Abstract
Study design
Retrospective Case Series.
Objectives
Describe the inpatient rehabilitation outcomes of four patients with COVID-19 tractopathy.
Setting
Olmsted County, Minnesota, United States of America.
Methods
Retrospective review of medical records was performed to collect patient data.
Results
Four individuals (n = 4, 3 men and 1 woman, mean age 58.25 years [range 56–61]) completed inpatient rehabilitation during the COVID-19 pandemic. All presented after COVID-19 infection and were admitted to acute care with progressive paraparesis. None were able to ambulate on admission to acute care. All received extensive evaluations which were largely negative except for mildly elevated CSF protein and MRI findings of longitudinally extensive T2 hyperintensity signal changes in the lateral (n = 3) and dorsal (n = 1) columns. All patients experienced incomplete spastic paraparesis. All patients experienced neurogenic bowel dysfunction; a majority experienced neuropathic pain (n = 3); half experienced impaired proprioception (n = 2); and a minority experienced neurogenic bladder dysfunction (n = 1). Between rehabilitation admission and discharge, the median improvement in lower extremity motor score was 5 (0–28). All patients were discharged home, but only one was a functional ambulator at time of discharge.
Conclusion
While the underlying mechanism is yet to be elucidated, in rare cases a COVID-19 infection can lead to a tractopathy, presenting as weakness, sensory deficits, spasticity, neuropathic pain, and neurogenic bladder/bowel. Patients with COVID-19 tractopathy would benefit from inpatient rehabilitation to enhance their functional mobility and independence.
Similar content being viewed by others
Introduction
The World Health Organization declared the SARS-CoV-2 (COVID-19) pandemic on March 11, 2020, and since then, there have been greater than 615 million cases reported worldwide. Although predominantly a respiratory pathogen, infection with the COVID-19 virus can lead to multisystem involvement. A number of neurological manifestations have been previously described, such as post-COVID transverse myelitis, spinal cord infarctions, and Guillain-Barre Syndrome [1,2,3,4,5]. These manifestations may be due to direct effects of the virus on the nervous system; however, it may instead be due to post-infectious immune-mediated effects.
COVID-19 tractopathy is a new diagnosis associated with a recent COVID-19 viral infection and injury to the lateral and dorsal tracts that lie within the spinal cord. Isolated tract pathology has rarely been reported. This retrospective case series describes the inpatient rehabilitation outcomes of four patients with COVID-19 tractopathy at an academic medical center.
Methods
Retrospective review of medical records was performed to collect patient data.
Results
Four individuals (n = 4, 3 men and 1 woman, mean age 58.25 years [range 56–61]) completed inpatient rehabilitation (length of stay [LOS]: mean 23.5 days [range 9–43]) during the COVID-19 pandemic. All presented after COVID-19 infection and were admitted to acute care (LOS: mean 18.25 days [range 10–26]) with progressive paraparesis. None were able to ambulate on admission to acute care. All received extensive evaluations which were largely negative (see Supplementary Table 1) except for mildly elevated CSF protein and MRI findings of longitudinally extensive T2 hyperintensity signal changes in the lateral (n = 3) and dorsal (n = 1) columns (see Fig. 1). The patients received intravenous (IV) methylprednisolone (n = 4), plasmapheresis (n = 4), oral prednisone (n = 4), rituximab infusion (n = 2), and intravenous immunoglobulin (IVIG) (n = 1) during acute care, with minimal improvement at that time. Each spinal cord injury was classified using ASIA/ISCoS International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI) [6]. All patients experienced incomplete spastic paraparesis and required medical management for spasticity with either oral baclofen (n = 3) or oral carbamazepine (n = 1). All patients experienced neurogenic bowel dysfunction necessitating the use of bowel medications as needed; a majority experienced neuropathic pain (n = 3); half experienced impaired proprioception (n = 2); and a minority experienced neurogenic bladder dysfunction requiring intermittent catheterization (n = 1). Between rehabilitation admission and discharge, the median improvement in lower extremity motor score (LEMS) was 5 (0–28). All patients were discharged home, but only one, with intact proprioception, was a functional ambulator at time of discharge. Additional details regarding each case are presented in Tables 1–3 [6].
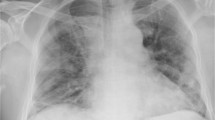
A Patient 1: MRI Thoracic Spine T2 hyperintensity in the dorsal columns of the spinal cord at T10 level. B Patient 2: MRI Thoracic Spine T2 hyperintensity in the lateral columns of the spinal cord at T10 level. C Patient 3: MRI Thoracic Spine T2 hyperintensity in the lateral columns of the spinal cord at T9 level. D Patient 4: MRI Thoracic Spine T2 hyperintensity in the lateral columns of the spinal cord at C2 level.
Discussion
The aim of this retrospective case series was to describe the clinical characteristics and inpatient rehabilitation outcomes of the COVID-19 tractopathy cases seen at our academic medical center. At this time, a variety of COVID-19 related spinal cord manifestations have been described [7,8,9,10]. In regards to anatomic and radiologic features of COVID-related myelopathy, a propensity for central lesions of the spinal cord, mainly affecting the grey matter, has been most commonly reported in the literature [9, 10]. This pattern is typical of viral myelitis. The reports of a relationship between COVID-19 and isolated spinal cord tractopathy, however, has been limited.
Apart from our case series, we found one other study from a single academic institution which reported five cases with tract-specific involvement of the dorsal and lateral columns [11]. The mechanism for isolated involvement of the lateral and dorsal columns is unclear, but the authors speculated a disturbance in the methylation pathway given its implication in a similar anatomic pattern of involvement seen in subacute combined degeneration. During the pandemic, many individuals prophylactically supplemented with oral zinc in hopes to strengthen their immune system against the circulating virus; however, high supplemental zinc may lead to copper deficiency which in turn can cause subacute combined degeneration. Among the four cases at our institution, serum copper levels were normal (see Supplementary Table 1). The lesions occurred in the cervical and/or thoracic spinal cord segments and all fulfilled criteria as longitudinally extensive, consistent with recent case reports [8]. Motor, sensory, and bowel and bladder symptoms predominated the clinical picture of the four patients treated at our institution. All patients had variable but beneficial responses to immunosuppressive therapy and were ultimately discharged from inpatient rehabilitation to home. Notably, patients #1 and #3 in our case series spontaneously improved and regained walking ability over the course of six months and one year, respectively, after all immunotherapy was stopped. At one year follow-up, patient #4 regained walking ability with a cane and bilateral ankle-foot-orthoses.
This retrospective case series attempted to provide a complete description of each of these four cases yet there are still limitations. Although each patient had a confirmed COVID-19 infection, the time course between COVID-19 infection onset and myelopathic symptoms was not reported and unable to be obtained in several cases. This may be due to several reasons, including recall bias, previous attribution of these symptoms to another diagnosis, and not reporting the date of a positive COVID-19 antigen test.
While the underlying mechanism has yet to be elucidated, in rare cases COVID-19 infection can be associated with a tractopathy, presenting as weakness, sensory deficits, spasticity, neuropathic pain, and neurogenic bladder/bowel. Patients with COVID-19 tractopathy demonstrated improvements in LEMS, mobility, and self-care during inpatient rehabilitation; all were discharged home. These patients would benefit from inpatient rehabilitation to enhance their functional mobility and independence.
Data availability
Data for this paper are available within the published article and Supplementary files.
References
Caress JB, Castoro RJ, Simmons Z, Scelsa SN, Lewis RA, Ahlawat A, et al. COVID-19-associated Guillain-Barré syndrome: the early pandemic experience. Muscle Nerve. 2020;62:485–91.
Chow CCN, Magnussen J, Ip J, Su Y. Acute transverse myelitis in COVID-19 infection. BMJ Case Rep. 2020;13:e236720.
Roy D, Ghosh R, Dubey S, Dubey MJ, Benito-León J, Kanti Ray B. Neurological and neuropsychiatric impacts of COVID-19 pandemic. Can J Neurol Sci. 2021;48:9–24.
Eissa M, Abdelhady M, Alqatami H, Salem K, Own A, El Beltagi AH. Spinal cord infarction in a 41-year-old male patient with COVID-19. Neuroradiol J. 2021;34:245–8.
Kahan J, Gibson CJ, Strauss SB, Bronstein M, Winchell RJ, Barie PS, et al. Cervical spinal cord infarction associated with coronavirus infectious disease (COVID)-19. J Clin Neurosci. 2021;87:89–91.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A, et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med. 2011;34:535–46.
Abrams RMC, Safavi F, Tuhrim S, Navis A, Steinberger J, Shin SC. MRI negative myelopathy post mild SARS-CoV-2 infection: vasculopathy or inflammatory myelitis? J Neurovirol. 2021;27:650–5.
Artemiadis A, Liampas A, Hadjigeorgiou L, Zis P. Myelopathy associated with SARS-COV-2 infection. A systematic review. Neurol Res. 2021;43:633–41.
Barman A, Sahoo J, Viswanath A, Roy SS, Swarnakar R, Bhattacharjee S. Clinical features, laboratory, and radiological findings of patients with acute inflammatory myelopathy after COVID-19 infection: a narrative review. Am J Phys Med Rehabil. 2021;100:919–39.
Canavero I, Valentino F, Colombo E, Franciotta D, Ferrandi D, Mussa M, et al. Acute myelopathies associated to SARS-CoV-2 infection: viral or immune-mediated damage? Travel Med Infect Dis. 2021;40:102000.
Huang HY, Shah LM, McNally JS, Sant T, Hutchins TA, Goldstein ED, et al. COVID-19-associated myelitis involving the dorsal and lateral white matter tracts: a case series and review of the literature. AJNR Am J Neuroradiol. 2021;42:1912–7.
Author information
Authors and Affiliations
Contributions
The six previously listed authors of this manuscript (JBM, CTH, KLG, BAS, EPF, RKR) meet the required elements for authorship.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Meiling, J.B., Ha, C.T., Garlanger, K.L. et al. Inpatient rehabilitation outcomes in patients with the new diagnosis of COVID-19 tractopathy: a case series. Spinal Cord Ser Cases 9, 25 (2023). https://doi.org/10.1038/s41394-023-00586-2
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41394-023-00586-2
- Springer Nature Limited