Abstract
Objective
To study the differences in the cardiometabolic profile between patients with non-functioning adrenal incidentalomas (NFAI) and incidentalomas with autonomous cortisol secretion (ACS).
Methods
A total of 149 patients with adrenal incidentalomas were retrospectively evaluated and followed-up for a mean time of 34.6 months at Departments of Endocrinology and Metabolic Diseases Units of four tertiary Spanish hospitals. Patients were grouped as NFAI or ACS adenomas based on two cutoffs in the dexamethasone suppression test (DST): 3.0 µg/dl (NFAIDST3 or ACSDST3) and 1.8 µg/dl (ACSDST1.8 and NFAIDST1.8).
Results
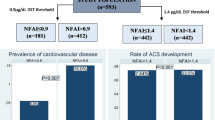
The mean age of both groups was 62.0 (10.31) and was similar in ACS and NFAI. The prevalence of diabetes, high blood pressure, cardiovascular, and cerebrovascular disease was higher in ACS than in NFAI, but differences only reached statistical significance for cerebrovascular disease using the 3.0 µg/dl cutoff (15.8% vs 2.3%, p = 0.01) and for diabetes using the 1.8 µg/dl cutoff (38.0% vs 22.0%, p = 0.04). No differences were found in the prevalence of dyslipidemia. The prevalence of obesity was lower in patients with ACS than in NFAI 26.3% vs 39.2%, p = 0.18 (NFAIDST3 vs ACSDST3) and 32.1% vs 40.6%, p = 0.56 (ACSDST1.8 vs NFAIDST1.8), but the differences did not reach statistical significance. Maximum adenoma diameter (R-squared = 0.15, p < 0.001) and cerebrovascular disease (OR = 1.59, p = 0.04) were the only parameters that could be predicted by the DST. The DST was an inadequate predictor of clinical (systolic and diastolic blood pressure, body mass index), hormonal (DHEAS, ACTH, UFC, and basal serum cortisol), biochemical (glucose, cholesterol, LDL, HDL, and triglycerides), and other radiological (laterality, lipid content) parameters. Throughout the follow-up, patients did not develop overt Cushing’s Syndrome; three NFAIDST3 developed ACSDST3, eight NFAIDST1.8 developed ACSDST1.8, and one NFAIDST1.8 progressed to ACSDST3. In both groups (NFAI and ACS) the metabolic profile remained stable.
Conclusions
Our data suggest higher prevalence of diabetes and cerebrovascular disease in ACS patients compared with NFAI. However, probably because of the small sample size, the differences only reached statistical significance using the cutoffs of 1.8 µg/dl for diabetes and 3.0 µg/dl for cerebrovascular disease. Patients with ACS and NFAI rarely progress to more aggressive forms of hypercortisolism, and the metabolic profile usually remains stable during the follow-up.

Similar content being viewed by others
References
M. Fassnacht, W. Arlt, I. Bancos, H. Dralle, J. Newell-Price, A. Sahdev et al. Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 175(2), G1–G34 (2016). https://doi.org/10.1530/EJE-16-0467
M. Terzolo, A. Stigliano, I. Chiodini, P. Loli, L. Furlani, G. Arnaldi et al. AME position statement on adrenal incidentaloma. Eur. J. Endocrinol. 164(6), 851–870 (2011). https://doi.org/10.1530/EJE-10-1147. Epub 2011 Apr 6
L.K. Nieman, B.M.K. Biller, J.W. Findling, J. Newell-Price, M.O. Savage, P.M. Stewart et al. The diagnosis of Cushing’s syndrome: an Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 93(5), 1526–1540 (2008). https://doi.org/10.1210/jc.2008-0125. Epub 2008 Mar 11
M. Araujo-Castro, M.A. Sampedro Núñez, M. Marazuela, Autonomous cortisol secretion in adrenal incidentalomas. Endocrine 64(1), 1–13 (2019). https://doi.org/10.1007/s12020-019-01888-y. Epub 2019 Mar 7
A. Ruiz, T. Michalopoulou, A. Megia, S. Näf, I. Simón-Muela, E. Solano et al. Accuracy of new recommendations for adrenal incidentalomas in the evaluation of excessive cortisol secretion and follow-up. Eur. J. Clin. Investig. 49(2), e13048 (2019). https://doi.org/10.1111/eci.13048. Epub 2018 Dec 7
M. Terzolo, A. Pia, G. Reimondo, Subclinical Cushing’s syndrome: definition and management. Clin. Endocrinol. 76(1), 12–18 (2012). https://doi.org/10.1111/j.1365-2265.2011.04253.x
R. Rossi, L. Tauchmanova, A. Luciano, M. Di Martino, C. Battista, L. Del Viscovo et al. Subclinical Cushing’s syndrome in patients with adrenal incidentaloma: clinical and biochemical features. J. Clin. Endocrinol. Metab. 85(4), 1440–1448 (2000)
M. Terzolo, A. Pia, A. Ali, G. Osella, G. Reimondo, S. Bovio et al. Adrenal incidentaloma: a new cause of the metabolic syndrome? J. Clin. Endocrinol. Metab. 87(3), 998–1003 (2002)
G. Di Dalmazi, V. Vicennati, E. Rinaldi, A.M. Morselli-Labate, E. Giampalma, C. Mosconi et al. Progressively increased patterns of subclinical cortisol hypersecretion in adrenal incidentalomas differently predict major metabolic and cardiovascular outcomes: a large cross-sectional study. Eur. J. Endocrinol. 166(4), 669–677 (2012). https://doi.org/10.1530/EJE-11-1039. Epub 2012 Jan 20
M. Debono, M. Bradburn, M. Bull, B. Harrison, R.J. Ross, J. Newell-Price, Cortisol as a marker for increased mortality in patients with incidental adrenocortical adenomas. J. Clin. Endocrinol. Metab. 99(12), 4462–4470 (2014). https://doi.org/10.1210/jc.2014-3007
I.I. Androulakis, G.A. Kaltsas, G.E. Kollias, A.C. Markou, A.K. Gouli, D.A. Thomas et al. Patients with apparently non-functioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J. Clin. Endocrinol. Metab. 99(8), 2754–2762 (2014). https://doi.org/10.1210/jc.2013-4064. Epub 2014 Apr 8
I. Chiodini, Clinical review: diagnosis and treatment of subclinical hypercortisolism. J. Clin. Endocrinol. Metab. 96(5), 1223–1236 (2011). https://doi.org/10.1210/jc.2010-2722. Epub 2011 Mar 2
I. Chiodini, V. Morelli, B. Masserini, A.S. Salcuni, C. Eller-Vainicher, R. Viti et al. Bone mineral density, prevalence of vertebral fractures, and bone quality in patients with adrenal incidentalomas with and without subclinical hypercortisolism: an Italian multicenter study. J. Clin. Endocrinol. Metab. 94(9), 3207–3214 (2009). https://doi.org/10.1210/jc.2009-0468. Epub 2009 Jun 23
M. Peppa, E. Boutati, C. Koliaki, N. Papaefstathiou, E. Garoflos, T. Economopoulos et al. Insulin resistance and metabolic syndrome in patients with non-functioning adrenal incidentalomas: A cause-effect relationship? Metabolism 59(10), 1435–1441 (2010). https://doi.org/10.1016/j.metabol.2010.01.007. Epub 2010 Feb 13
H. Yilmaz, N.B. Tütüncü, M. Şahin, Two-year follow-up of thirty-two non-functional benign adrenal incidentalomas. J. Endocrinol. Investig. 32(11), 913–916 (2009). https://doi.org/10.3275/6431. Epub2009 Jul 14
B. Masserini, V. Morelli, S. Bergamaschi, F. Ermetici, C. Eller-Vainicher, A.M. Barbieri et al. The limited role of midnight salivary cortisol levels in the diagnosis of subclinical hypercortisolism in patients with adrenal incidentaloma. Eur. J. Endocrinol. 160(1), 87–92 (2009). https://doi.org/10.1530/EJE-08-0485. Epub 2008 Oct 3
A. Tanabe, M. Naruse, T. Nishikawa, T. Yoshimoto, T. Shimizu, T. Seki et al. Autonomy of cortisol secretion in clinically silent adrenal incidentaloma. Horm. Metab. Res. 33(7), 444–450 (2001)
A.S. Salcuni, V. Morelli, C.E. Vainicher, S. Palmieri, E. Cairoli, A. Spada et al. Adrenalectomy reduces the risk of vertebral fractures in patients with monolateral adrenal incidentalomas and subclinical hypercortisolism. Eur. J. Endocrinol. 174(3), 261–269 (2016). https://doi.org/10.1530/EJE-15-0977. Epub 2015 Dec 2
V. Morelli, B. Masserini, A.S. Salcuni, C. Eller-Vainicher, C. Savoca, R. Viti et al. Subclinical hypercortisolism: correlation between biochemical diagnostic criteria and clinical aspects. Clin. Endocrinol. 73(2), 161–166 (2010). https://doi.org/10.1111/j.1365-2265.2010.03794.x. Epub 2010 Feb 23
Association American Diabetes., Updates to the standards of medical care in diabetes-2018. Diabetes Care. 41(9), 2045–2047 (2018). https://doi.org/10.2337/dc18-su09
National Cholesterol Education Program (NCEP), Third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report. Circulation. 106(25), 3143–3421 (2002).
B. Bulow, S. Jansson, C. Juhlin, L. Steen, M. Thoren, H. Wahrenberg et al. Adrenal incidentaloma - follow-up results from a Swedish prospective study. Eur. J. Endocrinol. 154(3), 419–423 (2006)
R. Libe, C. Dall’Asta, L. Barbetta, A. Baccarelli, P. Beck-Peccoz, B. Ambrosi, Long-term follow-up study of patients with adrenal incidentalomas. Eur. J. Endocrinol. 147(4), 489–494 (2002)
L. Barzon, N. Sonino, F. Fallo, G. Palù, M. Boscaro, Prevalence and natural history of adrenal incidentalomas. Eur. J. Endocrinol. 149(4), 273–285 (2003)
J.W. Dobbie, Adrenocortical nodular hyperplasia: the ageing adrenal. J. Pathol. 99(1), 1–18 (1969)
L. Papanastasiou, K. Alexandraki, I.I. Androulakis, S. Fountoulakis, T. Kounadi, A. Markou et al. Concomitant alterations of metabolic parameters, cardiovascular risk factors and altered cortisol secretion in patients with adrenal incidentalomas during prolonged follow-up. Clin. Endocrinol. 86(4), 488–498 (2017). https://doi.org/10.1111/cen.13294. Epub 2017 Jan 25
J.M. Baena Díez, J.L. del Val García, J.T. Pelegrina, J.L. Martínez Martínez, R.M. Peñacoba, I.G. Tejón et al. Epidemiología de las enfermedades cardiovasculares y factores de riesgo en atención primaria. Rev. Esp. Cardiol. 58, 367–373 (2005). https://doi.org/10.1157/13073893. Vol. 58 Núm.04
J.A. Whitworth, G.J. Mangos, J.J. Kelly, Cushing, cortisol, and cardiovascular disease. Hypertension 36(5), 912–916 (2000)
A.M. Isidori, C. Graziadio, R.M. Paragliola, A. Cozzolino, A.G. Ambrogio, A. Colao et al. The hypertension of Cushing’s syndrome: controversies in the pathophysiology and focus on cardiovascular complications. J. Hypertens. 33(1), 44–60 (2015). https://doi.org/10.1097/HJH.0000000000000415
D. Lopez, M.A. Luque-Fernandez, A. Steele, G.K. Adler, A. Turchin, A. Vaidya, “Nonfunctional” adrenal Tumors and the risk for incident diabetes and cardiovascular outcomes: a cohort study. Ann. Intern Med. 165(8), 533–542 (2016). https://doi.org/10.7326/M16-0547. Epub 2016 Aug 2
G. Mazziotti, C. Gazzaruso, A. Giustina, Diabetes in Cushing syndrome: basic and clinical aspects. Trends Endocrinol. Metab. 22(12), 499–506 (2011). https://doi.org/10.1016/j.tem.2011.09.001. Epub 2011 Oct 11
G.I. Sydney, K.J. Ioakim, S.A. Paschou, Insulin resistance and adrenal incidentalomas: a bidirectional relationship. Maturitas 121, 1–6 (2019). https://doi.org/10.1016/j.maturitas.2018.12.002. Epub 2018 Dec 5
A. Belfiore, F. Frasca, G. Pandini, L. Sciacca, R. Vigneri, Insulin receptor isoforms and insulin receptor/insulin-like growth factor receptor hybrids in physiology and disease. Endocr. Rev. 30(6), 586–623 (2009). https://doi.org/10.1210/er.2008-0047. Epub 2009 Sep 14
F. Peruzzi, M. Prisco, M. Dews, P. Salomoni, E. Grassilli, G. Romano et al. Multiple signaling pathways of the insulin-like growth factor 1 receptor in protection from apoptosis. Mol. Cell Biol. 19(10), 7203–7215 (1999)
E. Nyman, G. Cedersund, P. Strålfors, Insulin signaling—mathematical modeling comes of age. Trends Endocrinol. Metab. 23(3), 107–115 (2012). https://doi.org/10.1016/j.tem.2011.12.007. Epub 2012 Jan 28
D. Ish-Shalom, G. Tzivion, C.T. Christoffersen, B. Ursø, P. De Meyts, D. Naor, Mitogenic potential of insulin on lymphoma cells lacking IGF‐1 receptor. Ann. N Y Acad. Sci. 766, 409–415 (1995)
G. Di Dalmazi, V. Vicennati, S. Garelli, E. Casadio, E. Rinaldi, E. Giampalma et al. Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing’s syndrome: a 15-year retrospective study. Lancet Diabetes Endocrinol. 2(5), 396–405 (2014). https://doi.org/10.1016/S2213-8587(13)70211-0. Epub 2014 Jan 29
L.F. Starker, J.W. Kunstman, T. Carling, Subclinical Cushing syndrome: a review. Surg. Clin. N. Am. 94(3), 657–668 (2014). https://doi.org/10.1016/j.suc.2014.02.008. Epub 2014 Apr 24
S. Tsagarakis, D. Vassiliadi, N. Thalassinos, Endogenous subclinical hypercortisolism: diagnostic uncertainties and clinical implications. J. Endocrinol. Investig. 29(5), 471–482 (2006)
S. Kidambi, H. Raff, J.W. Findling, Limitations of nocturnal salivary cortisol and urine free cortisol in the diagnosis of mild Cushing’s syndrome. Eur. J. Endocrinol. 157(6), 725–731 (2007)
S. Yener, H. Yilmaz, T. Demir, M. Secil, A. Comlekci, DHEAS for the prediction of subclinical Cushing’s syndrome: perplexing or advantageous? Endocrine 48(2), 669–676 (2015). https://doi.org/10.1007/s12020-014-0387-7. Epub 2014 Aug 22
G. Osella, M. Terzolo, G. Borretta, G. Magro, A. Ali, A. Piovesan et al. Endocrine evaluation of incidentally discovered adrenal masses (incidentalomas). J. Clin. Endocrinol. Metab. 79(6), 1532–1539 (1994)
Z. Bencsik, I. Szabolcs, Z. Kovács, A. Ferencz, A. Vörös, I. Kaszás et al. Low dehydroepiandrosterone sulfate (DHEA-S) level is not a good predictor of hormonal activity in nonselected patients with incidentally detected adrenal tumors. J. Clin. Endocrinol. Metab. 81(5), 1726–1729 (1996)
I. Ilias, A. Sahdev, R.H. Reznek, A.B. Grossman, K. Pacak, The optimal imaging of adrenal tumours: a comparison of different methods. Endocr. Relat. Cancer 14(3), 587–599 (2007)
S. Yener, S. Ertilav, M. Secil, B. Akinci, T. Demir, L. Kebapcilar et al. Increased risk of unfavorable metabolic outcome during short-term follow-up in subjects with non-functioning adrenal adenomas. Med. Princ. Pract. 21(5), 429–434 (2012). https://doi.org/10.1159/000336589. Epub 2012 Mar 2
V. Morelli, G. Reimondo, R. Giordano, S. Della Casa, C. Policola, S. Palmieri et al. Long-term follow-up in adrenal incidentalomas: an Italian multicenter study. J. Clin. Endocrinol. Metab. 99(3), 827–834 (2014). https://doi.org/10.1210/jc.2013-3527. Epub 2014 Jan 1
L. Barzon, C. Scaroni, N. Sonino, F. Fallo, A. Paoletta, M. Boscaro, Risk factors and long-term follow-up of adrenal incidentalomas. J. Clin. Endocrinol. Metab. 84(2), 520–526 (1999)
L. Barzon, F. Fallo, N. Sonino, M. Boscaro, Development of overt Cushing’s syndrome in patients with adrenal incidentaloma. Eur. J. Endocrinol. 146(1), 61–66 (2002)
V. Morelli et al. Role of glucocorticoid receptor polymorphism in adrenal incidentalomas. Eur. J. Clin. Investig. 40(9), 803–811 (2010). https://doi.org/10.1111/j.1365-2362.2010.02330.x
V. Morelli et al. Cardiovascular events in patients with mild autonomous cortisol secretion: analysis with artificial neural networks. Eur. J. Endocrinol. 177(1), 73–83 (2017). https://doi.org/10.1530/EJE-17-0047
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Araujo-Castro, M., Robles Lázaro, C., Parra Ramírez, P. et al. Cardiometabolic profile of non-functioning and autonomous cortisol-secreting adrenal incidentalomas. Is the cardiometabolic risk similar or are there differences?. Endocrine 66, 650–659 (2019). https://doi.org/10.1007/s12020-019-02066-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-019-02066-w