Abstract
Purpose
Coronal tibiofemoral subluxation (CTFS) is considered a controversial and potential contraindication to unicompartmental knee arthroplasty (UKA) but is less discussed. The study aims to observe the CTFS in a cohort of patients before and after mobile-bearing UKA and to investigate the relationship between preoperative variables (preoperative CTFS and preoperative CTFS under valgus stress) and postoperative CTFS after mobile-bearing UKA.
Methods
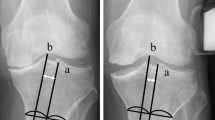
The study retrospectively analyzed 181 patients (224 knees) undergoing mobile-bearing UKA from September 1 2019 to December 31 2021. By using hip-to-ankle anterior–posterior (AP) standing radiographs and valgus stress force radiographs, preoperative CTFS, preoperative CTFS under valgus stress, and postoperative CTFS were measured. CTFS was defined as the distance between the tangent line to the outermost joint edge of the lateral condyle of the femur and the tangent line of the lateral tibial plateau. All patients were divided into two groups based on postoperative CTFS, group A (postoperative CTFS ≤ 5 mm) and group B (postoperative CTFS > 5 mm). The Student’s t-test, one-way ANOVA together with Tukey’s post hoc test, the chi-square test, the Fisher’s exact test, Pearson correlation analysis, simple and multiple linear regression, and univariate and multiple logistic regression were used in the analyses.
Results
The means ± standard deviations (SD) of preoperative CTFS, preoperative CTFS under valgus stress, and postoperative CTFS were 4.96 ± 1.82 mm, 3.06 ± 1.37 mm, and 3.19 ± 1.27 mm. The difference between preoperative CTFS and postoperative CTFS was statistically significant (p < 0.001). The preoperative CTFS (6.35 ± 1.34 mm) in Group B (n = 22) was significantly higher than that (4.81 ± 1.82 mm) in Group A (n = 202) (p < 0.001), so was the variable-preoperative CTFS under valgus stress (5.41 ± 1.00 mm (Group B) > 2.80 ± 1.14 mm (Group A), p < 0.001). In Pearson correlation analysis, there was a correlation between preoperative CTFS and postoperative CTFS (r = 0.493, p < 0.001), while the correlation between preoperative CTFS under valgus stress and postoperative CTFS was stronger (r = 0.842, p < 0.001). In multiple linear regression analysis, preoperative CTFS under valgus stress (β = 0.798, 95% confidence interval (CI) = 0.714–0.883, p < 0.001) was significantly correlated with postoperative CTFS. In multiple logistic regression analysis, preoperative CTFS under valgus stress (OR = 12.412, 95% CI = 4.757–32.384, and p < 0.001) was expressed as the risk factor of postoperative CTFS (> 5 mm).
Conclusion
Preoperative CTFS can be improved significantly after mobile-bearing UKA. In addition, postoperative CTFS is correlated with preoperative CTFS under valgus stress and a higher preoperative CTFS under valgus stress will increase the risk of higher postoperative CTFS (> 5 mm).
Level of evidence
Level III.



Similar content being viewed by others
Availability of data and materials
All of the data are available in contact with the correspondence author.
References
Glyn-Jones S, Palmer AJR, Agricola R, Price AJ, Vincent TL, Weinans H, Carr AJ (2015) Osteoarthritis. Lancet 386(9991):376–387. https://doi.org/10.1016/s0140-6736(14)60802-3
Salaffi F, Carotti M, Stancati A, Grassi W (2005) Health-related quality of life in older adults with symptomatic hip and knee osteoarthritis: a comparison with matched healthy controls. Aging Clin Exp Res 17(4):255–263. https://doi.org/10.1007/bf03324607
Vos T, Flaxman AD, Naghavi M et al (2012) Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380(9859):2163–2196. https://doi.org/10.1016/s0140-6736(12)61729-2
Seng CS, Ho DC, Chong HC, Chia SL, Chin PL, Lo NN, Yeo SJ (2017) Outcomes and survivorship of unicondylar knee arthroplasty in patients with severe deformity. Knee Surg Sports Traumatol Arthrosc 25(3):639–644. https://doi.org/10.1007/s00167-014-3464-9
Mortazavi SMJ, Vosoughi F (2022) Association of alignment variables, posteromedial tibial cartilage wear and anterior cruciate ligament insufficiency in participants with varus knee osteoarthritis: a cross-sectional study. Int Orthop. https://doi.org/10.1007/s00264-022-05358-5
Liddle AD, Judge A, Pandit H, Murray DW (2014) Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients: a study of data from the National Joint Registry for England and Wales. Lancet 384(9952):1437–1445. https://doi.org/10.1016/s0140-6736(14)60419-0
Ma J, Yan Y, Wang W, Wang B, Yue D, Guo W (2021) Lower early revision rates after uncemented Oxford Unicompartmental Knee Arthroplasty (UKA) than cemented Oxford UKA: A meta-analysis. Orthop Traumatol Surg Res 107(3):102802. https://doi.org/10.1016/j.otsr.2021.102802
Mohammad HR, Mellon S, Judge A, Dodd C, Murray D (2021) The effect of body mass index on the outcomes of cementless medial mobile-bearing unicompartmental knee replacements. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06549-0
Moore DM, Sheridan GA, Welch-Phillips A, O’Byrne JM, Kenny P (2021) Good mid- to long-term results of the cemented oxford phase 3 unicompartmental knee arthroplasty in a non-designer centre. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06665-x
Pongcharoen B, Timjang J (2020) The outcomes of mobile bearing unicompartmental knee arthroplasty and total knee arthroplasty on anteromedial osteoarthritis of the knee in the same patient. Arch Orthop Trauma Surg 140(11):1783–1790. https://doi.org/10.1007/s00402-020-03527-y
Crawford DA, Berend KR, Thienpont E (2020) Unicompartmental knee arthroplasty: US and Global Perspectives. Orthop Clin North Am 51(2):147–159. https://doi.org/10.1016/j.ocl.2019.11.010
Kozinn SC, Scott R (1989) Unicondylar knee arthroplasty. J Bone Joint Surg Am 71(1):145–150
Affatato S, Caputo D, Bordini B (2019) Does the body mass index influence the long-term survival of unicompartmental knee prostheses? Retrosp Multi Centre Study Int Orthop 43(6):1365–1370. https://doi.org/10.1007/s00264-018-4217-z
Greco NJ, Lombardi AV Jr, Price AJ, Berend ME, Berend KR (2018) Medial mobile-bearing unicompartmental knee arthroplasty in young patients aged less than or equal to 50 years. J Arthroplasty 33(8):2435–2439. https://doi.org/10.1016/j.arth.2018.03.069
Berend KR, Lombardi AV Jr, Morris MJ, Hurst JM, Kavolus JJ (2011) Does preoperative patellofemoral joint state affect medial unicompartmental arthroplasty survival? Orthopedics 34(9):e494-496. https://doi.org/10.3928/01477447-20110714-39
Crawford DA, Adams JB, Lombardi AV Jr, Berend KR (2019) Activity level does not affect survivorship of unicondylar knee arthroplasty at 5 year minimum follow-up. J Arthroplasty 34(7):1364–1368. https://doi.org/10.1016/j.arth.2019.03.038
Pandit H, Jenkins C, Gill HS, Smith G, Price AJ, Dodd CA, Murray DW (2011) Unnecessary contraindications for mobile-bearing unicompartmental knee replacement. J Bone Joint Surg Br 93(5):622–628. https://doi.org/10.1302/0301-620x.93b5.26214
Springer B, Waldstein W, Bechler U, Jungwirth-Weinberger A, Windhager R, Boettner F (2021) The functional status of the ACL in varus OA of the knee: The Association With Varus Deformity and Coronal Tibiofemoral Subluxation. J Arthroplasty 36(2):501–506. https://doi.org/10.1016/j.arth.2020.08.049
Greif DN, Epstein AL, Hodgens BH, Jose J, Baraga MG (2021) Current measurement strategies of coronal tibiofemoral subluxation: a systematic review of literature. AJR Am J Roentgenol 216(5):1183–1192. https://doi.org/10.2214/ajr.20.23503
Kamenaga T, Nakano N, Ishida K, Tsubosaka M, Kuroda Y, Hayashi S, Matsushita T, Niikura T, Kuroda R, Matsumoto T (2021) Preoperative uncorrectable tibiofemoral subluxation can worsen clinical outcomes after fixed-bearing unicompartmental knee arthroplasty: a retrospective analysis. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-04157-8
Kamenaga T, Hiranaka T, Hida Y, Nakano N, Kuroda Y, Tsubosaka M, Hayashi S, Kuroda R, Matsumoto T (2021) Lateral osteoarthritis progression is associated with a postoperative residual tibiofemoral subluxation in Oxford UKA. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06729-y
Berger RA, Della Valle CJ (2010) Unicompartmental knee arthroplasty: indications, techniques, and results. Instr Course Lect 59:47–56
Boettner F, Springer B, Windhager R, Waldstein W (2020) The tibial spine sign does not indicate cartilage damage in the central area of the distal lateral femoral condyle. Knee Surg Sports Traumatol Arthrosc 28(8):2592–2597. https://doi.org/10.1007/s00167-020-05881-1
Nam D, Khamaisy S, Gladnick BP, Paul S, Pearle AD (2013) Is tibiofemoral subluxation correctable in unicompartmental knee arthroplasty? J Arthroplasty 28(9):1575–1579. https://doi.org/10.1016/j.arth.2013.03.001
Kamenaga T, Takayama K, Ishida K, Hayashi S, Kuroda R, Matsumoto T (2020) Central implantation of the femoral component relative to the tibial insert improves clinical outcomes in fixed-bearing unicompartmental knee arthroplasty. J Arthroplasty 35(11):3108–3116. https://doi.org/10.1016/j.arth.2020.05.071
Kim YT, Choi JY, Lee JK, Lee YM, Kim JI (2019) Coronal tibiofemoral subluxation is a risk factor for postoperative overcorrection in high tibial osteotomy. Knee 26(4):832–837. https://doi.org/10.1016/j.knee.2019.05.011
Buyukkuscu MO, Misir A, Kirat A, Albayrak K, Sencan K, Camurcu IY, Gursu SS (2021) Tibiofemoral subluxation in the coronal plane does not affect WOMAC and KOOS after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 29(3):914–920. https://doi.org/10.1007/s00167-020-06047-9
** G, Wang HH, Li H, Zhang M (2022) Short-term outcomes of Oxford unicompartmental knee arthroplasty with coronal subluxation of the knee: a retrospective case-control study. J Orthop Traumatol 23(1):6. https://doi.org/10.1186/s10195-022-00626-x
Kang KT, Son J, Koh YG, Kwon OR, Kwon SK, Lee YJ, Park KK (2018) Effect of femoral component position on biomechanical outcomes of unicompartmental knee arthroplasty. Knee 25(3):491–498. https://doi.org/10.1016/j.knee.2018.03.003
Hazratwala K, O’Callaghan WB, Dhariwal S, Wilkinson MPR (2021) Wide variation in tibial slopes and trochlear angles in the arthritic knee: a CT evaluation of 4116 pre-operative knees. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06725-2
Gielis WP, Rayegan H, Arbabi V, Ahmadi Brooghani SY, Lindner C, Cootes TF, de Jong PA, Weinans H, Custers RJH (2020) Predicting the mechanical hip-knee-ankle angle accurately from standard knee radiographs: a cross-validation experiment in 100 patients. Acta Orthop 91(6):732–737. https://doi.org/10.1080/17453674.2020.1779516
Wang JH, Weinberg DS, Amakoutou K, Cooperman DR, Liu RW (2021) The distal femur trochlear groove appears to compensate for tibial deformity but not femoral deformity in an investigation of five-hundred and seventy-nine cadaveric skeletons. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03998-7
Murray D, Goodfellow J, O’Connor J, Dodd C (1999) Oxford Unicompartmental knee: manual of the surgical technique. Biomet UK Ltd, Bridgend, pp. 1–40
Schadler P, Kasparek M, Boettner F, Sgroi M, Faschingbauer M (2017) Coronal tibiofemoral subluxation is not an independent risk factor for total knee arthroplasty in patients with moderate to severe varus-osteoarthritis: data from the “Osteoarthritis Initiative.” Arch Orthop Trauma Surg 137(10):1423–1428. https://doi.org/10.1007/s00402-017-2777-9
Ogawa H, Matsumoto K, Akiyama H (2018) Coronal tibiofemoral subluxation is correlated to correction angle in medial opening wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 26(11):3482–3490. https://doi.org/10.1007/s00167-018-4948-9
Khamaisy S, Zuiderbaan HA, Thein R, Nawabi DH, Joskowicz L, Pearle AD (2014) Coronal tibiofemoral subluxation: a new measurement method. Knee 21(6):1069–1071. https://doi.org/10.1016/j.knee.2014.07.013
Khamaisy S, Zuiderbaan HA, Thein R, Gladnick BP, Pearle AD (2016) Coronal tibiofemoral subluxation in knee osteoarthritis. Skeletal Radiol 45(1):57–61. https://doi.org/10.1007/s00256-015-2244-z
Pandit H, Spiegelberg B, Clavé A, McGrath C, Liddle AD, Murray DW (2016) Aetiology of lateral progression of arthritis following Oxford medial unicompartmental knee replacement: a case-control study. Musculoskelet Surg 100(2):97–102. https://doi.org/10.1007/s12306-015-0394-8
Tashiro Y, Matsuda S, Okazaki K, Mizu-Uchi H, Kuwashima U, Iwamoto Y (2014) The coronal alignment after medial unicompartmental knee arthroplasty can be predicted: usefulness of full-length valgus stress radiography for evaluating correctability. Knee Surg Sports Traumatol Arthrosc 22(12):3142–3149. https://doi.org/10.1007/s00167-014-3248-2
Ishibashi K, Sasaki E, Otsuka H, Kazushige K, Yamamoto Y, Ishibashi Y (2020) Valgus correctability and meniscal extrusion were associated with alignment after unicompartmental knee arthroplasty. Clin Orthop Relat Res 478(7):1636–1644. https://doi.org/10.1097/corr.0000000000001260
Zhang Q, Yue J, Wang W, Chen Y, Zhao Q, Guo W (2018) FTFA change under valgus stress force radiography is useful for evaluating the correctability of intra-articular varus deformity in UKA. Arch Orthop Trauma Surg 138(7):1003–1009. https://doi.org/10.1007/s00402-018-2945-6
Costa CR, Johnson AJ, Mont MA, Bonutti PM (2011) Unicompartmental and total knee arthroplasty in the same patient. J Knee Surg 24(4):273–278. https://doi.org/10.1055/s-0031-1280970
Khamaisy S, Nam D, Thein R, Rivkin G, Liebergall M, Pearle A (2015) Limb alignment, subluxation, and bone density relationship in the osteoarthritic varus knee. J Knee Surg 28(3):207–212. https://doi.org/10.1055/s-0034-1376327
Funding
This study was funded by the Capital Health Research and Development of Special (grant number 2020-2-4067), National Natural Science Foundation of China (grant number 82072494, 81972130), and Elite Medical Professionals Project of China-Japan Friendship Hospital (NO.ZRJY2021-GG08).
Author information
Authors and Affiliations
Contributions
CQL, QDZ and WSG designed the study. CQL, JCG and XWS did the data collection. CQL, JCG and CH did the data analysis. CQL wrote the article. QDZ and WSG revised the article. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the institutional review board of China-Japan Friendship Hospital (approval number 2020–50-k28).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent to publish
All authors had consented to the submission of the article to the journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, C., Ge, J., Sun, X. et al. Coronal tibiofemoral subluxation under valgus stress force radiography is useful for evaluating postoperative coronal tibiofemoral subluxation in mobile-bearing UKA. Arch Orthop Trauma Surg 143, 4349–4361 (2023). https://doi.org/10.1007/s00402-022-04666-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04666-0