Abstract
Purpose
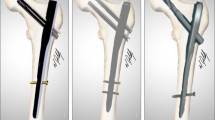
Intertrochanteric femoral fractures (IFF) are one of the most common traumatic conditions, but there are no established treatment methods for this condition due to implant failure and re-operation rates. The proximal femoral bionic nail (PFBN), which is a new design of the cephalomedullary nail, was developed by our team. The objective of this study was to assess the clinical and radiographic outcomes of PFBN in patients with unstable IFF.
Methods
From October 2020 to August 2021, 12 patients diagnosed with unstable IFF (31-A2, 3) were treated with PFBN at the Third Hospital of Hebei Medical University. We evaluated the clinical therapeutic effects of this treatment by measuring peri-operative indicators and post-operative complications. Clinical outcomes, specific radiographic parameters, and post-operative complications were collected and analyzed within the first post-operative year.
Results
The average age of the patients was 72.4 ± 16.1 years (five males and seven females). The mean operation time was 90.4 ± 16.0 min, whereas the operation time of 31-A2 fractures (83.1 ± 12.2 min) was shorter than that of 31-A3 fractures (105.0 ± 12.9 min) (p < 0.05). The blood loss was 175 ml (range: 50 to 500 ml), and the length of hospitalization was 10.0 ± 1.9 days. The prognosis evaluation was assessed at three, six and 12 months after the operation; for these time points, the Harris hip scores were 69.6 ± 4.1, 77.8 ± 3.8, and 82.6 ± 4.6, respectively, and the Parker-Palmer scores were 5.3 (5.0, 7.0), 6.3 (5.3, 7.0), and 7.8 (7.0, 8.0), respectively.
Conclusion
PFBN has shown advantages in the treatment of unstable IFF (particularly in geriatric patients) and possesses both stability and safety. This innovative method may provide a new option for treating unstable IFFs.






Similar content being viewed by others
Data availability
All data and materials were available for request.
Code availability
Not applicable.
References
Lambers A, Rieger B, Kop A et al (2019) Implant fracture analysis of the TFNA proximal femoral nail. J Bone Joint Surg Am 101:804–811. https://doi.org/10.2106/JBJS.18.00997
Radaideh AM, Qudah HA, Audat ZA et al (2018) Functional and radiological results of proximal femoral nail antirotation (PFNA) osteosynthesis in the treatment of unstable pertrochanteric fractures. J Clin Med 7(4):78. https://doi.org/10.3390/jcm7040078
Pincus D, Desai SJ, Wasserstein D et al (2017) Outcomes of after-hours hip fracture surgery. J Bone Joint Surg Am 99:914–922. https://doi.org/10.2106/jbjs.16.00788
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 37:691–697. https://doi.org/10.1016/j.injury.2006.04.130
Butler M, Forte ML, Joglekar SB et al (2011) Evidence summary: a systematic review of surgical treatments for geriatric hip fractures. J Bone Joint Surg Am 93:1104–1115. https://doi.org/10.2106/jbjs.J.00296
Roche JJ, Wenn RT, Sahota O et al (2005) Effect of comorbidities and postoperative complications on mortality after hip fracture in elderly people: prospective observational cohort study. BMJ 331:1374. https://doi.org/10.1136/bmj.38643.663843.55
Palm H, Jacobsen S, Sonne-Holm S et al (2007) Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation. J Bone Joint Surg Am 89:470–475. https://doi.org/10.2106/jbjs.F.00679
Müller F, Doblinger M, Kottmann T et al (2020) PFNA and DHS for AO/OTA 31–A2 fractures: radiographic measurements, morbidity and mortality. Eur J Trauma Emerg Surg 46:947–953. https://doi.org/10.1007/s00068-019-01251-w
Lewis SR, Macey R, Gill JR et al (2022) Cephalomedullary nails versus extramedullary implants for extracapsular hip fractures in older adults. Cochrane Database Syst Rev 1:Cd000093. https://doi.org/10.1002/14651858.CD000093.pub6
Bartoníček J, Rammelt S (2014) The history of internal fixation of proximal femur fractures Ernst Pohl-the genius behind. Int Orthop 38:2421–2426. https://doi.org/10.1007/s00264-014-2320-3
Zhu Q, Xu X, Yang X et al (2017) Intramedullary nails versus sliding hip screws for AO/OTA 31–A2 trochanteric fractures in adults: a meta-analysis. Int J Surg 43:67–74. https://doi.org/10.1016/j.ijsu.2017.05.042
Kashigar A, Vincent A, Gunton MJ et al (2014) Predictors of failure for cephalomedullary nailing of proximal femoral fractures. Bone Joint J 96-b:1029–1034. https://doi.org/10.1302/0301-620x.96b8.33644
Zhang W, Antony Xavier RP, Decruz J et al (2021) Risk factors for mechanical failure of intertrochanteric fractures after fixation with proximal femoral nail antirotation (PFNA II): a study in a Southeast Asian population. Arch Orthop Trauma Surg 141:569–575. https://doi.org/10.1007/s00402-020-03399-2
Ding K, Zhu Y, Li Y et al (2022) Triangular support intramedullary nail: a new internal fixation innovation for treating intertrochanteric fracture and its finite element analysis. Injury 53:1796–1804. https://doi.org/10.1016/j.injury.2022.03.032
Wang H, Yang W, Ding K et al (2022) Biomechanical study on the stability and strain conduction of intertrochanteric fracture fixed with proximal femoral nail antirotation versus triangular supporting intramedullary nail. Int Orthop 46:341–350. https://doi.org/10.1007/s00264-021-05250-8
Zhang L, Shen J, Chen S et al (2016) Treatment of unstable intertrochanteric femoral fractures with locking gamma nail (LGN): a retrospective cohort study. Int J Surg 26:12–17. https://doi.org/10.1016/j.ijsu.2015.12.064
Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am 51:737–755. https://doi.org/10.2106/00004623-196951040-00012
Parker MJ, Palmer CR (1993) A new mobility score for predicting mortality after hip fracture. J Bone Joint Surg Br 75:797–798. https://doi.org/10.1302/0301-620x.75b5.8376443
Barton TM, Gleeson R, Topliss C et al (2010) A comparison of the long gamma nail with the sliding hip screw for the treatment of AO/OTA 31–A2 fractures of the proximal part of the femur: a prospective randomized trial. J Bone Joint Surg Am 92:792–798. https://doi.org/10.2106/jbjs.I.00508
Vaquero J, Munoz J, Prat S et al (2012) Proximal femoral nail antirotation versus Gamma3 nail for intramedullary nailing of unstable trochanteric fractures. A randomised comparative study. Injury 43(Suppl 2):S47-54. https://doi.org/10.1016/s0020-1383(13)70179-7
Mereddy P, Kamath S, Ramakrishnan M et al (2009) The AO/ASIF proximal femoral nail antirotation (PFNA): a new design for the treatment of unstable proximal femoral fractures. Injury 40:428–432. https://doi.org/10.1016/j.injury.2008.10.014
Pu JS, Liu L, Wang GL et al (2009) Results of the proximal femoral nail anti-rotation (PFNA) in elderly Chinese patients. Int Orthop 33:1441–1444. https://doi.org/10.1007/s00264-009-0776-3
Cai L, Wang T, Di L et al (2016) Comparison of intramedullary and extramedullary fixation of stable intertrochanteric fractures in the elderly: a prospective randomised controlled trial exploring hidden perioperative blood loss. BMC Musculoskelet Disord 17:475. https://doi.org/10.1186/s12891-016-1333-z
Seyhan M, Turkmen I, Unay K et al (2015) Do PFNA devices and Intertan nails both have the same effects in the treatment of trochanteric fractures? A prospective clinical study. J Orthop Sci 20:1053–1061. https://doi.org/10.1007/s00776-015-0750-4
Kumar P, Rajnish RK, Sharma S et al (2020) Proximal femoral nailing is superior to hemiarthroplasty in AO/OTA A2 and A3 intertrochanteric femur fractures in the elderly: a systematic literature review and meta-analysis. Int Orthop 44:623–633. https://doi.org/10.1007/s00264-019-04351-9
Bannister GC, Gibson AG, Ackroyd CE et al (1990) The fixation and prognosis of trochanteric fractures. A randomized prospective controlled trial. Clin Orthop Relat Res 254:242–246. https://doi.org/10.1097/00003086-199005000-00036
Haidukewych GJ, Israel TA, Berry DJ (2001) Reverse obliquity fractures of the intertrochanteric region of the femur. J Bone Joint Surg Am 83:643–650. https://doi.org/10.2106/00004623-200105000-00001
Ramakrishnan M, Prasad SS, Parkinson RW et al (2004) Management of subtrochanteric femoral fractures and metastases using long proximal femoral nail. Injury 35:184–190. https://doi.org/10.1016/s0020-1383(03)00101-3
Al-yassari G, Langstaff RJ, Jones JW et al (2002) The AO/ASIF proximal femoral nail (PFN) for the treatment of unstable trochanteric femoral fracture. Injury 33:395–399. https://doi.org/10.1016/s0020-1383(02)00008-6
Macheras GA, Koutsostathis SD, Galanakos S et al (2012) Does PFNA II avoid lateral cortex im**ement for unstable peritrochanteric fractures? Clin Orthop Relat Res 470:3067–3076. https://doi.org/10.1007/s11999-012-2445-x
Knobe M, Drescher W, Heussen N et al (2012) Is helical blade nailing superior to locked minimally invasive plating in unstable pertrochanteric fractures? Clin Orthop Relat Res 470:2302–2312. https://doi.org/10.1007/s11999-012-2268-9
Nie S, Li M, Ji H et al (2020) Biomechanical comparison of medial sustainable nail and proximal femoral nail antirotation in the treatment of an unstable intertrochanteric fracture. Bone Joint Res 9:840–847. https://doi.org/10.1302/2046-3758.912.BJR-2020-0284.R1
Rencken ML, Chesnut CH 3rd, Drinkwater BL (1996) Bone density at multiple skeletal sites in amenorrheic athletes. JAMA 276:238–240
Amin S, Zhang Y, Sawin CT et al (2000) Association of hypogonadism and estradiol levels with bone mineral density in elderly men from the Framingham study. Ann Intern Med 133:951–963. https://doi.org/10.7326/0003-4819-133-12-200012190-00010
Gallagher CA, Jones CW, Kimmel L et al (2019) Osteoarthritis is associated with increased failure of proximal femoral fracture fixation. Int Orthop 43:1223–1230. https://doi.org/10.1007/s00264-018-4014-8
Funding
This study was supported by Hebei Province Fund for Distinguished Young Scholars (Grant NO. H2021206329).
Author information
Authors and Affiliations
Contributions
Haiyue Zhao: conception design and original manuscript writing. **angtian Deng: draft modification and article revision. Weijian Liu: data analysis and curation. Wei Chen: investigation and resources. Lei Wang and Yiran Zhang: data collection. Zhongzheng Wang and Yuchuan Wang: resources; **aodong Lian: resource. Zhiyong Hou: validation. Qi Zhang: project supervision. Yingze Zhang: data curation and project administration. All the authors have reached an agreement on the content of this manuscript.
Corresponding authors
Ethics declarations
Ethics approval
This study conforms to the provisions of the Declaration of Helsinki and has been approved by the Ethics Committee of the Third Hospital of Hebei Medical University (2021–059-1).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The authors affirm that participants provided informed consent for the publication of the images in Figs. 5 and 6.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhao, H., Deng, X., Liu, W. et al. Proximal femoral bionic nail (PFBN)—an innovative surgical method for unstable femoral intertrochanteric fractures. International Orthopaedics (SICOT) 47, 1089–1099 (2023). https://doi.org/10.1007/s00264-023-05696-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05696-y