Abstract
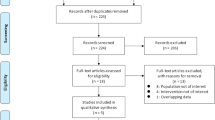
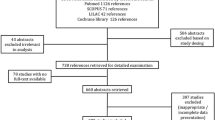
Since almost a decade, the use of bioprosthetic valves (BPV) has been increasing for the replacement of stenosed aortic valves. With the increasing use, a rise in the BPV failure is noted considering their limited durability. Redo-surgical aortic valve replacement (rSAVR) is by far the only gold standard treatment modality for replacement of deteriorated BPV. Recently, valve in valve-transcatheter aortic valve replacement (ViV-TAVR) is explored as the alternative minimally invasive procedure compared to the gold standard rSAVR. However, its efficacy remains the major concern. Hence, we aimed to conduct the meta-meta-analysis to evaluate the safety and efficacy of ViV-TAVI compared to redo-SAVR. Following PRISMA guidelines, we searched for a meta-analysis comparing the safety and efficacy of ViV-TAVR vs rSAVR from PubMed and included 9 analyses which compared the two modalities head-to-head in terms of outcomes and complications. We included various complications and outcomes like 30-day mortality, long-term mortality, procedural mortality, hospital readmission, and complications including acute MI, stroke, major bleeding, vascular complications, acute kidney injury, and new pacemaker implantation. We carried out a meta-meta-analysis by obtaining pooled odds ratio, 95% CI using random effect models. We found out that there was a significantly low risk of 30-day mortality (pooled OR:0.60; 95%CI:0.53–0.68; p < 0.00001) with no heterogeneity (p = 0.53; I2 = 0%) with ViV-TAVR vs rSAVR. Also, there was a reduced risk of procedural mortality (pooled OR:0.52; 95%CI:0.27–0.98; p = 0.04) with 0% heterogeneity with ViV-TAVR vs rSAVR. ViV-TAVI is associated with significantly reduced risk of 30-day mortality compared to rSAVR. Our meta-meta-analysis reinforces the safety and efficacy of ViV-TAVR as the procedure of choice for failed bioprosthetic (BP) valves in high-risk candidates.







Similar content being viewed by others
Data Availability
The data is collected from the studies published online, publicly available, and specific details related to data and/or analysis will be made available upon request.
Code Availability
Not applicable.
References
Osnabrugge RL, Mylotte D, Head SJ, Van Mieghem NM, Nkomo VT, LeReun CM, Bogers AJ, Piazza N, Kappetein AP. Aortic stenosis in the elderly: disease prevalence and number of candidates for transcatheter aortic valve replacement: a meta-analysis and modeling study. J Am Coll Cardiol. 2013;62(11):1002–12. https://doi.org/10.1016/j.jacc.2013.05.015.
Nkomo VT, Gardin JM, Skelton TN, Gottdiener JS, Scott CG, Enriquez-Sarano M. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368(9540):1005–11. https://doi.org/10.1016/s0140-6736(06)69208-8.
Otto CM, Prendergast B. Aortic-valve stenosis–from patients at risk to severe valve obstruction. N Engl J Med. 2014;371(8):744–56. https://doi.org/10.1056/NEJMra1313875.
Makkar RR, Fontana GP, Jilaihawi H, Kapadia S, Pichard AD, Douglas PS, Thourani VH, Babaliaros VC, Webb JG, Herrmann HC, Bavaria JE, Kodali S, Brown DL, Bowers B, Dewey TM, Svensson LG, Tuzcu M, Moses JW, Williams MR, Siegel RJ, Akin JJ, Anderson WN, Pocock S, Smith CR, Leon MB. Transcatheter aortic-valve replacement for inoperable severe aortic stenosis. N Engl J Med. 2012;366(18):1696–704. https://doi.org/10.1056/NEJMoa1202277.
Baumgartner H, Falk V, Bax JJ, De Bonis M, Hamm C, Holm PJ, Iung B, Lancellotti P, Lansac E, Rodriguez Muñoz D, Rosenhek R, Sjögren J, Tornos Mas P, Vahanian A, Walther T, Wendler O, Windecker S, Zamorano JL. 2017 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2017;38(36):2739–91. https://doi.org/10.1093/eurheartj/ehx391.
Rodriguez-Gabella T, Voisine P, Puri R, Pibarot P, Rodés-Cabau J. Aortic bioprosthetic valve durability: incidence, mechanisms, predictors, and management of surgical and transcatheter valve degeneration. J Am Coll Cardiol. 2017;70(8):1013–28. https://doi.org/10.1016/j.jacc.2017.07.715.
Brown JM, O’Brien SM, Wu C, Sikora JA, Griffith BP, Gammie JS. Isolated aortic valve replacement in North America comprising 108,687 patients in 10 years: changes in risks, valve types, and outcomes in the Society of Thoracic Surgeons National Database. J Thorac Cardiovasc Surg. 2009;137(1):82–90. https://doi.org/10.1016/j.jtcvs.2008.08.015.
Johnston DR, Soltesz EG, Vakil N, Rajeswaran J, Roselli EE, Sabik JF 3rd, Smedira NG, Svensson LG, Lytle BW, Blackstone EH. Long-term durability of bioprosthetic aortic valves: implications from 12,569 implants. Ann Thorac Surg. 2015;99(4):1239–47. https://doi.org/10.1016/j.athoracsur.2014.10.070.
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Fleisher LA, Jneid H, Mack MJ, McLeod CJ, O’Gara PT, Rigolin VH, Sundt TM 3rd, Thompson A. 2017 AHA/ACC Focused Update of the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2017;135(25):e1159–95. https://doi.org/10.1161/cir.0000000000000503.
Borger MA, Prasongsukarn K, Armstrong S, Feindel CM, David TE. Stentless aortic valve reoperations: a surgical challenge. Ann Thorac Surg. 2007;84(3):737–43. https://doi.org/10.1016/j.athoracsur.2007.04.061 (discussion 743-734).
François K, De Backer L, Martens T, Philipsen T, Van Belleghem Y, Bové T. Repeat aortic valve surgery: contemporary outcomes and risk stratification. Interact Cardiovasc Thorac Surg. 2021;32(2):213–21. https://doi.org/10.1093/icvts/ivaa257.
Chan V, Malas T, Lapierre H, Boodhwani M, Lam BK, Rubens FD, Hendry PJ, Masters RG, Goldstein W, Mesana TG, Ruel M. Reoperation of left heart valve bioprostheses according to age at implantation. Circulation. 2011;124(11 Suppl):S75-80. https://doi.org/10.1161/circulationaha.110.011973.
Dvir D, Webb JG, Bleiziffer S, Pasic M, Waksman R, Kodali S, Barbanti M, Latib A, Schaefer U, Rodés-Cabau J, Treede H, Piazza N, Hildick-Smith D, Himbert D, Walther T, Hengstenberg C, Nissen H, Bekeredjian R, Presbitero P, Ferrari E, Segev A, de Weger A, Windecker S, Moat NE, Napodano M, Wilbring M, Cerillo AG, Brecker S, Tchetche D, Lefèvre T, De Marco F, Fiorina C, Petronio AS, Teles RC, Testa L, Laborde JC, Leon MB, Kornowski R. Transcatheter aortic valve implantation in failed bioprosthetic surgical valves. JAMA. 2014;312(2):162–70. https://doi.org/10.1001/jama.2014.7246.
Tam DY, Vo TX, Wijeysundera HC, Dvir D, Friedrich JO, Fremes SE. Transcatheter valve-in-valve versus redo surgical aortic valve replacement for the treatment of degenerated bioprosthetic aortic valve: a systematic review and meta-analysis. Catheter Cardiovasc Interv. 2018;92(7):1404–11. https://doi.org/10.1002/ccd.27686.
Gozdek M, Raffa GM, Suwalski P, Kolodziejczak M, Anisimowicz L, Kubica J, Navarese EP, Kowalewski M. Comparative performance of transcatheter aortic valve-in-valve implantation versus conventional surgical redo aortic valve replacement in patients with degenerated aortic valve bioprostheses: systematic review and meta-analysis. Eur J Cardiothorac Surg. 2018;53(3):495–504. https://doi.org/10.1093/ejcts/ezx347.
Nalluri N, Atti V, Munir AB, Karam B, Patel NJ, Kumar V, Vemula P, Edla S, Asti D, Paturu A, Gayam S, Spagnola J, Barsoum E, Maniatis GA, Tamburrino F, Kandov R, Lafferty J, Kliger C. Valve in valve transcatheter aortic valve implantation (ViV-TAVI) versus redo-surgical aortic valve replacement (redo-SAVR): a systematic review and meta-analysis. J Interv Cardiol. 2018;31(5):661–71. https://doi.org/10.1111/joic.12520.
Sá M, Van den Eynde J, Simonato M, Cavalcanti LRP, Doulamis IP, Weixler V, Kampaktsis PN, Gallo M, Laforgia PL, Zhigalov K, Ruhparwar A, Weymann A, Pibarot P, Clavel MA. Valve-in-valve transcatheter aortic valve replacement versus redo surgical aortic valve replacement: an updated meta-analysis. JACC Cardiovasc Interv. 2021;14(2):211–20. https://doi.org/10.1016/j.jcin.2020.10.020.
Al-Abcha A, Saleh Y, Boumegouas M, Prasad R, Herzallah K, Baloch ZQ, Abdelkarim O, Rayamajhi S, Abela GS. Meta-analysis of valve-in-valve transcatheter aortic valve implantation versus redo-surgical aortic valve replacement in failed bioprosthetic aortic valve. Am J Cardiol. 2021. https://doi.org/10.1016/j.amjcard.2021.01.028.
Neupane S, Singh H, Lämmer J, Othman H, Yamasaki H, Rosman HS, Bossone E, Mehta RH, Eggebrecht H. Meta-analysis of transcatheter valve-in-valve implantation versus redo aortic valve surgery for bioprosthetic aortic valve dysfunction. Am J Cardiol. 2018;121(12):1593–600. https://doi.org/10.1016/j.amjcard.2018.02.054.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71.
Takagi H, Mitta S, Ando T. Meta-analysis of valve-in-valve transcatheter versus redo surgical aortic valve replacement. Thorac Cardiovasc Surg. 2019;67(4):243–50. https://doi.org/10.1055/s-0038-1668135.
Ahmed A, Levy KH. Valve-in-valve transcatheter aortic valve replacement versus redo surgical aortic valve replacement: a systematic review and meta-analysis. J Card Surg. 2021. https://doi.org/10.1111/jocs.15546.
Thandra A, Abusnina W, Jhand A, Shaikh K, Bansal R, Pajjuru VS, Al-Abdouh A, Kanmanthareddy A, Alla VM. Valve-in-valve transcatheter aortic valve replacement versus redo surgical valve replacement for degenerated bioprosthetic aortic valve: an updated meta-analysis comparing midterm outcomes. Catheter Cardiovasc Interv. 2021. https://doi.org/10.1002/ccd.29541.
GA Wells, B Shea, D O'Connell, J Peterson, V Welch, M Losos, P Tugwell. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Professor GA Wells, Department of Epidemiology and Commuunity Medicine. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. 2020.
Raschpichler MC, Woitek F, Chakravarty T, Flint N, Yoon SH, Mangner N, Patel CG, Singh C, Kashif M, Kiefer P, Holzhey D, Linke A, Stachel G, Thiele H, Borger MA, Makkar RR. Valve‐in‐valve for degenerated transcatheter aortic valve replacement versus valve‐in‐valve for degenerated surgical aortic bioprostheses: a 3‐center comparison of hemodynamic and 1‐year outcome. J Am Heart Assoc. 2020;9(14):e013973. https://doi.org/10.1161/JAHA.119.013973.
Hirji SA, Percy ED, Zogg CK, Malarczyk A, Harloff MT, Yazdchi F, Kaneko T. Comparison of in-hospital outcomes and readmissions for valve-in-valve transcatheter aortic valve replacement vs. reoperative surgical aortic valve replacement: a contemporary assessment of real-world outcomes. Eur Heart J. 2020;41(29):2747–55. https://doi.org/10.1093/eurheartj/ehaa252.
Ejiofor JI, Yammine M, Harloff MT, McGurk S, Muehlschlegel JD, Shekar PS, Cohn LH, Shah P, Kaneko T. Reoperative surgical aortic valve replacement versus transcatheter valve-in-valve replacement for degenerated bioprosthetic aortic valves. Ann Thorac Surg. 2016;102(5):1452–8. https://doi.org/10.1016/j.athoracsur.2016.05.086.
Silaschi M, Wendler O, Seiffert M, Castro L, Lubos E, Schirmer J, Blankenberg S, Reichenspurner H, Schäfer U, Treede H, MacCarthy P, Conradi L. Transcatheter valve-in-valve implantation versus redo surgical aortic valve replacement in patients with failed aortic bioprostheses†. Interact Cardiovasc Thorac Surg. 2016;24(1):63–70. https://doi.org/10.1093/icvts/ivw300.
Grubitzsch H, Zobel S, Christ T, Holinski S, Stangl K, Treskatsch S, Falk V, Laule M. Redo procedures for degenerated stentless aortic xenografts and the role of valve-in-valve transcatheter techniques†. Eur J Cardiothorac Surg. 2017;51(4):653–9. https://doi.org/10.1093/ejcts/ezw397.
Tuzcu EM, Kapadia SR, Vemulapalli S, Carroll JD, Holmes DR Jr, Mack MJ, Thourani VH, Grover FL, Brennan JM, Suri RM, Dai D, Svensson LG. Transcatheter aortic valve replacement of failed surgically implanted bioprostheses: The STS/ACC Registry. J Am Coll Cardiol. 2018;72(4):370–82. https://doi.org/10.1016/j.jacc.2018.04.074.
Onorati F, Biancari F, De Feo M, Mariscalco G, Messina A, Santarpino G, Santini F, Beghi C, Nappi G, Troise G, Fischlein T, Passerone G, Heikkinen J, Faggian G. Mid-term results of aortic valve surgery in redo scenarios in the current practice: results from the multicentre European RECORD (REdo Cardiac Operation Research Database) initiative†. Eur J Cardiothorac Surg. 2014;47(2):269–80. https://doi.org/10.1093/ejcts/ezu116.
Vogt PR, Brunner-LaRocca H, Sidler P, Zünd G, Truniger K, Lachat M, Turina J, Turina MI. Reoperative surgery for degenerated aortic bioprostheses: predictors for emergency surgery and reoperative mortality. Eur J Cardiothorac Surg. 2000;17(2):134–9. https://doi.org/10.1016/s1010-7940(99)00363-2.
Dvir D, Webb J, Brecker S, Bleiziffer S, Hildick-Smith D, Colombo A, Descoutures F, Hengstenberg C, Moat NE, Bekeredjian R, Napodano M, Testa L, Lefevre T, Guetta V, Nissen H, Hernández J-M, Roy D, Teles RC, Segev A, Dumonteil N, Fiorina C, Gotzmann M, Tchetche D, Abdel-Wahab M, Marco FD, Baumbach A, Laborde J-C, Kornowski R. Transcatheter aortic valve replacement for degenerative bioprosthetic surgical valves. Circulation. 2012;126(19):2335–44. https://doi.org/10.1161/CIRCULATIONAHA.112.104505.
Erlebach M, Wottke M, Deutsch MA, Krane M, Piazza N, Lange R, Bleiziffer S. Redo aortic valve surgery versus transcatheter valve-in-valve implantation for failing surgical bioprosthetic valves: consecutive patients in a single-center setting. J Thorac Dis. 2015;7(9):1494–500. https://doi.org/10.3978/j.issn.2072-1439.2015.09.24.
Grabert S, Lange R, Bleiziffer S. Incidence and causes of silent and symptomatic stroke following surgical and transcatheter aortic valve replacement: a comprehensive review. Interact Cardiovasc Thorac Surg. 2016;23(3):469–76. https://doi.org/10.1093/icvts/ivw142.
Woitek FJ, Stachel G, Kiefer P, Haussig S, Leontyev S, Schlotter F, Mende M, Hommel J, Crusius L, Spindler A, Mohr FW, Schuler G, Thiele H, Borger MA, Linke A, Holzhey D, Mangner N. Treatment of failed aortic bioprostheses: an evaluation of conventional redo surgery and transfemoral transcatheter aortic valve-in-valve implantation. Int J Cardiol. 2020;300:80–6. https://doi.org/10.1016/j.ijcard.2019.09.039.
Stankowski T, Aboul-Hassan SS, Seifi Zinab F, Herwig V, Stępiński P, Grimmig O, Just S, Harnath A, Muehle A, Fritzsche D, Perek B. Femoral transcatheter valve-in-valve implantation as alternative strategy for failed aortic bioprostheses: a single-centre experience with long-term follow-up. Int J Cardiol. 2020;306:25–34. https://doi.org/10.1016/j.ijcard.2020.02.035.
Deharo P, Bisson A, Herbert J, Lacour T, Etienne CS, Porto A, Theron A, Collart F, Bourguignon T, Cuisset T, Fauchier L. Transcatheter valve-in-valve aortic valve replacement as an alternative to surgical re-replacement. J Am Coll Cardiol. 2020;76(5):489–99. https://doi.org/10.1016/j.jacc.2020.06.010.
Patel PM, Chiou E, Cao Y, Binongo J, Guyton RA, Leshnower B, Grubb KJ, Chen EP. Isolated redo aortic valve replacement versus valve-in-valve transcatheter valve replacement. Ann Thorac Surg. 2021;112(2):539–45. https://doi.org/10.1016/j.athoracsur.2020.08.048.
Czerwińska-Jelonkiewicz K, Michałowska I, Witkowski A, Dąbrowski M, Księżycka-Majczyńska E, Chmielak Z, Kuśmierski K, Hryniewiecki T, Demkow M, Stępińska J. Vascular complications after transcatheter aortic valve implantation (TAVI): risk and long-term results. J Thromb Thrombolysis. 2014;37(4):490–8. https://doi.org/10.1007/s11239-013-0996-7.
Smith CR, Leon MB, Mack MJ, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Williams M, Dewey T, Kapadia S, Babaliaros V, Thourani VH, Corso P, Pichard AD, Bavaria JE, Herrmann HC, Akin JJ, Anderson WN, Wang D, Pocock SJ. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med. 2011;364(23):2187–98. https://doi.org/10.1056/NEJMoa1103510.
Chaudhry MA, Sardar MR. Vascular complications of transcatheter aortic valve replacement: a concise literature review. World J Cardiol. 2017;9(7):574–82. https://doi.org/10.4330/wjc.v9.i7.574.
Author information
Authors and Affiliations
Contributions
Conceptualization: Surya Kiran Aedma, Nida Khan. Methodology: Urvish K. Patel. Acquisition of data: Nida Khan, Abbas Altamimi, Nawal Ali, Jigisha Rakholiya. Formal analysis and investigation: Urvish K. Patel, Surya Kiran Aedma. Writing—original draft preparation: Surya Kiran Aedma, Nida Khan, Abbas Altamimi, Nawal Ali, Shubhi Jain, Karanrajsinh Raol, Sowmya Madireddy, Jigisha Rakholiya, Abdur Raheem, Rutikbhai Desai. Writing—review, critical feedback, and editing: Urvish K. Patel, Rizwan Rabbani, Suveenkrishna Pothuru. Funding acquisition: None. Resources: Supervision: Suveenkrishna Pothuru.
Corresponding author
Ethics declarations
Ethics Approval/Informed Consent/IRB Approval
Though this article does not contain any studies with direct involvement of human participants or animals performed by any of the authors, all procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to Participate
The data used in this study is deidentified and collected from the studies published online; thus, informed consent or IRB approval was not needed for this study.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Surya Kiran Aedma and Nida Khan are equally contributing first authors
This article is part of the Topical Collection on Medicine
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Aedma, S.K., Khan, N., Altamimi, A. et al. Umbrella Meta-analysis Evaluating the Effectiveness of ViV-TAVI vs Redo SAVR. SN Compr. Clin. Med. 4, 63 (2022). https://doi.org/10.1007/s42399-022-01136-x
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-022-01136-x