Abstract
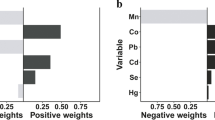
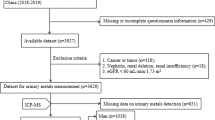
In the world, chronic kidney disease (CKD) has been recognized as one of the critical public health problems, and the prevalence is higher in the elderly people. However, there are few studies on the association between exposure to multiple serum metal levels and CKD. A case–control study, we established, for elderly people in Anhui Province, China, to explore the effects of different metals and analyze the effect of mixed exposure on CKD. In this study, 287 cases of CKD and 287 controls were selected in the elderly health physical examination project in Tongling City, Anhui Province. Questionnaire survey, physical examination, and blood collection were conducted. Graphite furnace atomic absorption spectrometry (GFAAS) and inductively coupled plasma optical emission spectrometry (ICP-OES) were used to measure the concentration of serum metals. After selecting by least absolute shrinkage and selection operator (LASSO), 5 metals were brought into the multi-metal model. After adjusting all potential covariates additionally, the concentrations of lead (Pb), cadmium (Cd), cobalt (Co), and manganese (Mn) were significantly associated with CKD risk, whereas Pb, Se, and Cd had significant non-linearity with CKD. Besides, patients with highest quartiles of cobalt (Co), lead (Pb), and manganese (Mn) were 1.64, 1.39, and 0.64 times more possible to have CKD, respectively, as compared with the lowest levels. In the Bayesian kernel machine regression (BKMR) model, cadmium (Cd) had a combined effect with lead (Pb) possibly. This study suggested that the CKD risk was associated with exposure of multiple metals in elderly people. The underlying mechanisms of serum metals and CKD need more experimental and prospective studies to elucidate.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Abdel-Moneim AM, El-Toweissy MY, Ali AM, Awad Allah AA, Darwish HS, Sadek IA (2015) Curcumin ameliorates lead (Pb(2+))-induced hemato-biochemical alterations and renal oxidative damage in a rat model. Biol Trace Elem Res 168:206–220. https://doi.org/10.1007/s12011-015-0360-1
Bobb JF, Valeri L, Claus Henn B, Christiani DC, Wright RO, Mazumdar M, Godleski JJ, Coull BA (2015) Bayesian kernel machine regression for estimating the health effects of multi-pollutant mixtures. Biostatistics 16:493–508. https://doi.org/10.1093/biostatistics/kxu058
Chen X, Chen X, Wang X, Wang M, Liang Y, Zhu G, ** T (2021) The association between estimated glomerular filtration rate and cadmium exposure: an 8-year follow-up study. Int J Hyg Environ Health 235:113774. https://doi.org/10.1016/j.ijheh.2021.113774
Edoardo G, Vito GA, Brunella L, Vincenzo T (2015) Selenium and iodine in autoimmune thyroiditis. Endocrine 4:288–292. https://doi.org/10.2174/1871530315666150619094242
Gandhi D, Rudrashetti AP, Rajasekaran S (2022) The impact of environmental and occupational exposures of manganese on pulmonary, hepatic, and renal functions. J Appl Toxicol 42:103–129. https://doi.org/10.1002/jat.4214
GBD Chronic Kidney Disease Collaboration (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease study 2017. Lancet 395:709–733. https://doi.org/10.1016/S0140-6736(20)30045-3
Grau-Perez M, Pichler G, Galan-Chilet I, Briongos-Figuero LS, Rentero-Garrido P, Lopez-Izquierdo R, Navas-Acien A, Weaver V, García-Barrera T, Gomez-Ariza JL, Martín-Escudero JC, Chaves FJ, Redon J, Tellez-Plaza M (2017) Urine cadmium levels and albuminuria in a general population from Spain: a gene-environment interaction analysis. Environ Int 106:27–36. https://doi.org/10.1016/j.envint.2017.05.008
Hagedoorn IJM, Gant CM, Huizen SV, Maatman R, Navis G, Bakker SJL, Laverman GD (2020) Lifestyle-related exposure to cadmium and lead is associated with diabetic kidney disease. J Clin Med 9:2432. https://doi.org/10.3390/jcm9082432
Harari F, Sallsten G, Christensson A, Petkovic M, Hedblad B, Forsgard N, Melander O, Nilsson PM, Borné Y, Engström G, Barregard L (2018) Blood lead levels and decreased kidney function in a population-based cohort. Am J Kidney Dis 72:381–389. https://doi.org/10.1053/j.ajkd.2018.02.358
He JL, Li GA, Zhu ZY, Hu MJ, Wu HB, Zhu JL, Zhao HH, Zhang HS, Huang F (2021) Associations of exposure to multiple trace elements with the risk of goiter: a case-control study. Environ Pollut 288:117739. https://doi.org/10.1016/j.envpol.2021.117739
Hsu LI, Hsieh FI, Wang YH, Lai TS, Wu MM, Chen CJ, Chiou HY, Hsu KH (2017) Arsenic exposure from drinking water and the incidence of CKD in low to moderate exposed areas of Taiwan: a 14-year prospective study. Am J Kidney Dis 70:787–797. https://doi.org/10.1053/j.ajkd.2017.06.012
Hsueh YM, Huang YL, Lin YF, Shiue HS, Lin YC, Chen HH (2021) Plasma vitamin B12 and folate alter the association of blood lead and cadmium and total urinary arsenic levels with chronic kidney disease in a Taiwanese population. Nutrients 13:3841. https://doi.org/10.3390/nu13113841
Jain RB (2019a) Lead and kidney: concentrations, variabilities, and associations across the various stages of glomerular function. J Trace Elem Med Biol 54:36–43. https://doi.org/10.1016/j.envpol.2019.113361
Jain RB (2019b) Co-exposures to toxic metals cadmium, lead, and mercury and their impact on unhealthy kidney function. Environ Sci Pollut Res Int 26:30112–30118. https://doi.org/10.1007/s11356-019-06182-y
** R, Zhu X, Shrubsole MJ, Yu C, **a Z, Dai Q (2018) Associations of renal function with urinary excretion of metals: evidence from NHANES 2003–2012. Environ Int 121:1355–1362. https://doi.org/10.1016/j.envint.2018.11.002
Johri N, Jacquillet G, Unwin R (2010) Heavy metal poisoning: the effects of cadmium on the kAssociations of plasma metal concentrations with the decline in kidney function: a longitudinal study of Chinese adults. idney. Biometals 23:783–792. https://doi.org/10.1007/s10534-010-9328-y
Kulathunga M, Wijayawardena MAA, Naidu R (2021) Dietary heavy metal(loid)s exposure and prevalence of chronic kidney disease of unknown aetiology (CKDu) in Sri Lanka. Environ Geochem Health. https://doi.org/10.1007/s10653-021-01144-1
Liu YK, Xu H, Liu F, Tao R, Yin J (2010) Effects of serum cobalt ion concentration on the liver, kidney and heart in mice. Orthop Surg 2:134–140. https://doi.org/10.1111/j.1757-7861.2010.00076.x
Liu Y, Yuan Y, **ao Y, Li Y, Yu Y, Mo T, Jiang H, Li X, Yang H, Xu C, He M, Guo H, Pan A, Wu T (2020) Associations of plasma metal concentrations with the decline in kidney function: a longitudinal study of Chinese adults. Ecotoxicol Environ Saf 189:110006. https://doi.org/10.1016/j.ecoenv.2019.110006
Lv Y, Wei Y, Zhou J, Xue K, Guo Y, Liu Y, Ju A, Wu B, Zhao F, Chen C, **ong J, Li C, Gu H, Cao Z, Ji JS, Shi X (2021) Human biomonitoring of toxic and essential metals in younger elderly, octogenarians, nonagenarians and centenarians: analysis of the healthy ageing and biomarkers cohort study (HABCS) in China. Environ Int 156:106717. https://doi.org/10.1016/j.envint.2021.106717
Ma YC, Zuo L, Chen JH, Luo Q, Yu XQ, Li Y, Xu JS, Huang SM, Wang LN, Huang W, Wang M, Xu GB, Wang HY (2006) Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. J Am Soc Nephrol 17:2937–2944. https://doi.org/10.1681/ASN.2006040368
Mascarenhas S, Mutnuri S, Ganguly A (2017) Deleterious role of trace elements - silica and lead in the development of chronic kidney disease. Chemosphere 177:239–249. https://doi.org/10.1016/j.chemosphere.2017.02.155
Miao H, Liu L, Wang Y, Wang Y, He Q, Jafar TH, Tang S, Zeng Y, Ji JS (2022) Chronic kidney disease biomarkers and mortality among older adults: A comparison study of survey samples in China and the United States. PLoS One 17:e0260074. https://doi.org/10.1371/journal.pone.0260074
Nigra AE, Navas-Acien A (2021) Racial inequalities in drinking water lead exposure: a wake-up call to protect patients with end stage kidney disease. J Am Soc Nephrol 32:2419–2421. https://doi.org/10.1681/ASN.2021060793
Orr SE, Bridges CC (2017) Chronic kidney disease and exposure to nephrotoxic metals. Int J Mol Sci 18:1039. https://doi.org/10.3390/ijms18051039
Pan CF, Lin CJ, Chen SH, Huang CF, Lee CC (2019) Association between trace element concentrations and anemia in patients with chronic kidney disease: a cross-sectional population-based study. J Investig Med 67:995–1001. https://doi.org/10.1136/jim-2018-000833
Peters BA, Hall MN, Liu X, Slavkovich V, Ilievski V, Alam S, Siddique AB, Islam T, Graziano JH, Gamble MV (2015) Renal function is associated with indicators of arsenic methylation capacity in Bangladeshi adults. Environ Res 143:123–130. https://doi.org/10.1016/j.envres.2015.10.001
Rana MN, Tangpong J, Rahman MA (2020) Xanthones protects lead-induced chronic kidney disease (CKD) via activating Nrf-2 and modulating NF-kB, MAPK Pathway. Biochem Biophys Rep 21:100718. https://doi.org/10.1016/j.bbrep.2019.100718
Ren Q, Shi Q, Ma T, Wang J, Li Q, Li X (2019) Quality of life, symptoms, and sleep quality of elderly with end-stage renal disease receiving conservative management: a systematic review. Health Qual Life Outcomes 17:78. https://doi.org/10.1186/s12955-019-1146-5
Sanders AP, Mazzella MJ, Malin AJ, Hair GM, Busgang SA, Saland JM, Curtin P (2019) Combined exposure to lead, cadmium, mercury, and arsenic and kidney health in adolescents age 12–19 in NHANES 2009–2014. Environ Int 131:104993. https://doi.org/10.1016/j.envint.2019.104993
Satarug S, Vesey DA, Gobe GC (2017) Current health risk assessment practice for dietary cadmium: data from different countries. Food Chem Toxicol 106:430–445. https://doi.org/10.1016/j.fct.2017.06.013
Satarug S, Gobe GC, Vesey DA, Phelps KR (2020) Cadmium and lead exposure, nephrotoxicity, and mortality. Toxics 8:86. https://doi.org/10.3390/toxics8040086
Scammell MK, Sennett CM, Petropoulos ZE, Kamal J, Kaufman JS (2019) Environmental and occupational exposures in kidney disease. Semin Nephrol 39:230–243. https://doi.org/10.1016/j.semnephrol.2019.02.001
Shen Y, Yin Z, Lv Y, Luo J, Shi W, Fang J, Shi X (2020) Plasma element levels and risk of chronic kidney disease in elderly populations (>/= 90 years old). Chemosphere 254:126809. https://doi.org/10.1016/j.chemosphere.2020.126809
Totoli C, Carvalho AB, Ammirati AL, Draibe SA, Canziani MEF (2019) Associated factors related to chronic kidney disease progression in elderly patients. PLoS One 14:e0219956. https://doi.org/10.1371/journal.pone.0219956
Tsai TL, Kuo CC, Pan WH, Chung YT, Chen CY, Wu TN, Wang SL (2017) The decline in kidney function with chromium exposure is exacerbated with co-exposure to lead and cadmium. Kidney Int 92:710–720. https://doi.org/10.1016/j.kint.2017.03.013
Tsai HJ, Hung CH, Wang CW, Tu HP, Li CH, Tsai CC, Lin WY, Chen SC, Kuo CH (2021a) Associations among heavy metals and proteinuria and chronic kidney disease. Diagnostics (basel) 11:282. https://doi.org/10.3390/diagnostics11020282
Tsai HJ, Wu PY, Huang JC, Chen SC (2021b) Environmental pollution and chronic kidney disease. Int J Med Sci 18:1121–1129. https://doi.org/10.7150/ijms.51594
Tugcu M, Barutcu Atas D (2021) Chronic kidney disease progression in aged patients. Int Urol Nephrol 53:2619–2625. https://doi.org/10.1007/s11255-021-02806-w
Wang L, Wang H, Hu M, Cao J, Chen D, Liu Z (2009) Oxidative stress and apoptotic changes in primary cultures of rat proximal tubular cells exposed to lead. Arch Toxicol 83:417–427. https://doi.org/10.1007/s00204-009-0425-z
Wang X, Cui W, Wang M, Liang Y, Zhu G, ** T, Chen X (2021) The association between life-time dietary cadmium intake from rice and chronic kidney disease. Ecotoxicol Environ Saf 211:111933. https://doi.org/10.1016/j.ecoenv.2021.111933
Webster AC, Nagler EV, Morton RL, Masson P (2017) Chronic kidney disease. the. Lancet 389:1238–1252. https://doi.org/10.1016/S0140-6736(16)32064-5
Wei J, Yin X, Liu Q, Tan L, Jia C (2018) Association between hypertension and cognitive function: a cross-sectional study in people over 45 years old in China. J Clin Hypertens (greenwich) 20:1575–1583. https://doi.org/10.1111/jch.13393
Wu W, Zhang K, Jiang S, Liu D, Zhou H, Zhong R, Zeng Q, Cheng L, Miao X, Tong Y, Lu Q (2018) Association of co-exposure to heavy metals with renal function in a hypertensive population. Environ Int 112:198–206. https://doi.org/10.1016/j.envint.2017.12.023
Zelko IN, Mariani TJ, Folz RJ (2002) Superoxide dismutase multigene family: a comparison of the CuZn-SOD (SOD1), Mn-SOD (SOD2), and EC-SOD (SOD3) gene structures, evolution, and expression. Free Radic Biol Med 33:337–349. https://doi.org/10.1016/s0891-5849(02)00905-x
Zhang H, Tsao R (2016) Dietary polyphenols, oxidative stress and antioxidant and anti-inflammatory effects. Curr Opin Food Sci 8:33–42. https://doi.org/10.1016/j.cofs.2016.02.002
Zhang Q, Zhang C, Ge J, Lv MW, Talukder M, Guo K, Li YH, Li JL (2020) Ameliorative effects of resveratrol against cadmium-induced nephrotoxicity via modulating nuclear xenobiotic receptor response and PINK1/Parkin-mediated Mitophagy. Food Funct 11:1856–1868. https://doi.org/10.1039/c9fo02287b
Zheng LY, Umans JG, Yeh F, Francesconi KA, Goessler W, Silbergeld EK, Bandeen-Roche K, Guallar E, Howard BV, Weaver VM, Navas-Acien A (2015) The association of urine arsenic with prevalent and incident chronic kidney disease: evidence from the Strong Heart Study. Epidemiology 26:601–612. https://doi.org/10.1097/EDE.0000000000000313
Zhou TT, Hu B, Meng XL, Sun L, Li HB, Xu PR, Cheng BJ, Sheng J, Tao FB, Yang LS, Wu QS (2021) The associations between urinary metals and metal mixtures and kidney function in Chinese community-dwelling older adults with diabetes mellitus. Ecotoxicol Environ Saf 226:112829. https://doi.org/10.1016/j.ecoenv.2021.112829
Zhu XJ, Wang JJ, Mao JH, Shu Q, Du LZ (2019) Relationships of cadmium, lead, and mercury levels with albuminuria in US adults: results from the National Health and Nutrition Examination Survey Database, 2009–2012. Am J Epidemiol 188:1281–1287. https://doi.org/10.1093/aje/kwz070
Acknowledgements
This study was supported by The Project for Top Disciplinary Talents of Majors in Universities of Anhui Province (gxbjZD09). Thanks to all the subjects that participated in this research. The final manuscript was read and approved by all the authors.
Funding
This study was supported by The Project for Top Disciplinary Talents of Majors in Universities of Anhui Province (gxbjZD09).
Author information
Authors and Affiliations
Contributions
Wenlei Hu: study concept and design, acquisition of data, analysis and interpretation of the data, and drafting of the article. Guoao Li: acquisition of data, analysis and interpretation of data, and drafting of the article. Jialiu He: acquisition of the data, analysis and interpretation of the data. Huanhuan Zhao: acquisition of the data, critical review of manuscript. Hanshuang Zhang: acquisition of the data, critical review of the manuscript. Huan-huan Lu: analysis and interpretation of the data. Jian-jun Liu: analysis and interpretation of the data. Fen Huang: study concept and design, critical review of the manuscript, and funding acquisition. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
The questionnaire and methodology for this study was approved by the Biomedical Ethics Committee of the Anhui Medical University (Ethics approval number: 20180085).
Consent to participate
All the participants were required to provide written informed consent for admission.
Consent for publication
All the authors contributed to the article and approved the submitted version.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Wenlei Hu and Guoao Li contributed equally to this work and should be considered as co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hu, W., Li, G., He, J. et al. Association of exposure to multiple serum metals with the risk of chronic kidney disease in the elderly: a population-based case–control study. Environ Sci Pollut Res 30, 17245–17256 (2023). https://doi.org/10.1007/s11356-022-23303-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-022-23303-2