Abstract
Background
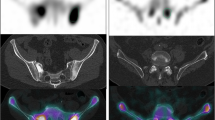
Planar bone scintigraphy (PBS) is a standard radiological technique to detect skeletal metastases from prostate cancer (PC), the addition of SPECT-CT to PBS improves its diagnostic accuracy. The aim of this study was to assess the additional value of targeted SPECT-CT with PBS in detecting skeletal metastasis form prostate cancer, considering resource implications in an Irish hospital setting.
Methods
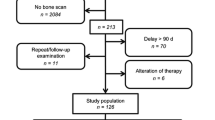
54 PC patients with increased radiotracer uptake on PBS were retrospectively recruited from 2012 to 2013. All underwent targeted evaluation with SPECT-CT. PBS and SPECT-CT images were reviewed by two nuclear medicine radiologists and reported independently. The final diagnosis was made based on the CT finding corresponding to the area of radiotracer uptake.
Results
The mean age was 70.9 years (48–88 years) and median PSA at presentation was 13.9 ng/ml (4.2–215 ng/ml). 68.5 % (n = 37) men received treatment for PC while 31.5 % (n = 17) patients had not received treatment prior to PBS. 164 areas of increased radiotracer uptake were identified on PBS; 13 areas were characterised as metastatic on SPECT-CT; iliac bone (n = 3), ribs (n = 1), skull (n = 2), sacrum (n = 1), ischium (n = 1), femur (n = 3), thoracic spine (n = 1) and cervical spine (n = 1). 151 areas were characterised as benign on SPECT-CT. One area of increased radiotracer uptake in the ribs was subsequently described as indeterminate after evaluation with SPECT-CT.
Conclusion
SPECT-CT improves the diagnostic accuracy of PBS in detecting skeletal metastasis from PC and is superior to PBS alone in differentiating benign from malignant lesions. Notwithstanding resource implications of increased cost, specialist equipment and specialist manpower hours; we recommend the use of SPECT-CT in conjunction with PBS for targeted evaluation of suspicious bony lesions in this cohort of patients.

Similar content being viewed by others
References
Hassan FU, Mohan HK, Gnanasegaran G, Vijayanathan S, Fogelman I (2011) Beware of the focal uptake at the ischium on the bone scan in prostate cancer. Nucl Med Commun 32(4):320–323 Epub 2011/01/13
Saitoh H, Hida M, Shimbo T, Nakamura K, Yamagata J, Satoh T (1984) Metastatic patterns of prostatic cancer. Correlation between sites and number of organs involved. Cancer 54(12):3078–3084 (Epub 1984/12/15)
Strobel K, Burger C, Seifert B, Husarik DB, Soyka JD, Hany TF (2007) Characterization of focal bone lesions in the axial skeleton: performance of planar bone scintigraphy compared with SPECT and SPECT fused with CT. Am J Roentgenol 188(5):W467–W474
Jacobson AF, Fogelman I (1998) Bone scanning in clinical oncology: does it have a future? Eur J Nucl Med 25(9):1219–1223 (Epub 1998/09/02)
Love C, Din AS, Tomas MB, Kalapparambath TP, Palestro CJ (2003) Radionuclide bone imaging: an illustrative review. Radiographics 23(2):341–358 (Epub 2003/03/18)
Palmedo H, Marx C, Ebert A, Kreft B, Ko Y, Turler A et al (2014) Whole-body SPECT/CT for bone scintigraphy: diagnostic value and effect on patient management in oncological patients. Eur J Nucl Med Mol Imaging 41(1):59–67 (Epub 2013/08/27)
Schirrmeister H, Guhlmann A, Elsner K, Kotzerke J, Glatting G, Rentschler M et al (1999) Sensitivity in detecting osseous lesions depends on anatomic localization: planar bone scintigraphy versus 18F PET. J Nucl Med Off Publ Soc Nucl Med 40(10):1623–1629 (Epub 1999/10/16)
Schirrmeister H, Glatting G, Hetzel J, Nussle K, Arslandemir C, Buck AK et al (2001) Prospective evaluation of the clinical value of planar bone scans, SPECT, and (18)F-labeled NaF PET in newly diagnosed lung cancer. J Nucl Med Off Publ Soc Nucl Med 42(12):1800–1804 (Epub 2001/12/26)
Minoves M (2003) Bone and joint sports injuries: the role of bone scintigraphy. Nucl Med Commun 24(1):3–10 (Epub 2002/12/26)
Cook GJ, Ott RJ (2001) Dual-modality imaging. Eur Radiol 11(10):1857–1858 (Epub 2001/11/10)
Even-Sapir E, Metser U, Mishani E, Lievshitz G, Lerman H, Leibovitch I (2006) The detection of bone metastases in patients with high-risk prostate cancer: Tc-99 m-MDP planar bone scintigraphy, single- and multi-field-of-view SPECT, F-18-fluoride PET, and F-18-fluoride PET/CT. J Nucl Med 47(2):287–297
Savelli G, Maffioli L, Maccauro M, De Deckere E, Bombardieri E (2001) Bone scintigraphy and the added value of SPECT (single photon emission tomography) in detecting skeletal lesions. Q J Nucl Med 45(1):27–37
Utsunomiya D, Shiraishi S, Imuta M, Tomiguchi S, Kawanaka K, Morishita S et al (2006) Added value of SPECT/CT fusion in assessing suspected bone metastasis: comparison with scintigraphy alone and nonfused scintigraphy and CT. Radiology 238(1):264–271 (Epub 2005/11/24)
Even-Sapir E, Martin RH, Barnes DC, Pringle CR, Iles SE, Mitchell MJ (1993) Role of SPECT in differentiating malignant from benign lesions in the lower thoracic and lumbar vertebrae. Radiology 187(1):193–198 (Epub 1993/04/01)
Savelli G, Maffioli L, Maccauro M, De Deckere E, Bombardieri E (2001) Bone scintigraphy and the added value of SPECT (single photon emission tomography) in detecting skeletal lesions. Q J Nucl Med 45(1):27–37 (Epub 2001/07/18)
Helyar V, Mohan HK, Barwick T, Livieratos L, Gnanasegaran G, Clarke SE et al (2010) The added value of multislice SPECT/CT in patients with equivocal bony metastasis from carcinoma of the prostate. Eur J Nucl Med Mol Imaging 37(4):706–713 (Epub 2009/12/18)
Rybak LD, Rosenthal DI (2001) Radiological imaging for the diagnosis of bone metastases. Q J Nucl Med 45(1):53–64 (Epub 2001/07/18)
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McLoughlin, L.C., O’Kelly, F., O’Brien, C. et al. The improved accuracy of planar bone scintigraphy by adding single photon emission computed tomography (SPECT-CT) to detect skeletal metastases from prostate cancer. Ir J Med Sci 185, 101–105 (2016). https://doi.org/10.1007/s11845-014-1228-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-014-1228-7