Abstract
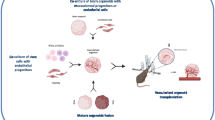
Angiogenesis plays an essential role in embryonic development, organ remodeling, wound healing, and is also associated with many human diseases. The process of angiogenesis in the brain during development is well characterized in animal models, but little is known about the process in the mature brain. Here, we use a tissue-engineered post-capillary venule (PCV) model incorporating stem cell derived induced brain microvascular endothelial-like cells (iBMECs) and pericyte-like cells (iPCs) to visualize the dynamics of angiogenesis. We compare angiogenesis under two conditions: in response to perfusion of growth factors and in the presence of an external concentration gradient. We show that both iBMECs and iPCs can serve as tip cells leading angiogenic sprouts. More importantly, the growth rate for iPC-led sprouts is about twofold higher than for iBMEC-led sprouts. Under a concentration gradient, angiogenic sprouts show a small directional bias toward the high growth factor concentration. Overall, pericytes exhibited a broad range of behavior, including maintaining quiescence, co-migrating with endothelial cells in sprouts, or leading sprout growth as tip cells.





Similar content being viewed by others
References
Paredes I, Himmels P, de Almodóvar CR (2018) Neurovascular communication during CNS development. Dev Cell 45(1):10–32
Tata M, Ruhrberg C, Fantin A (2015) Vascularisation of the central nervous system. Mech Dev 138:26–36
Brown CE et al (2007) Extensive turnover of dendritic spines and vascular remodeling in cortical tissues recovering from stroke. J Neurosci 27(15):4101–4109
Jiang X et al (2018) Blood-brain barrier dysfunction and recovery after ischemic stroke. Prog Neurobiol 163–164:144–171
Yao Y (2018) Basement membrane and stroke. J Cereb Blood Flow Metab. https://doi.org/10.1177/0271678X18801467
Croll SD, Wiegand SJ (2001) Vascular growth factors in cerebral ischemia. Mol Neurobiol 23(2–3):121–135
Lange C et al (2016) Vascular endothelial growth factor: a neurovascular target in neurological diseases. Nat Rev Neurol 12(8):439–454
Jain RK et al (2007) Angiogenesis in brain tumours. Nat Rev Neurosci 8(8):610–622
Salehi A, Zhang JH, Obenaus A (2017) Response of the cerebral vasculature following traumatic brain injury. J Cereb Blood Flow Metab 37(7):2320–2339
Shlosberg D et al (2010) Blood-brain barrier breakdown as a therapeutic target in traumatic brain injury. Nat Rev Neurol 6(7):393–403
Swain RA et al (2003) Prolonged exercise induces angiogenesis and increases cerebral blood volume in primary motor cortex of the rat. Neuroscience 117(4):1037–1046
Pereira, A.C., et al., An in vivo correlate of exercise-induced neurogenesis in the adult dentate gyrus. Proceedings of the National Academy of Sciences, 2007. 104(13): p. 5638-5643.
Park HY et al (2016) The effects of altitude/hypoxic training on oxygen delivery capacity of the blood and aerobic exercise capacity in elite athletes - a meta-analysis. J Exerc Nutrition Biochem 20(1):15–22
Bogorad MI et al (2019) Cerebrovascular plasticity: processes that lead to changes in the architecture of brain microvessels. J Cereb Blood Flow Metab 39(8):1413–1432
Lindahl P et al (1997) Pericyte loss and microaneurysm formation in PDGF-B-deficient mice. Science 277(5323):242–245
Daneman R et al (2010) Pericytes are required for blood–brain barrier integrity during embryogenesis. Nature 468(7323):562–566
Ogunshola OO et al (2000) Neuronal VEGF expression correlates with angiogenesis in postnatal develo** rat brain. Dev Brain Res 119(1):139–153
Virgintino D et al (2007) An intimate interplay between precocious, migrating pericytes and endothelial cells governs human fetal brain angiogenesis. Angiogenesis 10(1):35–45
Wälchli T et al (2015) Quantitative assessment of angiogenesis, perfused blood vessels and endothelial tip cells in the postnatal mouse brain. Nat Protoc 10(1):53–74
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473(7347):298–307
Gerhardt H, Betsholtz C (2003) Endothelial-pericyte interactions in angiogenesis. Cell Tissue Res 314(1):15–23
Benjamin LE, Hemo I, Keshet E (1998) A plasticity window for blood vessel remodelling is defined by pericyte coverage of the preformed endothelial network and is regulated by PDGF-B and VEGF. Development 125(9):1591–1598
Potente M, Gerhardt H, Carmeliet P (2011) Basic and therapeutic aspects of angiogenesis. Cell 146(6):873–887
Conway EM, Collen D, Carmeliet P (2001) Molecular mechanisms of blood vessel growth. Cardiovasc Res 49(3):507–521
Coelho-Santos, V., et al., Imaging the construction of capillary networks in the neonatal mouse brain. Proceedings of the National Academy of Sciences, 2021. 118(26).
Fruttiger M (2002) Development of the mouse retinal vasculature: angiogenesis versus vasculogenesis. Invest Ophthalmol Vis Sci 43(2):522–527
Wälchli, T., et al., Nogo-A is a negative regulator of CNS angiogenesis. Proceedings of the National Academy of Sciences, 2013. 110(21): p. E1943-E1952.
Nehls V, Denzer K, Drenckhahn D (1992) Pericyte involvement in capillary sprouting during angiogenesis in situ. Cell Tissue Res 270(3):469–474
Amselgruber W, Schäfer M, Sinowatz F (1999) Angiogenesis in the bovine corpus luteum: an immunocytochemical and ultrastructural study. Anat Histol Embryol 28(3):157–166
DeCicco-Skinner KL et al (2014) Endothelial cell tube formation assay for the in vitro study of angiogenesis. JoVE (Journal of Visualized Experiments) 91:e51312
Nakatsu MN, Davis J, Hughes CC (2007) Optimized fibrin gel bead assay for the study of angiogenesis. JoVE (Journal of Visualized Experiments) 3:e186
Linville RM et al (2020) Three-dimensional induced pluripotent stem-cell models of human brain angiogenesis. Microvasc Res 132:104042
Nguyen, D.-H.T., et al., Biomimetic model to reconstitute angiogenic sprouting morphogenesis in vitro. Proceedings of the National Academy of Sciences, 2013. 110(17): p. 6712-6717.
Shin Y et al (2011) In vitro 3D collective sprouting angiogenesis under orchestrated ANG-1 and VEGF gradients. Lab Chip 11(13):2175–2181
Shirure VS et al (2017) Low levels of physiological interstitial flow eliminate morphogen gradients and guide angiogenesis. Angiogenesis 20(4):493–504
Abaci HE et al (2014) Recapitulating physiological and pathological shear stress and oxygen to model vasculature in health and disease. Sci Rep 4(1):1–9
Lee E et al (2018) A 3D in vitro pericyte-supported microvessel model: visualisation and quantitative characterisation of multistep angiogenesis. J Mater Chem B 6(7):1085–1094
Silvestri VL et al (2020) A tissue-engineered 3D microvessel model reveals the dynamics of mosaic vessel formation in breast cancer. Can Res 80(19):4288–4301
Price GM et al (2010) Effect of mechanical factors on the function of engineered human blood microvessels in microfluidic collagen gels. Biomaterials 31(24):6182–6189
Kim S et al (2013) Engineering of functional, perfusable 3D microvascular networks on a chip. Lab Chip 13(8):1489–1500
Lee H et al (2014) A microfluidic platform for quantitative analysis of cancer angiogenesis and intravasation. Biomicrofluidics 8(5):054102
Zervantonakis, I.K., et al., Three-dimensional microfluidic model for tumor cell intravasation and endothelial barrier function. Proceedings of the National Academy of Sciences, 2012. 109(34): pp. 13515-13520.
Morgan JP et al (2013) Formation of microvascular networks in vitro. Nat Protoc 8(9):1820–1836
Bischel LL et al (2013) Tubeless microfluidic angiogenesis assay with three-dimensional endothelial-lined microvessels. Biomaterials 34(5):1471–1477
Kim C et al (2015) A quantitative microfluidic angiogenesis screen for studying anti-angiogenic therapeutic drugs. Lab Chip 15(1):301–310
Zheng, Y., et al., In vitro microvessels for the study of angiogenesis and thrombosis. Proceedings of the national academy of sciences, 2012. 109(24): pp. 9342-9347.
Tran KA et al (2022) Oxygen gradients dictate angiogenesis but not barriergenesis in a 3D brain microvascular model. J Cellular Physiol. https://doi.org/10.1002/jcp.30840
Zhao N et al (2022) Engineering the human blood-brain barrier at the capillary scale using a double-templating technique. Adv Functional Mater. https://doi.org/10.1002/adfm.202110289
Linville RM et al (2019) Human iPSC-derived blood-brain barrier microvessels: validation of barrier function and endothelial cell behavior. Biomaterials 190:24–37
Lippmann ES et al (2012) Derivation of blood-brain barrier endothelial cells from human pluripotent stem cells. Nat Biotechnol 30(8):783–791
Lippmann ES et al (2020) Commentary on human pluripotent stem cell-based blood–brain barrier models. Fluids and Barriers of the CNS 17(1):1–6
Linville RM et al (2020) Long-term cryopreservation preserves blood–brain barrier phenotype of iPSC-derived brain microvascular endothelial cells and three-dimensional microvessels. Mol Pharm 17(9):3425–3434
Wang K et al (2020) Robust differentiation of human pluripotent stem cells into endothelial cells via temporal modulation of ETV2 with modified mRNA. Sci Adv 6(30):7606
Stebbins MJ et al (2019) Human pluripotent stem cell–derived brain pericyte–like cells induce blood-brain barrier properties. Sci Adv 5(3):eaau7375
Jamieson JJ et al (2019) Role of iPSC-derived pericytes on barrier function of iPSC-derived brain microvascular endothelial cells in 2D and 3D. Fluids and Barriers of the CNS 16(1):1–16
Wong AD et al (2013) The blood-brain barrier: an engineering perspective. Front Neuroeng 6:7
Huxley VH, Curry FE, Adamson RH (1987) Quantitative fluorescence microscopy on single capillaries - alpha-lactalbumin transport. Am J Physiol 252(1):H188–H197
Red-Horse K et al (2010) Coronary arteries form by developmental reprogramming of venous cells. Nature 464(7288):549–553
Bussmann J, Wolfe SA, Siekmann AF (2011) Arterial-venous network formation during brain vascularization involves hemodynamic regulation of chemokine signaling. Development 138(9):1717–1726
Xu C et al (2014) Arteries are formed by vein-derived endothelial tip cells. Nat Commun 5(1):1–11
Lee H-W et al (2021) Role of venous endothelial cells in developmental and pathologic angiogenesis. Circulation 144(16):1308–1322
Abbott NJ et al (2010) Structure and function of the blood-brain barrier. Neurobiol Dis 37(1):13–25
Sweeney MD et al (2019) Blood-brain barrier: from physiology to disease and back. Physiol Rev 99(1):21–78
Lippmann ES et al (2020) Commentary on human pluripotent stem cell-based blood-brain barrier models. Fluids Barriers CNS 17(1):64
Linville RM, Searson PC (2021) Next-generation in vitro blood-brain barrier models: benchmarking and improving model accuracy. Fluids Barriers CNS 18(1):56
Wu H et al (1996) VEGF induces NO-dependent hyperpermeability in coronary venules. Am J Physiology-Heart Circulatory Physiol 271(6):H2735–H2739
Bates D, Curry F (1996) Vascular endothelial growth factor increases hydraulic conductivity of isolated perfused microvessels. Am J Physiol-Heart Circulatory Physiol 271(6):H2520–H2528
Weis S et al (2004) Src blockade stabilizes a Flk/cadherin complex, reducing edema and tissue injury following myocardial infarction. J Clin Investig 113(6):885–894
Roberts WG, Palade GE (1995) Increased microvascular permeability and endothelial fenestration induced by vascular endothelial growth factor. J Cell Sci 108(6):2369–2379
Ghajar CM et al (2006) Mesenchymal stem cells enhance angiogenesis in mechanically viable prevascularized tissues via early matrix metalloproteinase upregulation. Tissue Eng 12(10):2875–2888
Galie PA et al (2014) Fluid shear stress threshold regulates angiogenic sprouting. Proc Natl Acad Sci 111(22):7968–7973
Phng L-K, Gerhardt H (2009) Angiogenesis: a team effort coordinated by notch. Dev Cell 16(2):196–208
Mathiisen TM et al (2010) The perivascular astroglial sheath provides a complete covering of the brain microvessels: an electron microscopic 3D reconstruction. Glia 58(9):1094–1103
Frank RN et al (1983) Galactose-induced retinal capillary basement membrane thickening: prevention by Sorbinil. Invest Ophthalmol Vis Sci 24(11):1519–1524
Crouch EE, Doetsch F (2018) FACS isolation of endothelial cells and pericytes from mouse brain microregions. Nat Protoc 13(4):738–751
Chen J et al (2017) CD146 coordinates brain endothelial cell–pericyte communication for blood–brain barrier development. Proc Natl Acad Sci 114(36):E7622–E7631
Kang T-Y et al (2019) Pericytes enable effective angiogenesis in the presence of proinflammatory signals. Proc Natl Acad Sci 116(47):23551–23561
Kim J et al (2015) Engineering of a biomimetic pericyte-covered 3D microvascular network. PLoS ONE 10(7):e0133880
Campisi M et al (2018) 3D self-organized microvascular model of the human blood-brain barrier with endothelial cells, pericytes and astrocytes. Biomaterials 180:117–129
Gerhardt H et al (2003) VEGF guides angiogenic sprouting utilizing endothelial tip cell filopodia. J Cell Biol 161(6):1163–1177
Linville RM et al (2022) Three-dimensional microenvironment regulates gene expression, function, and tight junction dynamics of iPSC-derived blood–brain barrier microvessels. Fluids Barriers of the CNS 19(1):1–18
Weis SM, Cheresh DA (2005) Pathophysiological consequences of VEGF-induced vascular permeability. Nature 437(7058):497–504
Acknowledgments
The authors would like to thank Mr. Grant Kitchen, Dr. Dinh-Tuan Phan, and Dr. Yi Lu for help with the design and fabrication of the mold. This work was supported by NIH (NINDS R01NS106008 and NHLBI R61HL154252).
Author information
Authors and Affiliations
Contributions
NZ and PS conceived the original idea. NZ wrote the manuscript. NZ, SK, SZ, RL, TC, ZG, JJ, DN, LL, and AP contributed to the data acquisition, analysis, and interpretation. PS supervised all work.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhao, N., Kulkarni, S., Zhang, S. et al. Modeling angiogenesis in the human brain in a tissue-engineered post-capillary venule. Angiogenesis 26, 203–216 (2023). https://doi.org/10.1007/s10456-023-09868-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-023-09868-7