Abstract
To investigate factors associated with online sex-seeking behaviors among men who have sex with men (MSM) in Bei**g, China. MSM participants were recruited from two cohort studies with multiple enrollment methods from November 2006 to February 2007 and from March to June 2008, respectively. Data collected included demographics and sexual behaviors. Of the 901 participants, 68.1% were single; 69.3% were non-Bei**g residents; 94.4% considered themselves to be homosexual; 65.2% received college or higher levels of education; the median age was 26 years; 73.0% sought male sex partners via the Internet in the past 3 months; 66.2% had ≥2 sex partners. Younger age, higher levels of education and having had ≥2 male sex partners in the past 3 months were independently associated with seeking sex partners on the Internet. These findings indicate that Internet-based intervention programs could encourage younger high-risk MSM to use condoms and reduce their numbers of sexual partners.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In recent years, men who have sex with men (MSM) in China have emerged as a group at high risk of contracting and subsequently spreading HIV [1–6]. Homosexual transmission contributed to 11.0% of the newly infected in 2007; this rate increased to 30% in 2008 [7]. The proportion of reported HIV cases among MSM increased sevenfold from 0.4% in 2005 to 3.3% in 2007 [8]. Our recent cohort study showed that HIV rapidly spread among MSM in Bei**g, with an incidence rate of 2.6/100 person-years [5]. The confluence of high HIV prevalence and incidence, along with common high-risk behaviors, suggests the HIV epidemic among MSM in China has emerged as a significant public health challenge [2, 4–6].
In the past decade, the use of the Internet in China has grown rapidly [9]. Evidence has shown that the Internet is becoming a burgeoning sex-seeking environment [10–13]. Moreover, MSM are more likely to use the Internet to find sexual partners than heterosexuals [14]. A London study found that about 40% to 50% of MSM used the Internet to seek sex [15]. Another report found that 81% of the participants had access to the Internet [16]. The use of the Internet among MSM to find sexual partners is increasing, including MSM who are HIV-positive [17]; young MSM who seek partners online also engage in other behaviors that place them at risk of acquisition and transmission of HIV and other sexually transmitted diseases (STDs) [18, 19]. Several studies have shown that MSM participants recruited online report higher rates of high-risk behaviors than those recruited offline [20, 21], especially among HIV-positive men [22]. MSM who engage in high-risk sex were more likely to use the Internet for meeting sexual partners [23].
By the end of 2009, the number of Internet users had reached 384 million in China, the most of any country. Of Internet users, 54% were male [9]. This includes approximately 4–10 million MSM Internet users [24]. Currently, almost all cities have local gay-oriented websites that facilitate the communication and sex partner-seeking among MSM [25]. However, little is known about the use of the Internet among MSM in China. The objective of this study was to assess the correlates for sex-seeking via the Internet among MSM in Bei**g.
Methods
Study Design and Study Participants
Study subjects included all participants enrolled in the baseline of two cohort studies conducted among MSM in Bei**g from November 2006 to February 2007 and from March 2008 to June 2008, respectively. Participants in both studies were recruited using three similar recruitment methods: (1) study staff contacted potential participants and made appointments with willing participants who provided contact information through website advertisements by a non-governmental AIDS volunteer group (http://www.hivolunt.net); (2) peer recruiters were hired and trained to distribute flyers with study-related information at MSM-frequented venues (e.g., gay-oriented clubs, bars, parks and bathhouses); and (3) participants were encouraged to refer their peers to attend the study, as described elsewhere [2]. All potential participants came to a district HIV voluntary counseling and testing clinic in downtown Bei**g. The location of the clinic was easy to access via various transportation routes. Confidentiality and privacy were ensured in the study. Eligibility criteria for these two cohorts included ≥18 years, male, had anal or oral sex with another man in the past 3 months, provided written informed consent and willingness to complete the study. Those who met the screening criteria were assigned a unique and confidential identification code and then completed a questionnaire-based interview. At the end of the interview, client-centered risk reduction counseling was provided on HIV, hepatitis B virus, hepatitis C virus, syphilis, and other STDs. Blood samples were tested for HIV and syphilis. Participants were instructed to return in one month for their results; a pre-assigned unique code was used to inform participants of their results. The reimbursement amount for participants was 50 Yuan RMB (approximately $7 USD), 12 free condoms and one free lubricant. The study was approved by the Institutional Review Boards of the National Center for AIDS/STD Control and Prevention of the China Center for Disease Control and Prevention.
Measures
In both studies, identical questionnaire-based interviews were conducted on a one-on-one basis in a separate and private room of the district clinic. Trained health professionals conducted the interviews. Data collected included sociodemographic information (e.g., age, ethnicity, education, residence, income, marital status, and housing status), behavioral information (e.g., self-identified sexual orientation, sought male sex partners on the Internet in the past 3 months, the number of male sex partners in the past 3 months, had foreign male partners in the past 3 months, participated in male group sex in the past 3 months, had commercial sex with male partners in the past 3 months, had unprotected anal intercourse [UAI] with regular or casual male partners in the past month, had sex with female sex partners in the past 3 months, frequency of alcohol intoxication in the past 3 months, illicit drug use in the past 3 months, ever had an HIV test, attended any AIDS program in the past 3 months) and psychological information (experienced discrimination in the past month, experienced loneliness in the past month, experienced depression in the past month, experienced sadness in the past month).
Laboratory Tests
HIV status was determined by an enzyme immunoassay (EIA) (Bei**g Wantai Biological Medicine Company, China) screening and an HIV-1/2 Western Blot confirmation (HIV Blot 2.2 WBTM, Genelabs Diagnostics). Syphilis infection was determined using an EIA (Bei**g Wantai Biological Production Company, Bei**g, China) and confirmed using a Passive Particle Agglutination Test for Detection of Antibodies to Treponema pallidum (TPHA™, OMEGA, UK) in the first cohort study and confirmed by a Passive Particle Agglutination Test for Detection of Antibodies to Treponema pallidum (TPPA™, FUJIREBIO, Japan) in the second cohort study.
Statistical Analysis
Questionnaire-based data and biological testing results were recorded, double-checked and compared with EpiData software (EpiData 3.0™ for Windows; The EpiData Association Odense, Denmark). After corrections, data were then converted and analyzed using Statistical Analysis System (SAS 9.1™ for Windows; SAS Institute Inc., NC, USA). Univariate analyses were conducted using Chi-square tests and Fisher’s exact tests. Variables with P-values < 0.20 were entered into a multivariable logistic regression model in order to identify factors independently associated with seeking male sex partners on the Internet. Only factors with P-values < 0.05 (two-tailed) were deemed statistically significant.
Results
Baseline Characteristics of the Participants
A total of 901 eligible MSM (541 in the first cohort and 360 in the second cohort) were included in the data analyses. Of the 901 participants, 5.3% were infected with HIV, 22.3% with syphilis, 6.0% with HBsAg, and 0.7% with HCV. Of the participants, 38.6% were recruited via the Internet and 43.8% via peer referral; the median age was 26 years (range from 18 to 62 years) with 54.8% being ≤26 years; 92.1% belonged to the Han ethnic group; and 65.2% completed college or higher levels of education. Bei**g residents accounted for 30.7%; the median monthly income was US$ 294; 18.9% were rural residents; 68.1% were single and 11.4% were married or cohabiting with female sex partners (Table 1).
Sexual Behaviors
Participants who identified as exclusively homosexual and predominantly homosexual accounted for 53.3 and 41.2%, respectively, whereas 5.6% of the participants identified as predominantly heterosexual with only incidental homosexual activities. The median number of male partners in a lifetime was 10. In the past 3 months, 62.2% had ≥2 male sexual partners; 3.4% had sex with foreign male partners; 7.7% participated in male group sex; 7.6% had commercial sex with men; 4.9% were “money boys” (local parlance for male commercial sex workers); 13.0% had sex with female partners. In the past month, 18.3 and 14.2% of the participants had UAI with regular male partners and casual sex partners, respectively; 6.2% had unprotected sex with female partners. Of the participants, 5.7% reported feeling discriminated against in the past month; 54.1% experienced loneliness in the past month; 44.5% experienced depression in the past month; and 42.3% have ever experienced sadness. Of the participants, 38.7% drank alcohol in the past 3 months and only 0.8% used illicit drugs (mainly ecstasy and ketamine), 10% attended an AIDS program in the past 3 months, 51.8% had ever received an HIV test and 26.9% had ever received an STD diagnosis by a clinic physician (Table 1).
Factors Associated with Seeking Sex Partners on the Internet
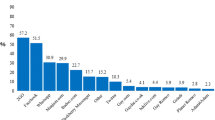
Of the 901 participants, 73.0% had sought male sex partners through the Internet in the past 3 months. The proportion of online sex-seeking was 68.9, 81.3 and 65.2% among study participants recruited through peer referral, the Internet and MSM-frequented venues, respectively. In the univariate analysis, factors significantly associated with seeking male sex partners via the Internet in the past 3 months were younger age, higher levels of education, rural residency, married or cohabiting with female sex partners in the past 3 months, exclusively homosexual sexual orientation, more male sex partners in the past 3 months, drinking alcohol ≥1 times per week in the past 3 months and having an STD diagnosed by a clinic physician in the past (Table 2). In multivariable logistic regression analysis, after controlling for five variables (rural residency, married or cohabiting with female sex partners in the past 3 months, exclusively homosexual sexual orientation, drank alcohol ≥1 times per week in the past 3 months, and had an STD diagnosed by a clinic physician), seeking male sex partners on the Internet in the past 3 months was independently associated with younger age (AOR = 2.6, 95% CI: 1.9–3.6; ≤26 vs. >26 years of age), higher levels of education (AOR = 2.3, 95% CI 1.9–2.9) and having more sex partners (AOR = 2.0, 95% CI 1.5–2.8; ≥2 vs. <2) (Table 3).
Discussion
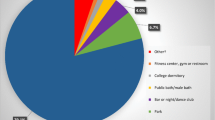
Our study found an extremely high prevalence (73%) of online sex-seeking in the past 3 months among MSM in Bei**g; this rate is substantially higher than in a previous meta-analysis (approximately 40% [95%CI, 35.2%–45.2%]) [13]. The Internet has been playing an increasingly important role in people’s daily lives, particularly as an efficient mode of communication in many developed metropolitan cities in China. Economic development and improved literacy rates have allowed a growing number of people to access the Internet. In China, MSM are highly stigmatized and they face social pressures from those who adhere to the traditional culture. Hence, the Internet is especially popular with MSM because of its accessibility, affordability and anonymity [26]. When seeking sex partners on the Internet, MSM can be open about their sexual orientation and yet remain anonymous. Besides the Internet, MSM seek sex partners mainly through bars, parks, bathhouses, and public washrooms [27, 28]. However, these venues are less effective compared to online sex seeking, because of the relatively fewer opportunities to satisfy unique preferences in sex partners. Moreover, seeking sex partners offline has disadvantages due to transportation costs, time, potential disclosure of their sexual orientation, and privacy concerns. On the contrary, MSM can seek sex partners via the Internet more efficiently as they can search for other MSM who satisfy specific personal preferences. In addition, seeking partners online allows men the opportunity to get to know someone better [26] before engaging in sex. All of these advantages may lead to more MSM seeking male sex partners online.
That the rate of online sex-seeking among MSM in Bei**g found in this study is higher than any other report [12, 13, 15] might be a result of the high density of residents, rising individual incomes, technological development, and increasing availability, accessibility, and knowledge of computers in the past decade in Bei**g. More tolerant views and broader sexual freedoms due to the dramatic socioeconomic transition in China, particularly in modern metropolitan areas such as Bei**g, could be another contributor for extremely common online sex seeking. The growing popularity of the Internet suggests increasingly prevalent online sex-seeking among MSM in the near future. This indicates that the Internet could provide opportunities for recruiting study participants [29, 30] into either qualitative or quantitative studies [26], as well as intervention service delivery. For example, QQ, a software service like MSN instant messaging, is popular in China; it could serve as a platform for peer education and intervention. Information on HIV/AIDS intervention and prevention can be delivered via peer networks of QQ users. The Internet offers an opportunity to delivery information more effectively and quickly to MSM. Further research is needed to better understanding how to effectively deliver HIV prevention messages via the Internet.
This study found that younger age and higher levels of education were independently associated with online sex seeking among MSM in Bei**g, which is consistent with other reports [12, 31]. Young and educated MSM are more likely to adopt innovative technologies and learn the skills necessary to access the Internet [12, 31]. Furthermore, most well-educated MSM with higher social status might be more afraid of disclosure of their sexual orientation, so the Internet becomes their preferred way to seek sex partners [26, 32]. Results from studies in developed countries differed [20, 33], in that community-based sampling recruited more educated participants than those recruited via the Internet. This might result from differences in Internet user populations and literacy patterns in China compared with developed countries. In China, the overall proportion of the population who use the Internet is relatively low; therefore, education could be a critical factor to accessing the Internet [34]. This study found that participants who had more male sex partners were more likely to seek sex partners on the Internet. Other studies have found that online sex-seeking is associated with high-risk sexual behaviors and increased rates of STDs [14, 20, 21]. Given the high prevalence rates of HIV and syphilis among MSM in Bei**g, future studies need to achieve a better understanding of the different characteristics of venue versus non-venue community-based HIV and syphilis disease distributions. This study provides useful preliminary data in guiding interventions and furthers research on Internet use among this group.
Previous studies have found that social isolation, loneliness, desperation, and sexual orientation were the main reasons for men’s use of the Internet to facilitate sexual encounters [35]. Loneliness in particular was the primary motivator for MSM to meet sex partners in online chat rooms [36]. MSM in China are traditionally marginalized, causing them to suffer long-term sexual depression and hide their sexual orientations, which in turn leads to even higher degrees of depression [37]. Although a statistically significant association between experiencing loneliness, depression or sadness and online sex seeking was not shown in this study, these psychological syndromes were common among participants. These findings underscore that intervention efforts should tackle prevalent psychological syndromes among this group; the Internet could be one of the venues to deliver such intervention measures.
Some studies have found associations between meeting sex partners online and having unprotected sex, but others have noted that when studying specific online versus offline encounters there is no difference [23]. This study suggested that online sex seeking is associated with HIV/STD risk behaviors. Further research with longitudinal cohort designs is needed to better understand the lack of differences between men who seek partners online versus those who do not.
We realize the limitations of this study. First, recall bias may exist due to the self-reported questionnaire. Second, we used dichotomous yes/no questions to measure discrimination, loneliness, depression, and sadness. The pilot survey showed Chinese MSM liked this dichotomous format, but further validation of the survey’s psychological questions is needed. Third, only one-third of participants were Bei**g residents; the interpretations of this study may not accurately pertain to MSM in Bei**g. However, Bei**g, like many other cities in China, has a significant proportion of people living and working in the city for months or years without a permanent resident identification “hukou.” These residents were classified as “non-Bei**g residents” in this analysis. Participants were required to have physically lived in Bei**g for 12 months or more, per the study inclusion criteria. Lastly, the nature of this cross-sectional study design precludes causal association. In spite of these limitations, this study using multiple recruiting methods with sociodemographic map** strategies provides a first examination of Internet sex seeking behaviors in Bei**g.
The Internet reduces physical, geographic, social, psychological, and financial barriers and enables people to communicate efficiently on a massive global scale. This study found that online sex seeking was extremely common among MSM in Bei**g and that online sex seeking was independently associated with more sexual partners, higher education, and younger age. These findings indicate that Internet-based intervention programs could encourage younger high-risk MSM to use condoms and reduce their numbers of sexual partners. Extremely common online sex-seeking in confluence with high prevalence and incidence of HIV/syphilis/other STDs and high-risk behaviors among MSM in Bei**g [2, 5, 6, 8] highlighted the urgent need to harness the Internet as a medium of conducting HIV research, intervention, information delivery, education/skills building, and health promotion in China [2, 12, 26, 29, 30, 38–42].
References
Liu L, Luan R, Yang W, et al. Projecting dynamic trends for HIV/AIDS in a highly endemic area of China: estimation models for Liangshan Prefecture, Sichuan Province. Curr HIV Res. 2009;7(4):390–7.
Li D, Jia Y, Ruan Y, et al. Correlates of Incident Infections for HIV, Syphilis, and Hepatitis B Virus in A Cohort of Men Who Have Sex with Men in Bei**g. AIDS Patient Care STDS. 2010;24(9):595–602.
State Council AIDS Working Committee Office, UN theme Group on HIV/AIDS in China. A Joint Assessment of HIV/AIDS Prevention, Treatment and Care in China (2007). Bei**g, 2007.
**ao Y, Sun J, Li C, et al. Prevalence and correlates of HIV and syphilis infections among men who have sex with men in seven provinces in China with historically low HIV prevalence. J Acquir Immune Defic Syndr. 2010;53(Suppl 1):S66–73.
Ruan Y, Jia Y, Zhang X, et al. Incidence of HIV-1, syphilis, hepatitis B, and hepatitis C virus infections and predictors associated with retention in a 12-month follow-up study among men who have sex with men in Bei**g, China. J Acquir Immune Defic Syndr. 2009;52(5):604–10.
Ruan Y, Luo F, Jia Y, et al. Risk factors for syphilis and prevalence of HIV, hepatitis B and C among men who have sex with men in Bei**g, China: implications for HIV prevention. AIDS Behav. 2009;13(4):663–70.
China Ministry of Health. Status of the AIDS epidemic in China. Bei**g: China Ministry of Health, 2009.
China CDC. National Surveillance Report for HIV/AIDS in 2007. Bei**g: National Center for AIDS/STD Control and Prevention; 2008.
China Internet Network Information Center. The 25th Statistics Report of China internet development. Bei**g: China Internet Network Information Center, 2010.
Berg RC. Barebacking among MSM Internet users. AIDS Behav. 2008;12(5):822–33.
Leobon A, Frigault LR. Frequent and systematic unprotected anal intercourse among men using the Internet to meet other men for sexual purposes in France: results from the “Gay Net Barometer 2006” survey. AIDS Care. 2008;20(4):478–84.
Lau JT, Kim JH, Lau M, Tsui HY. Prevalence and risk behaviors of Chinese men who seek same-sex partners via the internet in Hong Kong. AIDS Educ Prev. 2003;15(6):516–28.
Liau A, Millett G, Marks G. Meta-analytic examination of online sex-seeking and sexual risk behavior among men who have sex with men. Sex Transm Dis. 2006;33(9):576–84.
McFarlane M, Bull SS, Rietmeijer CA. The Internet as a newly emerging risk environment for sexually transmitted diseases. JAMA. 2000;284(4):443–6.
Bolding G, Davis M, Hart G, Sherr L, Elford J. Gay men who look for sex on the Internet: is there more HIV/STI risk with online partners? AIDS. 2005;19(9):961–8.
Elford J, Bolding G, Sherr L. Seeking sex on the Internet and sexual risk behaviour among gay men using London gyms. AIDS. 2001;15(11):1409–15.
Golden MR, Wood RW, Buskin SE, Fleming M, Harrington RD. Ongoing risk behavior among persons with HIV in medical care. AIDS Behav. 2007;11(5):726–35.
Garofalo R, Herrick A, Mustanski BS, Donenberg GR. Tip of the Iceberg: young men who have sex with men, the Internet, and HIV risk. Am J Public Health. 2007;97(6):1113–7.
Horvath KJ, Rosser BR, Remafedi G. Sexual risk taking among young internet-using men who have sex with men. Am J Public Health. 2008;98(6):1059–67.
Elford J, Bolding G, Davis M, Sherr L, Hart G. Web-based behavioral surveillance among men who have sex with men: a comparison of online and offline samples in London, UK. J Acquir Immune Defic Syndr. 2004;35(4):421–6.
Evans AR, Wiggins RD, Mercer CH, Bolding GJ, Elford J. Men who have sex with men in Great Britain: comparison of a self-selected internet sample with a national probability sample. Sex Transm Infect. 2007;83(3):200–5, discussion 5.
Halkitis PN, Parsons JT. Intentional unsafe sex (barebacking) among HIV-positive gay men who seek sexual partners on the internet. AIDS Care. 2003;15(3):367–78.
Mustanski BS. Are sexual partners met online associated with HIV/STI risk behaviours? Retrospective and daily diary data in conflict. AIDS Care. 2007;19(6):822–7.
Zhang BC, Li XF, Shi TX, Yang LG, Zhang JD. Estimation of the population and the HIV prevalence among MSM in China. Chin J STD/AIDS Prev Cont. 2002;8(4):197–9.
Lin K, Gao YN, Chen YF. Study on the function of homosexual websites and HIV/AIDS health education among men who have sex with men in China. Chin J Health Educ. 2008;24(3):179–84.
Ross MW, Rosser BR, McCurdy S, Feldman J. The advantages and limitations of seeking sex online: a comparison of reasons given for online and offline sexual liaisons by men who have sex with men. J Sex Res. 2007;44(1):59–71.
Bolding G, Davis M, Hart G, Sherr L, Elford J. Where young MSM meet their first sexual partner: the role of the Internet. AIDS Behav. 2007;11(4):522–6.
Grov C, Parsons JT, Bimbi DS. Sexual risk behavior and venues for meeting sex partners: an intercept survey of gay and bisexual men in LA and NYC. AIDS Behav. 2007;11(6):915–26.
Bowen A, Williams M, Horvath K. Using the internet to recruit rural MSM for HIV risk assessment: sampling issues. AIDS Behav. 2004;8(3):311–9.
Fernandez MI, Varga LM, Perrino T, et al. The Internet as recruitment tool for HIV studies: viable strategy for reaching at-risk Hispanic MSM in Miami? AIDS Care. 2004;16(8):953–63.
Yun G, Trumbo C. Comparative response to a survey executed by post, email and web form. JCMC. 2006. doi:10.1111/j.1083-6101.2000.tb00112.x. Available at: http://onlinelibrary.wiley.com/doi/10.1111/j.1083-6101.2000.tb00112.x/abstract. Accessed 12 July 2011.
Rietmeijer CA, Bull SS, McFarlane M. Sex and the internet. AIDS. 2001;15(11):1433–4.
Ross MW, Tikkanen R, Mansson SA. Differences between Internet samples and conventional samples of men who have sex with men: implications for research and HIV interventions. Soc Sci Med. 2000;51(5):749–58.
Binik YM, Mah K, Kiesler S. Ethical issues in conducting sex research on the Internet. J Sex Res. 1999;36(1):82–90.
Benotsch EG, Kalichman S, Cage M. Men who have met sex partners via the Internet: prevalence, predictors, and implications for HIV prevention. Arch Sex Behav. 2002;31(2):177–83.
Poon MK, Ho PT, Wong JP, Wong G, Lee R. Psychosocial Experiences of East and Southeast Asian men who use gay Internet chatrooms in Toronto: an implication for HIV/AIDS prevention. Ethn Health. 2005;10(2):145–67.
Cochran SD, Mays VM. Relation between psychiatric syndromes and behaviorally defined sexual orientation in a sample of the US population. Am J Epidemiol. 2000;151(5):516–23.
Klausner JD, Levine DK, Kent CK. Internet-based site-specific interventions for syphilis prevention among gay and bisexual men. AIDS Care. 2004;16(8):964–70.
Flicker S, Goldberg E, Read S, et al. HIV-positive youth’s perspectives on the Internet and e-health. J Med Internet Res. 2004;6(3):e32.
Goold PC, Ward M, Carlin EM. Can the Internet be used to improve sexual health awareness in web-wise young people? J Fam Plann Reprod Health Care. 2003;29(1):28–30.
Bowen AM, Horvath K, Williams ML. A randomized control trial of Internet-delivered HIV prevention targeting rural MSM. Health Educ Res. 2007;22(1):120–7.
Noar SM, Clark A, Cole C, Lustria ML. Review of interactive safer sex Web sites: practice and potential. Health Commun. 2006;20(3):233–41.
Acknowledgments
This study was supported by grants from the National Natural Science Foundation of China (30972548), the Ministry of Science and Technology of China (2008ZX10001-004, 2009ZX10004-903 and 2009DFB30420) and the National Institutes of Health (grants #R01AI078933). We would like to thank Ms. Meredith Bortz from Vanderbilt University for article assistance.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Qingchun Li, Yingjie Liu, Zhenhai Zhou contributed to this paper equally.
Rights and permissions
About this article
Cite this article
Li, Q., Liu, Y., Zhou, Z. et al. Online Sex-Seeking Behaviors Among Men Who have Sex with Men: Implications for Investigation and Intervention. AIDS Behav 16, 1690–1698 (2012). https://doi.org/10.1007/s10461-011-0005-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-011-0005-0