Abstract
Purpose
To review the diagnostic and therapeutic procedures of patients diagnosed with Endometrial Stromal Sarcoma (ESS) and Undifferentiated Uterine Sarcoma (USS) at our institution and investigate their clinical outcomes and factors affecting prognosis.
Methods
We retrospectively collected demographic data, preoperative diagnostic methods and therapeutic management of patients treated for ESS and UUS between January 1995 and December 2019 at Vall d’Hebron Barcelona Hospital Campus, Spain. Overall survival and disease-free survival were calculated. Cox proportional-hazards regression models were calculated.
Results
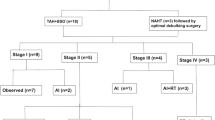
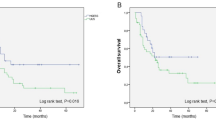
Sixty-three patients were included in the study, of which 51(81%) had a diagnosis of ESS and 12(19%) of UUS. Twenty patients (31.7%) were diagnosed after a previous non-oncologic surgery, and 12 of them (60%) suffered from tumor disruption. Cytoreductive procedures were needed in 29 patients (46%), and optimal cytoreduction was achieved in 80.9% of the patients. The median follow-up was 7.6 years (IQR = 0.99–14.31). Five-year overall survival was 57.6% (44.2–68.8) and was significantly better for low-grade ESS (LG-ESS) patients (p < 0.01). Five-year disease-free survival was 57.1% (42.8–69.1) and was also significantly higher in LG-ESS cohort (p = 0.03). After multivariate analysis histological type, age, FIGO stage, optimal surgery and mitotic index were found significantly correlated with survival. For high-grade EES (HG-ESS) and USS patients adjuvant radiotherapy also correlated with improved survival.
Conclusion
Overall survival and disease-free survival are significantly better in patients with LG-ESS cohort. HG-ESS and UUS show similar survival outcomes. Age, FIGO stage, optimal surgery and histological type were significantly correlated with survival in the global cohort, whilst adjuvant radiotherapy correlated with improved survival in HG-ESS and UUS patients.

Similar content being viewed by others
References
Horng H-C, et al. Uterine sarcoma Part II—Uterine endometrial stromal sarcoma: The TAG systematic review. Taiwan J Obstet Gynecol. 2016;55(4):472–9. https://doi.org/10.1016/j.tjog.2016.04.034.
Conklin CMJ, Longacre TA. Endometrial stromal tumors: the new WHO classification. Adv Anat Pathol. 2014;21(6):383–93. https://doi.org/10.1097/PAP.0000000000000046.
Chan JK, et al. Endometrial stromal sarcoma: a population-based analysis. Br J Cancer. 2008;99(8):1210–5. https://doi.org/10.1038/sj.bjc.6604527.
Prat J, Mbatani N. Uterine sarcomas. Int J Gynecol Obstet. 2015;131:S105–10. https://doi.org/10.1016/j.ijgo.2015.06.006.
Lee C-H, et al. The clinicopathologic features of YWHAE-FAM22 endometrial stromal sarcomas: a histologically high-grade and clinically aggressive tumor. Am J Surg Pathol. 2012;36(5):641–53. https://doi.org/10.1097/PAS.0b013e31824a7b1a.
Parra-Herran C, Howitt BE. Uterine Mesenchymal Tumors: Update on Classification, Staging, and Molecular Features. Surg Pathol Clin. 2019;12(2):363–96. https://doi.org/10.1016/j.path.2019.01.004.
Cuppens T, Tuyaerts S, Amant F. Potential therapeutic targets in uterine sarcomas. Sarcoma. 2015;2015:243298. https://doi.org/10.1155/2015/243298.
Cotzia P, et al. Undifferentiated uterine sarcomas represent under-recognized high-grade endometrial stromal sarcomas. Am J Surg Pathol. 2019;43(5):662–9. https://doi.org/10.1097/PAS.0000000000001215.
Hardell E, Westbom-Fremer S, Schoolmeester JK, Ma A, Carlson JW. Validation of a mitotic index cutoff as a prognostic marker in undifferentiated uterine sarcomas. Am J Surg Pathol. 2017;41(9):7.
Amant F, et al. Gynecologic Cancer InterGroup (GCIG) consensus review for endometrial stromal sarcoma. J Int Gynecol Cancer Soc. 2014. https://doi.org/10.1097/IGC.0000000000000205.
Wang M, Meng S-H, Li B, He Y, Wu Y-M. Survival outcomes of different treatment modalities in patients with low-grade endometrial stromal sarcoma. Chin Med J (Engl). 2019;132(9):1128–32. https://doi.org/10.1097/CM9.0000000000000259.
Bai H, et al. Ovary and uterus-sparing procedures for low-grade endometrial stromal sarcoma: a retrospective study of 153 cases. Gynecol Oncol. 2014;132(3):654–60. https://doi.org/10.1016/j.ygyno.2013.12.032.
Ryu H, et al. Long-term treatment of residual or recurrent low-grade endometrial stromal sarcoma with aromatase inhibitors: A report of two cases and a review of the literature. Oncol Lett. 2015;10(5):3310–4. https://doi.org/10.3892/ol.2015.3674.
Cui R, Yuan F, Wang Y, Li X, Zhang Z, Bai H. Clinicopathological characteristics and treatment strategies for patients with low-grade endometrial stromal sarcoma. Medicine (Baltimore). 2017;96(15):e6584. https://doi.org/10.1097/MD.0000000000006584.
Meurer M, et al. Localized high grade endometrial stromal sarcoma and localized undifferentiated uterine sarcoma: a retrospective series of the French Sarcoma Group. Int J Gynecol Cancer. 2019;29(4):691–8. https://doi.org/10.1136/ijgc-2018-000064.
Wais M, Tepperman E, Bernardini MQ, Gien LT, Jimenez W, Murji A. A multicentre retrospective review of clinical characteristics of uterine sarcoma. J Obstet Gynaecol Can. 2017;39(8):652–8. https://doi.org/10.1016/j.jogc.2017.03.090.
Graebe K, et al. Incidental power morcellation of malignancy: a retrospective cohort study. Gynecol Oncol. 2015;136(2):274–7. https://doi.org/10.1016/j.ygyno.2014.11.018.
Bretthauer M, et al. Uterine morcellation and survival in uterine sarcomas. Eur J Cancer Oxf Engl. 2018;101:62–8. https://doi.org/10.1016/j.ejca.2018.06.007.
Bogani G, et al. Morcellation of undiagnosed uterine sarcoma: A critical review. Crit Rev Oncol Hematol. 2016;98:302–8. https://doi.org/10.1016/j.critrevonc.2015.11.015.
Bogani G, Dowdy SC, Cliby WA, Ghezzi F, Rossetti D, Mariani A. Role of pelvic and para-aortic lymphadenectomy in endometrial cancer: Current evidence. J Obstet Gynaecol Res. 2014;40(2):301–11. https://doi.org/10.1111/jog.12344.
Zhang J, Li T, Zhang J, Zhu L, Lang J, Leng J. ‘Clinical characteristics and prognosis of unexpected uterine sarcoma after hysterectomy for presumed myoma with and without transvaginal scalpel morcellation. Int J Gynecol Cancer Soc. 2016;26(3):456–63. https://doi.org/10.1097/IGC.0000000000000638.
Shah JP, Bryant CS, Kumar S, Ali-Fehmi R, Malone JM, Morris RT. Lymphadenectomy and ovarian preservation in low-grade endometrial stromal sarcoma. Obstet Gynecol. 2008;112(5):1102–8. https://doi.org/10.1097/AOG.0b013e31818aa89a.
Seagle B-LL, Shilpi A, Buchanan S, Goodman C, Shahabi S. Low-grade and high-grade endometrial stromal sarcoma: A National Cancer Database study. Gynecol Oncol. 2017;146(2):254–62. https://doi.org/10.1016/j.ygyno.2017.05.036.
Yamazaki H, et al. Long-term survival of patients with recurrent endometrial stromal sarcoma: a multicenter, observational study. J Gynecol Oncol. 2015;26(3):214–21. https://doi.org/10.3802/jgo.2015.26.3.214.
Zhang Y-Y, Li Y, Qin M, Cai Y, ** Y, Pan L-Y. High-grade endometrial stromal sarcoma: a retrospective study of factors influencing prognosis. Cancer Manag Res. 2019;11:831–7. https://doi.org/10.2147/CMAR.S187849.
Kim WY, et al. Low-grade endometrial stromal sarcoma: a single center’s experience with 22 cases. Int J Gynecol Cancer Off J Int Gynecol Cancer Soc. 2008;18(5):1084–9. https://doi.org/10.1111/j.1525-1438.2007.01159.x.
Chu MC, Mor G, Lim C, Zheng W, Parkash V, Schwartz PE. Low-grade endometrial stromal sarcoma: hormonal aspects. Gynecol Oncol. 2003;90(1):170–6. https://doi.org/10.1016/s0090-8258(03)00258-0.
Cui R, Cao G, Bai H, Zhang Z. The clinical benefits of hormonal treatment for LG-ESS: a meta-analysis. Arch Gynecol Obstet. 2019. https://doi.org/10.1007/s00404-019-05308-4.
Kyriazoglou A, et al. Management of uterine sarcomas and prognostic indicators: real world data from a single-institution. BMC Cancer. 2018;18(1):1247. https://doi.org/10.1186/s12885-018-5156-1.
Funding
The present work was not supported by any grant or organization.
Author information
Authors and Affiliations
Contributions
S. Cabrera is the principal investigator, designed the study, reviewed the literature, collected and analyzed data, and wrote the paper. V. Bebia, S. Franco-Camps, L. Mañalich and U. Acosta contributed to the collection of data, critical revision of the manuscript, and read and approved the final draft here uploaded. V. Bebia performed the statistical analyses. A. Gil-Moreno and A. García-Jimenez reviewed the manuscript for intellectual and scientific content, and approved the final draft.
Corresponding author
Ethics declarations
Availability of data and material
Data of this work are available under justified request to the corresponding author.
Conflicts of interest
The authors state that they have neither financial nor personal relationships with any organization that could inappropriately influence the present work.
Ethics approval
The present research was submitted and approved by Vall d’Hebron Ethics Committee (Project Code PR(AMI)526/2019) on date Dec 11th, 2019.
Consent to participate
Not applicable regarding the decision made by Ethics Committee.
Consent for publication
All of the authors are in agreement with the final draft and consent for its publication.
Informed consent
For this type of study, no informed consent is required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cabrera, S., Bebia, V., Acosta, U. et al. Survival outcomes and prognostic factors of endometrial stromal sarcoma and undifferentiated uterine sarcoma. Clin Transl Oncol 23, 1210–1219 (2021). https://doi.org/10.1007/s12094-020-02512-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-020-02512-6