Abstract
Background
Seizures are a common complication after intracerebral hemorrhage (ICH) but there is a substantial lack of information on the long-term incidence in ICH survivors and whether post-ICH seizures affect functional long-term outcome.
Methods
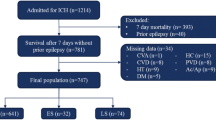
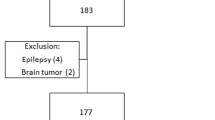
Over a five-year period 464 consecutive patients with spontaneous ICH were analyzed. Focussing on 1-year ICH survivors, clinical, and radiological parameters were retrieved from institutional prospective databases. The occurrence of seizures was categorized as early (≤7 days) or late (>7 days). Functional outcome was assessed by mailed questionnaires and telephone interviews, and was categorized into good vs. poor (mRS: 0–2 vs. 3–5) and favorable vs. unfavorable (mRS: 0–3 vs. 4–5). Multivariate regression models were calculated to investigate risk factors associated with post-ICH seizures including an a priori defined subgroup analysis of lobar ICH patients.
Results
Among 203 long-term ICH survivors, 19.7 % developed seizures of which 55 % occurred late. Factors associated with seizures were lobar location (OR 8.10; 95 % CI 3.04–21.59; p < 0.001), sepsis (OR 4.59; 95 % CI 1.20–17.53; p = 0.026), and history of alcohol abuse (OR 3.36; 95 % CI 1.25–9.06; p = 0.017). Subgroup analysis of lobar ICH patients revealed history of alcohol abuse as the only independent predictor of post-ICH seizures (OR 5.22; 95 % CI 1.25–21.78; p = 0.024). Functional long-term outcome among survivors was slightly worse in patients with post-ICH seizures (p = 0.059). In multivariate regression modeling for prediction of poor outcome, the parameter “post-ICH seizures” again reached a statistical trend (p = 0.065), and established parameters such as age, GCS, and hemorrhage volume were independently related to poor outcome.
Conclusions
Post-ICH seizures among long-term ICH survivors are common and may contribute to unfavorable functional outcome. Especially lobar ICH patients with a history of alcohol abuse are at risk to develop post-ICH seizures. Therefore, this subgroup may represent a target population for a prophylactic anticonvulsive treatment approach, preferably investigated in a prospective randomized trial.

Similar content being viewed by others
References
Alberti A, Paciaroni M, Caso V, Venti M, Palmerini F, Agnelli G. Early seizures in patients with acute stroke: frequency, predictive factors, and effect on clinical outcome. Vasc Health Risk Manag. 2008;4:715–20.
Kilpatrick CJ, Davis SM, Tress BM, Rossiter SC, Hopper JL, Vandendriesen ML. Epileptic seizures in acute stroke. Arch Neurol. 1990;47:157–60.
Bladin CF, Alexandrov AV, Bellavance A, et al. Seizures after stroke: a prospective multicenter study. Arch Neurol. 2000;57:1617–22.
Beghi E, D’Alessandro R, Beretta S, et al. Incidence and predictors of acute symptomatic seizures after stroke. Neurology. 2011;77:1785–93.
Menon B, Shorvon SD. Ischaemic stroke in adults and epilepsy. Epilepsy Res. 2009;87:1–11.
Kammersgaard LP, Olsen TS. Poststroke epilepsy in the Copenhagen stroke study: incidence and predictors. J Stroke Cerebrovasc Dis. 2005;14:210–4.
Burn J, Dennis M, Bamford J, Sandercock P, Wade D, Warlow C. Epileptic seizures after a first stroke: the Oxfordshire Community Stroke Project. BMJ. 1997;315:1582–7.
Yang TM, Lin WC, Chang WN, et al. Predictors and outcome of seizures after spontaneous intracerebral hemorrhage. J Neurosurg. 2009;111:87–93.
Garrett MC, Komotar RJ, Starke RM, Merkow MB, Otten ML, Connolly ES. Predictors of seizure onset after intracerebral hemorrhage and the role of long-term antiepileptic therapy. J Crit Care. 2009;24:335–9.
Passero S, Rocchi R, Rossi S, Ulivelli M, Vatti G. Seizures after spontaneous supratentorial intracerebral hemorrhage. Epilepsia. 2002;43:1175–80.
Morgenstern LB, Hemphill JC 3rd, Anderson C, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2010;41:2108–29.
Arboix A, Garcia-Eroles L, Massons JB, Oliveres M, Comes E. Predictive factors of early seizures after acute cerebrovascular disease. Stroke. 1997;28:1590–4.
Vespa PM, O’Phelan K, Shah M, et al. Acute seizures after intracerebral hemorrhage: a factor in progressive midline shift and outcome. Neurology. 2003;60:1441–6.
Claassen J, Jette N, Chum F, et al. Electrographic seizures and periodic discharges after intracerebral hemorrhage. Neurology. 2007;69:1356–65.
Kuramatsu JB, Sauer R, Mauer C, et al. Correlation of age and haematoma volume in patients with spontaneous lobar intracerebral haemorrhage. J Neurol Neurosurg Psychiatry. 2011;82:144–9.
Tejerina E, Esteban A, Fernandez-Segoviano P, et al. Accuracy of clinical definitions of ventilator-associated pneumonia: comparison with autopsy findings. J Crit Care. 2010;25:62–8.
Wilson ML, Gaido L. Laboratory diagnosis of urinary tract infections in adult patients. Clin Infect Dis. 2004;38:1150–8.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of the Third Report of National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult TREATMENT panel III). JAMA. 2001;285:2486–97.
Reeves RA. The rational clinical examination. Does this patient have hypertension? How to measure blood pressure. JAMA. 1995;273:1211–8.
Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care. 1997;20:1183–97.
Commission on Epidemiology and Prognosis, International League Against Epilepsy. Guidelines for epidemiologic studies on epilepsy. Epilepsia. 1993;34:592–6.
Brott T, Broderick J, Kothari R, et al. Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke. 1997;28:1–5.
Kothari RU, Brott T, Broderick JP, et al. The ABCs of measuring intracerebral hemorrhage volumes. Stroke. 1996;27:1304–5.
Graeb DA, Robertson WD, Lapointe JS, Nugent RA, Harrison PB. Computed tomographic diagnosis of intraventricular hemorrhage. Etiology and prognosis. Radiology. 1982;143:91–6.
Szaflarski JP, Rackley AY, Kleindorfer DO, et al. Incidence of seizures in the acute phase of stroke: a population-based study. Epilepsia. 2008;49:974–81.
Andaluz N, Zuccarello M. Recent trends in the treatment of spontaneous intracerebral hemorrhage: analysis of a nationwide inpatient database. J Neurosurg. 2009;110:403–10.
Mayer SA, Rincon F. Treatment of intracerebral haemorrhage. Lancet Neurol. 2005;4:662–72.
Faught E, Peters D, Bartolucci A, Moore L, Miller PC. Seizures after primary intracerebral hemorrhage. Neurology. 1989;39:1089–93.
Giroud M, Gras P, Fayolle H, Andre N, Soichot P, Dumas R. Early seizures after acute stroke: a study of 1,640 cases. Epilepsia. 1994;35:959–64.
Willmore LJ. Post-traumatic seizures. Neurol Clin. 1993;11:823–34.
Goswami RP, Karmakar PS, Ghosh A. Early seizures in first-ever acute stroke patients in India: incidence, predictive factors and impact on early outcome. Eur J Neurol. 2012;19:1361–6.
Brathen G, Brodtkorb E, Helde G, Sand T, Bovim G. The diversity of seizures related to alcohol use. A study of consecutive patients. Eur J Neurol. 1999;6:697–703.
Hillbom ME. Occurrence of cerebral seizures provoked by alcohol abuse. Epilepsia. 1980;21:459–66.
Leone M, Bottacchi E, Beghi E, et al. Alcohol use is a risk factor for a first generalized tonic-clonic seizure. The ALC.E. (Alcohol and Epilepsy) Study Group. Neurology. 1997;48:614–20.
Naidech AM, Garg RK, Liebling S, et al. Anticonvulsant use and outcomes after intracerebral hemorrhage. Stroke. 2009;40:3810–5.
Messe SR, Sansing LH, Cucchiara BL, Herman ST, Lyden PD, Kasner SE. Prophylactic antiepileptic drug use is associated with poor outcome following ICH. Neurocrit Care. 2009;11:38–44.
Goldstein LB. Common drugs may influence motor recovery after stroke. The Sygen In Acute Stroke Study Investigators. Neurology. 1995;45:865–71.
Oddo M, Carrera E, Claassen J, Mayer SA, Hirsch LJ. Continuous electroencephalography in the medical intensive care unit. Crit Care Med. 2009;37:2051–6.
Grill MF, Maganti RK. Neurotoxic effects associated with antibiotic use: management considerations. Br J Clin Pharmacol. 2011;72:381–93.
Kuramatsu JB, Gerner ST, Lucking H, et al. Anemia is an independent prognostic factor in intracerebral hemorrhage: an observational cohort study. Crit Care. 2013;17:R148.
Stefan H, May TW, Pfafflin M, et al. Epilepsy in the elderly: comparing clinical characteristics with younger patients. Acta Neurol Scand. 2014;. doi:10.1111/ane.12218.
Blum DE, Eskola J, Bortz JJ, Fisher RS. Patient awareness of seizures. Neurology. 1996;47:260–4.
Acknowledgments
We would like to thank Petra Burkardt and Kerstin Wagner for hel** with data acquisition and Stefan Schwab for valuable discussions.
Conflict of interest
The authors have nothing to disclose. The study was not funded.
Author information
Authors and Affiliations
Corresponding author
Additional information
Dominik Madžar and Joji B. Kuramatsu have contributed equally to this study.
Rights and permissions
About this article
Cite this article
Madžar, D., Kuramatsu, J.B., Gollwitzer, S. et al. Seizures Among Long-Term Survivors of Conservatively Treated ICH Patients: Incidence, Risk Factors, and Impact on Functional Outcome. Neurocrit Care 21, 211–219 (2014). https://doi.org/10.1007/s12028-014-9968-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-014-9968-9