3.
Taylor JJ, Kurt HG, Anand A. Resting state functional connectivity biomarkers of treatment response in mood disorders: a review. Front Psychiatry. 2021;12:565136.
Wang A, Nikolin S, Moffa AH, Loo CK, Martin DM. A novel approach for targeting the left dorsolateral prefrontal cortex for transcranial magnetic stimulation using a cognitive task. Exp Brain Res. 2022;240:71–80.
Petrosino NJ, Cosmo C, Berlow YA, Zandvakili A, van ‘t Wout-Frank M, Philip NS. Transcranial magnetic stimulation for post-traumatic stress disorder. Ther Adv Psychopharmacol. 2021;11:20451253211049921.
Acknowledgements
The authors would like to thank Liam Lochhead for his valuable input during development of this paper.
Funding
Support was generously provided by the Kreutzkamp gift to UCSD to support the authors time in preparing this manuscript.
Author information
Authors and Affiliations
Contributions
LGA: conceptualization, investigation, resources, writing—original draft, writing—review and editing, supervision, project administration. MAS and LS: conceptualization, investigation, resources, writing—original draft, writing—review and editing. ZD: conceptualization, resources, writing—original draft, writing—review and editing, supervision, funding acquisition.
Corresponding author
Ethics declarations
Competing interests
ZD has received research and equipment in-kind support for an investigator-initiated study through Brainsway Inc and Magventure Inc. He is also on the scientific advisory board for Brainsway Inc. His work has been supported by the National Institutes of Mental Health (NIMH), the Canadian Institutes of Health Research (CIHR), Brain Canada and the Temerty Family and Grant Family Foundations. All other authors have no disclosures or conflicts of interest to report.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Appelbaum, L.G., Shenasa, M.A., Stolz, L. et al. Synaptic plasticity and mental health: methods, challenges and opportunities. Neuropsychopharmacol. 48, 113–120 (2023). https://doi.org/10.1038/s41386-022-01370-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-022-01370-w
- Springer Nature Switzerland AG
This article is cited by
-
A systematic review and meta-analysis of neuroimaging studies examining synaptic density in individuals with psychotic spectrum disorders
BMC Psychiatry (2024)
-
Quantitative Proteomic and Phosphoproteomic Analyses Reveal a Role of Death-Associated Protein Kinase 1 in Regulating Hippocampal Synapse
Molecular Neurobiology (2024)
-
Sleep is Essential for Mental Health: Potential Role of Slow Oscillations
Current Sleep Medicine Reports (2024)
-
Latent toxoplasmosis impairs learning and memory yet strengthens short-term and long-term hippocampal synaptic plasticity at perforant pathway-dentate gyrus, and Schaffer collatterals-CA1 synapses
Scientific Reports (2023)
-
Pre-clinical indications of brain stimulation treatments for non-affective psychiatric disorders, a status update
Translational Psychiatry (2023)