Abstract
Purpose
To compare the evolution of the cardiometabolic parameters in patients with nonfunctioning adrenal incidentalomas (NFAI) and autonomous cortisol secretion (ACS) who underwent adrenalectomy and those who were conservatively managed.
Methods
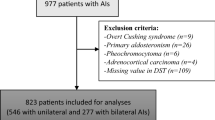
A retrospective study of all patients with NFAI and ACS submitted to surgery or in follow-up in our center between January 2011-October 2020. NFAI was defined as an adrenal incidentaloma with cortisol post-dexamethasone suppression test (DST) ≤ 50 nmol/L and ACS as values >50 nmol/L without specific clinical signs of overt Cushing´s syndrome.
Results
A total of 486 patients with NFAI (16 in the surgical group and 470 in the control group) and 259 with ACS (42 in the surgical group and 217 in the control group) were included. At baseline, patients with ACS were older than those with NFAI (P = 0.010). After adjusting by age, patients with ACS had a higher prevalence of hypertension (adjusted OR = 1.9 [1.36–2.60]) and higher levels of fasting plasma glucose and HbA1c (adjusted β = 6.9 [2.05–11.83] and adjusted β = 0.4 [0.12–0.63]) than NFAI. During follow-up, ACS patients who underwent adrenalectomy had a greater decrease in glucose levels (−16.6 ± 45.07 vs. −1.0 ± 26.92 mg/dL, P = 0.035) and in triglycerides (−20.21 ± 55.97 vs. 1.3 ± 59.23 mg/dL, P = 0.029) than ACS patients conservatively managed. NFAI patients who underwent surgery experienced an improvement in systolic blood pressure compared to NFAI of the conservative group (−11.1 ± 15.94 vs 1.0 ± 17.54 mmHg, P = 0.009).
Conclusion
The benefits of adrenalectomy in the cardiometabolic profile in adrenal incidentalomas are not limited only to the group of patients with ACS, an improvement in blood pressure control is also observed in NFAI patients after surgery.

Similar content being viewed by others
References
M. Fassnacht, W. Arlt, I. Bancos, H. Dralle, J. Newell-Price, A. Sahdev et al. Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 175, G1–G34 (2016). https://doi.org/10.1530/EJE-16-0467
M. Araujo-Castro, M. Iturregui Guevara, M. Calatayud Gutiérrez, P. Parra Ramírez, P. Gracia Gimeno, F.A. Hanzu et al. Practical guide on the initial evaluation, follow-up, and treatment of adrenal incidentalomas Adrenal Diseases Group of the Spanish Society of Endocrinology and Nutrition. Endocrinol. Diabetes y. Nutr. 67, 408–419 (2020). https://doi.org/10.1016/j.endinu.2020.03.002
I. Chiodini, V. Morelli, Subclinical hypercortisolism: How to deal with it? Front Horm. Res 46, 28–38 (2016). https://doi.org/10.1159/000443862
I. Bancos, F. Alahdab, R.K. Crowley, V. Chortis, D.A. Delivanis, D. Erickson et al. Improvement of cardiovascular risk factors after adrenalectomy in patients with adrenal tumors and subclinical Cushing’s syndrome: A systematic review and meta-Analysis. Eur. J. Endocrinol. 175, R283–R295 (2016). https://doi.org/10.1530/EJE-16-0465
I. Chiodini, V. Morelli, A.S. Salcuni, C. Eller-Vainicher, M. Torlontano, F. Coletti et al. Beneficial metabolic effects of prompt surgical treatment in patients with an adrenal incidentaloma causing biochemical hypercortisolism. J. Clin. Endocrinol. Metab. 95, 2736–2745 (2010). https://doi.org/10.1210/jc.2009-2387
M. Iacobone, M. Citton, M. Scarpa, G. Viel, M. Boscaro, Nitti D. Systematic review of surgical treatment of subclinical Cushing’s syndrome. Br J Surg. 2015;102. https://doi.org/10.1002/bjs.9742.
L. Petramala, G. Cavallaro, M. Galassi, C. Marinelli, G. Tonnarini, A. Concistrè et al. Clinical benefits of unilateral adrenalectomy in patients with subclinical hypercortisolism due to adrenal incidentaloma: results from a single center. High. Blood Press Cardiovasc Prev. 24, 69–75 (2017). https://doi.org/10.1007/s40292-017-0182-7
A. Toniato, I. Merante-Boschin, G. Opocher, M.R. Pelizzo, F. Schiavi, E. Ballotta, Surgical versus conservative management for subclinical cushing syndrome in adrenal incidentalomas: A prospective randomized study. Ann. Surg. 249, 388–391 (2009). https://doi.org/10.1097/SLA.0b013e31819a47d2
V. Morelli, C. Aresta, E. Passeri, F. Pugliese, S. Corbetta, M. Arosio et al. Adrenalectomy Improves Blood Pressure and Metabolic Control in Patients With Possible Autonomous Cortisol Secretion: Results of a RCT. Front. Endocrinol. 13, 1–10 (2022). https://doi.org/10.3389/fendo.2022.898084
T. Deutschbein, G. Reimondo, G. Di Dalmazi, I. Bancos, J. Patrova, D.A. Vassiliadi, et al. Age-dependent and sex-dependent disparity in mortality in patients with adrenal incidentalomas and autonomous cortisol secretion: an international, retrospective, cohort study. Lancet Diabetes Endocrinol. 2022. https://doi.org/10.1016/S2213-8587(22)00100-0
G. Di Dalmazi, V. Vicennati, E. Rinaldi, A.M. Morselli-Labate, E. Giampalma, C. Mosconi et al. Progressively increased patterns of subclinical cortisol hypersecretion in adrenal incidentalomas differently predict major metabolic and cardiovascular outcomes: A large cross-sectional study. Eur. J. Endocrinol. 166, 669–677 (2012). https://doi.org/10.1530/EJE-11-1039
M. Peppa, E. Boutati, C. Koliaki, N. Papaefstathiou, E. Garoflos, T. Economopoulos et al. Insulin resistance and metabolic syndrome in patients with nonfunctioning adrenal incidentalomas: A cause-effect relationship? Metabolism 59, 1435–1441 (2010). https://doi.org/10.1016/j.metabol.2010.01.007
H. Yilmaz, N.B. Tütüncü, M. Şahin, Two-year follow-up of thirty-two non-functional benign adrenal incidentalomas. J. Endocrinol. Invest 32, 913–916 (2009). https://doi.org/10.3275/6431
J.H. Kim, M.J. Kim, J.H. Lee, J.W. Yoon, C.S. Shin, M.J. Kim et al. Nonfunctioning adrenal incidentalomas are not clinically silent: A longitudinal cohort study. Endocr. Pr. 26, 1406–1415 (2020). https://doi.org/10.4158/EP-2020-0182
F. Athanasouli, G. Georgiopoulos, N. Asonitis, F. Petychaki, A. Savelli, E. Panou et al. Nonfunctional adrenal adenomas and impaired glucose metabolism: a systematic review and meta-analysis. Endocrine 74, 50–60 (2021). https://doi.org/10.1007/s12020-021-02741-x
R. Emral, B.İ. Aydoğan, A.D. Köse, Ö. Demir, D. Çorapçıoğlu, Could a nonfunctional adrenal incidentaloma be a risk factor for increased carotid intima-media thickness and metabolic syndrome. Endocrinol. Diabetes y. Nutr. 66, 402–409 (2019). https://doi.org/10.1016/j.endinu.2019.01.007
M. Araujo‐Castro. Cardiometabolic profile and urinary metabolomic alterations in non‐functioning adrenal incidentalomas. A review. Clin Endocrinol (Oxf). 2022. https://doi.org/10.1111/cen.14745.
U. Khan, Nonfunctioning and subclinical cortisol secreting adrenal incidentalomas and their association with metabolic syndrome: A systematic review. Indian J. Endocrinol. Metab. 23, 332–346 (2019). https://doi.org/10.4103/ijem.IJEM-52-19
G.B. Cansu, R. Sari, N. Yilmaz, S. Özdem, M. Çubuk, C. GB et al. Markers of subclinical cardiovascular disease in nonfunctional adrenal incidentaloma patients without traditional cardiovascular risk factors. Exp. Clin. Endocrinol. Diabetes 125, 57–63 (2017). https://doi.org/10.1055/s-0042-109866
M. Arruda, E. Mello Ribeiro Cavalari, M. Pessoa De Paula, F. Fernandes Cordeiro De Morais, G. Furtado Bilro, M.C. Alves Coelho et al. The presence of nonfunctioning adrenal incidentalomas increases arterial hypertension frequency and severity, and is associated with cortisol levels after dexamethasone suppression test. J. Hum. Hypertens. 32, 3–11 (2017). https://doi.org/10.1038/s41371-017-0011-4
G. Bernini, A. Moretti, P. Iacconi, P. Miccoli, R. Nami, B. Lucani et al. Anthropometric, haemodynamic, humoral and hormonal evaluation in patients with incidental adrenocortical adenomas before and after surgery. Eur. J. Endocrinol. 148, 213–219 (2003). https://doi.org/10.1530/eje.0.1480213
S. Midorikawa, H. Sanada, S. Hashimoto, T. Suzuki, T. Watanabe, The improvement of insulin resistance in patients with adrenal incidentaloma by surgical resection. Clin. Endocrinol. (Oxf.) 54, 797–804 (2001). https://doi.org/10.1046/j.1365-2265.2001.01274.x
M. Araujo-Castro, A. García Cano, L. Jiménez Mendiguchía, H. F. Escobar-Morreale, P. Valderrábano. Diagnostic accuracy of the different hormonal tests used for the diagnosis of autonomous cortisol secretion. Sci Rep. 2021;11. https://doi.org/10.1038/s41598-021-00011-4.
P.A. Harris, R. Taylor, R. Thielke, J. Payne, N. Gonzalez, J.G. Conde, Research electronic data capture (REDCap)-A metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inf. 42, 377–381 (2009). https://doi.org/10.1016/j.jbi.2008.08.010
P.A. Harris, R. Taylor, B.L. Minor, V. Elliott, M. Fernandez, L. O’Neal, et al. The REDCap consortium: Building an international community of software platform partners. J Biomed Inform. 2019;95. https://doi.org/10.1016/j.jbi.2019.103208.
M. Araujo-Castro, M.A. Sampedro Núñez, M. Marazuela, Autonomous cortisol secretion in adrenal incidentalomas. Endocrine 64(1), 1–13 (2019). https://doi.org/10.1007/s12020-019-01888-y. Epub 2019 Mar
L. Tauchmanovà, R. Rossi, B. Biondi, M. Pulcrano, V. Nuzzo, E.A. Palmieri et al. Patients with subclinical Cushing’s syndrome due to adrenal adenoma have increased cardiovascular risk. J. Clin. Endocrinol. Metab. 87, 4872–4878 (2002). https://doi.org/10.1210/JC.2001-011766
V. Morelli, G. Reimondo, R. Giordano, S. Della Casa, C. Policola, S. Palmieri et al. Long-term follow-up in adrenal incidentalomas: An Italian multicenter study. J. Clin. Endocrinol. Metab. 99, 827–834 (2014). https://doi.org/10.1210/jc.2013-3527
R. Rossi, L. Tauchmanova, A. Luciano, M. Di Martino, C. Battista, L. Del Viscovo et al. Subclinical Cushing’s syndrome in patients with adrenal incidentaloma: clinical and biochemical features. J. Clin. Endocrinol. Metab. 85, 1440–1448 (2000). https://doi.org/10.1210/JCEM.85.4.6515
B.Y. Kim, A.R. Chun, K.J. Kim, C.H. Jung, S.K. Kang, J.O. Mok et al. Clinical characteristics and metabolic features of patients with adrenal incidentalomas with or without subclinical cushing’s syndrome. Endocrinol. Metab. (Seoul., Korea) 29, 457–463 (2014). https://doi.org/10.3803/ENM.2014.29.4.457
G. Di Dalmazi, V. Vicennati, S. Garelli, E. Casadio, E. Rinaldi, E. Giampalma et al. Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing’s syndrome: a 15-year retrospective study. Lancet Diabetes Endocrinol. 2, 396–405 (2014). https://doi.org/10.1016/S2213-8587(13)70211-0
L. Papanastasiou, K. Alexandraki, I.I. Androulakis, S. Fountoulakis, T. Kounadi, A. Markou et al. Concomitant alterations of metabolic parameters, cardiovascular risk factors and altered cortisol secretion in patients with adrenal incidentalomas during prolonged follow-up. Clin. Endocrinol. (Oxf.) 86, 488–498 (2017). https://doi.org/10.1111/cen.13294
M. Araujo-Castro, C. Robles Lázaro, P. Parra Ramírez, M. Cuesta Hernández, M.A. Sampedro Núñez, M. Marazuela et al. Cardiometabolic profile of non-functioning and autonomous cortisol-secreting adrenal incidentalomas. Is the cardiometabolic risk similar or are there differences? Endocrine 66, 650–659 (2019). https://doi.org/10.1007/s12020-019-02066-w
J.A. Whitworth, G.J. Mangos, J.J. Kelly, Cushing, cortisol, and cardiovascular disease. Hypertension 36, 912–916 (2000). https://doi.org/10.1161/01.HYP.36.5.912
G. Mazziotti, C. Gazzaruso, A. Giustina, Diabetes in Cushing syndrome: Basic and clinical aspects. Trends Endocrinol. Metab. 22, 499–506 (2011). https://doi.org/10.1016/j.tem.2011.09.001
M. Araujo-Castro, C. Robles Lázaro, P. Parra Ramírez, R. García Centeno, P. Gracia Gimeno, M.T. Fernández-Ladreda et al. Maximum adenoma diameter, regardless of uni- or bilaterality, is a risk factor for autonomous cortisol secretion in adrenal incidentalomas. J. Endocrinol. Invest 44, 2349–2357 (2021). https://doi.org/10.1007/s40618-021-01539-y
H. Olsen, E. Nordenström, A. Bergenfelz, U. Nyman, S. Valdemarsson, E. Palmqvist, Subclinical hypercortisolism and CT appearance in adrenal incidentalomas: A multicenter study from Southern Sweden. Endocrine 42, 164–173 (2012). https://doi.org/10.1007/s12020-012-9622-2
E. Vassilatou, A. Vryonidou, S. Michalopoulou, J. Manolis, J. Caratzas, C. Phenekos et al. Hormonal activity of adrenal incidentalomas: Results from a long-term follow-up study. Clin. Endocrinol. (Oxf.) 70, 674–679 (2009). https://doi.org/10.1111/j.1365-2265.2008.03492.x
D.A. Vassiliadi, G. Ntali, E. Vicha, S. Tsagarakis, High prevalence of subclinical hypercortisolism in patients with bilateral adrenal incidentalomas: A challenge to management. Clin. Endocrinol. (Oxf.) 74, 438–444 (2011). https://doi.org/10.1111/j.1365-2265.2010.03963.x
E. Vassilatou, A. Vryonidou, D. Ioannidis, S.A. Paschou, M. Panagou, I. Tzavara, Bilateral adrenal incidentalomas differ from unilateral adrenal incidentalomas in subclinical cortisol hypersecretion but not in potential clinical implications. Eur. J. Endocrinol. 171, 37–45 (2014). https://doi.org/10.1530/EJE-13-0848
F. Ceccato, I. Tizianel, G. Voltan, G. Maggetto, I. Merante Boschin, E. Quaia et al. Attenuation Value in Adrenal Incidentalomas: A Longitudinal Study. Front Endocrinol. (Lausanne) 12, 1–9 (2021). https://doi.org/10.3389/fendo.2021.794197
M. Iacobone, M. Citton, G. Viel, R. Boetto, I. Bonadio, I. Mondi et al. Adrenalectomy may improve cardiovascular and metabolic impairment and ameliorate quality of life in patients with adrenal incidentalomas and subclinical Cushing’s syndrome. Surg. (U. S.). 152, 991–997 (2012). https://doi.org/10.1016/j.surg.2012.08.054
M.P. Ricciato, V. Di Donna, G. Perotti, A. Pontecorvi, R. Bellantone, S.M. Corsello, The role of adrenal scintigraphy in the diagnosis of subclinical Cushing’s syndrome and the prediction of post-surgical hypoadrenalism. World J. Surg. 38, 1328–1335 (2014). https://doi.org/10.1007/S00268-014-2482-6
M. Tsuiki, A. Tanabe, S. Takagi, M. Naruse, K. Takano, Cardiovascular risks and their long-term clinical outcome in patients with subclinical Cushing’s syndrome. Endocr. J. 55, 737–745 (2008). https://doi.org/10.1507/endocrj.K07E-177
B. Masserini, V. Morelli, S. Palmieri, C. Eller-Vainicher, V. Zhukouskaya, E. Cairoli et al. Lipid abnormalities in patients with adrenal incidentalomas: Role of subclinical hypercortisolism and impaired glucose metabolism. J. Endocrinol. Invest 38, 623–628 (2015). https://doi.org/10.1007/s40618-014-0232-0
M. Peppa, C. Koliaki, S.A. Raptis, Adrenal incidentalomas and cardiometabolic morbidity: An emerging association with serious clinical implications. J. Intern Med 268, 555–566 (2010). https://doi.org/10.1111/j.1365-2796.2010.02291.x
A. Comlekci, S. Yener, S. Ertilav, M. Secil, B. Akinci, T. Demir et al. Adrenal incidentaloma, clinical, metabolic, follow-up aspects: Single centre experience. Endocrine 37, 40–46 (2010). https://doi.org/10.1007/s12020-009-9260-5
I.I. Androulakis, G.A. Kaltsas, G.E. Kollias, A.C. Markou, A.K. Gouli, D.A. Thomas et al. Patients with apparently nonfunctioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J. Clin. Endocrinol. Metab. 99, 2754–2762 (2014). https://doi.org/10.1210/jc.2013-4064
M. Araujo-Castro, P. Valderrábano, H.F. Escobar-Morreale, F.A. Hanzu, G. Casals, Urine steroid profile as a new promising tool for the evaluation of adrenal tumors. Literature review. Endocrine 72, 40–48 (2020). https://doi.org/10.1007/s12020-020-02544-6
M.M. Tuna, N.N. Imga, B.A. Doǧan, F.M. Yilmaz, C. Topçuoǧlu, G. Akbaba et al. Non-functioning adrenal incidentalomas are associated with higher hypertension prevalence and higher risk of atherosclerosis. J. Endocrinol. Invest 37, 765–768 (2014). https://doi.org/10.1007/s40618-014-0106-5
F. Yılmaz, H. Sözel, M. Keleş, Ü Yılmaz. Frequency of masked hypertension in patients with nonfunctioning adrenal incidentalomas with normal and high normal blood pressure. Ir J Med Sci. 2021. https://doi.org/10.1007/s11845-021-02734-9
L.K. Nieman, B.M.K.K. Biller, J.W. Findling, J. Newell-Price, M.O. Savage, P.M. Stewart et al. The diagnosis of cushing’s syndrome: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 93, 1526–1540 (2008). https://doi.org/10.1210/jc.2008-0125
Funding
SENDIMAD: BECA SENDIMAD de Ayuda a la Investigación en Endocrinología, Nutrición y Diabetes 2019 IRYCIS: Convocatoria intramural de ayudas a proyectos de investigación de investigadores noveles, investigadores clínicos asociados y/o grupos emergentes del Hospital Universitario Ramón y Cajal 2019.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The study was approved by the Ethics Committee of Hospital Universitario Ramón y Cajal on 5TH August 2020 (Approval date: 28th of July 2020, Code: 395.
Informed consent
Due to the retrospective nature of the study, the Ethical Committee has approved the need of informed consent only in those patients who continued in follow-up in our center.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Araujo-Castro, M., Mínguez Ojeda, C., Sánchez Ramírez, M.N. et al. Adrenalectomy improves blood pressure control in nonfunctioning adrenal incidentalomas and glycemic and lipid control in patients with autonomous cortisol secretion. Endocrine 78, 142–150 (2022). https://doi.org/10.1007/s12020-022-03120-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-022-03120-w