Abstract
Objective
To study the various comorbidities and their impact on outcome of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infected children.
Methodology
Review of medical records of 120 children (58.4% males), aged 1 month to 18 years, admitted between 1 March and 31 December, 2020 with at least one positive RT-PCR test for SARS-CoV-2. Clinical and demographic variables were compared between children with and without co-morbidities.
Results
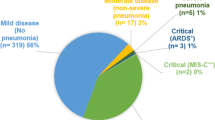
62 (51.7%) children had comorbidities. The most common comorbidity was tuberculosis (32.3%) followed by other infections (27.4%) and hematological (19.4%) conditions. Fever (89.2%) was the most common clinical feature followed by respiratory (52.5%) and gastrointestinal (32.5%) manifestations. There was no significant difference in the severity of COVID illness, length of hospital stay and adverse outcomes (ventilation and mortality) among children with and without comorbidities.
Conclusion
The presence of a comorbid illness in pediatric inpatients with COVID-19 did not impact the illness severity, length of hospitalization, ventilation requirement and mortality.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Guan W, Liang W, Zhao Y, et al. Comorbidity and its impact on 1590 patients with COVID-19 in China: A nationwide analysis. European Respiratory J. 2020; 55
Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult in-patients with COVID-19 in Wuhan, China: A retrospective cohort study. The Lancet. 2020; 395:1054–62
Tsankov BK, Allaire JM, Irvine MA, et al. Severe COVID-19 Infection and pediatric comorbidities: A systematic review and meta-analysis. Intern J Infect Dis. 2021; 103: 246–56.
Valdres J M, Starfield B, Sibbald B, et al. Defining comorbidity: implications for understanding health and health services. Ann Fam Med. 2009; 7: 357–63.
Clinical management of severe acute respiratory infection when COVID-19 is suspected. Accessed October 31, 2020. Available at: https://www.who.int/publications-detail/clinical-management-of-severe-acuterespiratory-infection-when-novel-coronavirus-(ncov)-infection-issuspected
Dong Y, Mo X, Hu Y, et al. Epidemiological characteristics of 2143 pediatric patients with 2019 coronavirus disease in China. Pediatrics. 2020; e20200702.
Meena J, Yadav J, Saini L, et al. Clinical features and outcome of SARS-CoV-2 infection in children: A systematic review and meta-analysis. Indian Pediatr. 2020; 57: 820–26.
Shrinivasan R, Rane S, Pai M. India’s syndemic of Tuberculosis and COVID-19. BMJ Global Health. 2020; 5: e003979.
Girmenia C, Gentile G, Micozzi A, et al. COVID-19 in patients with hematologic disorders undergoing therapy: Perspective of a large referral hematology center in Rome. Acta Haematol. 2020; 143: 574–82.
Adeiza SS, Shuaibu AB, Shuaibu GM. Random effects meta-analysis of COVID-19/S. Aureus partnership in co-infection GMS. Hygiene and Infection Control. 2020;15: 2196–5226.
Saddique A, Rana MS, Alam MM, et al. Emergence of co-infection of COVID-19 and dengue: A serious public health threat. J Infect. 2020;81:16–18.
Collange O, Tacquard C, Delabranche X, et al. Coronavirus disease 2019: associated multiple organ damage. Open Forum Infect Dis. 2020;7:249.
Rao S, Gavali V, Prabhu S, et al. Outcome of children admitted with SARS-CoV-2 infection: Experiences from a pediatric public hospital. Indian Pediatr. 2021;58:358–62.
Author information
Authors and Affiliations
Corresponding author
Additional information
Ethical clearance
Institutional Ethical Committee, LH Medical College; No. LHMC/IEC/2020/97, dated November 6, 2020.
Contributors
DK: collected data and wrote the initial manuscript; VK, PK: critically analyzed the manuscript; PS: helped in data collection and revision of manuscript. All the authors read and approved the final manuscript.
Funding
None
Competing interests
None stated
Rights and permissions
About this article
Cite this article
Kapoor, D., Kumar, V., Pemde, H. et al. Impact of Comorbidities on Outcome in Children With COVID-19 at a Tertiary Care Pediatric Hospital. Indian Pediatr 58, 572–575 (2021). https://doi.org/10.1007/s13312-021-2244-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-021-2244-0