ABSTRACT
BACKGROUND
Little is known about older women’s experience with a benign breast biopsy.
OBJECTIVES
To examine the psychological impact and experience of women ≥ 65 years of age with a benign breast biopsy.
DESIGN
Prospective cohort study using quantitative and qualitative methods.
SETTING
Three Boston-based breast imaging centers.
PARTICIPANTS
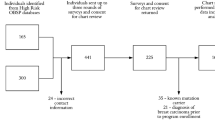
Ninety-four English-speaking women ≥ 65 years without dementia referred for breast biopsy as a result of an abnormal mammogram, not aware of their biopsy results at baseline, and with a subsequent negative biopsy.
MEASUREMENTS
We interviewed women at the time of breast biopsy (before women knew their results) and 6 months post-biopsy. At both interviews, participants completed the validated negative psychological consequences of screening mammography questionnaire (PCQ, scores range from 0 to 36 [high distress], PCQ ≥ 1 suggests a psychological consequence, PCQs <1 are reported at time of screening) and women responded to open-ended questions about their experience. At follow-up, participants described the quality of information received after their benign breast biopsy. We used a linear mixed effects model to examine if PCQs declined over time. We also reviewed participants’ open-ended comments for themes.
RESULTS
Overall, 88 % (83/94) of participants were non-Hispanic white and 33 % (31/94) had a high-school degree or less. At biopsy, 76 % (71/94) reported negative psychological consequences from their biopsy compared to 39 % (37/94) at follow-up (p < 0.01). In open-ended comments, participants noted the anxiety (29 %, 27/94) and discomfort (28 %, 26/94) experienced at biopsy (especially from positioning on the biopsy table). Participants requested more information to prepare for a biopsy and to interpret their negative results. Forty-four percent (39/89) reported at least a little anxiety about future mammograms.
CONCLUSIONS
The high psychological burden of a benign breast biopsy among older women significantly diminishes with time but does not completely resolve. To reduce this burden, older women need more information about undergoing a breast biopsy.


Similar content being viewed by others
REFERENCES
Gotzsche PC, Jorgensen KJ. Screening for breast cancer with mammography. Cochrane Database Syst Rev. 2013;6, CD001877.
Marmot MG, Altman DG, Cameron DA, Dewar JA, Thompson SG, Wilcox M. The benefits and harms of breast cancer screening: an independent review. Br J Cancer. 2013;108:2205–2240.
Nelson HD, Zakher B, Cantor A, Fu R, Griffin J, O’Meara ES, Buist DS, Kerlikowske K, van Ravesteyn NT, Trentham-Dietz A, Mandelblatt JS, Miglioretti DL. Risk factors for breast cancer for women aged 40 to 49 years: a systematic review and meta-analysis. Ann Intern Med. 2012;156:635–648.
Lee SJ, Boscardin WJ, Stijacic-Cenzer I, Conell-Price J, O’Brien S, Walter LC. Time lag to benefit after screening for breast and colorectal cancer: meta-analysis of survival data from the United States, Sweden, United Kingdom, and Denmark. BMJ. 2013;346:e8441.
Schonberg MA, Breslau ES, McCarthy EP. Targeting of mammography screening according to life expectancy in women aged 75 and older. J Am Geriatr Soc. 2013;61:388–395.
Schonberg MA, Leveille SG, Marcantonio ER. Preventive health care among older women: missed opportunities and poor targeting. Am J Med. 2008;121:974–981.
Schonberg MA, Silliman RA, Marcantonio ER. Weighing the benefits and burdens of mammography screening among women age 80 years or older. J Clin Oncol. 2009;27:1774–1780.
Welch HG, Fisher ES. Diagnostic testing following screening mammography in the elderly. J Natl Cancer Inst. 1998;90:1389–1392.
Brett J, Bankhead C, Henderson B, Watson E, Austoker J. The psychological impact of mammographic screening: a systematic review. Psycho Oncol. 2005;14:917–938.
Heckman BD, Fisher EB, Monsees B, Merbaum M, Ristvedt S, Bishop C. Co** and anxiety in women recalled for additional diagnostic procedures following an abnormal screening mammogram. Health Psychol. 2004;23:42–48.
Liao MN, Chen MF, Chen SC, Chen PL. Healthcare and support needs of women with suspected breast cancer. J Adv Nurs. 2007;60:289–298.
Lindfors KK, O’Connor J, Acredolo CR, Liston SE. Short-interval follow-up mammography versus immediate core biopsy of benign breast lesions: assessment of patient stress. AJR Am J Roentgenol. 1998;171:55–58.
Novy DM, Price M, Huynh PT, Schuetz A. Percutaneous core biopsy of the breast: correlates of anxiety. Acad Radiol. 2001;8:467–472.
Poole K. The emergence of the ‘waiting game’: a critical examination of the psychosocial issues in diagnosing breast cancer. J Adv Nurs. 1997;25:273–281.
Sherbourne CD, Stewart AL. The MOS social support survey. Soc Sci Med. 1991;32(6):705–714.
Schonberg MA, Davis RB, McCarthy EP, Marcantonio ER. External validation of an index to predict up to 9-year mortality of community-dwelling adults aged 65 and older. J Am Geriatr Soc. 2011;59:1444–1451.
Cockburn J, De Luise T, Hurley S, Clover K. Development and validation of the PCQ: a questionnaire to measure the psychological consequences of screening mammography. Soc Sci Med. 1992;34:1129–1134.
Pineault P. Breast cancer screening: women’s experiences of waiting for further testing. Oncol Nurs Forum. 2007;34:847–853.
Brett J, Austoker J. Women who are recalled for further investigation for breast screening: psychological consequences 3 years after recall and factors affecting re-attendance. J Public Health Med. 2001;23:292–300.
Lerman C, Daly M, Sands C, Balshem A, Lustbader E, Heggan T, Goldstein L, James J, Engstrom P. Mammography adherence and psychological distress among women at risk for breast cancer. J Natl Cancer Inst. 1993;85:1074–1080.
Lerman C, Trock B, Rimer BK, Boyce A, Jepson C, Engstrom PF. Psychological and behavioral implications of abnormal mammograms. Ann Intern Med. 1991;114:657–661.
Ware J Jr, Kosinski M, Keller SD. A 12-Item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996;34:220–233.
Rehnberg G, Absetz P, Aro AR. Women’s satisfaction with information at breast biopsy in breast cancer screening. Patient Educ Couns. 2001;42:1–8.
Drageset S, Lindstrom TC. Co** with a possible breast cancer diagnosis: demographic factors and social support. J Adv Nurs. 2005;51:217–226.
Steffens RF, Wright HR, Hester MY, Andrykowski MA. Clinical, demographic, and situational factors linked to distress associated with benign breast biopsy. J Psychosoc Oncol. 2011;29:35–50.
Strauss A, Corbin J. Basics of qualitative research: grounded theory-procedures and techniques. Newbury Park: Sage Publication; 1990.
Crabtree F, Miller WL, eds. Doing qualitative research. Newbury Park, CA: Sage Publications; 1992.
Chen CC, David A, Thompson K, Smith C, Lea S, Fahy T. Co** strategies and psychiatric morbidity in women attending breast assessment clinics. J Psychosom Res. 1996;40:265–270.
Lebel S, Jakubovits G, Rosberger Z, Loiselle C, Seguin C, Cornaz C, Ingram J, August L, Lisbona A. Waiting for a breast biopsy. Psychosocial consequences and co** strategies. J Psychosom Res. 2003;55:437–443.
Nosarti C, Roberts JV, Crayford T, McKenzie K, David AS. Early psychological adjustment in breast cancer patients: a prospective study. J Psychosom Res. 2002;53:1123–1130.
Schnur JB, Montgomery GH, Hallquist MN, Goldfarb AB, Silverstein JH, Weltz CR, Kowalski AV, Bovbjerg DH. Anticipatory psychological distress in women scheduled for diagnostic and curative breast cancer surgery. Int J Behav Med. 2008;15:21–28.
Seckel MM, Birney MH. Social support, stress, and age in women undergoing breast biopsies. Clin Nurs Spec. 1996;10:137–143.
Deane KA, Degner LF. Determining the information needs of women after breast biopsy procedures. AORN J. 1997;65(767–72):75–76.
Montgomery M, McCrone SH. Psychological distress associated with the diagnostic phase for suspected breast cancer: systematic review. J Adv Nurs. 2010;66:2372–2390.
Olsson P, Armelius K, Nordahl G, Lenner P, Westman G. Women with false positive screening mammograms: how do they cope? J Med Screen. 1999;6:89–93.
Di Maio M, Perrone F. Quality of life in elderly patients with cancer. Health Qual Life Outcomes. 2003;1:44.
Ganz PA, Guadagnoli E, Landrum MB, Lash TL, Rakowski W, Silliman RA. Breast cancer in older women: quality of life and psychosocial adjustment in the 15 months after diagnosis. J Clin Oncol. 2003;21:4027–4033.
Sammarco A. Quality of life of breast cancer survivors: a comparative study of age cohorts. Cancer Nurs. 2009;32:347–356. quiz 57–8.
Mandelblatt JS, Edge SB, Meropol NJ, Senie R, Tsangaris T, Grey L, Peterson BM Jr, Hwang YT, Kerner J, Weeks J. Predictors of long-term outcomes in older breast cancer survivors: perceptions versus patterns of care. J Clin Oncol. 2003;21:855–863.
Silliman RA, Dukes KA, Sullivan LM, Kaplan SH. Breast cancer care in older women: sources of information, social support, and emotional health outcomes. Cancer. 1998;83:706–711.
Mor V, Allen S, Malin M. The psychosocial impact of cancer on older versus younger patients and their families. Cancer. 1994;74:2118–2127.
Ballantyne PJ. Social context and outcomes for the ageing breast cancer patient: considerations for clinical practitioners. J Clin Nurs. 2004;13:11–21.
Deimling GT, Arendt JA, Kypriotakis G, Bowman KF. Functioning of older, long-term cancer survivors: the role of cancer and comorbidities. J Am Geriatr Soc. 2009;57(Suppl 2):S289–S292.
Neale AV, Tilley BC, Vernon SW. Marital status, delay in seeking treatment and survival from breast cancer. Soc Sci Med. 1986;23:305–312.
Ong G, Austoker J, Brett J. Breast screening: adverse psychological consequences one month after placing women on early recall because of a diagnostic uncertainty. A multicentre study. J Med Screen. 1997;4:158–168.
Degnim AC, Visscher DW, Berman HK, et al. Stratification of breast cancer risk in women with atypia: a Mayo cohort study. J Clin Oncol. 2007;25(19):2671–2677.
Chun J, Pocock B, Joseph KA, El-Tamer M, Klein L, Schnabel F. Breast cancer risk factors in younger and older women. Ann Surg Oncol. 2009;16(1):96–99.
Schonberg MA, Ramanan RA, McCarthy EP, Marcantonio ER. Decision making and counseling around mammography screening for women aged 80 or older. J Gen Intern Med. 2006;21(9):979–985.
Tosteson AN, Fryback DG, Hammond CS. Consequences of false-positive screening mammograms. JAMA Intern Med. 2014;174(6):954–961.
Barton MB, Moore S, Polk S, Shtatland E, Elmore JG, Fletcher SW. Increased patient concern after false-positive mammograms: clinician documentation and subsequent ambulatory visits. J Gen Intern Med. 2001;16:150–156.
Acknowledgements
We are grateful to Rossana Valencia, MPH, Christine Gordon, MPH, and Maria Cecilia Griggs, RN, MPH, for their work recruiting patients to this study. We are also grateful to Elena Morozov at Beth Israel Deaconess Medical Center, and Julie Ferragamo and Jane Pietrantonio at Brigham and Women’s Hospital for hel** us to identify patients for this study. Written permission has been obtained from all persons named in this acknowledgment. Dr. Schonberg had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Dr. Mara Schonberg was supported by a Paul B. Beeson Career Development Award in Aging supported by the National Institute on Aging K23 [K23AG028584], the John A. Hartford Foundation, the Atlantic Philanthropies, the Starr Foundation, and the American Federation for Aging Research. Dr. Ngo received support from Harvard Catalyst, the Harvard Clinical and Translational Science Center (NIH Award #UL1 RR 025758 and financial contributions from Harvard University and its affiliated academic health care centers). Dr. Marcantonio was supported by a Midcareer Investigator Award in Patient-Oriented Research from the National Institute on Aging (K24 AG035075). The sponsors had no role in design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Presentations
This work was presented in part at the Presidential poster session of the 2014 annual meeting of the American Geriatrics Society, 15 May 2014. This work was also presented at the 2014 annual meeting of the New England Region of the Society of General Internal Medicine, 7 March 2014.
Conflict of Interest
Dr. Fein-Zachary worked as a consultant for Siemens Medical Solutions USA, Inc., in 2014. All other authors declare that they do not have a conflict of interest.
Financial Disclosure Information
This research was supported by a Paul B. Beeson Career Development Award in Aging supported by the National Institute on Aging K23 [K23AG028584], the John A. Hartford Foundation, the Atlantic Philanthropies, the Starr Foundation, and the American Federation for Aging Research. Dr. Marcantonio was supported by a Midcareer Investigator Award in Patient-Oriented Research from the National Institute on Aging (K24 AG035075).
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Schonberg, M.A., Silliman, R.A., Ngo, L.H. et al. Older Women’s Experience with a Benign Breast Biopsy—A Mixed Methods Study. J GEN INTERN MED 29, 1631–1640 (2014). https://doi.org/10.1007/s11606-014-2981-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-014-2981-z