Abstract
Purpose
Patients with papillary thyroid carcinoma (PTC) frequently present a relatively poor prognosis when they coexist with cervical lymph node metastasis (LNM). Moreover, it remains controversial whether prophylactic lymph node dissection (LND) should be performed for patients without clinically lymph node metastasis. Thus, we hereby develop a nomogram for predicting the cervical LNM (including central and lateral LNM) in patients with PTC.
Methods
We retrospectively reviewed the clinical characteristics of adult patients with PTC in the surveillance, epidemiology, and end results (SEER) database between 2010 and 2015 and in our Department of Breast and Thyroid Surgery in the Second Affiliated Hospital of Chongqing Medical University between 2019 and 2020.
Result
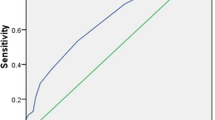
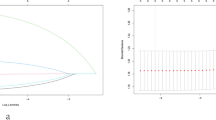
A total of 21,972 patients in the SEER database and 747 patients in our department who met the inclusion criteria were enrolled in this study. Ultimately, six clinical features including age, gender, race, extrathyroidal invasion, multifocality, and tumor size were identified to be associated with cervical LNM in patients with PTC, which were screened to develop a nomogram. This model had satisfied discrimination with a concordance index (C-index) of 0.733, supported by both internal and external validation with a C-index of 0.731 and 0.716, respectively. A decision curve analysis was subsequently made to evaluate the feasibility of this nomogram for predicting cervical LNM. Besides, a positive correlation between nomogram score and the average number of lymph node metastases was observed in all groups.
Conclusion
This visualized multipopulational-based nomogram model was successfully established. We determined that various clinical characteristics were significantly associated with cervical LNM, which would be better hel** clinicians make individualized clinical decisions for PTC patients.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
The software application generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Wang J, Yu F, Shang Y, ** Z, Liu L (2020) Thyroid cancer: incidence and mortality trends in China, 2005–2015. Endocrine 68(1):163–173. https://doi.org/10.1007/s12020-020-02207-6
Kim J, Gosnell JE, Roman SA (2020) Geographic influences in the global rise of thyroid cancer. Nat Rev Endocrinol 16(1):17–29. https://doi.org/10.1038/s41574-019-0263-x
Gao M, Ge M, Ji Q, Cheng R, Lu H, Guan H, Gao L, Guo Z, Huang T, Huang X, Li X, Lin Y, Liu Q, Ni X, Pan Y, Qin J, Shan Z, Sun H, Wang X, Xu Z, Yu Y, Zhao D, Zhang N, Zhang S, Zheng Y, Zhu J, Li D, Zheng X, Chinese Association Of Thyroid Oncology Cato Chinese Anti-Cancer A (2017) 2016 Chinese expert consensus and guidelines for the diagnosis and treatment of papillary thyroid microcarcinoma. Cancer Biol Med 14(3):203–211. https://doi.org/10.20892/j.issn.2095-3941.2017.0051
Moo TA, McGill J, Allendorf J, Lee J, Fahey T 3rd, Zarnegar R (2010) Impact of prophylactic central neck lymph node dissection on early recurrence in papillary thyroid carcinoma. World J Surg 34(6):1187–1191. https://doi.org/10.1007/s00268-010-0418-3
Lee YS, Kim SW, Kim SW, Kim SK, Kang HS, Lee ES, Chung KW (2007) Extent of routine central lymph node dissection with small papillary thyroid carcinoma. World J Surg 31(10):1954–1959. https://doi.org/10.1007/s00268-007-9171-7
Shirley LA, Jones NB, Phay JE (2017) The role of central neck lymph node dissection in the management of papillary thyroid cancer. Front Oncol 7:122. https://doi.org/10.3389/fonc.2017.00122
Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, Pacini F, Randolph GW, Sawka AM, Schlumberger M, Schuff KG, Sherman SI, Sosa JA, Steward DL, Tuttle RM, Wartofsky L (2016) 2015 American Thyroid Association Management Guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American Thyroid Association Guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26(1):1–133. https://doi.org/10.1089/thy.2015.0020
Cho SJ, Suh CH, Baek JH, Chung SR, Choi YJ, Chung KW, Shong YK, Lee JH (2019) Active surveillance for small papillary thyroid cancer: a systematic review and meta-analysis. Thyroid 29(10):1399–1408. https://doi.org/10.1089/thy.2019.0159
Sugitani I, Ito Y, Takeuchi D, Nakayama H, Masaki C, Shindo H, Teshima M, Horiguchi K, Yoshida Y, Kanai T, Hirokawa M, Hames KY, Tabei I, Miyauchi A (2020) Indications and strategy for active surveillance of adult low-risk papillary thyroid microcarcinoma: consensus statements from the Japan Association of Endocrine Surgery task force on management for papillary thyroid microcarcinoma. Thyroid. https://doi.org/10.1089/thy.2020.0330
Zhou SC, Liu TT, Zhou J, Huang YX, Guo Y, Yu JH, Wang YY, Chang C (2020) An ultrasound radiomics Nomogram for preoperative prediction of central neck lymph node metastasis in papillary thyroid carcinoma. Front Oncol 10:1591. https://doi.org/10.3389/fonc.2020.01591
Tian X, Song Q, **e F, Ren L, Zhang Y, Tang J, Zhang Y, ** Z, Zhu Y, Zhang M, Luo Y (2020) Papillary thyroid carcinoma: an ultrasound-based nomogram improves the prediction of lymph node metastases in the central compartment. Eur Radiol 30(11):5881–5893. https://doi.org/10.1007/s00330-020-06906-6
Dou Y, Chen Y, Hu D, **ong W, **ao Q, Su X (2020) Development and validation of web-based nomograms for predicting lateral lymph node metastasis in patients with papillary thyroid carcinoma. Gland Surg 9(2):172–182. https://doi.org/10.21037/gs.2020.01.11
Thompson AM, Turner RM, Hayen A, Aniss A, Jalaty S, Learoyd DL, Sidhu S, Delbridge L, Yeh MW, Clifton-Bligh R, Sywak M (2014) A preoperative nomogram for the prediction of ipsilateral central compartment lymph node metastases in papillary thyroid cancer. Thyroid 24(4):675–682. https://doi.org/10.1089/thy.2013.0224
Song M, Huang Z, Wang S, Huang J, Shi H, Liu Y, Huang Y, Yin Y, Wu Z (2020) Predictive factors of lateral lymph node metastasis in conventional papillary thyroid carcinoma. Gland Surg 9(4):1000–1007. https://doi.org/10.21037/gs-20-482
Huang C, Cong S, Liang T, Feng Z, Gan K, Zhou R, Guo Y, Luo S, Liang K, Wang Q (2020) Development and validation of an ultrasound-based nomogram for preoperative prediction of cervical central lymph node metastasis in papillary thyroid carcinoma. Gland Surg 9(4):956–967. https://doi.org/10.21037/gs-20-75
Yang Z, Heng Y, Lin J, Lu C, Yu D, Tao L, Cai W (2020) Nomogram for predicting central lymph node metastasis in papillary thyroid cancer: a retrospective cohort study of two clinical centers. Cancer Res Treat 52(4):1010–1018. https://doi.org/10.4143/crt.2020.254
Tuttle RM, Haugen B, Perrier ND (2017) Updated American Joint Committee on cancer/tumor-node-metastasis staging system for differentiated and anaplastic thyroid cancer (Eighth Edition): what changed and why? Thyroid 27(6):751–756. https://doi.org/10.1089/thy.2017.0102
Sasaki T, Miyauchi A, Ito Y, Kudo T, Kanemura N, Sano T, Kawano S, Yamamoto M, Fujishima M, Masuoka H, Higashiyama T, Kihara M, Miya A (2020) Marked decrease over time in conversion surgery after active surveillance of low-risk papillary thyroid microcarcinoma. Thyroid. https://doi.org/10.1089/thy.2020.0319
Ramundo V, Sponziello M, Falcone R, Verrienti A, Filetti S, Durante C, Grani G (2020) Low-risk papillary thyroid microcarcinoma: optimal management toward a more conservative approach. J Surg Oncol 121(6):958–963. https://doi.org/10.1002/jso.25848
Calò PG, Lombardi CP, Podda F, Sessa L, Santini L, Conzo G (2017) Role of prophylactic central neck dissection in clinically node-negative differentiated thyroid cancer: assessment of the risk of regional recurrence. Updates Surg 69(2):241–248. https://doi.org/10.1007/s13304-017-0438-8
Zhao W, He L, Zhu J, Su A (2020) A nomogram model based on the preoperative clinical characteristics of papillary thyroid carcinoma with Hashimoto’s thyroiditis to predict central lymph node metastasis. Clin Endocrinol (Oxf). https://doi.org/10.1111/cen.14302
Kim SK, Chai YJ, Park I, Woo JW, Lee JH, Lee KE, Choe JH, Kim JH, Kim JS (2017) Nomogram for predicting central node metastasis in papillary thyroid carcinoma. J Surg Oncol 115(3):266–272. https://doi.org/10.1002/jso.24512
Zhou B, Qin J (2020) High-risk factors for lymph node metastasis in contralateral central compartment in unilateral papillary thyroid carcinoma (cT1N0). Eur J Surg Oncol. https://doi.org/10.1016/j.ejso.2020.10.018
Zhao L, Sun X, Luo Y, Wang F, Lyu Z (2020) Clinical and pathologic predictors of lymph node metastasis in papillary thyroid microcarcinomas. Ann Diagn Pathol 49:151647. https://doi.org/10.1016/j.anndiagpath.2020.151647
Mao J, Zhang Q, Zhang H, Zheng K, Wang R, Wang G (2020) Risk factors for lymph node metastasis in papillary thyroid carcinoma: a systematic review and meta-analysis. Front Endocrinol (Lausanne) 11:265. https://doi.org/10.3389/fendo.2020.00265
Yan B, Hou Y, Chen D, He J, Jiang Y (2018) Risk factors for contralateral central lymph node metastasis in unilateral cN0 papillary thyroid carcinoma: a meta-analysis. Int J Surg 59:90–98. https://doi.org/10.1016/j.ijsu.2018.09.004
Ma B, Wang Y, Yang S, Ji Q (2016) Predictive factors for central lymph node metastasis in patients with cN0 papillary thyroid carcinoma: a systematic review and meta-analysis. Int J Surg 28:153–161. https://doi.org/10.1016/j.ijsu.2016.02.093
Zhu M, Zheng W, **ang Y, Gu J, Wang K, Shang J (2020) The relationship between central lymph node metastasis and the distance from tumor to thyroid capsule in papillary thyroid microcarcinoma without capsule invasion. Gland surgery 9(3):727–736. https://doi.org/10.21037/gs-20-478
Acknowledgements
None.
Funding
None.
Author information
Authors and Affiliations
Contributions
(I) Conception and design: YM, YF; (II) Administrative support: XW, GY; (III) Provision of study materials or patients: YF, HC, YM; (IV) Collection and assembly of data: YM, KX; (V) Data analysis and interpretation: YM, YF; (VI) Manuscript writing: All authors.; (VII) Final approval of manuscript: All authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethics approval
Ethical approval was waived by the local Ethics Committee of the Chongqing Medical University in view of the retrospective nature of the study and all the procedures being performed were part of the routine care.
Informed consent
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Feng, Y., Min, Y., Chen, H. et al. Construction and validation of a nomogram for predicting cervical lymph node metastasis in classic papillary thyroid carcinoma. J Endocrinol Invest 44, 2203–2211 (2021). https://doi.org/10.1007/s40618-021-01524-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-021-01524-5