Abstract
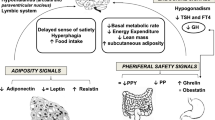
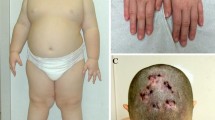
Prader-Willi syndrome (PWS) is a genetic disorder characterized by short stature, low lean body mass, muscular hypotonia, mental retardation, behavioral abnormalities, dysmorphic features, and excessive appetite with progressive obesity. It is caused by lack of expression of genes on the paternally inherited chromosome 15q11.2-q13. This genetic disorder has an estimated prevalence that ranges between 1/10,000–1/30,000. Hypothalamic dysfunction is a common finding in PWS and it has been implicated in several manifestations of this syndrome such as hyperphagia, temperature instability, high pain threshold, sleep disordered breathing, and multiple endocrine abnormalities. These include growth hormone deficiency, central adrenal insufficiency, hypogonadism, hypothyroidism, and obesity often complicated by type 2 diabetes. The aim of this manuscript is to overview the current literature on metabolic and endocrine complications of PWS, focusing on human studies and providing insights on the physio pathological mechanisms. A careful management of metabolic and endocrine complications can contribute to improve quality of life, prevent complications, and prolong life expectancy of PW patients.




Similar content being viewed by others
References
Kanaka-Gantenbein C, Kogia C, Abdel-Naser MB, Chrousos GP. Skin manifestations of growth hormone-induced diseases. Rev Endocr Metab Disord. 2016;17(3):259–67.
Crinò A, Fintini D, Bocchini S, Grugni G. Obesity management in Prader-Willi syndrome: current perspectives. Diabetes Metab Syndr Obes. 2018;11:579–93. https://doi.org/10.2147/DMSO.S141352 eCollection 2018.
Cassidy SB, Schwartz S, Miller JL, Driscoll DJ. Prader-Willi syndrome. Genet Med. 2012;14(1):10–26. https://doi.org/10.1038/gim.0b013e31822bead0.
Butler MG. Prader-Willi syndrome: obesity due to genomic imprinting. Curr Genomics. 2011;12:204–15.
Fitch A. Effective dietary therapies for pediatric obesity treatment. Rev Endocr Metab Disord. 2009;10(3):231–6.
Butler JV, Whittington JE, Holland AJ, Boer H, Clarke D, Webb T. Prevalence of, and risk factors for, physical ill-health in people with Prader-Willi syndrome: a population-based study. Dev Med Child Neurol. 2002;44(4):248–55.
Lind van Wijngaarden RF, Otten BJ, Festen DA, Joosten KF, de Jong FH, Sweep FC, et al. High prevalence of central adrenal insufficiency in patients with PraderWilli syndrome. J Clin Endocrinol Metab. 2008;93:1649–54.
Tauber M, Barbeau C, Jouret B, Pienkowski C, Malzac P, Moncla A, et al. Auxological and endocrine evolution of 28 children with Prader-Willi syndrome: effect of GH therapy in 14 children. Horm Res. 2000;53(6):279–87.
Angulo MA, Castro-Magana M, Lamerson M, Arguello R, Accacha S, Khan A. Final adult height in children with Prader-Willi syndrome with and without human growth hormone treatment. Am J Med Genet A. 2007;143A(13):1456–61.
Zhang Y, Wang J, Zhang G, et al. The neurobiological drive for overeating implicated in Prader–Willi syndrome. Brain Res. 2015;1620:72–80.
Butler MG, Theodoro MF, Bittel DC, Donnelly JE. Energy expenditure and physical activity in Prader–Willi syndrome: comparison with obese subjects. Am J Med Genet A. 2007;143A:449–59.
Burman P, Ritzen EM, Lindgren AC. Endocrine dysfunction in Prader–Willi syndrome: a review with special reference to GH. Endocr Rev. 2001;22:787–799.2.
Dimitropoulos A, Schultz RT. Food-related neural circuitry in Prader- Willi syndrome: response to high- versus low-calorie foods. J Autism Dev Disord. 2008;38(9):1642–53.
Pujol J, Blanco-Hinojo L, Esteba-Castillo S, Caixàs A, Harrison BJ, Bueno M, et al. Anomalous basal ganglia connectivity and obsessive-compulsive behaviour in patients with Prader-Willi syndrome. J Psychiatry Neurosci. 2016;41(4):261–71.
Miller JL, Lynn CH, Driscoll DC, Goldstone AP, Gold JA, Kimonis V, et al. Nutritional phases in Prader Willi syndrome. Am J Med Genet A. 2011;155(5):1040–9.
Goldstone AP, Holland AJ, Butler JV, Whittington JE. Appetite hormones and the transition to hyperphagia in children with Prader-Willi syndrome. Int J Obes. 2012;36(12):1564–70.
Butler MG, Moore J, Morawiecki A, Nicolson M. Comparison of leptin protein levels in Prader-Willi syndrome and control individuals. Am J Med Genet. 1998;75(1):7–12.
Lim CT, Kola B, Korbonits M. The ghrelin/GOAT/GHS-R system and energy metabolism. Rev Endocr Metab Disord. 2011;12(3):173–86.
Wren AM, Seal LJ, Cohen MA, Brynes AE, Frost GS, Murphy KG, et al. Ghrelin enhances appetite and increases food intake in humans. J Clin Endocrinol Metab. 2001;86(12):5992.
Irizarry KA, Miller M, Freemark M, Haqq AM. Prader Willi syndrome: genetics, metabolomics, hormonal function, and new approaches to therapy. Adv Pediatr. 2016;63:47–77.
Bekx MT, Carrel AL, Shriver TC, Li Z, Allen DB. Decreased energy expenditure is caused by abnormal body composition in infants with Prader-Willi syndrome. J Pediatr. 2003;143(3):372–6.
Purtell L, Viardot A, Sze L, Loughnan G, Steinbeck K, Sainsbury A, et al. Postprandial metabolism in adults with Prader-Willi syndrome. Obesity (Silver Spring). 2015;23(6):1159–65.
Brambilla P, Crinò A, Bedogni G, Genetic Obesity Study Group of the Italian Society of Pediatric Endocrinology and Diabetology (ISPED), et al. Metabolic syndrome in children with Prader-Willi syndrome: the effect of obesity. Nutr Metab Cardiovasc Dis. 2011;21(4):269–76.
Goldstone AP, Thomas EL, Brynes AE, et al. Visceral adipose tissue and metabolic complications of obesity are reduced in Prader-Willi syndrome female adults: evidence for novel influences on body fat distribution. J Clin Endocrinol Metab. 2001;86(9):4330–8.
Schuster DP, Osei K, Zipf WB. Characterization of alterations in glucose and insulin metabolism in Prader-Willi subjects. Metabolism. 1996;45(12):1514–20.
Talebizadeh Z, Butler MG. Insulin resistance and obesity-related factors in Prader-Willi syndrome: comparison with obese subjects. Clin Genet. 2004;67(3):230–9.
Fintini D, Grugni G, Brufani C, Bocchini S, Cappa M, Crino A. Use of GLP-1 receptor agonists in Prader-Willi syndrome: report of six cases. Diabetes Care. 2014;37:e76–7.
Berthoud HR, Powley TL. Morphology and distribution of efferent vagal innervation of rat pancreas as revealed with anterograde transport of Dil. Brain Res. 1991;553:336–41.
Fitch A, Bock J. Effective dietary therapies for pediatric obesity treatment. Rev Endocr Metab Disord. 2009;10(3):231–6.
Sze L, Purtell L, Jenkins A, Loughnan G, Smith E, Herzog H, et al. Effects of a single dose of exenatide on appetite, gut hormones, and glucose homeostasis in adults with Prader-Willi syndrome. J Clin Endocrionl Metab. 2011;96:E1314–9.
Butler MG, Theodoro M, Skouse JD. Thyroid Function Studies in Prader–Willi Syndrome. Am J Med Genet A. 2007;143A:488–92.
Sharkia M, Michaud S, Berthier MT. Thyroid function from birth to adolescence in Prader-Willi syndrome. J Pediatr. 2013;163:800–5.
Diene G, Mimoun E, Feigerlova E, Caula S, Molinas C, Grandjean H. Endocrine disorders in children with Prader-Willi syndrome – data from 142 children of the French database. Horm Res Paediatr. 2010;74:121–8.
Vaiani E, Herzovich V, Chaler E, Chertkoff L, Rivarola M, Torrado M, et al. Thyroid axis dysfunction in patients with Prader-Willi syndrome during the first 2 years of life. Clin Endocrinol. 2010;73:546–50.
Goldstone AP, Holland AJ, Hauffa BP, Hokken-Koelega AC, Tauber M. Recommendations for the diagnosis and management of Prader-Willi Syndrome. J Clin Endocrinol Metab. 2008;93(11):4183–97.
Festen D, Visser T, Otten B, Wit J. Thyroid hormone levels in children with Prader–Willi syndrome before and during growth hormone treatment. Clin Endocrinol. 2007;67:449–56.
Bocchini S, Fintini D, Grugni G, Boiani A, Convertino A, Crinò A. Congenital hypothyroidism due to ectopic sublingual thyroid gland in Prader-Willi syndrome: a case report. Ital J Pediatr. 2017;43:87.
Sher C, Bistritzer T, Reisler G, Reish O. Congenital hypothyroidism with Prader-Willi syndrome. J Pediatr Endocrinol Metab. 2002;15:105–7.
Insoft RM, Hurvitz J, Estrella E, Krishnamoorthy KS. Prader-Willi syndrome associated with fetal goiter: a case report. Am J Perinatol. 1999;16:29–31 14.
Whittington JE, Holland AJ, Webb T, Butler J, Clarke D, Boer H. Population prevalence and estimated birth incidence and mortality rate for people with Prader-Willi syndrome in one UK Health Region. J Med Genet. 2001;38:792–8.
Stevenson DA, Anaya TM, Clayton-Smith J, Hall BD, van Allen MI, Zori RT, et al. Unexpected death and critical illness in Prader-Willi syndrome: Report of ten individuals. Am J Med Genet A. 2004;124:158–64.
Corrias A, Grugni G. Assessment of central adrenal insufficiency in children and adolescents with Prader-Willi syndrome. Clin Endocrinol. 2012;76:843–50.
Grugni G, Beccaria L, Corias A, Crino A, Cappa M, de Medici C, et al. Central adrenal insufficiency in young adults with Prader-Willi syndrome. Clin Endocrinol. 2013;79:371–8.
Beauloye V, Dhondt K, Buysse W, Nyakasane A. Evaluation of the hypothalamic-pituitaryadrenal axis and its relationship with central respiratory dysfunction in children with Prader-Willi syndrome. Orphanet J Rare Diss. 2015;10:106.
Connell, Paterson WF, Wallace AM, Donaldson MDC. Adrenal function and mortality in children and adolescents with Prader–Willi syndrome attending a single centre from 1991–2009. Clin Endocrinol. 2010;73:686–8.
Nyunt O, Cotterill AM, Archbold SM, Wu JY, Leong GM, Verge CF, et al. Normal cortisol response on low-dose synacthen (1 microg) test in children with Prader Willi syndrome. J Clin Endocrinol Metab. 2010;95:E464–7.
Farholt S, Sode-Carlsen R, Christiansen JS, Ostergaard JR, Hoybye C. Normal cortisol response to high dose synacthen and insulin tolerance test in children and adults with Prader-Willi syndrome. J Clin Endocrinol Metab. 2011;96:E173–80.
de Lind van Wijngaarden RFA, Joosten KFM, van den Berg S, Otten BJ. The relationship between central adrenal insufficiency and sleep-related breathing disorders in children with Prader-Willi syndrome. J Clin Endocrinol Metabol. 2009;94(7):2387–93.
Barbara DW, Hannon JD, Hartman WR. Intraoperative adrenal insufficiency in patients with Prader-Willi syndrome. J Clin Endocrinol Metab. 2008;93:1649–54.
Angulo MA, Butler MG, Cataletto ME. Prader Willi syndrome: a review of clinical, genetic, and endocrine findings. J Endocrinol Investig. 2015;38:1249–63. https://doi.org/10.1007/s40618-015-0312-9.
Heksch R, Kamboj M, Anglin K, Obrynba K. Review of Prader-Willi syndrome: the endocrine approach. Transl Pediatr. 2017;6(4):274–85. https://doi.org/10.21037/tp.2017.09.04.
Vogels A, Moerman P, Frijns JP, Bogaert GA. Testicular histology in boys with Prader-Willi syndrome: fertile or infertile? J Urol. 2008;180(1800–1804):113.
Siemensma EP, de Lind van Wijngaarden RF, Otten BJ, de Jong FH, Hokken-Koelega AC. Testicular failure in boys with Prader-Willi syndrome: longitudinal studies of reproductive hormones. J Clin Endocrinol Metab. 2012;97:E452–9 114.
Eldar-Geva T, Hirsch HJ, Rabinowitz R, Benarroch F, Rubinstein O, Gross-Tsur V. Primary ovarian dysfunction contributes to the hypogonadism in women with Prader-Willi syndrome. Horm Res. 2009;72(3):153–9 120.
Eldar-Geva T, Hirsch HJ, Benarroch F, Rubinstein O, GrossTsur V. Hypogonadism in females with Prader-Willi syndrome from infancy to adulthood: variable combinations of a primary gonadal defect and hypothalamic dysfunction. Eur J Endocrinol. 2010;162(2):377–84 121.
Radicioni AF, Di Giorgio G, Grugni G, Cuttini M, Losacco V, Anzuini A, et al. Multiple forms of hypogonadism of central, peripheral or combined origin in males with Prader-Willi syndrome. Clin Endocrinol (Oxf). 2012;76:72–7 115.
Eiholzer U, l’Allemand D, Rousson V, Schlumpf M, Gasser T, Girard J, et al. Hypothalamic and gonadal components of hypogonadism in boys with Prader-Labhart-Willi syndrome. J Clin Endocrinol Metab. 2006;91:892–8.
Crinò A, Schiaffini R, Ciampalini P, Spera S, Beccaria L, Benzi F, et al. Genetic obesity study Group of Italian Society of pediatric endocrinology and diabetology (SIEDP). Hypogonadism and pubertal development in Prader-Willi syndrome. Eur J Pediatr. 2003;162(5):327–33.
Bakker NE, Wolffenbuttel KP, Looijenga LH, Hokken-Koelega AC. Testes in infants with Prader-Willi syndrome: human chorionic gonadotropin treatment, surgery and histology. J Urol. 2015;193(1):291–8.
Fillion M, Deal CL, Van Vliet G. Normal minipuberty of infancy in boys with Prader-Willi syndrome. J Pediatr. 2006;149(874–876):117.
Hirsch HJ, Eldar-Geva T, Benarroch F, Rubinstein O, Gross-Tsur V. Primary testicular dysfunction is a major contributor to abnormal pubertal development in males with Prader-Willi syndrome. J Clin Endocrinol Metab. 2009;94(7):2262–8.
Hirsch HJ, Eldar-Geva T, Erlichman M, Pollak Y, Gross-Tsur V. Characterization of minipuberty in infants with PraderWilli syndrome. Horm Res Paediatr. 2014;82(230–237):118.
Brandau DT, Theodoro M, Garg U, Butler MG. Follicle stimulating and leutinizing hormones, estradiol and testosterone in Prader-Willi syndrome. Am J Med Genet A. 2008;146A(5):665–9.
Hirsch HJ, Eldar-Geva T, Bennaroch F, Pollak Y, Gross-Tsur V. Sexual dichotomy of gonadal function in Prader-Willi syndrome from early infancy through the fourth decade. Hum Reprod. 2015;30(11):2587–96.
Gross-Tsur V, Hirsch HJ, Benarroch F, et al. The FSH-inhibin axis in Prader-Willi syndrome: heterogeneity of gonadal dysfunction. Reprod Biol Endocrinol. 2012;10:39. https://doi.org/10.1186/1477-7827-10-39.
Hirsch HJ, Eldar-Geva T, Erlichman M, Pollak Y, Gross-Tsur V. Characterization of minipuberty in infants with Prader Willi syndrome. Horm Res Paediatr. 2014;82(230–237):118.
Eldar-Geva T, Hirsch HJ, Pollak Y, Benarroch F, Gross-Tsur V. Management of hypogonadism in adolescent girls and adult women with Prader-Willi syndrome. Am J Med Genet A. 2013;161A:3030–4.
Akefeldt A, Tornhage CJ, Gillberg C. A woman with Prader-Willi syndrome gives birth to a healthy baby girl. Dev Med Child Neurol. 1999;41(789–790):122.
Schulze A, Mogensen H, Hamborg-Petersen B, Graem N, Ostergaard JR, Brondum-Nielsen K. Fertility in PraderWilli syndrome: a case report with Angelman syndrome in the offspring. Acta Paediatr. 2001;90(455–459):123.
Schmidt H, Schwarz PS. Premature adrenarche, increased growth velocity and accelerated bone age in male patients with Prader-Labhart-Willi syndrome. Eur J Pediatr. 2001;160(69–70):124.
Butler MG, Haber L, Mernaugh R, Carlson MG, Price R, Feurer ID. Decreased bone mineral density in PraderWilli syndrome: comparison with obese subjects. Am J Med Genet. 2001;103(216–222):127.
Vestergaard P, Kristensen K, Bruun JM, Østergaard JR, Heickendorff L, Mosekilde L, et al. Reduced bone mineral density and increased bone turnover in Prader-Willi syndrome compared with controls matched for sex and body mass index—a cross-sectional study. J Pediatr. 2004;144(5):614–9 128.
Young J. Approach to the male patient with congenital hypogonadotropic hypogonadism. J Clin Endocrinol Metab. 2012;97:707–18.
Bridges N. What is the value of growth hormone therapy in Prader Willi syndrome? Arch Dis Child. 2014;99:166–70.
Petriczko E, Horodnicka-Józwa A, Szmit-Domagalska J, et al. Aspekty endokrynne zespołu Pradera i Williego u dzieci i młodzieży. Pediatr Pol. 2008;83(5):522–8.
Cohen M, Harrington J, Narang I, Hamilton J. Growth hormone secretion decreases with age in paediatric Prader-Willi syndrome. Clin Endocrinol. 2015;83:212–5.
Di Giorgio G, Grugni G, Fintini D, et al. Growth hormone response to standard provocative stimuli and combined tests in very young children with Prader-Willi syndrome. Horm Res Paediatr. 2014;81:189–95.
Deal CL, Tony M, Hoybye C, et al. Growth hormone in Prader Willi syndrome clinical care guidelines workshop participants. Growth Hormone Research Society workshop summary: consensus guidelines for recombinant human growth hormone therapy in PraderWilli syndrome. J Clin Endocrinol Metab 2013. 2013;98:E1072–e87.
Miller JL, Goldstone AP, Couch JA, Shuster J, He G, Driscoll DJ, et al. Pituitary abnormalities in Prader-Willi syndrome and early onset morbid obesity. Am J Med Genet A. 2008;146A:570–7.
Cassidy SB, Schwartz S, Miller JL, et al. Prader Willi syndrome. Genet Med. 2012;14:10e26.
Góralska M, Bednarczuk T, Rosłon M, Libura M, Szalecki M, Hilczer M, et al. Management of Prader-Willi Syndrome (PWS) in adults - what an endocrinologist needs to know. Recommendations of the Polish Society of Endocrinology and the Polish Society of Paediatric Endocrinology and Diabetology. Endokrynol Pol. 2018;69.
Grugni G, Marzullo P. Diagnosis and treatment of GH deficiency in Prader-Willi syndrome. Best Pract Res Clin Endocrinol Metab. 2016;30(6):785–94.
Lafortuna CL, Minocci A, Capodaglio P, et al. Growth hormone therapy improves exercise capacity in adult patients with Prader-Willi syndrome. J Endocrinol Investig. 2008;31(9):765–72.
Siemensma EP, de Lind van Wijngaarden RF, Festen DA, et al. Beneficial effects of growth hormone treatment on cognition in children with Prader-Willi syndrome: a randomized controlled trial and longitudinal study. J Clin Endocrinol Metab. 2012;97:2307–14.
Höybye C, Thorén M, Böhm B. Cognitive, emotional, physical and social effects of growth hormone treatment in adults with Prader-Willi syndrome. J Intellect Disabil Res. 2005;49(Pt 4):245–52.
Sode-Carlsen R, Farholt S, Rabben KF, et al. One year of growth hormone treatment in adults with Prader-Willi syndrome improves body composition: results from a randomized, placebo-controlled study. J Clin Endocrinol Metab. 2010;95(11):4943–50.
Deal CL, Tony M, Höybye C, Allen DB, Tauber M, Christiansen JS, et al. Growth Hormone Research Society workshop summary: consensus guidelines for recombinant human growth hormone therapy in Prader-Willi syndrome. J Clin Endocrinol Metab. 2013;98:E1072–87.
Festen DA, de Lind van Wijngaarden R, van Eekelen M, et al. Randomized controlled GH trial: effects on anthropometry, body composition and body proportions in a large group of children with Prader-Willi syndrome. Clin Endocrinol (Oxf). 2008;69:443–5.
Bakker NE, Kuppens RJ, Siemensma EP, Wijngaarden RF, Festen DA, Bindels-de Heus GC, et al. Eight years of growth hormone treatment in children with Prader-Willi syndrome: maintaining the positive effects. J Clin Endocrinol Metab. 2013;98:4013–22.
Colmenares A, Pinto G, Taupin P, Giuseppe A, Odent T, Trivin C, et al. Effects on growth and metabolism of growth hormone treatment for 3 years in 36 children with Prader-Willi syndrome. Horm Res Paediatr. 2011;75:123–30.
Myers SE, Whitman BY, Carrel AL, Moerchen V, Bekx MT, Allen DB. Two years of growth hormone therapy in young children with Prader-Willi syndrome: physical and neurodevelopmental benefits. Am J Med Genet A. 2007;143A:443–8.
Carrel AL, Myers SE, Whitman BY, Allen DB. Benefits of long-term GH therapy in Prader-Willi syndrome: a 4-year study. J Clin Endocrinol Metab. 2002;87:1581–5.
Passone CBG, Pasqualucci PL, Franco RR, Ito SS, Mattar LBF, Koiffmann CP, et al. Prader-Willi syndrome: what is the general pediatrician supposed to do? A review. Rev Paul Pediatr. 2018;36(3):345–52.
Van Vliet G, Deal CL, Crock PA, et al. Sudden death in growth hormone-treated children with Prader-Willi syndrome. J Pediatr. 2004;144:129–31.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Muscogiuri, G., Formoso, G., Pugliese, G. et al. Prader- Willi syndrome: An uptodate on endocrine and metabolic complications. Rev Endocr Metab Disord 20, 239–250 (2019). https://doi.org/10.1007/s11154-019-09502-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11154-019-09502-2