Abstract
Aims/hypothesis
Type 1 diabetes mellitus is caused by autoimmune pancreatic beta cell destruction, and the destructive process involves several molecular mechanisms including oxygen-reactive species. A cysteine derivative, N-acetyl-cysteine, is widely used as an antioxidant, but the role of N-acetyl-cysteine in the protection of pancreatic beta cells in Type 1 diabetes remains unclear. The aim of this study was to clarify the effect of N-acetyl-cysteine on beta cells using an adoptive transfer system in a murine model of Type 1 diabetes.
Methods
Splenocytes from diabetic female non-obese diabetic mice were transferred into female non-obese diabetic scid/scid recipients to induce diabetes. Just after transfer, N-acetyl-cysteine was administered to non-obese diabetic scid recipients. Two weeks after transfer, the pancreas of the recipients was examined histologically, and cytokine mRNA expression in the pancreas was analysed. In vitro, CD4-positive splenocytes from diabetic donor mice were stimulated with anti-CD3 and anti-CD28 antibodies with or without N-acetyl-cysteine.
Results
Treatment with N-acetyl-cysteine significantly accelerated the transfer of diabetes into non-obese diabetic scid recipients. Treatment with N-acetyl-cysteine accelerated the infiltration of mononuclear cells accompanied by CD8-positive cells into the intra-islet region of the recipient’s pancreas, and enhanced interferon-gamma mRNA expression in the pancreas. In vitro, treatment with N-acetyl-cysteine enhanced interferon-gamma and interleukin-2 production by CD4-positive splenocytes of the diabetic donor mice.
Conclusions/interpretation
N-acetyl-cysteine accelerates the transfer of diabetes into non-obese diabetic scid mice and this effect is accompanied by the promotion of local infiltration and T-helper cell type 1 responses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 1 diabetes mellitus is considered to be caused by autoimmune-mediated pancreatic beta cell destruction. The destructive process involves several cellular mechanisms, mediated by CD4-positive T cells, CD8-positive T cells and antigen-presenting cells, and molecular mechanisms, including perforin, Fas, cytokines and oxygen-reactive species [1]. In animal models of Type 1 diabetes, such as the non-obese diabetic (NOD) mouse, several antioxidants could prevent diabetes onset by reducing oxidative stress in pancreatic beta cells [2, 3, 4, 5].
A cysteine derivative, N-acetyl-cysteine (NAC), is now a widely used drug and is recommended as an antidote for the treatment of acetaminophen overdose and is also used as an antioxidant [6]. As an antioxidant, NAC has been reported to have the beneficial effects of reducing the number of cases of renal dysfunction induced by contrast media [7] and reducing cardiovascular events in haemodialysis patients [8].
With regard to immunological properties, NAC enhances T cell function through mitogenesis, IL-2 production, and growth [9]. Treatment with NAC in vivo improved the function of macrophages and lymphocytes, in terms of, for example, the ability of adherence, chemotaxis, phagocytosis, and oxygen-reactive species production [10]. Treatment with NAC was reported to suppress the spontaneous development of diabetes in young NOD mice [11]. However, it is possible that administration of NAC would rather promote the development of T lymphocytes to IFN-γ-producing cells and accelerate pancreatic beta cell destruction, based upon the above-mentioned effect of NAC on T cell function. To clearly evaluate the effect of NAC on beta cell protection, we used an adoptive transfer system of diabetogenic splenocytes into NOD scid/scid (NOD scid) recipients treated with NAC.
Materials and methods
Animals
Female NOD and female NOD scid mice (5–10 weeks old) were purchased from CLEA Japan (Tokyo, Japan). They were kept under specific pathogen-free conditions and treated in accordance with the institutional animal care guidelines of Keio University School of Medicine. The principles of animal care were followed (NIH publication no. 85-23, revised 1985). Urinary glucose analysis was performed using Tes-tape (Shionogi, Osaka, Japan) every other day. Plasma glucose levels were determined using Glutest-Ace (Sanwa Kagaku, Nagoya, Japan) when glycosuria was detected, and mice with a blood glucose level above 13.9 mmol/l were considered to be diabetic.
Preparation of splenocytes and adoptive transfer experiment
The spleen from each mouse was removed aseptically and minced. After lysing red blood cells, the cells were washed three times with PBS. Splenocytes from donor diabetic female NOD mice (16–32 weeks old; blood glucose >13.9 mmol/l) were resuspended at an appropriate concentration for transfer (0.8×107 cells/ml), and 250 µl of the cell suspension (including 2×106 splenocytes) was injected intraperitoneally into each female NOD scid recipient.
Drug administration
N-acetyl-cysteine (A7250; Sigma, St. Louis, Mo., USA) was administered to NOD scid recipients in the drinking water (1 mg/ml) in the NAC group for the indicated period in each experiment. In the control group, the recipient mice had free access to water.
Histological examination
The pancreas of each recipient was removed 2 weeks after transfer, then fixed in 10% formaldehyde, and embedded in paraffin. Thin sections at ten levels, 150 µm apart, were cut for staining with haematoxylin–eosin to evaluate islet-infiltrating cells by light microscopy. At least 40 islets from each recipient mouse were observed and scored using the following criteria: grade 0, islets free of insulitis; grade 1, peri-insulitis; grade 2, intra-insulitis with mononuclear cell infiltration of less than 50% of the area of each islet; grade 3, intra-insulitis with mononuclear cell infiltration of more than 50% of the area of each islet.
Immunohistochemical examination
The pancreas of each recipient mouse was embedded in optimal cutting temperature compound (Tissue TEK, Tokyo, Japan) and frozen in liquid nitrogen. Sections (10 µm thick) were cut with a cryostat, placed on 3-amino-propyltriethoxysilane-coated slides and fixed in ice-cold acetone for 10 min. Slides were washed with PBS and then incubated with FITC-conjugated anti-CD8 antibody or PE-conjugated anti-CD4 antibody (Pharmingen, San Diego, Calif., USA) at 37 °C for 1 h. Following subsequent washes with PBS, specimens were observed with a fluorescence microscope (Olympus, Tokyo, Japan).
Cell purification and polyclonal stimulation of splenocytes
To purify CD4-positive or CD8-positive splenocytes, splenocytes were prepared by magnetic separation using a MiniMACS system (Miltenyi Biotec, Auburn, Calif., USA) according to the manufacturer’s instructions. Briefly, splenocytes were incubated with anti-CD4 or anti-CD8 magnetic microbeads for 15 min, washed and collected on a magnetic flow-through column. To stimulate CD4-positive or CD8-positive splenocytes, cells were suspended in RPMI 1640 medium (Gibco-BRL, Grand Island, N.Y., USA) supplemented with 2% heat-inactivated fetal bovine serum (Gibco-BRL) and penicillin/streptomycin (Gibco-BRL). The CD4-positive or CD8-positive splenocytes (0.5×106) resuspended in 250 µl culture medium were transferred to each well of a 96-well plate precoated with anti-CD3 antibody, and anti-CD28 antibody was added to each well (final concentration 1 µg/ml; Pharmingen). In other sets of experiments “unpurified” splenocytes were used, and were transferred in amounts of (1×106) to each well of a 96-well plate and stimulated with anti-CD3 antibody (final concentration 5 µg/ml). The cells were cultured for 72 h at 37 °C in a humidified 5% CO2 atmosphere. The supernatant was collected at the end of culture and frozen at −80 °C until cytokine assay.
Flow cytometry
FITC- or PE-labelled antibodies against CD4, CD8 and T-cell receptor were purchased from Pharmingen. Cells were incubated with labelled antibodies for 20 min at 4 °C and washed twice. Samples were analysed on an EPICS XL (Beckman Coulter, Miami, Fla., USA). The numbers of CD4-positive and CD8-positive cells with T-cell receptor were counted.
Cytokine measurement by ELISA
Each cytokine (IFN-γ, IL-4, IL-2) was measured by ELISA. Briefly, a flat-bottom 96-well plate was coated with anti-IFN-γ, anti-IL-4 or anti-IL-2 antibodies (Pharmingen) with overnight incubation at 4 °C. Collected supernatants and standards (purified recombinant IFN-γ, IL-4, IL-2; Pharmingen) were added, and the plate was incubated for another 2 h. After washing, biotinylated anti-IFN-γ, anti-IL-4 or anti-IL-2 antibodies (Pharmingen) were added, which was followed by another 1-h period of incubation. AB solution (Vecstatin ABC kit; Vector Laboratories, Burlingame, Calif., USA) was then added and the plate was incubated for another 30 min. Finally, the colour reagent (TMB substrate; Pharmingen) was added and the optical density was measured using an ELISA reader (Bio-Rad, Richmond, Calif., USA) at 450 nm. The amount of cytokine present was determined from standard curves.
Semi-quantitative PCR analysis of cytokine mRNA
Total RNA was extracted from the pancreas of recipients using an Rneasy Mini Kit (Qiagen, Tokyo, Japan). The extracted RNA was reverse-transcribed using a Not I-d(T)18 primer and a First-Strand cDNA synthesis kit (Amersham Pharmacia Biotech, UK), according to the manufacturer’s instructions. Semi-quantitative PCR was carried out for IFN-γ, IL-4, IL-1β, IL-2, TNF-α, FAS and GAPDH (internal control) in an ABI Prism 7700 sequence detector (PE Applied Biosystems, Tokyo, Japan). Briefly, the probes were labelled with the fluorescent reporter dye FAM (6-carboxylfluorescein, covalently linked to the 5′ end of the oligonucleotide) and the quencher TAMRA. The primer and probe sequences used have been reported elsewhere [12, 13]. All reactions were performed using TaqMan Universal MasterMix (PE Applied Biosystems, Tokyo, Japan). The obtained mRNA level was expressed relative to the GAPDH PCR product amplified from the same sample ([sample PCR product/GAPDH PCR product]×constant).
Statistical analysis
Results are presented as means ± SEM. Log-rank test was used to compare the incidence of diabetes in the recipients. Differences in insulitis score, cytokine production levels and mRNA expression levels between the two groups were analysed using the Mann–Whitney U test for non-parametric unpaired observations.
Results
Firstly, we assessed the effect of NAC on the induction of diabetes by splenocytes from diabetic NOD mice. We transferred 2×106 splenocytes from donor diabetic female NOD mice into female NOD scid recipients, and just after transfer, NAC was delivered via the drinking water to recipient NOD scid mice in the NAC group. Surprisingly, as shown in Fig. 1, treatment with NAC significantly accelerated the transfer of diabetes to NOD scid recipients (p<0.002 by log-rank test). When splenocytes were transferred from non-diabetic donor female NOD mice (8 weeks old) to NOD scid recipients and NAC was delivered just after transfer, NAC-induced acceleration of diabetes was not observed in the recipients of non-diabetic NOD splenocytes, indicating that the accelerating effect of NAC is limited to the late stage (diabetic phase; data not shown). To exclude the possibility that NAC treatment could affect the vulnerability of beta cells in the recipients, we treated NOD scid recipients with NAC from 4 weeks before transfer to just before transfer and discontinued the treatment after the transfer of splenocytes from diabetic donor NOD mice. Treatment before transfer did not accelerate the transfer of diabetes into NOD scid recipients (Fig. 2).
Cumulative incidence of diabetes in NOD scid recipients after transfer of diabetogenic splenocytes. After transfer of splenocytes from diabetic NOD mice to NOD scid recipients, N-acetyl-cysteine was administered to NOD scid mice in the drinking water in the NAC group (n=25, white circles). In the control group (n=25, black circles), NOD scid recipient mice had free access to water. * p<0.002 vs control by log-rank test
Cumulative incidence of diabetes in NOD scid recipients treated with N-acetyl-cysteine before transfer of diabetogenic splenocytes. NOD scid recipients were treated with N-acetyl-cysteine for 4 weeks before transfer of splenocytes from diabetic NOD mice, and the treatment was discontinued after transfer (NAC group, n=10, white circles; control group, n=10, black circles)
To dissect the process of disease acceleration, we evaluated the pancreas of the recipients 14 days after transfer. Infiltration of mononuclear cells into pancreatic islets was observed in both the NAC group and the control group. However, the grade of mononuclear cell infiltration, “insulitis score” (Fig. 3), was significantly higher in the NAC group than in the control group (p=0.025, Mann–Whitney U test). In addition, immunohistochemical analysis revealed that CD8-positive cells invaded pancreatic islets in the NAC group that were greater than those in the control group (Fig. 4). When an islet with CD8-positive cell infiltration of more than 50% of its area was described as a CD8-dominant islet, the number of CD8-dominant islets in the NAC group was significantly greater than that in the control group (14 CD8-dominant islets/23 islets in the NAC group vs 1 CD8-dominant islet/21 islets in the control group; p<0.0001, Fisher’s exact test). Next we examined cytokine mRNA expression levels in the pancreas of the recipients 14 days after transfer or at the onset of diabetes. Expression of IFN-γ in the pancreas of the NAC group was higher than that in the pancreas of the control group at the onset of diabetes (p=0.004 vs control by Mann–Whitney U test; Fig. 5). Expression of FAS and TNF-α in the pancreas of the NAC group was higher than that in the control group, but the difference was not statistically significant. There was no difference between the two groups in the expression levels of IL-4, IL-2 and IL-1β in the pancreas (data not shown).
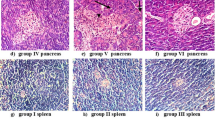
Histological evaluation of the pancreas of NOD scid recipients in the NAC group and the control group 14 days after transfer of diabetogenic splenocytes. The pancreas of NOD scid recipients in the NAC group and the control group was studied by staining with haematoxylin–eosin to evaluate islet-infiltrating cells. Mononuclear infiltration into pancreatic islets was graded in each group as follows: grade 0 (unfilled), grade 1 (solid diamonds), grade 2 (solid lines) and grade 3 (filled). p=0.025 by Mann–Whitney U test
Immunohistochemical evaluation of pancreas of NOD scid recipients in the NAC group and the control group 14 days after transfer of diabetogenic splenocytes. CD4-positive cells were stained with PE-conjugated antibody (red), and CD8-positive cells were stained with FITC-conjugated antibody (green). Each islet was analysed using identical sections
Expression level of IFN-γ in the pancreas of NOD scid recipients in the NAC group and the control group 14 days after transfer or at the onset of diabetes. The expression level of IFN-γ mRNA in the pancreas was evaluated by semi-quantitative PCR and expressed as relative ratio to GAPDH mRNA. * p=0.004 vs control by Mann–Whitney U test
Subsequently, we evaluated the effect of NAC on expansion and cytokine production of transferred lymphocytes in the periphery of NOD scid recipients. At 14 days after transfer, the numbers of CD4-positive and CD8-positive T cells in the spleen of the recipients in the NAC group (1.16×106 vs 0.23×106 respectively) were not different from those in the spleen of the recipients in the control group (1.18×106 vs 0.31×106 respectively). There was no difference in IFN-γ and IL-2 production by splenocytes of recipients stimulated with anti-CD3 antibody in vitro between the NAC group and the control group 14 days after transfer (Fig. 6). However, at the onset of diabetes, IFN-γ production of splenocytes in recipients in the NAC group was significantly higher than that in recipients in the control group (p=0.033, Mann–Whitney U test; Fig. 6). IL-2 production of splenocytes in the NAC group was also significantly higher than that in the control group (p=0.015, Mann–Whitney U test; Fig. 6), whereas there was no difference in IL-4 production between the two groups (data not shown).
Cytokine production of splenocytes from NOD scid recipients in the NAC group and the control group 14 days after transfer or at the onset of diabetes. Splenocytes from NOD scid recipients were stimulated with anti-CD3 antibody, and cytokines in the supernatants were measured by ELISA. Panel a: IFN-γ, b: IL-2. * p=0.033 vs control; # p=0.015 vs control by Mann–Whitney U test
Finally, we evaluated the effect of NAC in vitro on cytokine production by CD4 (or CD8)-positive splenocytes from diabetic NOD mice. Splenic CD4-positive cells from NOD mice with overt diabetes were stimulated with anti-CD3 antibody and anti-CD28 antibody, and NAC was added at a final concentration of 1 mmol/l. The production of IFN-γ and IL-2 after 72-h stimulation was accelerated by NAC, although acceleration of IL-4 production was not evident (Fig. 7). IFN-γ production by splenic CD8-positive cells was also enhanced by NAC.
Effect of N-acetyl-cysteine on cytokine production by splenic CD4-positive cells from diabetic NOD mice. Half a million splenic CD4-positive cells from female NOD mice were stimulated with anti-CD3 antibody and anti-CD28 antibody for 72 h. In the indicated wells, N-acetyl-cysteine was added at a final concentration of 1 mmol/l; NAC (+). In control wells, only medium was added; NAC (−). The concentration of IFN-γ, IL-4 and IL-2 in the supernatant after 72-h stimulation was measured by ELISA. The data are representative of three separate experiments
Discussion
NAC is a thiol-containing compound that has been widely used as a mucolytic agent and is recommended as an antidote for the treatment of acetaminophen overdose. It is generally thought that NAC is transported into cells and hydrolysed, and that it increases the synthesis of glutathione. However, the precise metabolic mechanism of NAC remains unclear [6]. NAC is used as an antioxidant because it increases the intracellular pool of glutathione and scavenges oxidants directly, and it may reduce cardiovascular events and renal dysfunction by increasing the reductive capacity of cells and improving coronary vascular function by a reduction of oxidative stress [7, 8]. It has also been reported that NAC could preserve pancreatic beta cells and insulin secretion in an animal model of Type 2 diabetes [14].
In this study, using an adoptive transfer system, we revealed that administration of NAC accelerated the transfer of autoimmune diabetes. The time taken to transfer diabetes to NOD scid recipients observed in the control group was consistent with that reported by another group [15], supporting our finding that administration of NAC accelerated the transfer of diabetes into the recipients in this system. After the onset of diabetes, NAC treatment affected cytokine profile both in the pancreas and in the periphery. However, there was no difference in the expansion of T cells and cytokine profiles in the periphery of the recipients 14 days after transfer, and accelerated pancreatic islet infiltration was found at this point, suggesting that treatment with NAC induced the accumulation and expansion of lymphocytes in the pancreas specifically at the pre-diabetic stage. Treatment with NAC in vivo could promote the proliferation of islet-reactive T cells in the pancreas and could thereby exacerbate islet destruction. The findings that the production of IL-2 by CD4-positive cells from diabetic NOD donor mice was significantly enhanced by NAC in vitro, and that a large number of CD8-positive cells invaded pancreatic islets of recipients treated with NAC (but very few without NAC) 14 days after transfer, support this hypothesis. NAC is also reported to promote cytolytic effector cell generation against tumours and viruses [16, 17]. The higher expression of IFN-γ and TNF-α in the pancreas of the recipients with NAC indicated accelerated immune-mediated beta cell destruction with NAC treatment as well. In addition, it is possible that NAC enhances cytotoxic activity of macrophage in the islets. We observed that the intracellular thiol level in peritoneal macrophages of recipients in the NAC group was higher compared with in the control group (data not shown), and it was reported that macrophages with higher thiol levels produced greater NO2 and IFN-γ than those with lower levels [11].
Regarding T-helper cell function, namely T-helper cell type 1 (Th1) and T-helper cell type 2 (Th2) balance, it was reported that treatment with NAC in vivo and in vitro promoted a Th1 response through increased intracellular glutathione level in antigen-presenting cells [18]. However, others reported that cytokine production by splenocytes of BALB/c mice was skewed towards a Th2 pattern when NAC was added in vitro [19]. In this study, we have shown that NAC enhances Th1 responses of NOD splenocytes in vitro and in vivo. Because diabetic NOD mice are likely to show Th1 responses while BALB/c mice are likely to show Th2 responses, this discrepancy might reflect the strain genetic backgrounds [20]. NAC may promote or suppress disease by supplying cystine and cysteine non-specifically to activate T cells and macrophages. In NOD mice it was reported that skewed Th1 responses (malignant phase) follow Th2 responses (benign phase), and that IFN-γ production by Th1 cells is accelerated just before the onset of diabetes [20]. Therefore, the outcomes of intervention with NAC depend on timing [11]. In fact, we did not observe NAC-induced acceleration of diabetes transfer in recipients of non-diabetic NOD splenocytes (8 weeks old), as they may not have Th1-skewed splenocytes. For patients with established pathogenic T cells, NAC treatment may become a double-edged sword. Finally, the possibility of a direct toxic effect of NAC on pancreatic islets was excluded by the finding that treatment with NAC before transfer did not accelerate the diabetes in recipients.
In human Type 1 diabetes and murine models of Type 1 diabetes, strong Th1 and defective Th2 responses were reported to be one of multiple defects in immunological responses [21, 22]. NAC has been used worldwide and many beneficial effects have been reported [6, 7, 8]; however, as shown here, in vivo administration of NAC can promote autoimmune reactivity, at least in a disease model of Type 1 diabetes. It may therefore be beneficial for clinicians to recognise the possible risk of promoting disease activity with the administration of NAC at a certain stage of autoimmune diabetes.
Abbreviations
- NAC:
-
N-acetyl-cysteine
- NOD:
-
non-obese diabetic
- scid :
-
severe combined immunodeficiency
- Th1:
-
T-helper cell type 1
- Th2:
-
T-helper cell type 2
References
Mathis D, Vence L, Benoist C (2001) β-cell death during progression to diabetes. Nature 414:792–798
Nomikos IN, Wang Y, Lafferty KJ (1989) Involvement of O2 radicals in “autoimmune” diabetes. Immunol Cell Biol 67:85–87
Corbett JA, Mikhael A, Shimizu J et al. (1993) Nitric oxide production in islets from nonobese diabetic mice: aminoguanidine-sensitive and resistant stages in the immunological diabetic process. Proc Natl Acad Sci USA 90:8992–8995
Fukuda M, Ikegami H, Kawaguchi Y, Sano T, Ogihara T (1995) Antioxidant, probucol, can inhibit the generation of hydrogen peroxide in islet cells induced by macrophages and prevent islet cell destruction in NOD mice. Biochem Biophys Res Commun 209:953–958
Piganelli JD, Flores SC, Cruz C et al. (2002) A metalloporphyrin-based superoxide dismutase mimic inhibits adoptive transfer of autoimmune diabetes by a diabetogenic T-cell clone. Diabetes 51:347–355
Meister A (1991) Glutathione deficiency produced by inhibition of its synthesis, and its reversal; applications in research and therapy. Pharmacol Ther 51:155–194
Tepel M, Giet M van der, Schwarzfeld C, Laufer U, Liermann D, Zidek W (2000) Prevention of radiographic-contrast-agent-induced reductions in renal function by acetylcysteine. N Engl J Med 343:180–184
Tepel M, Giet M van der, Statz M, Jankowski J, Zidek W (2003) The antioxidant acetylcysteine reduces cardiovascular events in patients with end-stage renal failure. Circulation 107:992–995
Eylar E, Rivera-Quinones C, Molina C, Baez I, Molina F, Mercado CM (1993) N-acetylcysteine enhances T cell functions and T cell growth in culture. Int Immunol 5:97–101
Puerto M, Guayerbas N, Victor VM, Fuente MD (2002) Effects of N-acetylcysteine on macrophage and lymphocyte functions in a mouse model of premature ageing. Pharmacol Biochem Behav 73:797–804
Murata Y, Amao M, Hamuro J (2003) Sequential conversion of the redox status of macrophages dictates the pathological progression of autoimmune diabetes. Eur J Immunol 33:1001–1011
Oikawa Y, Shimada A, Kasuga A et al. (2003) Systemic administration of IL-18 promotes diabetes development in young nonobese diabetic mice. J Immunol 171:5865–5875
Overbergh L, Valckx D, Waer M, Mathieu C (1999) Quantification of murine cytokine mRNAs using real time quantitative reverse transcriptase PCR. Cytokine 11:305–312
Kaneto H, Kajimoto Y, Miyagawa J et al. (1999) Beneficial effects of antioxidants in diabetes. Diabetes 48:2398–2406
Tarbell KV, Lee M, Ranheim E et al. (2002) CD4+ T cells from glutamic acid decarboxylase (GAD)65-specific T cell receptor transgenic mice are not diabetogenic and can delay diabetes transfer. J Exp Med 196:481–492
Yim CY, Hibbs JB, McGregor JR, Galinsky RE, Samlowski WE (1994) Use of N-acetyl cysteine to increase intracellular glutathione during the induction of antitumor responses by IL-2. J Immunol 152:5796–5805
Boon ACM, Vos AP, Graus YMF, Rimmelzwaan GF, Osterhaus ADME (2002) In vitro effect of bioactive compounds on influenza virus specific B- and T-cell responses. Scand J Immunol 55:24–32
Peterson JD, Herzenberg LA, Vasquez K, Waltenbaugh C (1998) Glutathione levels in antigen-presenting cells modulate Th1 versus Th2 response patterns. Proc Natl Acad Sci USA 95:3071–3076
Monick MM, Samavati L, Butler NS et al. (2003) Intracellular thiols contribute to Th2 function via a positive role in IL-4 production. J Immunol 171:5107–5115
Shimada A, Charlton B, Edwards CT, Fathman CG (1996) β-cell destruction may be a late consequence of the autoimmune process in nonobese diabetic mice. Diabetes 45:1063–1067
Berman MA, Sandborg CI, Wang Z et al. (1996) Decreased IL-4 production in new onset type 1 insulin-dependent diabetes mellitus. J Immunol 157:4690–4696
Delovitch TL, Singh B (1997) The nonobese diabetic mouse as a model of autoimmune diabetes: immune dysregulation gets the NOD. Immunity 7:727–738
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Irie, J., Shimada, A., Oikawa, Y. et al. N-acetyl-cysteine accelerates transfer of diabetes into non-obese diabetic scid mice. Diabetologia 47, 1803–1809 (2004). https://doi.org/10.1007/s00125-004-1529-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-004-1529-x