Abstract
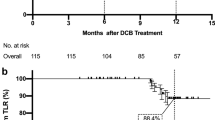
The Academic Research Consortium (ARC) recently published a definition of patients at high bleeding risk (HBR) undergoing percutaneous coronary intervention. However, the prevalence of the ARC-HBR criteria in patients undergoing endovascular therapy (EVT) for femoropopliteal arterial lesions has not been thoroughly investigated. The study population comprised 165 patients undergoing initial EVT for femoropopliteal lesions between June 2018 and June 2020. They were divided into two groups according to the ARC-HBR criteria. The primary end point was a composite of all-cause death, Bleeding Academic Research Consortium type 3 or 5 bleeding, and target lesion revascularization (TLR) within 2 years of EVT. The 165 patients were divided into two groups: 125 (75.8%) patients at HBR (HBR group) and 40 (24.2%) patients at no HBR (non-HBR group). The cumulative incidence of the primary endpoint was significantly higher in the HBR group than in the non-HBR group (40.6% vs. 0%, log-rank p < 0.001). The HBR group had a significantly higher risk of all-cause death, major bleeding, and TLR than the non-HBR group (25.2% vs. 0%, log-rank p = 0.004, 13.9% vs. 0%, log-rank p = 0.047, 16.8% vs. 0%, log-rank p = 0.035). Most patients with peripheral artery disease were classified as HBR patients, and HBR patients were at higher risk of death, major bleeding, and TLR than non-HBR patients.
Graphical abstract





Similar content being viewed by others
Data availability
The database generated during the current study are available from the corresponding author on reasonable request.
References
Bhardwaj B, Spertus JA, Kennedy KF, Jones WS, Safey D, Tsai TT, et al. Bleeding complications in lower-extremity peripheral vascular interventions: insights from the NCDR PVI registry. JACC Cardiovasc Interv. 2019;12:1140–9.
Urban P, Mehran R, Colleran R, Angiolillo DJ, Byrne RA, Capodanno D, et al. Defining high bleeding risk in patients undergoing percutaneous coronary intervention: a consensus document from the Academic Research Consortium for High Bleeding Risk. Eur Heart J. 2019;40:2632–53.
Cao D, Mehran R, Dangas G, Baber U, Sartori S, Chandiramani R, et al. Validation of the Academic Research Consortium high bleeding risk defnition in contemporary PCI patients. J Am Coll Cardiol. 2020;75:2711–22.
Natsuaki M, Morimoto T, Shiomi H, Yamaji K, Watanabe H, Shizuta S, et al. Application of the Academic Research Consortium high bleeding risk criteria in an all-comers registry of percutaneous coronary intervention. Circ Cardiovasc Interv. 2019;12(11):e008307.
Miura K, Shimada T, Ohya M, Murai R, Amano H, Kubo S, et al. Prevalence of the academic research consortium for high bleeding risk criteria and prognostic value of a simplifed defnition. Circ J. 2020;84:1560–7.
Nakamura M, Kadota K, Nakao K, Nakagawa Y, Shite J, Yokoi H, et al. High bleeding risk and clinical outcomes in East Asian patients undergoing percutaneous coronary intervention: the PENDULUM Registry. EuroIntervention. 2021;16:1154–62.
Shima Y, Miura K, Shimada T, Ohya M, Murai R, Kubo S, et al. Impact of ischemic risk factors on long-term outcomes in patients with and without high bleeding risk. Int J Cardiol. 2021;326:12–8.
Ueki Y, Bär S, Losdat S, Otsuka T, Zanchin C, Zanchin T, et al. Validation of the Academic Research Consortium for high bleeding risk (ARC-HBR) criteria in patients undergoing percutaneous coronary intervention and comparison with contemporary bleeding risk scores. EuroIntervention. 2020;16:371–9.
Hashimoto R, Numasawa Y, Yokokura S, Daigo K, Sakata S, Imaeda S, et al. Prevalence of the Academic Research Consortium high bleeding risk criteria in patients undergoing endovascular therapy for peripheral artery disease in lower extremities. Heart Vessels. 2021;36:1350–8.
Yoshioka N, Takagi K, Morita Y, Kanzaki Y, Nagai H, Watanabe N, et al. Bleeding events and mid-term mortality in the patients undergoing endovascular interventions for peripheral artery disease of the lower limbs based on the academic research consortium high bleeding risk criteria. Heart Vessels. 2021;36:1336–49.
Mehran R, Rao SV, Bhatt DL, Gibson CM, Caixeta A, Eikelboom J, et al. Standardized bleeding defnitions for cardiovascular clinical trials: a consensus report from the bleeding Academic Research Consortium. Circulation. 2011;123:2736–47.
Soga Y, Iida O, Takahara M, Hirano K, Suzuki K, Kawasaki D, et al. Two-year life expectancy in patients with critical limb ischemia. JACC Cardiovasc Interv. 2014;7:1444–9.
Guo X, Xue G, Huang X, **e H, Liang W, Zhang J, et al. Outcomes of endovascular treatment for patients with TASC II D femoropopliteal occlusive disease: a single center study. BMC Cardiovasc Disord. 2015;15:44.
Khan MS, Zou F, Khan AR, Moustafa A, Schmid CH, Baig M, et al. Meta-analysis comparing endovascular treatment modalities for femoropopliteal peripheral artery disease. Am J Cardiol. 2020;128:181–8.
Takahara M, Iida O, Kohsaka S, Soga Y, Fujihara M, Shinke T, et al. Diabetes mellitus and other cardiovascular risk factors in lower-extremity peripheral artery disease versus coronary artery disease: an analysis of 1,121,359 cases from the nationwide databases. Cardiovasc Diabetol. 2019;18:155.
Numasawa Y, Inohara T, Ishii H, Kuno T, Kodaira M, Kohsaka S, et al. Comparison of outcomes of women versus men with non-ST-elevation acute coronary syndromes undergoing percutaneous coronary intervention (from the Japanese nationwide registry). Am J Cardiol. 2017;119(6):826–31.
Chandiramani R, Cao D, Claessen BE, Sorrentino S, Guedeney P, Blum M, et al. Sex-related differences in patients at high bleeding risk undergoing percutaneous coronary intervention: a patient-level pooled analysis from 4 postapproval studies. J Am Heart Assoc. 2020;9:e014611.
Shu J, Santulli G. Update on peripheral artery disease: epidemiology and evidence-based facts. Atherosclerosis. 2018;275:379–81.
Takeji Y, Yamaji K, Tomoi Y, Okazaki J, Tanaka K, Nagae A, et al. Impact of frailty on clinical outcomes in patients with critical limb ischemia. Circ Cardiovasc Interv. 2018;11:e006778.
Gebauer K, Engelbertz C, Malyar NM, Meyborg M, Lüders F, Freisinger E, et al. Long-term mortality after invasive angiography and endovascular revascularization in patients with PAD having chronic kidney disease. Angiology. 2016;67:556–64.
Senthong V, Wu Y, Hazen SL, Tang WH. Predicting longterm prognosis in stable peripheral artery disease with baseline functional capacity estimated by the Duke Activity Status Index. Am Heart J. 2017;184:17–25.
Soga Y, Iida O, Takahara M, Takahaera M, Hirano K, Suzuki K, et al. Two-year life expectancy in patients with critical limb ischemia. JACC Cardiovasc Interv. 2014;7:1444–9.
Shiraki T, Iida O, Takahara M, Masuda M, Okamoto S, Ishihara T, et al. The geriatric nutritional risk index is independently associated with prognosis in patients with critical limb ischemia following endovascular therapy. Eur J Vasc Endovasc Surg. 2016;52:218–24.
Garimella PS, Hirsch AT. Peripheral artery disease and chronic kidney disease: clinical synergy to improve outcomes. Adv Chronic Kidney Dis. 2014;21:460–71.
Baber U, Mehran R, Giustino G, Cohen DJ, Henry TD, Sartori S, et al. Coronary thrombosis and major bleeding after PCI with drug-eluting stents: risk scores from PARIS. J Am Coll Cardiol. 2016;67:2224–34.
Ward R, Huang Z, Rockhold FW, Baumgartner I, Berger JS, Blomster JI, et al. Major bleeding in patients with peripheral artery disease: insights from the EUCLID trial. Am Heart J. 2020;220:51–8.
Spiliopoulos S, Tsochatzis A, Festas G, Reppas L, Christidi F, Palialexis K, et al. A new preprocedural score to predict bleeding complications of endovascular interventions for peripheral artery disease. J Endovasc Ther. 2019;26:816–25.
Matsi PJ, Manninen HI. Complications of lower-limb percutaneous transluminal angioplasty: a prospective analysis of 410 procedures on 295 consecutive patients. Cardiovasc Intervent Radiol. 1998;21:361–6.
Acknowledgements
We are grateful to Miho Kobayashi for her editing assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shima, Y., Taninobu, N., Ikuta, A. et al. Two-year outcomes of endovascular therapy for femoropopliteal arterial lesions for patients with high bleeding risk. Cardiovasc Interv and Ther 39, 284–292 (2024). https://doi.org/10.1007/s12928-024-00999-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12928-024-00999-2