Abstract
Background
Establishing a molecular genetic diagnosis of focal segmental glomerulosclerosis (FSGS)/steroid-resistant nephrotic syndrome (SRNS) can be useful for predicting post-transplant recurrence. Monogenic causes are reportedly present in approximately 20–30% of patients with FSGS/SRNS. However, the characteristics of patients who are likely to have a monogenic cause remain to be determined.
Methods
Pediatric recipients with SRNS and/or biopsy-proven FSGS who underwent their first kidney transplantation at our center between 1999 and 2019 were analyzed. Patients with secondary FSGS/SRNS were excluded. The recipients were divided into three groups: familial/syndromic, presumed primary, and undetermined FSGS/SRNS. Patients who met all of the following criteria were categorized as having presumed primary FSGS/SRNS: (i) nephrotic syndrome, (ii) complete or partial remission with initial steroid therapy and/or additional immunosuppressive therapies, and (iii) diffuse foot process effacement on electron microscopy in the native kidney biopsy. All patients underwent genetic testing using next-generation sequencing.
Results
Twenty-four patients from 23 families were analyzed in this study. Pathogenic or likely pathogenic variants in FSGS/SRNS-related genes were identified in four of four families, zero of eight families, and 10 of 11 families with familial/syndromic, presumed primary, and undetermined FSGS/SRNS, respectively. Post-transplant recurrence only occurred in patients with presumed primary FSGS/SRNS.
Conclusions
Our systematic approach based on precise clinicopathological findings including nephrotic syndrome, treatment responses, and diffuse foot process effacement might be useful to differentiate pediatric kidney transplant recipients with FSGS/SRNS who are likely to have a monogenic cause from patients who are not, and to predict post-transplant recurrence.
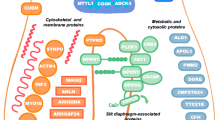
Graphical abstract
A higher resolution version of the Graphical abstract is available as Supplementary information.


Similar content being viewed by others
Data availability
The datasets of the current study are available from the corresponding author on reasonable request.
References
Bacchetta J, Cochat P (2015) Primary disease recurrence-effects on paediatric renal transplantation outcomes. Nat Rev Nephrol 11:371–384. https://doi.org/10.1038/nrneph.2015.54
Francis A, Trnka P, McTaggart SJ (2016) Long-term outcome of kidney transplantation in recipients with focal segmental glomerulosclerosis. Clin J Am Soc Nephrol 11:2041–2046. https://doi.org/10.2215/CJN.03060316
Canaud G, Delville M, Legendre C (2016) Recurrence of focal and segmental glomerulosclerosis after transplantation. Transplantation 100:284–287. https://doi.org/10.1097/TP.0000000000000902
Cosio FG, Cattran DC (2017) Recent advances in our understanding of recurrent primary glomerulonephritis after kidney transplantation. Kidney Int 91:304–314. https://doi.org/10.1016/j.kint.2016.08.030
Fine RN (2007) Recurrence of nephrotic syndrome/focal segmental glomerulosclerosis following renal transplantation in children. Pediatr Nephrol 22:496–502. https://doi.org/10.1007/s00467-006-0361-6
D’Agati VD, Kaskel FJ, Falk RJ (2011) Focal segmental glomerulosclerosis. N Engl J Med 365:2398–2411. https://doi.org/10.1056/NEJMra1106556
De Vriese AS, Sethi S, Nath KA, Glassock RJ, Fervenza FC (2018) Differentiating primary, genetic, and secondary FSGS in adults: a clinicopathologic approach. J Am Soc Nephrol 29:759–774. https://doi.org/10.1681/ASN.2017090958
Rosenberg AZ, Kopp JB (2017) Focal segmental glomerulosclerosis. Clin J Am Soc Nephrol 12:502–517. https://doi.org/10.2215/CJN.05960616
Weber LT, Tönshoff B, Grenda R, Bouts A, Topaloglu R, Gülhan B, Printza N, Awan A, Battelino N, Ehren R, Hoyer PF, Novljan G, Marks SD, Oh J, Prytula A, Seeman T, Sweeney C, Dello Strologo L, Pape L (2021) Clinical practice recommendations for recurrence of focal and segmental glomerulosclerosis/steroid-resistant nephrotic syndrome. Pediatr Transplant 25:e13955. https://doi.org/10.1111/petr.13955
Sadowski CE, Lovric S, Ashraf S, Pabst WL, Gee HY, Kohl S, Engelmann S, Vega-Warner V, Fang H, Halbritter J, Somers MJ, Tan W, Shril S, Fessi I, Lifton RP, Bockenhauer D, El-Desoky S, Kari JA, Zenker M, Kemper MJ, Mueller D, Fathy HM, Soliman NA; SRNS Study Group, Hildebrandt F (2015) A single-gene cause in 29.5% of cases of steroid-resistant nephrotic syndrome. J Am Soc Nephrol 26:1279–1289. https://doi.org/10.1681/ASN.2014050489
Bierzynska A, McCarthy HJ, Soderquest K, Sen ES, Colby E, Ding WY, Nabhan MM, Kerecuk L, Hegde S, Hughes D, Marks S, Feather S, Jones C, Webb NJ, Ognjanovic M, Christian M, Gilbert RD, Sinha MD, Lord GM, Simpson M, Koziell AB, Welsh GI, Saleem MA (2017) Genomic and clinical profiling of a national nephrotic syndrome cohort advocates a precision medicine approach to disease management. Kidney Int 91:937–947. https://doi.org/10.1016/j.kint.2016.10.013
Warejko JK, Tan W, Daga A, Schapiro D, Lawson JA, Shril S, Lovric S, Ashraf S, Rao J, Hermle T, Jobst-Schwan T, Widmeier E, Majmundar AJ, Schneider R, Gee HY, Schmidt JM, Vivante A, van der Ven AT, Ityel H, Chen J, Sadowski CE, Kohl S, Pabst WL, Nakayama M, Somers MJG, Rodig NM, Daouk G, Baum M, Stein DR, Ferguson MA, Traum AZ, Soliman NA, Kari JA, El Desoky S, Fathy H, Zenker M, Bakkaloglu SA, Müller D, Noyan A, Ozaltin F, Cadnapaphornchai MA, Hashmi S, Hopcian J, Kopp JB, Benador N, Bockenhauer D, Bogdanovic R, Stajić N, Chernin G, Ettenger R, Fehrenbach H, Kemper M, Munarriz RL, Podracka L, Büscher R, Serdaroglu E, Tasic V, Mane S, Lifton RP, Braun DA, Hildebrandt F (2018) Whole exome sequencing of patients with steroid-resistant nephrotic syndrome. Clin J Am Soc Nephrol 13:53–62. https://doi.org/10.2215/CJN.04120417
Trautmann A, Vivarelli M, Samuel S, Gipson D, Sinha A, Schaefer F, Hui NK, Boyer O, Saleem MA, Feltran L, Müller-Deile J, Becker JU, Cano F, Xu H, Lim YN, Smoyer W, Anochie I, Nakanishi K, Hodson E, Haffner D, International Pediatric Nephrology Association (2020) IPNA clinical practice recommendations for the diagnosis and management of children with steroid-resistant nephrotic syndrome. Pediatr Nephrol 35:1529–1561. https://doi.org/10.1007/s00467-020-04519-1
Preston R, Stuart HM, Lennon R (2019) Genetic testing in steroid-resistant nephrotic syndrome: why, who, when and how? Pediatr Nephrol 34:195–210. https://doi.org/10.1007/s00467-017-3838-6
Mann N, Braun DA, Amann K, Tan W, Shril S, Connaughton DM, Nakayama M, Schneider R, Kitzler TM, van der Ven AT, Chen J, Ityel H, Vivante A, Majmundar AJ, Daga A, Warejko JK, Lovric S, Ashraf S, Jobst-Schwan T, Widmeier E, Hugo H, Mane SM, Spaneas L, Somers MJG, Ferguson MA, Traum AZ, Stein DR, Baum MA, Daouk GH, Lifton RP, Manzi S, Vakili K, Kim HB, Rodig NM, Hildebrandt F (2019) Whole-exome sequencing enables a precision medicine approach for kidney transplant recipients. J Am Soc Nephrol 30:201–215. https://doi.org/10.1681/ASN.2018060575
Sethi S, Glassock RJ, Fervenza FC (2015) Focal segmental glomerulosclerosis: towards a better understanding for the practicing nephrologist. Nephrol Dial Transplant 30:375–384. https://doi.org/10.1093/ndt/gfu035
Ishizuka K, Miura K, Hashimoto T, Kaneko N, Harita Y, Yabuuchi T, Hisano M, Fu**aga S, Omori T, Yamaguchi Y, Hattori M (2021) Degree of foot process effacement in patients with genetic focal segmental glomerulosclerosis: a single-center analysis and review of the literature. Sci Rep 11:12008. https://doi.org/10.1038/s41598-021-91520-9
Ding WY, Koziell A, McCarthy HJ, Bierzynska A, Bhagavatula MK, Dudley JA, Inward CD, Coward RJ, Tizard J, Reid C, Antignac C, Boyer O, Saleem MA (2014) Initial steroid sensitivity in children with steroid-resistant nephrotic syndrome predicts post-transplant recurrence. J Am Soc Nephrol 25:1342–1348. https://doi.org/10.1681/ASN.2013080852
Miura K, Ando T, Kanda S, Hashimoto T, Kaneko N, Ishizuka K, Hamada R, Hataya H, Hotta K, Gotoh Y, Nishiyama K, Hamasaki Y, Shishido S, Fujita N, Hattori M (2021) Response to steroid and immunosuppressive therapies may predict post-transplant recurrence of steroid-resistant nephrotic syndrome. Pediatr Transplant. https://doi.org/10.1111/petr.14103
Glassock RJ, Fervenza FC (2022) “Presumed” primary focal segmental glomerulosclerosis: a novel nuance for steroid therapy. Kidney Int Rep 7:9–12. https://doi.org/10.1016/j.ekir.2021.11.021
Rood IM, Bavinck A, Lipska-Zietkiewicz BS, Lugtenberg D, Schaefer F, Deegens JKJ, Wetzels JFM (2022) Later response to corticosteroids in adults with primary focal segmental glomerular sclerosis is associated with favorable outcomes. Kidney Int Rep 7:87–98. https://doi.org/10.1016/j.ekir.2021.10.016
Kidney Disease: Improving Global Outcomes (KDIGO) Glomerular Diseases Work Group (2021) KDIGO 2021 Clinical Practice Guideline for the Management of Glomerular Disease. Kidney Int 100:S1–S276. https://doi.org/10.1016/j.kint.2021.05.021
Ogino D, Hashimoto T, Hattori M, Sugawara N, Akioka Y, Tamiya G, Makino S, Toyota K, Mitsui T, Hayasaka K (2016) Analysis of the genes responsible for steroid-resistant nephrotic syndrome and/or focal segmental glomerulosclerosis in Japanese patients by whole-exome sequencing analysis. J Hum Genet 61:137–141. https://doi.org/10.1038/jhg.2015.122
Hashimoto T, Harita Y, Takizawa K, Urae S, Ishizuka K, Miura K, Horita S, Ogino D, Tamiya G, Ishida H, Mitsui T, Hayasaka K, Hattori M (2019) In vivo expression of NUP93 and its alteration by NUP93 mutations causing focal segmental glomerulosclerosis. Kidney Int Rep 4:1312–1322. https://doi.org/10.1016/j.ekir.2019.05.1157
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, Grody WW, Hegde M, Lyon E, Spector E, Voelkerding K, Rehm HL, ACMG Laboratory Quality Assurance Committee (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17:405–424. https://doi.org/10.1038/gim.2015.30
Miyake N, Tsukaguchi H, Koshimizu E, Shono A, Matsunaga S, Shiina M, Mimura Y, Imamura S, Hirose T, Okudela K, Nozu K, Akioka Y, Hattori M, Yoshikawa N, Kitamura A, Cheong HI, Kagami S, Yamashita M, Fujita A, Miyatake S, Tsurusaki Y, Nakashima M, Saitsu H, Ohashi K, Imamoto N, Ryo A, Ogata K, Iijima K, Matsumoto N (2015) Biallelic mutations in nuclear pore complex subunit NUP107 cause early-childhood-onset steroid-resistant nephrotic syndrome. Am J Hum Genet 97:555–566. https://doi.org/10.1016/j.ajhg.2015.08.013
Shirai Y, Miura K, Kaneko N, Ishizuka K, Endo A, Hashimoto T, Kanda S, Harita Y, Hattori M (2021) A novel de novo truncating TRIM8 variant associated with childhood-onset focal segmental glomerulosclerosis without epileptic encephalopathy: a case report. BMC Nephrol 22:417. https://doi.org/10.1186/s12882-021-02626-1
Udagawa T, Jo T, Yanagihara T, Shimizu A, Mitsui J, Tsuji S, Morishita S, Onai R, Miura K, Kanda S, Kajiho Y, Tsurumi H, Oka A, Hattori M, Harita Y (2017) Altered expression of Crb2 in podocytes expands a variation of CRB2 mutations in steroid-resistant nephrotic syndrome. Pediatr Nephrol 32:801–809. https://doi.org/10.1007/s00467-016-3549-4
McCarthy HJ, Bierzynska A, Wherlock M, Ognjanovic M, Kerecuk L, Hegde S, Feather S, Gilbert RD, Krischock L, Jones C, Sinha MD, Webb NJ, Christian M, Williams MM, Marks S, Koziell A, Welsh GI, Saleem MA, RADAR the UK SRNS Study Group (2013) Simultaneous sequencing of 24 genes associated with steroid-resistant nephrotic syndrome. Clin J Am Soc Nephrol 8:637–648. https://doi.org/10.2215/CJN.07200712
Hommos MS, De Vriese AS, Alexander MP, Sethi S, Vaughan L, Zand L, Bharucha K, Lepori N, Rule AD, Fervenza FC (2017) The incidence of primary vs secondary focal segmental glomerulosclerosis: a clinicopathologic study. Mayo Clin Proc 92:1772–1781. https://doi.org/10.1016/j.mayocp.2017.09.011
Büscher AK, Beck BB, Melk A, Hoefele J, Kranz B, Bamborschke D, Baig S, Lange-Sperandio B, Jungraithmayr T, Weber LT, Kemper MJ, Tönshoff B, Hoyer PF, Konrad M, Weber S, GPN Association (GPN) (2016) Rapid response to cyclosporin A and favorable renal outcome in nongenetic versus genetic steroid-resistant nephrotic syndrome. Clin J Am Soc Nephrol 11:245–253. https://doi.org/10.2215/CJN.07370715
Deegens JK, Dijkman HB, Borm GF, Steenbergen EJ, van den Berg JG, Weening JJ, Wetzels JF (2008) Podocyte foot process effacement as a diagnostic tool in focal segmental glomerulosclerosis. Kidney Int 74:1568–1576. https://doi.org/10.1038/ki.2008.413
Nagano C, Yamamura T, Horinouchi T, Aoto Y, Ishiko S, Sakakibara N, Shima Y, Nakanishi K, Nagase H, Iijima K, Nozu K (2020) Comprehensive genetic diagnosis of Japanese patients with severe proteinuria. Sci Rep 10:270. https://doi.org/10.1038/s41598-019-57149-5
Park E, Ahn YH, Kang HG, Miyake N, Tsukaguchi H, Cheong HI (2017) NUP107 mutations in children with steroid-resistant nephrotic syndrome. Nephrol Dial Transplant 32:1013–1017. https://doi.org/10.1093/ndt/gfw103
Park E, Lee C, Kim NKD, Ahn YH, Park YS, Lee JH, Kim SH, Cho MH, Cho H, Yoo KH, Shin JI, Kang HG, Ha IS, Park WY, Cheong HI (2020) Genetic study in Korean pediatric patients with steroid-resistant nephrotic syndrome or focal segmental glomerulosclerosis. J Clin Med 9:2013. https://doi.org/10.3390/jcm9062013
Wang F, Zhang Y, Mao J, Yu Z, Yi Z, Yu L, Sun J, Wei X, Ding F, Zhang H, **ao H, Yao Y, Tan W, Lovric S, Ding J, Hildebrandt F (2017) Spectrum of mutations in Chinese children with steroid-resistant nephrotic syndrome. Pediatr Nephrol 32:1181–1192. https://doi.org/10.1007/s00467-017-3590-y
Acknowledgements
We thank the affected individuals, their families, and their physicians who contributed to this study. The following doctors recruited patients and gathered detailed clinical information for this study: Noriko Sugawara (Tohoku University), Shuichiro Fu**aga (Saitama Children’s Medical Center), Amane Endo (Juntendo University), Takeshi Yanagihara (Nippon Medical School), Daisuke Matsuoka (Shinshu University), Takayuki Miyai (Okayama University), and Mikiya Fujieda (Kochi University). We also thank Professor Kazuho Honda (Showa University) for his kind support in examination of the degree of FPE on EM, and Professor Kandai Nozu (Kobe University) and Dr. Hidenori Sato (Yamagata University School of Medicine) for performing genetic analysis in some patients.
In this research work, we used instruments in the Medical Research Institute (MRI), Tokyo Women’s Medical University.
We thank Georgia Lenihan-Geels, PhD, and Ryan Chastain-Gross, PhD, from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
This work was supported in part by Grants-in-Aid Scientific Research (C) (JP21K07829 [KM] and JP21K07857 [NK]) from the Ministry of Education, Culture, Sports, Science and Technology of Japan.
Author information
Authors and Affiliations
Contributions
K.M. and N.K. participated in research design, data analysis, and writing the manuscript. T.H., Y.H., and T.Y. participated in genetic analysis and comprehensive editing of the manuscript. K.I. and Y.S. participated in data acquisition and genetic analysis. M.Hi., H.C., Y.A., and S.K. participated in data acquisition and comprehensive editing of the manuscript. M.Ha. participated in research design and comprehensive editing of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Graphical Abstract
(PPTX 47 KB)
Supplementary file 2
(PDF 242 KB)
Rights and permissions
About this article
Cite this article
Miura, K., Kaneko, N., Hashimoto, T. et al. Precise clinicopathologic findings for application of genetic testing in pediatric kidney transplant recipients with focal segmental glomerulosclerosis/steroid-resistant nephrotic syndrome. Pediatr Nephrol 38, 417–429 (2023). https://doi.org/10.1007/s00467-022-05604-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05604-3