Abstract
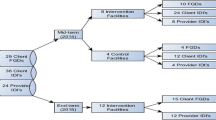
Objectives In order to improve maternal and neonatal outcomes, it is important to understand how to maximise the utilisation of MNCH services. The supply side (service-driven) factors affecting access to MNCH services are more commonly studied and are better understood than the demand side (community led) factors. The aim of this study was to identify demand and supply determinants of access to MNCH services in Malawi. Methods Research was conducted in two districts of the Central Region of Malawi (Nkhotakota & Mchinji). Qualitative interviews (n = 85) and focus group discussions (n = 20) were conducted with a range of community members, leaders and health workers. Data were managed in NVivo (v10) and analysed using framework analysis, using Levesque et al. (2013) access framework. Results Community members clearly recognise their need for and seek out MNCH care from the formal health system. Women experience difficulties reaching health services and when reached find them limited, characterised by many indirect costs. There are many technical and interpersonal deficits, which results in poor satisfaction and reportedly poor outcomes for women. Conclusions for practice Women are seeking and utilising MNCH services which they find under-resourced and unwelcoming. Utilising the Levesque et al. (2013) framework, a granular analysis of demand and supply factors has identified the many challenges that remain to achieving equitable access to MNCH services in Malawi. Community members experience lack of availability, acceptability and appropriateness of these essential services.

Similar content being viewed by others
References
Bailie, J., Schierhout, G., Laycock, A., et al. (2015). Determinants of access to chronic illness care: A mixed-methods evaluation of a national multifaceted chronic disease package for Indigenous Australians. British Medical Journal Open, 5, e008103. https://doi.org/10.1136/bmjopen-2015-008103.
Bisika, T. (2008). The effectiveness of the TBA programme in reducing maternal mortality and morbidity in Malawi. East African Journal of Public Health, 5(2), 103–110.
Brenner, S., Wilhelm, D., Lohmann, J., Kambala, C., Chinkhumba, J., Muula, A. S., et al. (2017). Implementation research to improve quality of maternal and newborn health care, Malawi. Bulletin of the World Health Organization, 95(7), 491–502.
Butrick, E., Diamond-Smith, N., Beyeler, N., Montagu, D., Sudhinaraset, M. (2014). Strategies to increase health facility deliveries: Three case studies. Global Health Group, Global Health Sciences, University of California, San Francisco. Retrieved June 17, 2019 from https://globalhealthsciences.ucsf.edu/sites/globalhealthsciences.ucsf.edu/files/pub/pshi-strategies-to-increase-health-facility-deliveries.pdf.
Campbell, Oona, M. R., et al. (2016). The scale, scope, coverage, and capability of childbirth care. The Lancet, 388(10056), 2193–2208.
Chanza, D., Chirwa, E., Maluwa, A., Malata, A., & Masache, G. (2012). Factors affecting the choice for home deliveries in Malawi. African Journal of Midwifery and Women’s Health, 6(3), 125–130.
Godlonton, S., & Okeke, E. N. (2016). Does a ban on informal health providers save lives? Evidence from Malawi. Journal of Development Economics, 118, 112–132.
ILO. (2014). World Social Protection Report 2014/15. Retrieved June 17, 2019 from https://www.ilo.org/wcmsp5/groups/public/—dgreports/—dcomm/documents/publication/wcms_245201.pdf.
Kerr, R. B., Dakishoni, L., Shumba, L., Msachi, R., & Chiwa, M. (2008). “We grandmothers know plenty”: Breastfeeding, complementary feeding and the multifaceted role of grandmothers in Malawi. Social Science and Medicine, 66(5), 1095–1105.
Koblinsky, M., et al. (2016). Quality maternity care for every woman, everywhere: A call to action. The Lancet, 388, 2307–2320.
Koenraads, M., Phuka, J., Maleta, K., et al. (2017). Understanding the challenges to caring for low birthweight babies in rural southern Malawi: A qualitative study exploring caregiver and health worker perceptions and experiences. BMJ Global Health, 2, e000301.
Kumbani, L., Bjune, G., Chirwa, E., Malata, A., & Odland, J. O. (2013). Why some women fil to give birth ay health facilities: A qualitative study of women’s perceptions of perinatal care in rural South Malawi. Reproductive Health, 10(1), 1. https://doi.org/10.1186/1742-4755-10-9.
Kumbani, L. C., Chirwa, E., Malata, A., Odland, J. Ø., & Bjune, G. (2012). Do Malawian women critically assess the quality of care? A qualitative study on women’s perceptions of perinatal care at a district hospital in Malawi. Reproductive Health, 9(1), 30.
Levesque, J., Harris, M., & Russell, G. (2013). Patient-centred access to healthcare: Conceptualising access at the interface of health systems and populations. International Journal of Equity in Health, 12, 18. https://doi.org/10.1186/1475-9276-12-18.
Ministry of Health of Malawi. (2011). Malawi Health Sector Strategic Plan (HSSP, 2011–2016). Retrieved June 17, 2019 from http://www.nationalplanningcycles.org/sites/default/files/country_docs/Malawi/2_malawi_hssp_2011_-2016_final_document_1.pdf.
National Statistical Office (NSO) [Malawi] and ICF. (2017). Malawi Demographic and Health Survey 2015–16. Zomba, Malawi, and Rockville, Maryland, USA. NSO and ICF. Retrieved April 1, 2019 from https://dhsprogram.com/pubs/pdf/FR319/FR319.pdf.
Rishworth, A., Dixon, J., Luginaah, I., Mkandawire, P., & Prince, C. T. (2016). ‘I was on the way to the hospital but delivered in the bush’: Maternal health in Ghana’s upper west region in the context of a traditional birth attendants’ ban. Social Science and Medicine, 148, 8–17. https://doi.org/10.1016/j.socscimed.2015.11.018.
Sialubanje, C., Massar, K., Hamer, D. H., & Ruiter, R. A. C. (2015). Reasons for home delivery and use of traditional birth attendants in rural Zambia: A qualitative study. BMC Pregnancy and Childbirth, 15, 216.
UNICEF. (2016). Maternal and Newborn Health Disparities. Retrieved June 17, 2019 from https://data.unicef.org/wp-content/uploads/country_profiles/Malawi/country%20profile_MWI.pdf
Uny, I. (2017). Weighing the options for delivery care in rural Malawi: Community actors’ perceptions of the 2007 policy guidelines and redefined Traditional Birth Attendants’ roles. PhD thesis. Queen Margaret University. Retrieved June 17, 2019 from https://eresearch.qmu.ac.uk/bitstream/handle/20.500.12289/7469/2618.pdf?sequence=1&isAllowed=y.
Walsh, A., Matthews, A., Manda-Taylor, L., Brugha, R., Mwale, D., Phiri, T., Phiri, T., & Byrne, E. (2018). The role of the traditional leader in implementing maternal, newborn and child health policy in Malawi. Health Policy and Planning, 33(8), 879–887.
WHO. (2018). Global Health Observatory data repository. Retrieved June 17, 2019 from http://apps.who.int/gho/data.
Yaya, S., Bishwajit, G., Uthman, O. A., & Amouzou, A. (2018). Why some women fail to give birth at health facilities: A comparative study between Ethiopia and Nigeria. PLoS ONE, 13(5), e0196896. https://doi.org/10.1371/journal.pone.0196896.
Yuan, E. D., Cherukuri, A. R., Ssembatya, R., Naylor, M. R., & DeStigter, K. K. (2017). An open conversation with traditional birth attendants in rural Uganda: The potential for collaborative care. Journal of Global Radiology, 3(1), 3.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Matthews, A., Walsh, A., Brugha, R. et al. The Demand and Supply Side Determinants of Access to Maternal, Newborn and Child Health Services in Malawi. Matern Child Health J 23, 1556–1563 (2019). https://doi.org/10.1007/s10995-019-02791-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-019-02791-8