Abstract
Aims
To observe the alterations in functional magnetic resonance imaging parameters in normoalbuminuric type 2 diabetic patients undergoing SGLT2 inhibitor empagliflozin treatment and investigate the early tubular protective effects of the inhibitor.
Methods
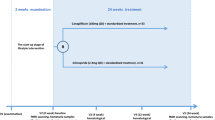
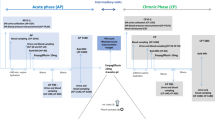
This study was performed in normoalbuminuric type 2 diabetes mellitus patients (UACR < 30 mg/g, eGFR ≥ 60 ml/min/1.73 m2). The patients were divided into the intervention group (empagliflozin) and the control group (27 cases each). The intervention group was treated with 10 mg/day empagliflozin tablets orally, while the control group had adjustments to their basic treatment stage. The patients were treated for 6 weeks.
Results
The baseline clinical data of the two groups were comparable (P˃0.05). The intervention group exhibited better improvements in blood lipid profiles and more significant reductions in blood uric acid levels compared to the control group (P < 0.05). The two groups had No significant difference in blood pressure changes (P˃0.05). Notably, the intervention group demonstrated a greater reduction in UACR and a more substantial decline in eGFR than the control group (P < 0.05). Regarding functional magnetic resonance imaging parameters, the MD value of the renal medulla region in the intervention group increased after treatment, while the MR2* value of the renal medulla region decreased (P < 0.05).
Conclusions
SGLT2 inhibitor empagliflozin can reduce UACR and eGFR levels in early type 2 diabetic patients with normal proteinuria. Moreover, empagliflozin therapy led to an increase in the MD value and a decrease in the MR2* value of the renal medulla, evidencing the early tubular protective effects of this therapy.






Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Levin A et al (2013) Kidney disease: improving global outcomes (KDIGO) CKD work group. KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl 3(1):1–150
McQueen RB et al (2017) Economic burden of comorbid chronic kidney disease and diabetes. J Med Econ 20(6):585–591
Sun H et al (2022) IDF diabetes atlas: global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract 183:109119
Hoogeveen EK (2022) The epidemiology of diabetic kidney disease. Kidney Dial 2(3):433–442
Duan J et al (2019) Prevalence and risk factors of chronic kidney disease and diabetic kidney disease in Chinese rural residents: a cross-sectional survey. Sci Rep 9(1):10408
Yang C et al (2020) CKD in China: evolving spectrum and public health implications. Am J Kidney Dis 76(2):258–264
Gao B et al (2014) Chinese cohort study of chronic kidney disease: design and methods. Chin Med J 127(11):2180–2185
Yu X, Yang X (2015) Peritoneal dialysis in China: meeting the challenge of chronic kidney failure. Am J Kidney Dis 65(1):147–151
Bennett WL et al (2011) Comparative effectiveness and safety of medications for type 2 diabetes: an update including new drugs and 2-drug combinations. Ann Intern Med 154(9):602–613
Gnudi L, Coward RJ, Long DA (2016) Diabetic nephropathy: perspective on novel molecular mechanisms. Trends Endocrinol Metab 27(11):820–830
Tsimihodimos V et al (2017) Antidiabetic drugs and the kidney. Curr Pharm Des 23(41):6310–6320
Yang W et al (2017) Efficacy and safety of dapagliflozin in Asian patients: a pooled analysis. J Diabet 9(8):787–799
Wanner C et al (2016) Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med 375(4):323–334
Wiviott SD et al (2019) Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med 380(4):347–357
Neal B, Perkovic V, Matthews DR (2017) Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 377(21):2099
Perkovic V et al (2019) Canagliflozin and renal outcomes in type 2 diabetes and nephropathy. N Engl J Med 380(24):2295–2306
Hegde NC et al (2023) Dose-dependent renoprotection efficacy of sglt2 inhibitors in type 2 diabetes: systematic review and network meta-analysis. Acta Diabetol 60(10):1311–1331
Gilbert RE (2017) Proximal tubulopathy: prime mover and key therapeutic target in diabetic kidney disease. Diabetes 66(4):791–800
Feng YZ et al (2018) Intravoxel incoherent motion (IVIM) at 3.0 T: evaluation of early renal function changes in type 2 diabetic patients. Abdom Radiol (NY) 43(10):2764–2773
Feng YZ et al (2020) Non-invasive assessment of early stage diabetic nephropathy by DTI and BOLD MRI. Br J Radiol 93(1105):20190562
[Clinical guidelines for prevention and treatment of type 2 diabetes mellitus in the elderly in China (2022 edition)]. Zhonghua Nei Ke Za Zhi, 61(1): 12–50.
Górriz JL et al (2015) Nephroprotection by hypoglycemic agents: do we have supporting data? J Clin Med 4(10):1866–1889
Zhang F et al (2022) Expert consensus on personalized initiation of glucose-lowering therapy in adults with newly diagnosed type 2 diabetes without clinical cardiovascular disease or chronic kidney disease. J Evid Based Med 15(2):168–179
Ma YC et al (2006) Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. J Am Soc Nephrol 17(10):2937–2944
Wei X et al (2022) Alterations of renal function in patients with diabetic kidney disease: a bold and DTI study. Comput Intell Neurosci 2022:6844102
Zhang Z et al (2023) The value of functional magnetic resonance imaging in the evaluation of diabetic kidney disease: a systematic review and meta-analysis. Front Endocrinol (Lausanne) 14:1226830
Heerspink HJ et al (2017) Canagliflozin slows progression of renal function decline independently of glycemic effects. J Am Soc Nephrol 28(1):368–375
Fine LG, Norman JT (2008) Chronic hypoxia as a mechanism of progression of chronic kidney diseases: from hypothesis to novel therapeutics. Kidney Int 74(7):867–872
Ndibalema AR et al (2020) Empagliflozin protects against proximal renal tubular cell injury induced by high glucose via regulation of hypoxia-inducible factor 1-alpha. Diabet Metab Syndr Obes 13:1953–1967
Laursen JC et al. (2021) Acute effects of dapagliflozin on renal oxygenation and perfusion in type 1 diabetes with albuminuria: a randomised, double-blind, placebo-controlled crossover trial. eClinicalMedicine 37
Acknowledgements
None.
Funding
This study was supported by the Medical Research Foundation of Guangdong Province (Grant Number: B2023376);Scientific research project of Guangdong Provincial Bureau of traditional Chinese Medicine (Grant Number: 20231083);Guangzhou Science and Technology Planning Project (Grant Number: 2023A04J1909).
Author information
Authors and Affiliations
Contributions
JL and XL conceived and designed the experiments. CZ, BZ, and YF contributed significantly to the experiments. CZ, BZ, YF, ZC, and XC helped with the experiments and arranging the data. XC and LF performed the data analyses. CZ and BZ wrote the draft manuscript. JL and XL critically revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there are no conflicts of interest.
Ethical approval
The study protocol was reviewed and approved by the Ethics Committee of the First Affiliated Hospital of **an University (approval no: JJ-202856-451). All patients agreed and signed informed consent.
Human accordance statement
All the authors confirm that all methods were carried out in accordance with relevant guidelines and regulations. Research involving human participants, human material, or human data, must have been performed in accordance with the Declaration of Helsinki.
Informed consent to participate
All the authors confirming that informed consent was obtained from all subjects and their legal guardians.
Consent for publication
Not applicable.
Additional information
This article belongs to the Topical Collection “Diabetic Nephropathy”, managed by Giuseppe Pugliese.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, C., Zhu, B., Feng, Y. et al. Assessing early tubular protective effects of SGLT2 inhibitor empagliflozin against type 2 diabetes mellitus using functional magnetic resonance imaging. Acta Diabetol 61, 473–483 (2024). https://doi.org/10.1007/s00592-023-02220-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-023-02220-x