Abstract
Background
Anterior cruciate ligament (ACL) injury is one of the most common injuries in sports, and the injury mechanisms are not completely clear. Bone bruises seen on magnetic resonance imaging (MRI) following ACL injuries may provide significant information for determining ACL injury mechanisms.
Objective
The aim was to determine ACL injury mechanisms through an evaluation of locations of bone bruises associated with ACL injury.
Methods
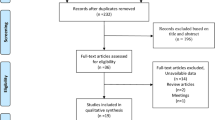
A search for related articles in PubMed and the EBSCO Sport Database was performed using selected search strings from inception to August 6, 2018. Original studies with specified bone bruise locations identified using MRI technology were reviewed.
Results
A total of 12 studies with 589 patients were selected for review. A total of 471 bone bruises in the lateral tibial plateau were reported. Of these bone bruises, 409 (87%) occurred in the posterior section. A total of 242 bone bruises in the medial tibial plateau were reported. Of these bone bruises, 208 (86%) occurred in the posterior section. A total of 266 bone bruises in the lateral femoral condyle were reported. Of these bone bruises, 65 (25%) and 184 (69%) occurred in the anterior and central sections, respectively. A total of 105 bone bruises in the medial femoral condyle were reported. Of these bone bruises, 49 (47%) and 41 (39%) occurred in the anterior and central sections, respectively.
Conclusions
Bone bruise location patterns indicate that tibial anterior translation relative to the femur was a primary injury mechanism in the majority of ACL injuries selected in this review, and that the maximal knee valgus apparently occurred after tibial anterior translation sufficient to injure the ACL. Bone bruise location patterns also indicate knee hyper-extension as another mechanism of non-contact ACL injury.

Similar content being viewed by others
References
Nicolini AP, de Carvalho RT, Matsuda MM, Sayum JF, Cohen M. Common injuries in athletes’ knee: experience of a specialized center. Acta Ortop Bras. 2014;22(3):127–31. https://doi.org/10.1590/1413-78522014220300475.
Mather RC, Koenig L, Kocher MS, Dall TM, Gallo P, Scott DJ, et al. Societal and economic impact of anterior cruciate ligament tears. J Bone Joint Surg Am. 2013;95(19):1751–9. https://doi.org/10.2106/JBJS.L.01705.
Lohmander LS, Ostenberg A, Englund M, Roos H. High prevalence of knee osteoarthritis, pain, and functional limitations in female soccer players twelve years after anterior cruciate ligament injury. Arthritis Rheum. 2004;50(10):3145–52. https://doi.org/10.1002/art.20589.
Lohmander LS, Roos EM. Clinical update: treating osteoarthritis. Lancet. 2007;370(9605):2082–4. https://doi.org/10.1016/S0140-6736(07)61879-0.
Griffin LY, Agel J, Albohm MJ, Arendt EA, Dick RW, Garrett WE, et al. Noncontact anterior cruciate ligament injuries: risk factors and prevention strategies. J Am Acad Orthop Surg. 2000;8(3):141–50.
Griffin LY, Albohm MJ, Arendt EA, Bahr R, Beynnon BD, DeMaio M, et al. Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January 2005. Am J Sports Med. 2006;34(9):1512–32. https://doi.org/10.1177/0363546506286866.
Sutton KM, Bullock JM. Anterior cruciate ligament rupture: differences between males and females. J Am Acad Orthop Surg. 2013;21(1):41–50. https://doi.org/10.5435/JAAOS-21-01-41.
Agel J, Arendt EA, Bershadsky B. Anterior cruciate ligament injury in national collegiate athletic association basketball and soccer: a 13-year review. Am J Sports Med. 2005;33(4):524–30. https://doi.org/10.1177/0363546504269937.
Hootman JM, Dick R, Agel J. Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives. J Athl Train. 2007;42(2):311–9.
Dai B, Herman D, Liu H, Garrett WE, Yu B. Prevention of ACL injury, part I: injury characteristics, risk factors, and loading mechanism. Res Sports Med. 2012;20(3–4):180–97. https://doi.org/10.1080/15438627.2012.680990.
Mink JH, Deutsch AL. Occult cartilage and bone injuries of the knee: detection, classification, and assessment with MR imaging. Radiology. 1989;170(3):823–9.
Speer KP, Spritzer CE, Bassett FH 3rd, Feagin JA Jr, Garrett WE Jr. Osseous injury associated with acute tears of the anterior cruciate ligament. Am J Sports Med. 1992;20(4):382–9. https://doi.org/10.1177/036354659202000403.
Vellet AD, Marks PH, Fowler PJ, Munro TG. Occult posttraumatic osteochondral lesions of the knee: prevalence, classification, and short-term sequelae evaluated with MR imaging. Radiology. 1991;178(1):271–6.
Lynch TC, Crues JV 3rd, Morgan FW, Sheehan WE, Harter LP, Ryu R. Bone abnormalities of the knee: prevalence and significance at MR imaging. Radiology. 1989;171(3):761–6.
Papalia R, Torre G, Vasta S, Zampogna B, Pedersen DR, Denaro V, et al. Bone bruises in anterior cruciate ligament injured knee and long-term outcomes. A review of the evidence. Open Access J Sports Med. 2015;6:37–48. https://doi.org/10.2147/oajsm.s75345.
Sanders TG, Medynski MA, Feller JF, Lawhorn KW. Bone contusion patterns of the knee at MR imaging: footprint of the mechanism of injury. Radiographics. 2000;20(1):S135–51.
Bisson LJ, Kluczynski MA, Hagstrom LS, Marzo JM. A prospective study of the association between bone contusion and intra-articular injuries associated with acute anterior cruciate ligament tear. Am J Sports Med. 2013;41(8):1801–7.
Chin YC, Wijaya R, Chong LR, Chang HC, Lee YHD. Bone bruise patterns in knee injuries: where are they found? Eur J Orthop Surg Traumatol. 2014;24(8):1481–7. https://doi.org/10.1007/s00590-013-1319-6.
Westermann RW, Wolf BR, Wahl CJ. Does lateral knee geometry influence bone bruise patterns after anterior cruciate ligament injury? A report of two cases. Iowa Orthop J. 2013;33:217–20.
Wittstein J, Vinson E, Garrett W. Comparison between sexes of bone contusions and meniscal tear patterns in noncontact anterior cruciate ligament injuries. Am J Sports Med. 2014;42(6):1401–7.
Filardo G, Kon E, Tentoni F, Andriolo L, Di Martino A, Busacca M, et al. Anterior cruciate ligament injury: post-traumatic bone marrow oedema correlates with long-term prognosis. Int Orthop. 2016;40(1):183–90. https://doi.org/10.1007/s00264-015-2672-3.
Driban JB, Lohmander S, Frobell RB. Posttraumatic bone marrow lesion volume and knee pain within 4 weeks after anterior cruciate ligament injury. J Athl Training. 2017;52(6):575–80.
Lattermann C, Jacobs CA, Reinke EK, Scaramuzza EA, Huston LJ, Dunn WR, et al. Are bone bruise characteristics and articular cartilage pathology associated with inferior outcomes 2 and 6 years after anterior cruciate ligament reconstruction? Cartilage. 2017;8(2):139–45. https://doi.org/10.1177/1947603516653209.
Temponi EF, de Carvalho Júnior LH, Saithna A, Thaunat M, Sonnery-Cottet B. Incidence and MRI characterization of the spectrum of posterolateral corner injuries occurring in association with ACL rupture. Skeletal Radiol. 2017;46(8):1063–70. https://doi.org/10.1007/s00256-017-2649-y.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6(7):e1000100. https://doi.org/10.1371/journal.pmed.1000100.
Burns PB, Rohrich RJ, Chung KC. The levels of evidence and their role in evidence-based medicine. Plast Reconstr Surg. 2011;128(1):305–10. https://doi.org/10.1097/PRS.0b013e318219c171.
Graf BK, Cook DA, De Smet AA, Keene JS. “Bone bruises” on magnetic resonance imaging evaluation of anterior cruciate ligament injuries. Am J Sports Med. 1993;21(2):220–3. https://doi.org/10.1177/036354659302100210.
Speer KP, Warren RF, Wickiewicz TL, Horowitz L, Henderson L. Observations on the injury mechanism of anterior cruciate ligament tears in skiers. Am J Sports Med. 1995;23(1):77–81. https://doi.org/10.1177/036354659502300113.
Viskontas DG, Giuffre BM, Duggal N, Graham D, Parker D, Coolican M. Bone bruises associated with ACL rupture: correlation with injury mechanism. Am J Sports Med. 2008;36(5):927–33. https://doi.org/10.1177/0363546508314791.
Yoon KH, Jae Ho Y, Kang-Il K. Bone contusion and associated meniscal and medial collateral ligament injury in patients with anterior cruciate ligament rupture. J Bone Joint Surg Am. 2011;93(16):1510–8. https://doi.org/10.2106/JBJS.J.01320.
Berger N, Andreisek G, Karer AT, Bouaicha S, Naraghi A, Manoliu A, et al. Association between traumatic bone marrow abnormalities of the knee, the trauma mechanism and associated soft-tissue knee injuries. Eur Radiol. 2017;27(1):393–403. https://doi.org/10.1007/s00330-016-4339-x.
Geeslin AG, LaPrade RF. Location of bone bruises and other osseous injuries associated with acute grade III isolated and combined posterolateral knee injuries. Am J Sports Med. 2010;38(12):2502–8. https://doi.org/10.1177/0363546510376232.
Ali AM, Pillai JK, Gulati V, Gibbons CER, Roberton BJ. Hyperextension injuries of the knee: do patterns of bone bruising predict soft tissue injury? Skeletal Radiol. 2018;47(2):173–9. https://doi.org/10.1007/s00256-017-2754-y.
Fayad LM, Parellada JA, Parker L, Schweitzer ME. MR imaging of anterior cruciate ligament tears: is there a gender gap? Skeletal Radiol. 2003;32(11):639–46. https://doi.org/10.1007/s00256-003-0694-1.
Kaplan PA, Gehl RH, Dussault RG, Anderson MW, Diduch DR. Bone contusions of the posterior lip of the medial tibial plateau (contrecoup injury) and associated internal derangements of the knee at MR imaging. Radiology. 1999;211(3):747–53.
Zeiss J, Paley K, Murray K, Saddemi SR. Comparison of bone contusion seen by MRI in partial and complete tears of the anterior cruciate ligament. J Comput Assist Tomogr. 1995;19(5):773–6. https://doi.org/10.1097/00004728-199509000-00014.
Lee K, Siegel MJ, Lau DM, Hildebolt CF, Matava MJ. Anterior cruciate ligament tears: MR imaging-based diagnosis in a pediatric population. Radiology. 1999;213(3):697–704.
Snearly WN, Kaplan PA, Dussault RG. Lateral-compartment bone contusions in adolescents with intact anterior cruciate ligaments. Radiology. 1996;198(1):205–8.
Kim SY, Spritzer CE, Utturkar GM, Toth AP, Garrett WE, DeFrate LE. Knee kinematics during noncontact anterior cruciate ligament injury as determined from bone bruise location. Am J Sports Med. 2015;43(10):2515–21. https://doi.org/10.1177/0363546515594446.
DeMorat G, Weinhold P, Blackburn T, Chudik S, Garrett W. Aggressive quadriceps loading can induce noncontact anterior cruciate ligament injury. Am J Sports Med. 2004;32(2):477–83. https://doi.org/10.1177/0363546503258928.
Patel SA, Hageman J, Quatman CE, Wordeman SC, Hewett TE. Prevalence and location of bone bruises associated with anterior cruciate ligament injury and implications for mechanism of injury: a systematic review. Sports Med. 2014;44(2):281–93. https://doi.org/10.1007/s40279-013-0116-z.
Meyer EG, Haut RC. Anterior cruciate ligament injury induced by internal tibial torsion or tibiofemoral compression. J Biomech. 2008;41(16):3377–83. https://doi.org/10.1016/j.jbiomech.2008.09.023.
Daia B, Maob M, Garrettc WE, Yub B. Biomechanical characteristics of an anterior cruciate ligament injury in javelin throwing. J Sport Health Sci. 2015;4(4):333–40. https://doi.org/10.1016/j.jshs.2015.07.004.
Markolf KL, Burchfield DM, Shapiro MM, Shepard MF, Finerman GA, Slauterbeck JL. Combined knee loading states that generate high anterior cruciate ligament forces. J Orthop Res. 1995;13(6):930–5. https://doi.org/10.1002/jor.1100130618.
Yu B, Lin CF, Garrett WE. Lower extremity biomechanics during the landing of a stop-jump task. Clin Biomech. 2006;21(3):297–305. https://doi.org/10.1016/j.clinbiomech.2005.11.003.
Dai B, Herman D, Liu H, Garrett WE, Yu B. Prevention of ACL injury, part II: effects of ACL injury prevention programs on neuromuscular risk factors and injury rate. Res Sports Med. 2012;20(3–4):198–222. https://doi.org/10.1080/15438627.2012.680987.
Liu H, Wu W, Yao W, Spang JT, Creighton RA, Garrett WE, et al. Effects of knee extension constraint training on knee flexion angle and peak impact ground-reaction force. Am J Sports Med. 2014;42(4):979–86. https://doi.org/10.1177/0363546513519323.
Szkopek K, Warming T, Neergaard K, Jørgensen HL, Christensen HE, Krogsgaard M. Pain and knee function in relation to degree of bone bruise after acute anterior cruciate ligament rupture. Scand J Med Sci Sports. 2012;22(5):635–42. https://doi.org/10.1111/j.1600-0838.2011.01297.x.
Yoon JP, Chang CB, Yoo JH, Kim SJ, Choi JY, Choi J-A, et al. Correlation of magnetic resonance imaging findings with the chronicity of an anterior cruciate ligament tear. J Bone Joint Surg Am. 2010;92(2):353–60. https://doi.org/10.2106/JBJS.I.00031.
Author information
Authors and Affiliations
Contributions
LZ selected the original studies, extracted data from the finally included studies, participated in data analysis, and wrote the first draft of the manuscript. JH and WG participated in data analysis and revised the manuscript. HL and BY designed the study, filtered selected studies, participated in data analysis, and revised the manuscript. All authors read and approved the final submitted manuscript.
Corresponding authors
Ethics declarations
Funding
This review was partially supported by two grants from the China National Natural Science Foundation (grant nos. 81572212 and 30870600). The funding source had no influence on the direction, planning or results of the research, nor on the interpretation of its findings.
Conflict of interest
Liwen Zhang, Jonathon Hacke, William Garrett, Hui Liu and Bing Yu declare that they have no conflicts of interest relevant to the content of this review.
Rights and permissions
About this article
Cite this article
Zhang, L., Hacke, J.D., Garrett, W.E. et al. Bone Bruises Associated with Anterior Cruciate Ligament Injury as Indicators of Injury Mechanism: A Systematic Review. Sports Med 49, 453–462 (2019). https://doi.org/10.1007/s40279-019-01060-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-019-01060-6