Abstract
Background
The burden of seasonal influenza in conflict counties is exacerbated due to limited resource and collapse of health system. During 2018 /2019 season, two-fold increase in the incidence of influenza was reported in Yemen with 22% case fatality of severe acute respiratory infection (SARI). The aims are to analyze the influenza circulating viruses, positivity rate and risk factors for hospitalizing influenza associated-SARI.
Methodology
We used a retrospective analytical study based on surveillance data. All reported patients during 2018/2019 season, fulfilling the WHO cases definition for SARI or influenza like illness (ILI), and had laboratory result from the National Laboratory were included. Influenza positivity rate was calculated, all SARI and ILI patients with positive influenza were included for further analysis by univariate and multivariate binary logistic regression. Crude and adjusted Odds ratio (AOR), 95% confidence interval and P-value < 0.05 were used for statistically significant.
Results
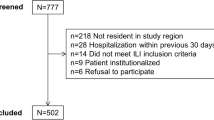
Out of 2186 patients enrolled, 768 patients were tested for influenza viruses,: 19% were children < 15 years, 15% were ≥ 65 years, 69% males and 18% had co-morbidity with chronic diseases. Patients with SARI were 37% and 63% were ILI patients. Influenza viruses were detected in 411 (53.5%), 68% were influenza A subtype (H1N1)pdm09, 27% influenza B and 5% was influenza A not subtyped. The influenza positivity was significantly higher in SARI compared to ILI for patients < 15 years (95% vs, 66%, p < 0.001), and patients ≥ 65 years (83% vs. 56%, p < 0.002), respectively. The highest positivity for influenza type A and B reached 44% and 33% for patients ≥ 65 years and < 15 years, respectively. The risk factors for influenza-associated SARI in multivariate analysis included age < 5 [AOR 2.8] and ≥ 65 years old [AOR 3.1] compared to age 5– < 25 years, diabetes [AOR 4.7], heart diseases [AOR 3.1] and chronic respiratory diseases [AOR 5.0].
Conclusion
The influenza positivity during 2018/2019 winter season was high in Yemen and varied by age distribution. Influenza subtype A (H1N1) pdm09 was the predominant and co circulated with influenza B. An influenza vaccination program for the risk group is necessary. Strengthening lab capacity to detect respiratory pathogens and further prospective study for more comprehensive picture are recommended.
Similar content being viewed by others
Background
Influenza is a respiratory diseases caused by influenza viruses. Type A and B are responsible for 3 to 5 million cases of severe acute respiratory infection (SARI) and 290,000 to 650,000 deaths per year [1]. The severity of influenza viruses is mainly due to exacerbations of some underlying conditions or due to bacterial co-infection and secondary infection that synergize influenza viruses and leading to severe complication, e.g. respiratory distress syndrome (ARDS), respiratory failure and death [2,25, 33,34,35]. As well as, they were within the risk group to whom WHO recommended influenza vaccination [17].
The risk of chronic renal disease is certainly the subject of a confounding effect due to the statistical association with the diabetes and heart disease.
In contest to result of study conducted in Morocco, males were found to be not associated with hospitalization of influenza associated-SARI. This might be due to equal proportion of patients according to sex in our study compared to the over-recruitment of women in that study.
There are some limitations in this study. It is based on secondary data collected from ten governorates patients co-morbidities included only the most common chronic disease in Yemen. The risk of other co morbidities such as HIV, malnourished people and pregnancy were not studied because either this information was not available in the data or the low prevalence such as HIV. Furthermore, the results for influenza B subtype and other respiratory viruses such as Respiratory Syncytial Virus were not available due to the shortage of laboratory kits. As well as bacterial etiology such as Streptococcus pneumoniae, Haemophilus influenzae, and Staphylococcus aureus that contributed in hospitalization of SARI [2] were not available.
Nevertheless, the current study provides information about influenza positivity and risk factors for hospitalization of influenza associated SARI in Yemen, particularly in cold climate governorates. It could help public health authorities to introduce influenza vaccine for people at high risk particular under 5 years and elderly people, diabetics, patients with cardiac diseases and respiratory diseases.
Conclusion
The positivity rate for influenza during 2018/2019 season was high in cold climate governorates of Yemen. The positivity rate for influenza viruses among patients with SARI and ILI varied according to age distribution. Influenza Type A virus and subtype AH1N1 were predominant circulating viruses and co circulated with influenza type B. Influenza type A virus was higher among elderly SARI patients, while influenza type B virus was higher among < 15 years old. Extremes age < 5 and ≥ 65 years, underlying conditions including diabetes, cardiac diseases, chronic respiratory diseases were the identified risk factors for hospitalization of influenza associated SARI. Introducing influenza vaccine for these risk groups is highly recommended. A prospective study to assess co morbidities as risk factors for influenza associated SARI should be conducted. Strengthening laboratory capacity to detect other respiratory pathogens is highly recommended.
Availability of data and materials
All relevant data are presented in this paper; and more information can be provided upon reasonable request from the correspondence author.
Abbreviations
- AOR:
-
Adjusted Odds Ratio
- CI:
-
Confidence Interval
- eDEWS:
-
Electronic disease early warning system
- ILI:
-
Influenza like illness
- NCPH:
-
National Central public Health Laboratory
- OR:
-
Odds Ratio
- RT-PCR:
-
Reverse transcription polymerase Chain Reaction
- SARI:
-
Severe acute respiratory infection
- WHO:
-
World health Organization
References
Influenza (Seasonal). https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal).
Gordon A, Reingold A. The burden of influenza: a complex problem. Curr Epidemiol Rep. 2018;5(1):1–9.
Jia L, **e J, Zhao J, Cao D, Liang Y, Hou X, Wang L, Li Z. Mechanisms of severe mortality-associated bacterial co-infections following influenza virus infection. Front Cell Infect Microbiol. 2017;7:338.
Manohar P, Loh B, Nachimuthu R, Hua X, Welburn SC, Leptihn S. Secondary bacterial infections in patients with viral pneumonia. Front Med. 2020;7:420.
Bellos A, Mulholland K, O’Brien KL, Qazi SA, Gayer M, Checchi F. The burden of acute respiratory infections in crisis-affected populations: a systematic review. Confl Heal. 2010;4:3.
Jaadan BM, Al-Shamahy HA, Al-Harazi AH, Al-Ademi DAA: Detection of Influenza Viruses among Hospitalized Cases Suffering from Severe Acute Respiratory Illness (Sari) in Sana’a City, Yemen. Univ J Pharm Res. 2019.
Al Amad MA, Al Mahaqri AA, Al Serouri AA, Khader YS. Severe acute respiratory infections with influenza and noninfluenza respiratory viruses: Yemen, 2011–2016. Inquiry. 2019;56:46958019850731.
Thabet AA, Al-Kohani A, Shadoul A, Al-Mahaqri A, Bin Yahya M, Saleh AH, Al-Adeemy D, Khan W, Malik M. Characteristics of severe acute respiratory infectionassociated hospitalization in Yemen, 2014/15. East Mediterr Health J. 2016;22(7):440–4.
Mayad M, Alyusfi R, Assabri A, Khader Y. An electronic disease early warning system in Sana’a governorate, Yemen: evaluation study. JMIR Public Health Surveill. 2019;5(4):e14295.
Dureab F, Ahmed K, Beiersmann C, Standley CJ, Alwaleedi A, Jahn A. Assessment of electronic disease early warning system for improved disease surveillance and outbreak response in Yemen. BMC Public Health. 2020;20(1):1422.
Dureab F. The usefulness of the electronic Disease Early Warning System (eDEWS) in the humanitarian crisis of Yemen. 2020.
Luyt CE, Rice TW. Co-infection in severe influenza: a new epidemiology? Intensive Care Med. 2017;43(1):107–9.
Sf MSF. Health system in Yemen close to collapse. Bull World Health Organ. 2015;93:670–1.
Zawiah M, Al-Ashwal FY, Saeed RM, Kubas M, Saeed S, Khan AH, Sulaiman SAS, Abduljabbar R. Assessment of healthcare system capabilities and preparedness in Yemen to confront the novel coronavirus 2019 (COVID-19) outbreak: a perspective of healthcare workers. Front Public Health. 2020;8(419):419.
El Bcheraoui C, Jumaan AO, Collison ML, Daoud F, Mokdad AH. Health in Yemen: losing ground in war time. Glob Health. 2018;14(1):42.
Al Amad MA AMA: Influenza epidemic with high mortality during the winter months in Yemen, 2018–2019. Oman Med J. 2020, 35(1).
World Health Organization: WHO Strategic Advisory Group of Experts on immunization: request for nominations. Weekly Epidemiological Record Relevé épidémiologique hebdomadaire. 2009, 84(15):131–132.
Global epidemiological surveillance standards for influenza.
Fitzner J, Qasmieh S, Mounts AW, Alexander B, Besselaar T, Briand S, Brown C, Clark S, Dueger E, Gross D, et al. Revision of clinical case definitions: influenza-like illness and severe acute respiratory infection. Bull World Health Organ. 2018;96(2):122–8.
Elhakim M, Hafiz Rasooly M, Fahim M, Sheikh Ali S, Haddad N, Cherkaoui I, Hjaija D, Nadeem S, Assiri A, Aljifri A, et al. Epidemiology of severe cases of influenza and other acute respiratory infections in the Eastern Mediterranean Region, July 2016 to June 2018. J Infect Public Health. 2020;13(3):423–9.
Malik M, Mahjour J, Khan W, Alwan A. Influenza in the Eastern Mediterranean Region: identifying the unknowns for detection and control of epidemic and pandemic threats. EMHJ. 2016;22(7):428–9.
Khan W, El Rifay AS, Malik M, Kayali G. Influenza research in the Eastern Mediterranean region: a review. Oman Med J. 2017;32(5):359–64.
Caini S, El-Guerche Seblain C, Ciblak MA, Paget J. Epidemiology of seasonal influenza in the Middle East and North Africa regions, 2010–2016: circulating influenza A and B viruses and spatial timing of epidemics. Influenza Other Respir Viruses. 2018;12(3):344–52.
Hammond A, Hundal K, Laurenson-Schafer H, Cozza V, Maharjan B, Fitzner J, Samaan M, Vandemaele K, Zhang W. Review of the 2018–2019 influenza season in the northern hemisphere. Wkly Epidemiol Rec. 2019;94(32):345–65.
Ezzine H, Cherkaoui I, Rguig A, Oumzil H, Mrabet M, Bimouhen A, Falaki FE, Regragui Z, Tarhda Z, Youbi M, et al. Influenza epidemiology and risk factors for severe acute respiratory infection in Morocco during the 2016/2017 and 2017/2018 seasons. Pan Afr Med J. 2020;36:159.
Hammond A, Laurenson-Schafer H, Marsland M, Besselaar T, Fitzner J, Vandemaele K, Zhang W. Review of the 2017–2018 influenza season in the northern hemisphere/Bilan de la saison grippale 2017–2018 dans l’hemisphere Nord. Wkly Epidemiol Rec. 2018;93(34):429–45.
Refaey S, Amin M, Labib M, Kandeel A. Influenza virus positivity and circulating subtypes among cases of influenza-like illness and severe acute respiratory infection, Egypt, 2012–2015. EMHJ. 2016;22(7):523–32.
Cheng W, Yu Z, Liu S, Zhang X, Wang X, Cai J, Ling F, Chen E. Comparison of influenza epidemiological and virological characteristics between outpatients and inpatients in Zhejiang Province, China, March 2011–June 2015. Int J Environ Res Public Health. 2017;14(2):217.
Caini S, Huang QS, Ciblak MA, Kusznierz G, Owen R, Wangchuk S, Henriques CM, Njouom R, Fasce RA, Yu H, et al. Epidemiological and virological characteristics of influenza B: results of the Global Influenza B Study. Influenza other Resp Viruses. 2015;9(Suppl 1):3–12.
Oh YN, Kim S, Choi YB, Woo SI, Hahn YS, Lee JK. Clinical similarities between influenza A and B in children: a single-center study, 2017/18 season, Korea. BMC Pediatr. 2019;19(1):472.
Ahmed AKT, Najeeb MM, Abdulhakeem A-K, Mohammed J. Epidemiology of fatal cases associated with pandemic influenza reported in Yemen. Nat Sci. 2012, 2012.
Al Amad M, Al Mahqri A, Al Serouri A. Severe acute respiratory infections associated with influenza and non-influenza viruses-Yemen, 2011–2014. Int J Infect Dis. 2016;45:291.
Tempia S, Walaza S, Moyes J, Cohen AL, von Mollendorf C, Treurnicht FK, Venter M, Pretorius M, Hellferscee O, Mtshali S, et al. Risk factors for influenza-associated severe acute respiratory illness hospitalization in South Africa, 2012–2015. Open Forum Infect Dis. 2017;4(1):ofw262.
Zhang Y, Muscatello DJ, Wang Q, Yang P, Pan Y, Huo D, Liu Z, Zhao X, Tang Y, Li C, et al. Hospitalizations for influenza-associated severe acute respiratory infection, Bei**g, China, 2014–2016. Emerg Infect Dis. 2018;24(11):2098–102.
Cummings MJ, Bakamutumaho B, Kayiwa J, Byaruhanga T, Owor N, Namagambo B, Wolf A, Wamala JF, Morse SS, Lutwama JJ, et al. Epidemiologic and spatiotemporal characterization of influenza and severe acute respiratory infection in Uganda, 2010–2015. Ann Am Thorac Soc. 2016;13(12):2159–68.
Acknowledgements
Not applicable.
Funding
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Author information
Authors and Affiliations
Contributions
MA and KA contributed to conception and design of the study. MA performed the statistical analysis, wrote the draft manuscript. KA organized the data, involved in statistical analysis. Both authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
As these data were secondary data, collected by surveillance staff, obtained from the influenza surveillance system and the use of such data is part of the national surveillance activities, the study did not require formal ethical review. An official permission to perform this study was obtained from Ministry of Public Health and Population. I confirm that all methods were performed in accordance with the relevant guidelines and regulations in the county. The study did not involve experiments on human subject or human participants under the age of 18 years. No human studies are presented in this manuscript.
Consent for publication
This study does not include any identifiable human images or data and thus does not require a consent to publish.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Al Amad, M., Almoayed, K. Influenza circulating viruses, positivity rate and risk factors for influenza associated severe acute respiratory infection during 2018/2019 winter season, Yemen. BMC Infect Dis 22, 111 (2022). https://doi.org/10.1186/s12879-022-07090-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-022-07090-2