Abstract
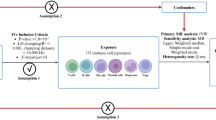
Prostatitis represents a common disease of the male genitourinary system, significantly impacting the physical and mental health of male patients. While numerous studies have suggested a potential link between immune cell activity and prostatitis, the exact causal role of immune cells in prostatitis remains uncertain. This study aims to explore the causal relationship between immune cell characteristics and prostatitis using a bidirectional Mendelian randomization approach. This study utilizes data from the public GWAS database and employs bidirectional Mendelian randomization analysis to investigate the causal relationship between immune cells and prostatitis. The causal relationship between 731 immune cell features and prostatitis was primarily investigated through inverse variance weighting (IVW), complemented by MR-Egger regression, a simple model, the weighted median method, and a weighted model. Ultimately, the results underwent sensitivity analysis to assess the heterogeneity, horizontal pleiotropy, and stability of Single Nucleotide Polymorphisms (SNPs) in immune cells and prostatitis. MR analysis revealed 17 immune cells exhibiting significant causal effects on prostatitis. In contrast, findings from reverse MR indicated a significant causal relationship between prostatitis and 13 immune cells. Our study utilizes bidirectional Mendelian Randomization to establish causal relationships between specific immune cell phenotypes and prostatitis, highlighting the reciprocal influence between immune system behavior and the disease. Our findings suggest targeted therapeutic approaches and the importance of including diverse populations for broader validation and personalized treatment strategies.



Similar content being viewed by others
Data availability
The datasets generated and analyzed in this study are accessible at https://gwas.mrcieu.ac.uk/
Abbreviations
- IVW:
-
Inverse Variance Weighted
- GWAS:
-
Genome-Wide Association Studies
- MR:
-
Mendelian Randomization
- SNPs:
-
Single Nucleotide Polymorphisms
- IV:
-
Instrumental Variable
- AC:
-
Absolute Count
- MFI:
-
Median Fluorescence Intensity
- MP:
-
Morphological Parameter
- RC:
-
Relative Count
- LD:
-
Linkage Disequilibrium
- OR:
-
Odds Ratio
- CI:
-
Confidence Interval
- HLA:
-
Human Leukocyte Antigen
References
Amu S, Gjertsson I, Tarkowski A et al (2006) B-cell CD25 expression in murine primary and secondary lymphoid tissue [J]. Scand J Immunol 64(5):482–492
Bowden J, Davey Smith G, Burgess S (2015) Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression [J]. Int J Epidemiol 44(2):512–525
Bowden J, Davey Smith G, Haycock PC et al (2016) Consistent estimation in mendelian randomization with some Invalid instruments using a weighted median estimator [J]. Genet Epidemiol 40(4):304–314
Breser ML, Salazar FC, Rivero VE et al (2017) Immunological mechanisms underlying Chronic Pelvic Pain and prostate inflammation in Chronic Pelvic Pain syndrome [J]. Front Immunol, 8898
Buchanan RM, Popowych Y, Arsic N et al (2011) B-cell activating factor (BAFF) promotes CpG ODN-induced B cell activation and proliferation [J]. Cell Immunol 271(1):16–28
Burgess S, Thompson SG (2017) Interpreting findings from mendelian randomization using the MR-Egger method [J]. Eur J Epidemiol 32(5):377–389
Chen X, Hu C, Peng Y et al (2016) Association of diet and lifestyle with chronic prostatitis/chronic pelvic pain syndrome and pain severity: a case-control study [J]. Prostate Cancer Prostatic Dis 19(1):92–99
Chen L, Zhang M, Liang C (2021) Chronic Prostatitis and Pelvic Pain Syndrome: another Autoimmune Disease? [J]. Arch Immunol Ther Exp (Warsz) 69(1):24
Collins MM, Stafford RS, O’Leary MP et al (1998) How common is prostatitis? A national survey of physician visits [J]. J Urol 159(4):1224–1228
Dhundee J, Maciver AG (1991) An immunohistological study of granulomatous prostatitis [J]. Histopathology 18(5):435–441
Emdin CA, Khera AV, Kathiresan S, Mendelian (2017) Randomization [J] Jama 318(19):1925–1926
Giovannetti A, Rosato E, Renzi C et al (2010) Analyses of T cell phenotype and function reveal an altered T cell homeostasis in systemic sclerosis. Correlations with disease severity and phenotypes [J]. Clin Immunol 137(1):122–133
Kraemer L, McKay DM, Russo RC et al (2022) Chemokines and chemokine receptors: insights from human disease and experimental models of helminthiasis [J]. Cytokine Growth Factor Rev, 6638–6652
Krieger JN, Nyberg L Jr., Nickel JC (1999) NIH consensus definition and classification of prostatitis [J]. JAMA 282(3):236–237
Li S, Wan J, Anderson W et al (2016) Downregulation of IL-10 secretion by Treg cells in osteoarthritis is associated with a reduction in Tim-3 expression [J]. Biomed Pharmacother, 79159–79165
Liu Y, Mikrani R, **e D et al (2020) Chronic prostatitis/chronic pelvic pain syndrome and prostate cancer: study of immune cells and cytokines [J]. Fundam Clin Pharmacol 34(2):160–172
Liu CP, Chen ZD, Ye ZY et al (2021a) Therapeutic applications of functional nanomaterials for prostatitis [J]. Front Pharmacol, 12685465
Liu Y, Zhang Y, Zhang M et al (2021b) Activated autophagy restored the impaired frequency and function of regulatory T cells in chronic prostatitis [J]. Prostate 81(1):29–40
Mahal BA, Cohen JM, Allsop SA et al (2011) The role of phenoty** in chronic prostatitis/chronic pelvic pain syndrome [J]. Curr Urol Rep 12(4):297–303
Matta BM, Castellaneta A, Thomson AW (2010) Tolerogenic plasmacytoid DC [J]. Eur J Immunol 40(10):2667–2676
Netea MG, Balkwill F, Chonchol M et al (2017) A guiding map for inflammation [J]. Nat Immunol 18(8):826–831
Orrù V, Steri M, Sidore C et al (2020) Complex genetic signatures in immune cells underlie autoimmunity and inform therapy [J]. Nat Genet 52(10):1036–1045
Parel Y, Chizzolini C (2004) CD4 + CD8 + double positive (DP) T cells in health and disease [J]. Autoimmun Rev 3(3):215–220
Pena VN, Engel N, Gabrielson AT et al (2021) Diagnostic and management strategies for patients with chronic Prostatitis and Chronic Pelvic Pain syndrome [J]. Drugs Aging 38(10):845–886
Rees J, Abrahams M, Doble A et al (2015) Diagnosis and treatment of chronic bacterial prostatitis and chronic prostatitis/chronic pelvic pain syndrome: a consensus guideline [J]. BJU Int 116(4):509–525
Schaeffer AJ (2008) Epidemiology and evaluation of chronic pelvic pain syndrome in men [J]. Int J Antimicrob Agents 31(Suppl 1):108–111
Sekula P, Del Greco MF, Pattaro C et al (2016) Mendelian randomization as an Approach to assess causality using Observational data [J]. J Am Soc Nephrol 27(11):3253–3265
Shattuck EC, Muehlenbein MP (2015) Human sickness behavior: Ultimate and proximate explanations [J]. Am J Phys Anthropol 157(1):1–18
Sidore C, Busonero F, Maschio A et al (2015) Genome sequencing elucidates sardinian genetic architecture and augments association analyses for lipid and blood inflammatory markers [J]. Nat Genet 47(11):1272–1281
Slobodin G, Ahmad MS, Rosner I et al (2010) Regulatory T cells (CD4(+)CD25(bright)FoxP3(+)) expansion in systemic sclerosis correlates with disease activity and severity [J]. Cell Immunol 261(2):77–80
Sugimoto M, Hijikata Y, Tohi Y et al (2022) Low quality of life in men with chronic prostatitis-like symptoms [J]. Prostate Cancer Prostatic Dis 25(4):785–790
Sun Y, Liu Y, Liu B et al (2021) Efficacy of acupuncture for Chronic Prostatitis/Chronic Pelvic Pain Syndrome: a randomized trial [J]. Ann Intern Med 174(10):1357–1366
Ugor E, Simon D, Almanzar G et al (2017) Increased proportions of functionally impaired regulatory T cell subsets in systemic sclerosis [J]. Clin Immunol, 18454–18462
Verbanck M, Chen CY, Neale B et al (2018) Detection of widespread horizontal pleiotropy in causal relationships inferred from mendelian randomization between complex traits and diseases [J]. Nat Genet 50(5):693–698
Vykhovanets EV, Resnick MI, Marengo SR (2005) The healthy rat prostate contains high levels of natural killer-like cells and unique subsets of CD4 + helper-inducer T cells: implications for prostatitis [J]. J Urol 173(3):1004–1010
Wong L, Done JD, Schaeffer AJ et al (2015) Experimental autoimmune prostatitis induces microglial activation in the spinal cord [J]. Prostate 75(1):50–59
Yavorska OO, Burgess S (2017) MendelianRandomization: an R package for performing mendelian randomization analyses using summarized data [J]. Int J Epidemiol 46(6):1734–1739
Yebes A, Toribio-Vazquez C, Martinez-Perez S et al (2023) Prostatitis: a review [J]. Curr Urol Rep 24(5):241–251
Zheng J, Baird D, Borges MC et al (2017) Recent developments in mendelian randomization studies [J]. Curr Epidemiol Rep 4(4):330–345
Acknowledgements
This research received partial funding from the Hunan Natural Science Foundation (NO.2021JJ41094) and the Hunan Province Natural Science Foundation (NO.2022JJ70085).
Author information
Authors and Affiliations
Contributions
Genyi Qu, Weimin Jiang and **ng Zhou authored the main manuscript. Guang Yang, Cheng Tang and Yong Xu conducted the experiments. Zhaohui Long and Yijie Wang were responsible for data collection. All authors reviewed, discussed the results, and edited the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Qu, G., Jiang, W., Long, Z. et al. Assessing the causal relationship between immune cells and prostatitis: evidence from bidirectional mendelian randomization analysis. Mamm Genome (2024). https://doi.org/10.1007/s00335-024-10044-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00335-024-10044-5