Abstract
Background
Symptoms of posttraumatic stress disorder (PTSD) after acute coronary syndrome (ACS) are associated with recurrent ACS events and mortality. Poor sleep may be a mechanism, but the association between PTSD and sleep after ACS is unknown.
Purpose
This study aims to estimate the association between ACS-induced PTSD symptoms and self-reported sleep.
Methods
ACS-induced PTSD symptoms were assessed 1-month post-ACS in 188 adults using the Impact of Events Scale-Revised. Sleep was assessed using the Pittsburgh Sleep Quality Index. Linear and logistic regression models were used to determine whether PTSD symptoms were associated with self-reported sleep, independent of sociodemographic and clinical covariates.
Results
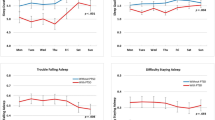
In adjusted models, ACS-induced PTSD symptoms were associated with worse overall sleep (β = 0.22, p = 0.003) and greater impairment in six of seven components of sleep (all p values <0.05).
Conclusions
ACS-induced PTSD symptoms may be associated with poor sleep, which may explain why PTSD confers increased cardiovascular risk after ACS.
Similar content being viewed by others
References
Edmondson D, Richardson S, Falzon L, Davidson KW, Mills MA, Neria Y. Posttraumatic stress disorder prevalence and risk of recurrence in acute coronary syndrome patients: A meta-analytic review. PLoS One. 2012;7:e38915.
Babson KA, Feldner MT. Temporal relations between sleep problems and both traumatic event exposure and PTSD: A critical review of the empirical literature. J Anxiety Disord. 2010;24:1-15.
Ohayon MM, Shapiro CM. Sleep disturbances and psychiatric disorders associated with posttraumatic stress disorder in the general population. Compr Psychiatry. 2000;41:469-478.
Schiza SE, Simantirakis E, Bouloukaki I, et al. Sleep patterns in patients with acute coronary syndromes. Sleep Med. 2010;11:149-153.
Schwartz SW, Cornoni-Huntley J, Cole S, Hays J, Blazer DG, Schocken DD. Are sleep complaints an independent risk factor for myocardial infarction? Ann Epidemiol. 1998;8:384-392.
Caska CM, Hendrickson BE, Wong MH, Ali S, Neylan T, Whooley MA. Anger expression and sleep quality in patients with coronary heart disease: Findings from the Heart and Soul Study. Psychosom Med. 2009;71:280-285.
Mundy E, Baum A. Medical disorders as a cause of psychological trauma and posttraumatic stress disorder. Curr Opin Psychiatry. 2004;17:123-127.
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989;28:193-213.
Weiss D. The impact of event scale: Revised. In: Wilson JP, Tang CS, eds. Cross-cultural assessment of psychological trauma and PTSD. New York: Springer; 2007:219-238.
First M, Spitzer R, Gibbon M, Williams J. Structured clinical interview for DSM-IV Axis I Disorders. Washington, DC: American Psychiatric Press; 1997.
Franklin CL, Sheeran T, Zimmerman M. Screening for trauma histories, posttraumatic stress disorders (PTSD) and subthreshold PTSD in psychiatric outpatients. Psychol Assess. 2002;14:467-471.
Goldberg RJ, Currie K, White K, et al. Six-month outcomes in a multinational registry of patients hospitalized with an acute coronary syndrome (the Global Registry of Acute Coronary Events [GRACE]). Am J Cardiol. 2004;93:288-293.
Charlson M, Szatrowski TP, Peterson J, Gold J. Validation of a combined comorbidity index. J Clin Epidemiol. 1994;47:1245-1251.
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561-571.
Paffenbarger RS Jr, Blair SN, Lee IM, Hyde RT. Measurement of physical activity to assess health effects in free-living populations. Med Sci Sports Exerc. 1993;25:60-70.
Beck A, Steer R, Garbin M. Psychometric properties of the Beck Depression Inventory: 25 years of evaluation. Clin Psychiatry Rev. 1988;8:77-100.
Paffenbarger RS, Wing AL, Hyde RT. Physical activity as an index of heart attack risk in college alumni. Am J Epidemiol. 1978;108:161-175.
Kuppermann M, Lubeck DP, Mazonson PD, et al. Sleep problems and their correlates in a working population. J Gen Intern Med. 1995;10:25-32.
Germain A, Buysse DJ, Shear MK, Fayyad R, Austin C. Clinical correlates of poor sleep quality in posttraumatic stress disorder. J Trauma Stress. 2004;17:477-484.
Sanchez-Ortuno MM, Edinger JD. Cognitive-behavioral therapy for the management of insomnia comorbid with mental disorders. Curr Psychiatry Rep. 2012;14:519-528.
Lichstein KL. Secondary insomnia: A myth dismissed. Sleep Med Rev. 2006;10:3-5.
Blechert J, Michael T, Grossman P, Lajtman M, Wilhelm FH. Autonomic and respiratory characteristics of posttraumatic stress disorder and panic disorder. Psychosom Med. 2007;69:935-943.
Yang AC, Tsai S-J, Yang C-H, Kuo C-H, Chen T-J, Hong C-J. Reduced physiologic complexity is associated with poor sleep in patients with major depression and primary insomnia. J Affect Disord. 2011;131:179-185.
Lijmer JG, Bossuyt PMM, Heisterkamp SH. Exploring sources of heterogeneity in systematic reviews of diagnostic tests. Stat Med. 2002;21:1525-1537.
Dørheim SK, Bondevik GT, Eberhard-Gran M, Bjorvatn B. Sleep and depression in postpartum women: A population-based study. Sleep. 2009;32:847-855.
Tsuno N, Besset A, Ritchie K. Sleep and depression. J Clin Psychiatry. 2005;66:1254-1269.
Knutson KL, Spiegel K, Penev P, Cauter EV. The metabolic consequences of sleep deprivation. Sleep Med Rev. 2007;11:163-178.
Voderholzer U, Al-Shajlawi A, Weske G, Feige B, Riemann D. Are there gender differences in objective and subjective sleep measures? A study of insomniacs and healthy controls. Depress Anxiety. 2003;17:162-172.
Loredo JS, Soler X, Bardwell W, Ancoli-Israel S, Dimsdale JE, Palinkas LA. Sleep health in U.S. Hispanic population. Sleep. 2007;33:962-967.
Koren D, Arnon I, Lavie P, Klein E. Sleep complaints as early predictors of posttraumatic stress disorder: A 1-year prospective study of injured survivors of motor vehicle accidents. Am J Psychiatry. 2002;159:855-857.
Creamer M, Bell R, Failla S. Psychometric properties of the Impact of Event Scale—Revised. Behav Res Ther. 2003;41:1489-1496.
Shemesh E, Yehuda R, Milo O, et al. Posttraumatic stress, nonadherence, and adverse outcome in survivors of a myocardial infarction. Psychosom Med. 2004;66:521-526.
Lichtman JH, Bigger JT Jr, Blumenthal JA, et al. Depression and coronary heart disease: Recommendations for screening, referral, and treatment: A science advisory from the American Heart Association Prevention Committee of the Council on Cardiovascular Nursing, Council on Clinical Cardiology, Council on Epidemiology and Prevention, and Interdisciplinary Council on Quality of Care and Outcomes Research: endorsed by the American Psychiatric Association. Circulation. 2008;118:1768-1775.
Acknowledgments
This work was supported by grants HL-088117, HL-076857, HL-080665, HL-101663, and HL-084034 from the National Heart, Lung, and Blood Institute (NHLBI) of the National Institutes of Health (NIH). Dr. Shaffer is supported by grants 12CRP8870004 from the American Heart Association and K23-HL112850 from NHLBI/NIH. Dr. Kronish is supported by grant K23-HL098359 from NHLBI/NIH.
Conflict of Interest Statement
The authors have no conflict of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Shaffer, J.A., Kronish, I.M., Burg, M. et al. Association of Acute Coronary Syndrome-Induced Posttraumatic Stress Disorder Symptoms with Self-Reported Sleep. ann. behav. med. 46, 349–357 (2013). https://doi.org/10.1007/s12160-013-9512-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-013-9512-8