Abstract
Coronavirus disease 2019 (COVID-19) may be associated with a wide range of bacterial and fungal co-infections. Acute invasive fungal sinusitis is an aggressive infection affecting immunocompromised patients and high mortality rate. Here, in this case series, we have reviewed three cases of COVID-19 associated rhino-orbital invasive fungal disease. Patients with COVID-19 associated pneumonia with diabetes mellitus are at an increased risk of develo** invasive pulmonary fungal infections probably due to their reduced immunological competence. Concurrent glucocorticoid therapy probably heightens the risk of mucormycosis. Physicians should be aware of and should have high index of suspicion of possible fungal infection in post COVID-19 patients. Aggressive management both medical and surgical, is required to improve outcomes of secondary invasive fungal infections in patients with COVID-19 infection.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
While the countries combat the second wave of COVID-19, the matter of significant concern that has emerged is post COVID-19 sepsis. India bears the dubious distinction of being the metropolis of both diabetes, as well as mucormycosis. The pre-morbidities along with COVID-19 provide fertile land for the growth of fungal elements in various parts of the body [1, 2].
Worldwide, COVID-19-associated pulmonary aspergillosis has received much attention [3]. While, the Indian epidemiology of invasive fungal infections in the Intensive care unit reveals a hefty burden of invasive mucormycosis [4]. It has emerged as a life-threatening complication of COVID-19 in our country. Although, highly fatal fungal infection occurs typically in individuals with underlying immunocompromised conditions, such as diabetes mellitus, hematologic malignancies, neutropenia, solid organ transplant, primary immunodeficiency, and treatment with immunosuppressants. Certain distinguished characteristics must be kept in mind to promptly suspect the infection, confirm the diagnosis and offer timely therapeutic intervention [5].
In this case series, we review three cases of COVID-19 associated invasive fungal rhino-orbital disease (CAIFR) and also perform a systematic review of the literature to identify cases of COVID-19 associated mucormycosis(CAM) and describe their clinical features, risk factors, diagnostic and therapeutic challenges encountered. COVID-19 associated acute invasive fungal rhino-orbital disease CAIFR) has not been reported with the review of the literature before.
Case 1
A 36-year-old woman with long-standing rheumatoid arthritis on medication with recently diagnosed diabetes mellitus, presented with a history of low-grade fever, non-productive cough, and difficulty in breathing for the last 2 days. At admission, the respiratory rate was 24 breaths/minute, blood pressure 128/86 mmHg, oxygen saturation was 91% on room air and heart rate was 90 beats/minute. She was diagnosed with type 2 diabetes mellitus on hospitalization for the current illness with her glycated hemoglobin (HbA1c) of 13.2 and high levels of random blood glucose. She was started on oxygen via venturi mask, diabetic diet, regular insulin, and basalog injection according to the blood glucose levels.
A nasopharyngeal swab was positive for SARS-CoV-2 by RT–PCR on the day of admission. The patient was transferred to the COVID-19 dedicated ward and was started intravenous Piperacillin-tazobactam, oral antipyretics, antitussive, and multivitamins. Intravenous Methylprednisolone 0.5 mg/kg in two divided doses started per day for a duration. Adequate hydration was maintained via an intravenous route along with temperature and oxygen saturation monitoring.
On day 3 of admission, swelling in the left side of the face was noticed, predominantly on the left periorbital region with ulceration over left side skin over the cheek which was acute in onset, persistent, and progressive associated with diminution of vision of the left eye (Fig. 1a). She underwent Magnetic resonance imaging (MRI) of the nose and paranasal sinuses the next day, which revealed soft tissue density involving the left maxillary and ethmoid sinus with T2 hypointensity. There is diffuse subcutaneous edema with fat stranding involving left buccal space, pre-maxillary space, masticator space, and pre-septal space causing proptosis (Fig. 2a, b and c).
On ophthalmological examination, the unaided visual acuity in the right eye was 6/6 and in the left eye was 6/12. The left eye was proptosed with upper eyelid edema and limitation of extraocular movements in all gazes. The anterior segment revealed chemosis of the conjunctiva and pupillary reactions were normal in both the eyes. The posterior segment examination was normal in both eyes. The examination of the right eye was unremarkable.
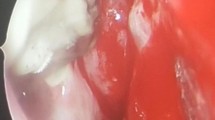
With proper precautions and using personal protective equipment, surgical debridement was done and tissue was sent for histopathological examination which confirmed the diagnosis of invasive fungal disease (Fig. 6). She was subsequently started on liposomal Amphotericin B at 3 mg/kg/day with close monitoring of renal function and serum electrolytes and it was stopped after a cumulative dose of 3600 mg. In between, she recovered from respiratory symptoms and was maintaining oxygen saturation of 98% on ambient air and underwent RT-PCR again after 17 days, was diagnosed COVID-19 negative. There was an improvement in facial swelling, proptosis and the ulcers started to heal by the 21st day of hospital stay, but without any improvement in the visual acuity. She was discharged after due course of antifungal (18 days) on oral medication comprising of oral cefixime, Itraconazole, oral hypoglycaemic drugs, and alkaline nasal douching and is followed on an outpatient department basis (Figs. 3 and 4).
Case 2
A 45-year-old woman presented to the emergency with the chief complaints of confusion, episodes of vomiting, and breathlessness. On general physical examination, she was semi-conscious, febrile to touch, and disoriented, her blood pressure was 104/70 mm Hg and blood glucose was 458 mmol/lit, and strongly positive for urine ketones. She was diagnosed with type 2 diabetes mellitus five years ago and was on irregular medications. Blood sugar monitoring was infrequent. She was diagnosed to have Diabetic ketoacidosis and was admitted to the department of internal medicine. She was started on intravenous crystalloids and insulin infusion with strict blood glucose monitoring. On taking further history after the patient got stable, she also complained of anosmia and dysgeusia. A nasopharyngeal swab was sent for RT–PCR and was tested positive for SARS-CoV-2.
Thereafter, she was shifted to the COVID-19 dedicated Medicine intensive care unit. Chest radiograph showed bilateral diffuse interstitial opacities. The hemoglobin at admission was 11.8 g/dL, serum potassium was 2.3 mmol/l, serum creatinine levels of 2.5 mg/dl, and glycated hemoglobin was 12.4%. She was started on an insulin infusion, potassium chloride, broad-spectrum intravenous antibiotics, and methyl-prednisolone. Supportive care, including oxygen supplementation, thromboprophylaxis for venous thrombosis, and maintenance hemodialysis initiated. Subsequently, on the third day in ICU, she started develo** swelling over the right side of the face and periorbital cellulitis, lid edema, and ulceration. On oral examination, there is an erythema and ulcerative lesion on the right side of the hard palate. The patient underwent nasal endoscopy which revealed blackish discoloration of the uncinate process and middle turbinate.. A nasal swab was non-contributory but a nasal biopsy from the uncinate process revealed broad aseptate hyphae but no rhizoids or root-like structures with global round sporangia filled with spores and carried on a stalk called sporangiophore suggestive of Mucor on Lactophenol Cotton Blue(LCB) mount (Fig. 5a).
a Mucor with broad aseptate hyphae but no rhizoids or root-like structures on LCB staining. b Rhizopus with broad aseptate hyphae and cluster of rhizoids on LCB staining. Both have global round sporangia filled with spores and carried on a stalk called sporangiophore. c Long aseptate, ribbon-like hyphae suggestive of Zygomycosis on KOH test
Furthermore, the patient was started on Liposomal Amphotericin B at 1.7 mg/kg/day after getting a medicine opinion in view of a constant de-arranged renal function test. A contrast-enhanced computed tomography was done which revealed heterogeneous enhancing soft tissue in the right maxillary, ethmoid sinus, and inferior meatus extending through the nasolacrimal duct upwards at the medial canthus involving lacrimal gland sac, extending to adjacent post septal and infra-orbital region. She subsequently was planned for debridement. But, over time her condition deteriorated for which she got intubated on day 7 of admission and was kept on mechanical ventilation because of falling oxygen saturation. Her health status continued to decline despite ongoing treatment. Unfortunately, she developed irreversible shock and expired on the tenth day of her hospital stay.
Case 3
A 62-year man was admitted under ICU for bilateral COVID-19 induced pneumonia with ARDS, with diabetes mellitus, hypertension, and deranged kidney functions developed right eye diminution of vision, periorbital swelling, and restricted eye movements on the fifth day of hospital admission. He received coverage for MRSA, regular insulin, Remdesivir, dexamethasone as per guidelines, and liposomal Amphotericin B was also started. He was intubated on the next day, required ventilatory and ionotropic support. Nasal endoscopy revealed purulent discharge, blackish discoloration of the middle turbinate, posterior part of the inferior turbinate, and the nasal swab was taken for staining and culture.
The patient continued to deteriorate and remained on inotropic support. Due to persistent hypotension, we were unable to carry out any debridement measures. Despite all measures, he died on day seven of this admission.
On follow-up, a swab which was taken from nasal cavity revealed long aseptate, ribbon-like hyphae suggestive of Zygomycosis on KOH test and broad aseptate hyphae and cluster of rhizoids with global round sporangia filled with spores and carried on a stalk called sporangiophore on LCB staining (Fig. 5b and c). Fungal culture confirmed the presence of Zygomycosis.
The clinical picture, CT picture, fungal staining, and culture strongly suggested the diagnosis of orbital cellulitis with cavernous sinus thrombosis due to invasive fungal infection of the nose and paranasal sinuses (Fig. 6).
Review of Literature
We carried a systematic review of the PubMed and Embase databases till 15th February 2021, using the text terms: COVID-19 or SARS-CoV or coronavirus and mucor or rhizopus or aspergillus and invasive mucormycosis. There were 24 citations, eight out of 24 described mucormycosis in association withCOVID-19.
COVID-19 Associated Pulmonary Mucormycosis
The index case was a 55-year-old man with diabetes mellitus, ischaemic cardiomyopathy, and end-stage renal disease. He developed COVID-19 with bilateral lung infiltrates on chest X-ray, lymphopenia on hemogram, and deranged renal function. He was started on a broad-spectrum antibiotic (Meropenem), Dexamethasone, and Amphotericin B at a dose of 3 mg/kg/day till 5gm. The diagnosis of COVID-19 associated pulmonary mucormycosis was made after the identification of Rhizopus in sputum.
Pasero et al. [6] reported a case of a 66-year-old man, who developed COVID-19 associated with ARDS with pulmonary mucormycosis. On investigation, he had lymphopenia and chronic renal failure due to long-term hypertension. He was started on Hydroxychloroquine and Lopinavir-ritonavir as per guidelines in Italy for COVID-19 and broad-spectrum antibiotics (Meropenem and Linezolid) with Liposomal Amphotericin B at 5 mg/kg/day for 20 days for COVID-19 associated pulmonary mucormycosis but, unfortunately, she couldn't survive.
Garg et al. [5] reported a 55-year-old man positive for SARS-CoV-2 by RT-PCR with long-standing uncontrolled diabetes mellitus, hypertension, and ischemic cardiomyopathy. Chest radiograph and CT chest confirmed a thick-walled cavity with intracavitary contents in the right upper lobe. Lactophenol cotton blue (LCB) mount from the sputum culture growth revealed fungal elements suggestive of pulmonary mucormycosis. The patient was treated with liposomal amphotericin B (3 mg/kg) and his symptoms improved, and he was discharged 54 days after hospitalization (cumulative dose of amphotericin B, 5 gm).
Another case report by Placik et al. [7] of a 49 years old male patient, who developed COVID-19 associated with ARDS and was started on Remdesivir, Tocilizumab, and Dexamethasone along with Amphotericin B (for 6 days) and Ceftriaxone. He was diagnosed with pulmonary mucormycosis with bronchopleural fistula and pneumothorax on day 14 after the diagnosis of COVID-19. He died in the ICU 1 week after diagnosis of pulmonary pathologies.
Monte junior et al. [8] reported a 86 year old man, known case of hypertension and COVID-19 associated with ARDS with Malena and loose stools. On blood investigation, the hemoglobin and lymphocytes were on the lower side, and on upper gastrointestinal endoscopy, it revealed large ulcers. He succumbed to death and was diagnosed on post-mortem examination that he had a fungal infection of the gut.
COVID-19 Associated Rhino-Orbital Mucormycosis
Mekkonen et al. [9] reported a 60-year-old man with a history of poorly controlled insulin-dependent diabetes, asthma, hypertension, hyperlipidemia with COVID-19 associated with ARDS. Because of declining oxygen saturation, he was intubated in the intensive care unit and started on remdesivir. The following day, the patient was found to have a prominence of the right eye. Intranasal tissue culture grew Rhizopus species. Based on clinical and radiological evidence a diagnosis of Rhino-orbital mucormycosis was made. The patient was treated with a series of 3 daily retrobulbar injections of liposomal amphotericin B (3.5 mg/dl) to the right orbit. Concurrently, the patient was also started on a 10-day course of dexamethasone 6 mg daily and a single dose of convalescent plasma as a treatment for COVID-19. But, there was no respite and he, unfortunately, expired on hospital day 31 from ARDS due to COVID-19.
Werthman-Ehrenreich et al. [10] reported a 33-year-old Somali female with a past medical history of hypertension and asthma, presented to the emergency department with altered mental status. She has a history of vomiting, cough, and shortness of breath 2 days before. This was also accompanied by left eye ptosis with 1 cm proptosis, a fixed dilated pupil with complete ophthalmoplegia. After proper CT evaluation, nasal swabs were taken and sent for fungal culture and were consistent with Rhino-orbital mucormycosis. Debridement was done under the cover of Vancomycin, piperacillin-tazobactam, and Amphotericin B. In addition, the patient received remdesivir and convalescent plasma. On MRI Brain features of cerebral edema with multiple encapsulated complex fluid collections suspicious for invasive mucormycosis. The patient expired on day 26 of her hospitalization.
A case report by Mehta et al. [11] of a 60-year-old male, who was admitted with a three-day history of severe breathlessness and pyrexia associated with longstanding diabetes mellitus and its complication (peripheral vascular disease). On further investigation (RT-PCR and CT chest) he was diagnosed to have COVID-19 associated ARDS. He was started on intravenous meropenem, oral oseltamivir, methylprednisolone, and insulin adjusted as per a sliding scale. On examination, the right eye was mildly proptotic with extensive areas of edema in the periorbital region with soft tissue necrosis along the medial half of the lids and conjunctival edema. The left eye appeared fixed and had a dilated non-reactive pupil. A nasal biopsy from the middle turbinate revealed broad aseptate filamentous fungal hyphae. The radiological and histopathological examination confirmed the diagnosis of Rhino-orbital mucormycosis. Debridement measures couldn't be done due to persistent hypotension. Despite all measures, the patient expired on day six of this admission.
Discussion
With more than one year since the emergence of COVID-19 in China, it has already claimed more than one million lives worldwide. In the absence of a proven efficient vaccine or definitive antiviral therapy, supportive care plays a vital role in the management of COVID-19. Having said that, there is a high probability that critically ill patients with COVID-19 and diabetes mellitus are at a higher risk of develo** invasive fungal rhinosinusitis as was seen in the above case series.
Immunomodulatory drugs like Glucocorticoids and antiviral agents like Remdesivir are the only drugs found to be beneficial in reducing mortality in hypoxemic patients with COVID-19 but are still under investigation [12,13,14]. Systemic corticosteroids have been shown to decrease mortality in particular subgroups of patients with COVID-19, with the greatest efficacy shown in patients receiving invasive mechanical ventilation [15, 16]. However, treatment with systemic corticosteroids causes suppression of the immune system, thereby predisposing patients to invasive fungal rhinosinusitis.
A cross-sectional study disclosed that 47% of Indians are oblivious of their diabetic status and only a quarter of all patients achieved adequate glycemic control on treatment [1]. The profane association between diabetes and the severity of SARS-CoV-2 infection has been repeatedly established in various studies from across the world [2].
COVID-19 patients with diabetes are at increased risk of develo** severe disease and are also more prone to invasive fungal infections [17]. According to Donnelly et al. prolonged use of corticosteroids at a therapeutic dose of ≥ 0.3 mg/kg for at least three weeks in the past 60 days is considered a risk factor for invasive fungal diseases, and also, it causes de-arranged blood glucose levels in known diabetes patients leading to an altered immunological response to pathogens, enhanced proliferation of moulds and diminished phagocytic capacity of host immune cells [18–20].
In a study by Chen et al. there is a decline in the circulating lymphocyte levels and T cell subtypes which leads to suboptimal cell-mediated immunity in patients of COVID-19 [14]. This was supported by a study done by Clancy et al. which states COVID-19 patients with acute respiratory distress might be susceptible to secondary infections as a result of immune dysregulation [21].
Based on the available literature and guidelines, systemic corticosteroids have shown to reduce mortality and are recommended for moderate to severe COVID-19 cases. However, it must be taken into contemplation the requirement and doses for specific severe cases according to the age and prognosis with austere monitoring of blood glucose and blood pressure levels. It is crucial to make the patient vigilant of the possible menace involved with and without the treatment. Blood sugar monitoring with charting should be done at least six times a day as there is a need for strict glycemic control.
Evidence-based prophylactic use of antifungals is required for patients at risk and those who develops unilateral facial or orbital pain, headache, periocular swelling, double vision, or diminution of vision. This should be done while kee** in mind the risk of development of drug resistance. Also, COVID-19 recovered patients are advised to seek immediate medical attention in case of any such danger signs and follow-up of high-risk patients with COVID-19 for sequelae is premptory. A high index of suspicion, combined efforts from multiple departments, and timely intervention both medical and surgical were critical aspects and further it help in improvement of the survival outcomes and reduction in morbidity.
References
Prenissl J, Jaacks LM, Mohan V et al (2019) Variation in health system performance for managing diabetes among states in India: a cross-sectional study of individuals aged 15 to 49 years. BMC Med 17:92
Lim S, Bae JH, Kwon HS et al (2021) COVID-19 and diabetes mellitus: from pathophysiology to clinical management. Nat Rev Endocrinol 17:11–30
Alanio A, Dellière S, Fodil S, Bretagne S, Mégarbane B (2020) Prevalence of putative invasive pulmonary aspergillosis in critically ill patients with COVID-19. Lancet Respir Med 8(6):e48–e49
Chakrabarti A, Kaur H, Savio J et al (2019) Epidemiology and clinical outcomes of invasive mould infections in Indian intensive care units (FISF study). J Crit Care 51:64–70
Garg D, Muthu V, Sehgal IS et al (2021) Coronavirus disease (Covid-19) associated mucormycosis (CAM): case report and systematic review of literature. Mycopathologia. https://doi.org/10.1007/s11046-021-00528-2
Pasero D, Sanna S, Liperi C, Piredda D, Branca GP, Casadio L et al (2020) A challenging complication following SARS-CoV- 2 infection: a case of pulmonary mucormycosis. Infection. https://doi.org/10.1007/s15010-020-01561-x
Placik DA, Taylor WL, Wnuk NM (2020) Bronchopleural fistula development in the setting of novel therapies for acute respiratory distress syndrome in SARS-CoV-2 pneumonia. Radiol Case Rep 15(11):2378–2381
Monte Junior ESD, Santos M, Ribeiro IB, Luz GO, Baba ER, Hirsch BS et al (2020) Rare and fatal gastrointestinal mucormycosis (Zygomycosis) in a COVID-19 patient: a case report. Clin Endosc 53(6):746–749
Mekonnen ZK, Ashraf DC, Jankowski T et al (2021) Acute invasive rhino-orbital mucormycosis in a patient with COVID-19-Associated acute respiratory distress syndrome. Ophthalmic Plastic Reconstruct Surg 37(2):e40–e80. https://doi.org/10.1097/iop.0000000000001889
Werthman-Ehrenreich A (2021) Mucormycosis with orbital compartment syndrome in a patient with COVID-19. Am J Emerg Med 42:264.e5-264.e8. https://doi.org/10.1016/j.ajem.2020.09.032
Mehta S, Pandey A (2020) Rhino-orbital mucormycosis associated with COVID-19. Cureus 12(9):e10726
Group WHOREAfC-TW, Sterne JAC, Murthy S, Diaz JV, Slutsky AS, Villar J et al (2020) Association between administration of systemic corticosteroids and mortality among critically Ill patients with COVID-19 a meta-analysis. JAMA 324(13):1330–13341
Cascella M, Rajnik M, Cuomo A, Dulebohn SC, Di Napoli R (2020) Features, evaluation and treatment coronavirus (COVID-19). Statpearls [internet].
Beigel JH, Tomashek KM, Dodd LE et al (2020) Remdesivir for the treatment of COVID-19—Final Report. N Engl J Med 383(19):1813–1826
The WHO Rapid Evidence Appraisal for COVID-19 Therapies Working Group (2020) Association between administration of systemic corticosteroids and mortality among critically Ill patients With COVID-19: a meta-ANALYSIS. JAMA 324(13):1330–1341
RECOVERY Collaborative Group (2021) Dexamethasone in hospitalized patients with COVID-19. N Engl J Med 384(8):693–704
Huang I, Lim MA, Pranata R (2020) Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia—a systematic review, meta-analysis, and meta-regression. Diabetes Metab Syndr 14(4):395–403
Donnelly JP, Chen SC, Kauffman CA et al (2020) Revision and update of the consensus definitions of invasive fungal disease from the European organization for research and treatment of cancer and the mycoses study group education and research consortium. Clin Infect Dis : An Off Publ Infect Dis Soc Am 71(6):1367–1376
Afroze SN, Korlepara R, Rao GV, Madala J (2017) Mucormycosis in a diabetic patient: a case report with an Insight into Its pathophysiology. Contemp Clin Dent 8(4):662–666
Chen G, Wu D, Guo W et al (2020) Clinical and immunological features of severe and moderate coronavirus disease 2019. J Clin Investig 130(5):2620–2629
Clancy CJ, Nguyen MH (2020) Coronavirus disease 2019, superinfections, and antimicrobial development: What can we expect? Clin Infect Dis 71(10):2736–2743
Acknowledgements
Dr. NC and Dr. ST are responsible for the concept of this paper, wrote the manuscript and made the figure and table outlines. Dr. AB provided Histopathological pictures valuable feedback, suggestions, and corrections to improve the quality of the manuscript. All the authors gave final approval of the version to be published and agree to be accountable for all aspects of the work.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
The procedure performed in study was in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was done in accordance with the ethical standards of our institution (IEC/VMMC/SJH/2021–11/13).
Informed Consent
Informed consent was obtained from all individuals and their attendants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Trehan, S., Chaudhary, N. & Bhasarkar, A. Wave of Invasive Fungal Disease on the Shores of COVID-19: A Case Series of COVID-19 Associated Rhino-Orbital Fungal Rhinosinusitis and Literature Review. Indian J Otolaryngol Head Neck Surg 74 (Suppl 2), 3359–3366 (2022). https://doi.org/10.1007/s12070-022-03213-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-022-03213-y