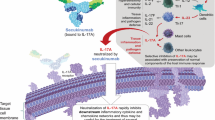
Abstract
Introduction
This study evaluated the efficacy of the interleukin-17A inhibitor secukinumab in patients with oligoarticular psoriatic arthritis (PsA).
Methods
A total of 84 patients with oligoarticular PsA, defined as 1–4 tender joints and 1–4 swollen joints, were pooled from the FUTURE 2–5 and MAXIMISE trials (NCT01752634, NCT01989468, NCT02294227, NCT02404350, and NCT02721966). Patients were grouped by treatment received at week 12 (secukinumab 300 mg, secukinumab 150 mg, or placebo) and week 52 (any secukinumab 300 mg or any secukinumab 150 mg). Efficacy was assessed by the proportion of patients achieving selected clinical outcomes. The predictors of Disease Activity index for Psoriatic Arthritis (DAPSA) responses at weeks 12 and 52 were identified by logistic regression analysis.
Results
Secukinumab treatment resulted in greater achievement of DAPSA-based low disease activity (LDA), DAPSA-based remission (REM), DAPSA50, and DAPSA75 than placebo at week 12, with improvements sustained or further increased through week 52. LDA or REM was achieved at week 52 by more than 90% of patients who received either secukinumab dose, although secukinumab 300 mg resulted in the highest achievement of the stringent DAPSA75 and DAPSA REM outcomes. At week 12, younger age was associated with DAPSA LDA or REM and DAPSA50, while lower baseline swollen joint count was associated with DAPSA REM. No predictors were identified at week 52. The safety profile was consistent with the full study populations.
Conclusion
Secukinumab demonstrated efficacy vs placebo across several outcome measures in patients with oligoarticular PsA at week 12, with sustained or improved responses through week 52.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
Oligoarticular psoriatic arthritis (PsA) occurs in approximately 50% of patients with PsA but has been underrepresented in clinical studies, particularly in registration trials of biologics. |
The objective of this analysis was to evaluate the clinical efficacy and safety of the interleukin-17A inhibitor secukinumab in patients with oligoarticular PsA using pooled data from five phase 3 studies. |
What was learned from the study? |
Patients with oligoarticular PsA who received secukinumab had greater improvements across multiple outcome measures, including minimal disease activity components and the stringent Disease Activity index for Psoriatic Arthritis (DAPSA) remission and DAPSA75 endpoints, than patients who received placebo at week 12; these responses were sustained through week 52. |
These results suggest that secukinumab treatment is safe and effective for patients with oligoarticular PsA. |
Introduction
Psoriatic arthritis (PsA) is a chronic inflammatory disease characterized by multiple musculoskeletal and dermatologic manifestations, including skin and nail changes, peripheral joint inflammation, enthesitis, dactylitis, and axial involvement [1, 2]. Oligoarticular PsA, defined as the involvement of ≤ 4 joints, is more commonly reported in early disease and can progress to polyarticular PsA if not adequately controlled with treatment [3]. Oligoarticular PsA affects a significant proportion of the PsA population and presents with similar clinical features and disease burden as polyarticular PsA, despite a lower number of joints involved [4, 5]. However, physician satisfaction with current therapies remains low; in some parts of the world, access to treatment is a significant challenge for patients with oligoarticular PsA [6, 7]. Because inclusion criteria of randomized controlled trials in PsA typically require elevated swollen and tender joint counts, the great majority of patients included in clinical trials have polyarticular PsA. There is currently a lack of evidence for the efficacy of biologics in patients with oligoarticular PsA.
In the updated 2019 European League Against Rheumatism (now known as the European Alliance of Associations for Rheumatology; EULAR) treatment guidelines for managing PsA, different treatment strategies were recommended for polyarticular vs oligoarticular PsA. Patients with polyarticular PsA should receive a conventional synthetic disease-modifying antirheumatic drug (csDMARD) as first-line treatment or after a short course of nonsteroidal anti-inflammatory drugs, while patients with oligoarticular PsA should receive first-line csDMARD treatment if poor prognostic factors are present, such as structural damage, high erythrocyte sedimentation rate or C-reactive protein (CRP), dactylitis, or nail involvement [8]. However, the EULAR guidelines for oligoarticular PsA were based on expert opinion because of a lack of clinical data for oligoarticular PsA. The clinical data that are available show mixed efficacy results for csDMARD treatment in patients with oligoarticular vs polyarticular PsA and interpretation of efficacy may depend on the clinical outcome measure used [9, 10].
Secukinumab is an interleukin (IL)-17A inhibitor that has demonstrated early and sustained efficacy with a favorable safety profile in psoriasis, PsA, ankylosing spondylitis, and nonradiographic axial spondyloarthritis [11,12,13,14,15,16]. However, like most biologics, the efficacy of secukinumab in patients with oligoarticular PsA is a clinically relevant question. Additionally, methods for optimally measuring treatment response in this patient population are not well determined.
To overcome the limitations of common clinical trial inclusion criteria that result in most enrolled patients displaying a polyarticular PsA phenotype, patient data were pooled for patients with < 5 tender and swollen joints among the secukinumab phase 3 PsA clinical trial program. This analysis evaluates the clinical efficacy and safety of secukinumab treatment for patients with oligoarticular PsA using pooled data from five phase 3 studies.
Methods
Study Design and Patient Population
This post hoc analysis included patients with active oligoarticular PsA from the phase 3/3b FUTURE 2–5 and MAXIMISE trials (NCT01752634, NCT01989468, NCT02294227, NCT02404350, and NCT02721966; Supplementary Material Fig. S1) [17,18,19,20,21]. Oligoarticular PsA was defined as the presence at baseline of 1–4 tender joints as measured by the tender joint count of 78 joints (TJC78) and 1–4 swollen joints as measured by the swollen joint count of 76 joints (SJC76). In the FUTURE 2–5 studies, patients aged ≥ 18 years who met the ClASsification criteria for Psoriatic ARthritis (CASPAR) and had active disease with ≥ 3 tender joints and ≥ 3 swollen joints despite treatment with nonsteroidal anti-inflammatory drugs were included. The MAXIMISE study included patients diagnosed with active PsA who met the CASPAR criteria, regardless of the number of swollen or tender joints. Patients also had active spinal disease with a Bath Ankylosing Spondylitis Disease Activity Index score ≥ 4 and spinal pain score ≥ 40 by a 100-mm visual analogue score (VAS).
Treatment groups assessed here included patients who received secukinumab 300 mg (n = 23), secukinumab 150 mg with or without a subcutaneous loading dose (n = 30), or placebo (n = 31) at week 12 and any secukinumab 300 mg (n = 35) or any secukinumab 150 mg (n = 49) at week 52. Week 12 was the last visit at which patients in all studies received placebo. Patients initially randomized to placebo were switched to secukinumab 300 mg or 150 mg at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5. The primary studies were approved by each central institutional review board and the ethics review boards of each additional center that participated in the individual studies. All included studies were performed in accordance with the Helsinki Declaration of 1964 and its later amendments, and written informed consent was obtained from all participants before study inclusion.
Assessments and Outcomes
The efficacy of secukinumab at weeks 12 and 52 was assessed by the proportion of patients achieving 50% or 75% improvement in Disease Activity index for Psoriatic Arthritis (DAPSA50/75) scores, DAPSA-based low disease activity (LDA; defined as DAPSA ≤ 14) or remission (REM; defined as DAPSA ≤ 4), 50% or 75% improvement in clinical DAPSA (cDAPSA50/75), cDAPSA-based LDA (cDAPSA ≤ 13) or cDAPSA-based REM (cDAPSA ≤ 4), and resolution of tender joint count (TJC78 = 0) and swollen joint count (SJC76 = 0).
Quality of life improvements were evaluated using patient-reported outcomes (PROs) at weeks 12 and 52. Physical function was assessed by achievement of the minimal clinically important difference (MCID) of ≥ 0.35 in the Health Assessment Questionnaire Disability Index (HAQ-DI; scale, 0–3). Fatigue was evaluated by achievement of the MCID of ≥ 4 in the Functional Assessment of Chronic Illness Therapy–Fatigue (FACIT-F; scale, 0–52). The mean change from baseline in FACIT-F was also determined at weeks 12 and 52. Pain and patient global assessment of disease activity were evaluated by mean change from baseline using a 100-mm VAS at weeks 12 and 52.
Because the MAXIMISE trial did not assess Psoriasis Area and Severity Index (PASI) scores or body surface area (BSA) affected by psoriasis, psoriasis-related assessments could not be included in a complete analysis of minimal disease activity (MDA) achievement. Instead, the achievement of individual components of a modified MDA (mMDA) index was assessed at weeks 12 and 52. The assessed mMDA components included TJC78 ≤ 1 among patients with baseline TJC78 > 1, SJC76 ≤ 1 among patients with baseline SJC76 > 1, total tender or swollen entheseal points ≤ 1 among patients with baseline total > 1, HAQ-DI score ≤ 0.5 among patients with baseline score > 0.5, PsA pain (VAS, 0–100) ≤ 15 among patients with baseline score > 15, and patient global assessment of disease activity (VAS, 0–100) ≤ 20 among patients with baseline score > 20.
Safety was assessed by the incidence of treatment-emergent adverse events (AEs), serious AEs, and discontinuation of treatment due to AE through weeks 12 and 52.
Statistical Analyses
Descriptive statistics are provided for each endpoint using an observed case approach. For binary and continuous outcome measures, no statistical hypothesis tests were planned in the protocol and none were performed. Unadjusted logistic regression analysis was used to identify potential predictors of DAPSA responses at weeks 12 and 52; multiple logistic regression analyses were performed thereafter.
Results
Baseline Characteristics
In total, 84 patients were included in this pooled analysis: 48 patients with active PsA from the FUTURE 2–5 trials and 36 patients with active PsA and axial manifestations from the MAXIMISE trial. Baseline demographics and disease characteristics were similar between treatment groups (Table 1). Patients with oligoarticular PsA had a mean (SD) disease duration of 4.2 (5.5) years and a mean (SD) baseline DAPSA score of 17.4 (4.7).
Efficacy
At week 12, patients who received secukinumab had higher DAPSA-based response rates than patients who received placebo (Fig. 1a). A higher proportion of patients who received secukinumab 300 mg or secukinumab 150 mg achieved DAPSA50 (65.2% and 44.4%, respectively) and DAPSA LDA or REM (82.6% and 78.6%, respectively) than placebo (30.0% and 56.7%, respectively). Additionally, more patients who received secukinumab 300 mg or secukinumab 150 mg achieved the higher-hurdle DAPSA75 (52.2% and 14.8%, respectively) and DAPSA REM (43.5% and 21.4%, respectively) endpoints than placebo (6.7% for both DAPSA75 and DAPSA REM). These improvements in DAPSA responses were sustained or further increased through week 52 in patients receiving either dose of secukinumab (Fig. 1b). At week 52, a higher proportion of patients who received any secukinumab 300 mg vs any secukinumab 150 mg achieved DAPSA75 (58.1% vs 43.6%) and DAPSA REM (61.3% vs 37.5%) (Fig. 1b). Similarly, the proportion of patients who achieved cDAPSA50, cDAPSA75, and cDAPSA-based LDA or REM was higher among patients who received secukinumab than placebo at week 12, and these improvements were sustained or further increased through week 52 (Supplementary Material Fig. S2). The proportion of patients who achieved each cDAPSA-based response was similar to the corresponding DAPSA-based response across treatment groups (Fig. 1, Supplementary Material Fig. S2). More than 90% of patients who received any secukinumab 300 mg or any secukinumab 150 mg achieved at least LDA at week 52 as measured by both DAPSA and cDAPSA. At week 52, cDAPSA REM and DAPSA REM were achieved by higher proportions of patients who received secukinumab 300 mg (59.4% and 61.3%, respectively) than secukinumab 150 mg (42.5% and 37.5%, respectively). Similarly, cDAPSA75 and DAPSA75 were achieved by higher proportions of patients who received secukinumab 300 mg (56.3% and 58.1%, respectively) than secukinumab 150 mg (43.6% for both cDAPSA75 and DAPSA75).
Proportion of patients with oligoarticular PsA achieving DAPSA responses at a week 12 and b week 52 (observed). DAPSA Disease Activity index for Psoriatic Arthritis, LDA low disease activity, PsA psoriatic arthritis, REM remission. aDAPSA LDA + REM is defined as DAPSA ≤ 14. bDAPSA REM is defined as DAPSA ≤ 4. cIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 300 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5). dIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 150 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5)
Patients who received secukinumab had greater improvements in musculoskeletal disease activity as determined by the achievement of TJC and SJC resolution than patients who received placebo (Fig. 2). At week 12, the proportion of patients who achieved TJC or SJC resolution was higher among patients who received secukinumab 300 mg (52.2% and 69.6%, respectively) or secukinumab 150 mg (40.0% and 60.0%, respectively) than placebo (12.9% and 45.2%, respectively). These improvements were sustained or further increased through week 52 in patients receiving either dose of secukinumab.
Proportion of patients with oligoarticular PsA achieving resolution of TJC and resolution of SJC at a week 12 and b week 52 (observed). PsA psoriatic arthritis, SJC swollen joint count, SJC76 swollen joint count of 76 joints, TJC tender joint count, TJC78 tender joint count of 78 joints. aIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 300 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5). bIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 150 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5)
Greater improvements in PROs were seen in patients who received secukinumab vs placebo (Fig. 3, Supplementary Material Fig. S3). At week 12, a higher proportion of patients who received secukinumab 300 mg or secukinumab 150 mg achieved the MCID of ≥ 0.35-point improvement in HAQ-DI (60.9% or 55.2%, respectively) than patients receiving placebo (38.7%) (Fig. 3). Similarly, more patients who received secukinumab 300 mg or secukinumab 150 mg achieved the MCID of ≥ 4-point improvement in FACIT-F at week 12 (60.9% and 62.1%, respectively) than those receiving placebo (51.6%). These HAQ-DI and FACIT-F responses were sustained or further increased through week 52 in patients receiving either dose of secukinumab.
Proportion of patients with oligoarticular PsA achieving a ≥ 0.35-point HAQ-DI score improvement and a ≥ 4-point FACIT-F score improvement at a week 12 and b week 52 (observed). FACIT-F Functional Assessment of Chronic Illness Therapy–Fatigue, HAQ-DI Health Assessment Questionnaire Disability Index, PsA psoriatic arthritis. aIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 300 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5). bIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 150 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5)
At week 12, patients who received secukinumab had greater improvements in FACIT-F, patient global assessment, and PsA pain than patients who received placebo (Supplementary Material Fig. S3); in general, the greatest improvements were observed in those who received secukinumab 300 mg compared with either secukinumab 150 mg or placebo. Improvements observed with secukinumab treatment were sustained or further increased through week 52.
Patients who received secukinumab 300 mg had greater achievement of all individual mMDA components at week 12 than patients who received placebo (Fig. 4a). The largest differences in treatment effects between secukinumab 300 mg and placebo were in the proportion of patients who achieved patient global assessment ≤ 20 (57.1% vs 28.0%), PsA pain ≤ 15 (54.5% vs 20.0%), and SJC76 ≤ 1 (80.0% vs 69.6%). A numerically greater proportion of patients who received secukinumab 300 mg than secukinumab 150 mg achieved all individual mMDA components except for tender or swollen entheseal points ≤ 1 at week 12. At week 52, a greater proportion of patients who received secukinumab 300 mg compared with those who received secukinumab 150 mg achieved HAQ-DI ≤ 0.50 (68.0% vs 44.4%), PsA pain ≤ 15 (70.0% vs 48.6%), and patient global assessment ≤ 20 (75.9% vs 54.1%) (Fig. 4b).
Proportion of patients with oligoarticular PsA achieving individual MDA components at a week 12 and b week 52 (observed)a. HAQ-DI Health Assessment Questionnaire Disability Index, MDA minimal disease activity, PBO placebo, PsA psoriatic arthritis, SEC secukinumab, SJC76 swollen joint count of 76 joints, TJC78 tender joint count of 78 joints. aIn these radar plots, greater distance from the origin corresponds to a greater proportion of patients achieving clinical response. bAmong patients with counts > 1 at baseline. cAmong patients with baseline HAQ-DI > 0.5. dAmong patients with baseline PsA pain > 15. eAmong patients with baseline patient global assessment > 20. fIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 300 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5). gIncludes patients initially randomized to receive placebo who were re-randomized to secukinumab 150 mg after week 12 (re-randomization occurred at week 12 in MAXIMISE and week 16 or 24 in FUTURE 2–5)
Predictors of Clinical Response
Several demographic and baseline disease characteristics were found to be potential predictors of DAPSA responses at week 12 (Fig. 5). Younger age at baseline was consistently found to be associated with achievement of all DAPSA outcome measures assessed at week 12. Lower baseline disease activity as measured by SJC76, DAPSA, and cDAPSA was associated with increased achievement of DAPSA REM at week 12. Male sex and lower baseline SJC76 were associated with greater achievement of DAPSA50 response at week 12. No potential predictors of DAPSA responses were identified at week 52.
Predictors of clinical response at week 12. cDAPSA clinical Disease Activity index for Psoriatic Arthritis, DAPSA Disease Activity index for Psoriatic Arthritis, LDA low disease activity, REM remission, SJC76 swollen joint count of 76 joints. aDAPSA LDA + REM is defined as DAPSA ≤ 14. bDAPSA REM is defined as DAPSA ≤ 4
Safety
The safety profile of secukinumab in patients with oligoarticular PsA was consistent with that reported in the full populations from the FUTURE 2–5 and MAXIMISE trials (Supplementary Material Tables S1 and S2) [17,18,19,20,21]. The most frequently reported AEs through week 12 for patients receiving secukinumab 300 mg, secukinumab 150 mg, and placebo, respectively, were nasopharyngitis (8.7%, 6.7%, and 6.5%), nausea (0%, 3.3%, and 6.5%), vomiting (0%, 3.3%, and 6.5%), and upper respiratory tract infections (4.3%, 0%, and 6.5%) (Supplementary Material Table S1). Through week 12, one serious AE was reported in a patient who received secukinumab 300 mg. No patients from any treatment group discontinued treatment because of AEs through week 12.
Through week 52, the most frequently reported AEs for patients receiving any secukinumab 300 mg and any secukinumab 150 mg, respectively, were nasopharyngitis (20.0% and 10.2%), otitis externa (5.7% and 6.1%), psoriatic arthropathy (2.9% and 8.2%), and upper respiratory tract infections (8.6% and 4.1%) (Supplementary Material Table S2). Serious AEs were reported in four patients (11.4%) who received any secukinumab 300 mg and seven patients (14.3%) who received any secukinumab 150 mg. Over the entire 52-week treatment period, AEs leading to treatment discontinuation were reported in one patient (2.9%) who received any secukinumab 300 mg and in three patients (6.1%) who received any secukinumab 150 mg.
Discussion
In this post hoc analysis of patients with oligoarticular PsA from the FUTURE 2–5 and MAXIMISE trials, secukinumab provided rapid and sustained improvements in signs and symptoms across a range of outcome measures. In particular, over 90% of patients who received any secukinumab achieved at least DAPSA LDA at week 52, and the higher-hurdle endpoints of DAPSA75 and DAPSA REM were achieved by over half of patients who received secukinumab 300 mg. Taken together, these results suggest that secukinumab treatment results in improvements across multiple outcome measures in patients with oligoarticular PsA. The current study adds important efficacy data for this patient population that has been underrepresented in clinical trials, which could support more tailored treatment guidelines for patients with oligoarticular PsA, as additional data become available.
Phase 3 clinical trials of biologics typically include patients with PsA and substantial burden of articular involvement as suggested by an elevated tender and swollen joint count, which limits the generalizability of these findings to a broader population of patients with PsA, including those with oligoarticular disease. The inclusion criteria for the FUTURE trials required ≥ 3 tender joints and ≥ 3 swollen joints at baseline; therefore, in order to analyze the efficacy of secukinumab in patients with oligoarticular PsA it was necessary to pool patient data from the FUTURE 2–5 trials with those with ≥ 1 swollen and ≥ 1 tender joints from MAXMISE, where swollen and tender joint counts were not among the inclusion criteria.
For the current analysis, we defined a FACIT-F response as an improvement of ≥ 4 from baseline. Although this threshold has previously been validated and used to define FACIT-F response in patients with PsA [22, 23], it has not been specifically validated in patients with oligoarticular PsA. Additionally, the DAPSA50/75 endpoints used here have not been validated in patients with oligoarticular PsA.
The relevance of identifying clinical factors or baseline disease characteristics that could predict long-term treatment response is well established [24], particularly among patients with oligoarticular joint involvement who are underrepresented in clinical research. Previous studies identified factors that could predict achievement of MDA in response to tumor necrosis factor inhibitors across diverse populations of patients with PsA; these factors include younger age, male sex, lower functional impairment and disease activity at baseline, and greater general well-being as assessed by patient global assessment [24]. In the current analysis of patients with oligoarticular PsA, younger age was identified as a predictor of LDA, REM, and DAPSA50 at week 12 in patients receiving secukinumab, potentially as a result of higher functional impairment and chronic pain from other causes that may be present in older age groups. Other predictors of DAPSA REM or DAPSA50 identified here include lower baseline disease severity measures (DAPSA, cDAPSA, and SJC76) and male sex. These are also predictors for better response in patients with polyarticular disease, demonstrating the similarity between oligoarticular and polyarticular PsA. However, these results should be interpreted with caution due to the limited number of patients included in the present analysis and the diverse settings of the pooled clinical trials. cDAPSA is a clinical version of DAPSA that includes all individual DAPSA components except CRP and has been shown to correlate with DAPSA-based assessment of disease activity [25]. Measuring CRP in a clinical setting might be challenging and is used by only 35% of rheumatologists and dermatologists in the USA to monitor disease activity [26], which makes cDAPSA a useful alternative for some populations in an outpatient setting [25]. Furthermore, DAPSA and cDAPSA measures have been found to be similar in patients with PsA, indicating little added value of including CRP measurements [25, 27]. Here we show good agreement between the proportion of patients who achieved DAPSA- and cDAPSA-based categorical responses for every treatment group, in line with previous research.
MDA is a validated treatment target for PsA that is defined by low or no disease activity across a number of criteria, including tender joint count, swollen joint count, number of tender entheseal points, PASI or BSA, patient assessment of pain, patient global assessment of disease activity, and HAQ-DI [24]. However, as the MAXIMISE trial did not assess PASI or BSA, a modified MDA that assessed all of the components of MDA except PASI or BSA was used. Although a higher percentage of patients who received secukinumab achieved TJC78 ≤ 1 and SJC76 ≤ 1 at week 12 compared with patients who received placebo, the relatively smaller difference most likely reflects the lower baseline TJC and SJC in patients with oligoarticular PsA.
There were several limitations to this study that could impact the interpretation of these results. No statistical hypothesis tests were planned for this analysis, and none were performed. Further clinical trials that include a large number of patients with oligoarticular PsA are needed to rigorously evaluate differences between the efficacy of secukinumab versus placebo. Despite pooling data from five clinical trials for this analysis, the overall number of patients that met the definition of oligoarticular PsA was still limited. The majority of patients included in this analysis had 3–4 tender and swollen joints at baseline; patients with 1–2 tender and swollen joints are still underrepresented in this analysis. While patients who had 1–2 tender and swollen joints were enrolled in MAXIMISE, the study inclusion criteria required that these patients also have active axial manifestations. Therefore, these patients may not be representative of the real-world population of patients with oligoarticular PsA. Additionally, pooling data from clinical trials under variable settings can present analytical challenges [28, 29].
Conclusions
In patients with oligoarticular PsA, secukinumab reduced disease activity across a range of outcome measures by week 12, with sustained responses through 52 weeks. Secukinumab 300 mg may provide additional clinical benefit compared with 150 mg in achieving higher-hurdle efficacy outcome measures such as LDA or REM. The safety profile of secukinumab observed here in patients with oligoarticular PsA was consistent with that reported in the full populations from the FUTURE 2–5 and MAXIMISE trials.
References
Coates LC, Helliwell PS. Psoriatic arthritis: state of the art review. Clin Med (Lond). 2017;17(1):65–70.
Ritchlin CT, Colbert RA, Gladman DD. Psoriatic arthritis. N Engl J Med. 2017;376(10):957–70.
Marchesoni A. Oligoarticular psoriatic arthritis: addressing clinical challenges in an intriguing phenotype. Rheumatol Ther. 2018;5(2):311–6.
Gladman DD, Ye JY, Chandran V, Lee KA, Cook RJ. Oligoarticular vs polyarticular psoriatic arthritis: a longitudinal study showing similar characteristics. J Rheumatol. 2021;48(12):1824–9.
Ogdie A, Weiss P. The epidemiology of psoriatic arthritis. Rheum Dis Clin N Am. 2015;41(4):545–68.
Cividino A, Nicholson D, Guindi S, Jelley J, Gaudreau AJ, Gladman D. Clinical presentation and treatment of oligoarticular psoriatic arthritis in Canada: high frequency of smaller joint involvement [abstract]. Arthritis Rheumatol 2019;71(Suppl 10).
van Mens LJJ, van de Sande MGH, Fluri IA, Atiqi S, van Kuijk AWR, Baeten DLP. Residual disease activity and treatment adjustments in psoriatic arthritis in current clinical practice. Arthritis Res Ther. 2017;19(1):226.
Gossec L, Baraliakos X, Kerschbaumer A, et al. EULAR recommendations for the management of psoriatic arthritis with pharmacological therapies: 2019 update. Ann Rheum Dis. 2020;79(6):700–12.
Coates LC, Helliwell PS. Methotrexate efficacy in the tight control in psoriatic arthritis study. J Rheumatol. 2016;43(2):356–61.
Kingsley GH, Kowalczyk A, Taylor H, et al. A randomized placebo-controlled trial of methotrexate in psoriatic arthritis. Rheumatology (Oxford). 2012;51(8):1368–77.
Langley RG, Elewski BE, Lebwohl M, et al. Secukinumab in plaque psoriasis–results of two phase 3 trials. N Engl J Med. 2014;371(4):326–38.
Blauvelt A, Prinz JC, Gottlieb AB, et al. Secukinumab administration by pre-filled syringe: efficacy, safety and usability results from a randomized controlled trial in psoriasis (FEATURE). Br J Dermatol. 2015;172(2):484–93.
Paul C, Lacour JP, Tedremets L, et al. Efficacy, safety and usability of secukinumab administration by autoinjector/pen in psoriasis: a randomized, controlled trial (JUNCTURE). J Eur Acad Dermatol Venereol. 2015;29(6):1082–90.
Mease PJ, McInnes IB, Kirkham B, et al. Secukinumab inhibition of interleukin-17A in patients with psoriatic arthritis. N Engl J Med. 2015;373(14):1329–39.
Baeten D, Sieper J, Braun J, et al. Secukinumab, an interleukin-17A inhibitor, in ankylosing spondylitis. N Engl J Med. 2015;373(26):2534–48.
Deodhar A, Blanco R, Dokoupilová E, et al. Improvement of signs and symptoms of nonradiographic axial spondyloarthritis in patients treated with secukinumab: primary results of a randomized, placebo-controlled phase III study. Arthritis Rheumatol. 2021;73(1):110–20.
McInnes IB, Mease PJ, Ritchlin CT, et al. Secukinumab sustains improvement in signs and symptoms of psoriatic arthritis: 2 year results from the phase 3 FUTURE 2 study. Rheumatology (Oxford). 2017;56(11):1993–2003.
Nash P, Mease PJ, McInnes IB, et al. Efficacy and safety of secukinumab administration by autoinjector in patients with psoriatic arthritis: results from a randomized, placebo-controlled trial (FUTURE 3). Arthritis Res Ther. 2018;20(1):47.
Kivitz A, Nash P, Tahir H, et al. Arthritis: primary results through 52 weeks from a phase-3 randomized placebo-controlled study (FUTURE 4) [abstract]. J Clin Rheumatol. 2018;24(S3):364.
Mease P, van der Heijde D, Landewé R, et al. Secukinumab improves active psoriatic arthritis symptoms and inhibits radiographic progression: primary results from the randomised, double-blind, phase III FUTURE 5 study. Ann Rheum Dis. 2018;77(6):890–7.
Baraliakos X, Gossec L, Pournara E, et al. Secukinumab in patients with psoriatic arthritis and axial manifestations: results from the double-blind, randomised, phase 3 MAXIMISE trial. Ann Rheum Dis. 2021;80:582–90.
Rahman P, Mease PJ, Helliwell PS, et al. Guselkumab demonstrated an independent treatment effect in reducing fatigue after adjustment for clinical response-results from two phase 3 clinical trials of 1120 patients with active psoriatic arthritis. Arthritis Res Ther. 2021;23(1):190.
Cella D, Wilson H, Shalhoub H, et al. Content validity and psychometric evaluation of Functional Assessment of Chronic Illness Therapy-Fatigue in patients with psoriatic arthritis. J Patient Rep Outcomes. 2019;3(1):30.
Gossec L, McGonagle D, Korotaeva T, et al. Minimal disease activity as a treatment target in psoriatic arthritis: a review of the literature. J Rheumatol. 2018;45(1):6–13.
Gonçalves RSG, de Almeida Martins LM, de Ataide MH, Dantas AT, Duarte ALBP. DAPSA versus cDAPSA: do we need to use CRP? Ann Rheum Dis. 2020;79(11):e142.
Ogdie A, Tillett W, Booth N, et al. Usage of C-reactive protein testing in the diagnosis and monitoring of psoriatic arthritis (PsA): results from a real-world survey in the USA and Europe. Rheumatol Ther. 2022;9(1):285–93.
van Mens LJJ, van de Sande MGH, van Kuijk AWR, Baeten D, Coates LC. Ideal target for psoriatic arthritis? Comparison of remission and low disease activity states in a real-life cohort. Ann Rheum Dis. 2018;77(2):251–7.
Wilkinson T, Sinha S, Peek N, Geifman N. Clinical trial data reuse—overcoming complexities in trial design and data sharing. Trials. 2019;20(1):513.
Bangdiwala SI, Bhargava A, O’Connor DP, et al. Statistical methodologies to pool across multiple intervention studies. Transl Behav Med. 2016;6(2):228–35.
Acknowledgements
The authors would like to thank **angyi Meng for his assistance with statistical analysis of the results and with drafting and reviewing the manuscript.
Funding
This study was sponsored by Novartis Pharmaceuticals Corporation, East Hanover, NJ. Support for third-party writing assistance for this manuscript and funding for the journal’s Rapid Service Fee was provided by Novartis.
Medical Writing, Editorial, and Other Assistance
Medical writing support was provided by Ken Gresham, PhD, of Health Interactions, Inc., and was funded by Novartis Pharmaceuticals Corporation. This manuscript was developed in accordance with Good Publication Practice (GPP 2022) guidelines (http://www.ismpp.org/gpp3). Authors had full control of the content and made the final decision on all aspects of this publication.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Author Contributions
Alexis Ogdie, Dafna D. Gladman, Laura C. Coates, Effie Pournara, Bhumik Parikh, and Philip J. Mease contributed to the design of this study, data analysis and interpretation, and drafting of the manuscript.
Prior Presentation
A portion of these results were previously presented online at ACR Convergence 2021; November 3–10, 2021 (Poster 1825).
Disclosures
Alexis Ogdie has received consulting fees from Amgen, AbbVie, Bristol Myers Squibb, Celgene, CorEvitas, Eli Lilly, Gilead, GSK, Happify Health, Janssen, Novartis, Pfizer, and UCB, and has received grant support from the National Institutes of Health/National Institute of Arthritis and Musculoskeletal and Skin Diseases, Rheumatology Research Foundation, National Psoriasis Foundation, Amgen, Pfizer, and Novartis. Dafna D. Gladman has received research grant support from AbbVie, Amgen, Celgene, Eli Lilly, Novartis, Pfizer, and UCB, and consulting fees from AbbVie, Amgen, Bristol Myers Squibb, Celgene, Eli Lilly, Galapagos, Gilead, Janssen, Novartis, Pfizer, and UCB. Laura C. Coates has received grants/research support from AbbVie, Amgen, Celgene, Eli Lilly, Janssen, Novartis, Pfizer, and UCB; has worked as a paid consultant for AbbVie, Amgen, Boehringer Ingelheim, Bristol Myers Squibb, Celgene, Eli Lilly, Gilead, Galapagos, Janssen, MoonLake, Novartis, Pfizer, and UCB; and has been paid as a speaker for AbbVie, Amgen, Biogen, Celgene, Eli Lilly, Galapagos, Gilead, GSK, Janssen, Medac, Novartis, Pfizer, and UCB. Effie Pournara is an employee and shareholder of Novartis Pharma AG. Bhumik Parikh was an employee and stockholder of Novartis at the time of this analysis and is currently an employee of AbbVie. Philip J. Mease has received research grants from AbbVie, Amgen, Bristol Myers Squibb, Celgene, Eli Lilly, Gilead, Janssen, Novartis, Pfizer, Sun Pharma, and UCB; consulting fees from AbbVie, Amgen, Boehringer Ingelheim, Bristol Myers Squibb, Celgene, Eli Lilly, Galapagos, Gilead, GlaxoSmithKline, Janssen, Novartis, Pfizer, Sun Pharma, and UCB; and speakers bureau fees from AbbVie, Amgen, Eli Lilly, Janssen, Novartis, Pfizer, and UCB.
Compliance with Ethics Guidelines
The primary studies were approved by each central institutional review board and the ethics review boards of each additional center that participated in the individual studies. All included studies were performed in accordance with the Helsinki Declaration of 1964 and its later amendments, and written informed consent was obtained from all participants before study inclusion.
Data Availability
All data generated or analyzed during this study are included in this article or uploaded as supplementary information.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Ogdie, A., Gladman, D.D., Coates, L.C. et al. Inhibition of Interleukin-17 in Patients with Oligoarticular Psoriatic Arthritis. Rheumatol Ther 10, 849–860 (2023). https://doi.org/10.1007/s40744-023-00548-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40744-023-00548-y