Abstract
Background
Obstructive sleep apnea (OSA) has been demonstrated to be associated with an increase of oxidative stress. However, whether circulating malondialdehyde (MDA), a widely used biomarker of oxidative stress, could be reduced by the treatment of OSA by continuous positive airway pressure (CPAP) is debated. The present meta-analysis was performed to determine the effect of CPAP treatment on circulating MDA among patients with OSA.
Methods
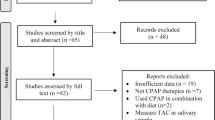
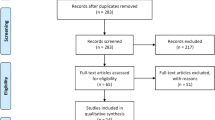
A systematic search of PubMed, Embase, and Web of Science was performed for literature covering the period between 1967 and August 2019. Standardized mean difference (SMD) was calculated to estimate the treatment effects of pre- and post-CPAP therapy.
Results
A total of 10 studies with 220 patients were included in this meta-analysis. A significant decrease in circulating MDA was observed after CPAP treatment (SMD = 1.164, 95% CI = 0.443 to 1.885, z = 3.16, p = 0.002) in OSA patients. Subgroup analyses revealed that CPAP therapy was associated with a significant decrease of circulating MDA in elder (SMD = 1.629, 95% CI = 0.265 to 2.994, z = 2.34, p = 0.019), more obese patients (SMD = 0.954, 95% CI = 0.435 to 1.473, z = 3.61, p = 0.000), more severe OSA patients (SMD = 0.879, 95% CI = 0.421 to 1.336, z = 3.76, p = 0.000), patients with therapeutic duration ≥ 3 months (SMD = 1.867, 95% CI = 0.563 to 3.172, z = 2.80, p = 0.005), and patients with good compliance (SMD = 1.004, 95% CI = 0.703 to 1.305, z = 6.54, p = 0.000).
Conclusions
This meta-analysis suggested that CPAP therapy exerted significant lowering effects on circulating MDA, especially in elder, more obese, and more severe OSA patients and patients with good compliance as well as longer duration of CPAP application.




Similar content being viewed by others
References
Lavie L (2009) Oxidative stress--a unifying paradigm in obstructive sleep apnea and comorbidities. Prog Cardiovasc Dis 51:303–312
Lavie L (2003) Obstructive sleep apnoea syndrome--an oxidative stress disorder. Sleep Med Rev 7:35–51
Niki E (2009) Lipid peroxidation: physiological levels and dual biological effects. Free Radic Biol Med 47:469–484
Esterbauer H, Zollner H (1989) Methods for determination of aldehydic lipid peroxidation products. Free Radic Biol Med 7:197–203
Ayala A, Munoz MF, Arguelles S (2014) Lipid peroxidation: production, metabolism, and signaling mechanisms of malondialdehyde and 4-hydroxy-2-nonenal. Oxidative Med Cell Longev 2014:360438
Janero DR (1990) Malondialdehyde and thiobarbituric acid-reactivity as diagnostic indices of lipid peroxidation and peroxidative tissue injury. Free Radic Biol Med 9:515–540
Jordan W, Cohrs S, Degner D, Meier A, Rodenbeck A, Mayer G, Pilz J, Ruther E, Kornhuber J, Bleich S (2006) Evaluation of oxidative stress measurements in obstructive sleep apnea syndrome. J Neural Transm 113:239–254
Vatansever E, Surmen-Gur E, Ursavas A, Karadag M (2011) Obstructive sleep apnea causes oxidative damage to plasma lipids and proteins and decreases adiponectin levels. Sleep Breath 15:275–282
Cao MT, Sternbach JM, Guilleminault C (2017) Continuous positive airway pressure therapy in obstuctive sleep apnea: benefits and alternatives. Expert Rev Respir Med 11:259–272
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135
Dal-Fabbro C, Garbuio S, D'Almeida V, Cintra FD, Tufik S, Bittencourt L (2014) Mandibular advancement device and CPAP upon cardiovascular parameters in OSA. Sleep Breath 18:749–759
Wu K, Su X, Li G, Zhang N (2016) Antioxidant carbocysteine treatment in obstructive sleep apnea syndrome: a randomized clinical trial. PLoS One 11:e0148519
Dorkova Z, Petrasova D, Molcanyiova A, Popovnakova M, Tkacova R (2008) Effects of continuous positive airway pressure on cardiovascular risk profile in patients with severe obstructive sleep apnea and metabolic syndrome. Chest 134:686–692
Ye LA, Ma GH, Chen L, Li M, Liu JL, Yang K, Li QY, Li N, Wan HY (2010) Quantification of circulating cell-free DNA in the serum of patients with obstructive sleep apnea-hypopnea syndrome. Lung 188:469–474
Jurado-Gamez B, Fernandez-Marin MC, Gomez-Chaparro JL, Munoz-Cabrera L, Lopez-Barea J, Perez-Jimenez F, Lopez-Miranda J (2011) Relationship of oxidative stress and endothelial dysfunction in sleep apnoea. Eur Respir J 37:873–879
Alzoghaibi MA, Bahammam AS (2012) The effect of one night of continuous positive airway pressure therapy on oxidative stress and antioxidant defense in hypertensive patients with severe obstructive sleep apnea. Sleep Breath 16:499–504
Yagihara F, Lucchesi LM, D'Almeida V, de Mello MT, Tufik S, Bittencourt LRA (2012) Oxidative stress and quality of life in elderly patients with obstructive sleep apnea syndrome: are there differences after six months of continuous positive airway pressure treatment? Clinics 67:565–571
Tichanon P, Wilaiwan K, Sopida S, Orapin P, Watchara B, Banjamas I (2016) Effect of continuous positive airway pressure on airway inflammation and oxidative stress in patients with obstructive sleep apnea. Can Respir J 2016:3107324
Wang XT, Zhao G, Tu L, Yue ZY, Liu ZH, Han J, Gao K, Zhou XC, Xu S, Li JF (2019) Continuous positive airway pressure effectively alleviates arrhythmias in patients with obstructive sleep apnea: possible relationship with counteracting oxidative stress. Curr Med Sci 39:52–58
Lavie L, Vishnevsky A, Lavie P (2004) Evidence for lipid peroxidation in obstructive sleep apnea. Sleep 27:123–128
Savas O, Suslu AE, Lay I, Ozer S (2019) Assessment of the relationship between polysomnography parameters and plasma malondialdehyde levels in patients with obstructive sleep apnea. Eur Arch Otorhinolaryngol 276:3533–3538
Badran M, Golbidi S, Devlin A, Ayas N, Laher I (2014) Chronic intermittent hypoxia causes endothelial dysfunction in a mouse model of diet-induced obesity. Sleep Med 15:596–602
Lorente L, Martin MM, Abreu-Gonzalez P, Ramos L, Argueso M, Sole-Violan J, Riano-Ruiz M, Jimenez A (2015) Serum malondialdehyde levels in patients with malignant middle cerebral artery infarction are associated with mortality. PLoS One 10:e0125893
Polidori MC, Cherubini A, Stahl W, Senin U, Sies H, Mecocci P (2002) Plasma carotenoid and malondialdehyde levels in ischemic stroke patients: relationship to early outcome. Free Radic Res 36:265–268
Chen LD, Lin L, Ou YW, Wu Z, Cai ZM, Wang TZ, Liu JN (2017) Effect of positive airway pressure on glomerular filtration rate in patients with sleep-disordered breathing: a meta-analysis. Sleep Breath 21:53–59
Chen LD, Lin L, Zhang LJ, Zeng HX, Wu QY, Hu MF, **e JJ, Liu JN (2018) Effect of continuous positive airway pressure on liver enzymes in obstructive sleep apnea: a meta-analysis. Clin Respir J 12:373–381
Chen X, Niu X, **ao Y, Dong J, Zhang R, Lu M, Kong W (2014) Effect of continuous positive airway pressure on homocysteine levels in patients with obstructive sleep apnea: a meta-analysis. Sleep Breath 18:687–694
Guo Y, Pan L, Ren D, **e X (2013) Impact of continuous positive airway pressure on C-reactive protein in patients with obstructive sleep apnea: a meta-analysis. Sleep Breath 17:495–503
Funding
This work was supported by the National Natural Science Foundation of China (81870074 and 81900088) and Startup Fund for scientific research from Fujian Medical University (2017XQ1117).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethics approval and consent to participate
All analyses were based on previous published studies, thus no ethical approval and patient consent are required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Q., Chen, LD., Chen, MX. et al. The effect of continuous positive airway pressure on circulating malondialdehyde among obstructive sleep apnea patients: a meta-analysis. Sleep Breath 24, 1407–1415 (2020). https://doi.org/10.1007/s11325-019-01998-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01998-x