Abstract
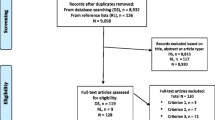
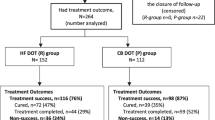
In many develo** countries, Directly Observed Therapy (DOT) for tuberculosis has been undertaken mainly in the clinic setting. However, clinic-based DOT may create a high patient load in already overburdened health facilities and increase barriers to care by requiring patients to travel to clinic frequently for therapy. Community-based DOT (CBDOT) may overcome some of these problems. This aims of this review are (a) to describe the main features of CBDOT programs, and (b) to compare features and outcomes of CBDOT programs that do and do not offer financial reward for CBDOT providers. Ten major features define CBDOT program structure and function. Programs that paid their CBDOT providers tended to differ from unpaid programs based on all of these features. CBDOT programs in which providers received financial reward had success rates of 85.7 versus 77.6% in programs without financial reward for providers. This difference was not statistically significant. CBDOT programs fall into two major archetypes, which differ in their structure and possibly in their outcomes.



Similar content being viewed by others
References
WHO. (2006). Global tuberculosis control: surveillance, planning, financing (p. 39). WHO report (2006). Geneva: World Health Organization (WHO/HTM/TB/2006.362). http://www.who.int/tb/publications/global_report/en/.
WHO. (2006). Global tuberculosis control: surveillance, planning, financing (p. 54) WHO report 2006. Geneva: World Health Organization (WHO/HTM/TB/2006.362). http://www.who.int/tb/publications/global_report/en/.
Gupta, S., Berg, D., De Lott, F., Kellner, P., & Driver, C. (2004). Directly observed therapy for tuberculosis in New York City: Factors associated with refusal. International Journal of Tuberculosis and Lung Disease, 8, 480–485.
Khan, M., Walley, J., Witter, S., Shah, S., & Javeed, S. (2005). Tuberculosis patient adherence to direct observation: Results of a social study in Pakistan. Health Policy and Planning, 20(6), 354–365.
Maher, D., Floyd, K., Sharma, B. V. et al. (2003). Community contribution to TB care: Practice and policy review of experience of community contribution to TB care and recommendations to national TB programs. WHO report 2003.
World Health Organization. (2006). The Global Plan to Stop TB, 2006–2015. Part III (p. 116). Geneva: World Health Organization, 2006 (WHO/HTM/STB/2006.35).
Faustini, A., Hall, A., & Perucci, C. A. (2005). Tuberculosis treatment outcomes in Europe: A systematic review. European Respiratory Journal, 26, 503–510.
Barker, R. D., Millard, F. J. C., & Nthangeni, M. E. (2002). Unpaid community volunteers-effective providers of directly observed therapy (DOT) in rural South Africa. South African Medical Journal, 92, 291–294.
Walley, J., Khan, M. A., Newel, J. N., & Khan, M. H. (2001). Effectiveness of the direct observation component of DOTS for tuberculosis: A randomized controlled trial in Pakistan. Lancet, 357, 664–669.
Khan, M. A., Walley, J., Witter, S. N., et al. (2002). Costs and cost-effectiveness of different DOT strategies for the treatment of tuberculosis in Pakistan. Health Policy and Planning, 17(2), 178–186.
Dudley, L., Azevedo, V., Grant, R., Schoeman, J. H., Dikweni, L., & Maher, D. (2003). Evaluation of community contribution to tuberculosis control in Cape Town, South Africa. The International Journal of Tuberculosis and Lung Disease, 9(Suppl 1), S48–S55.
Sinanovic, E., Floyd, K., Dudley, L., et al. (2003). Cost and cost-effectiveness of community-based care for tuberculosis in Cape Town, South Africa. The International Journal of Tuberculosis and Lung Disease, 7(9), S56–S62.
Mathew, A., Binks, C., Kuruvilla, J., et al. (2005). A comparison of two methods of undertaking directly observed therapy in a rural Indian setting. The International Journal of Tuberculosis and Lung Disease, 9(1), 69–74.
Wandwalo, E., Kapalata, N., Egwaga, S., & Morkve, O. (2004). Effectiveness of community-based directly observed treatment for tuberculosis in an urban setting in Tanzania: A randomised controlled trial. The International Journal of Tuberculosis and Lung Disease, 10, 1248–1254.
Zwarenstein, M., Schoeman, J. H., Lombard, C. J., et al. (2000). A randomized controlled trial of lay health workers as direct observers for treatment of tuberculosis. The International Journal of Tuberculosis and Lung Disease, 4, 550–554.
Dick, J., & Schoeman, J. H. (1996). Tuberculosis in the community: 1. Evaluation of a volunteer health worker program to enhance adherence to anti-tuberculosis treatment. Tubercle and Lung Disease, 77, 247–249.
Dick, J., Schoeman, J. H., Mohammed, A., et al. (1996). Tuberculosis in the community: 2. The perceptions of members of a tuberculosis health team towards a voluntary health worker program. Tubercle and Lung Disease, 77, 380–383.
Arora, V. K., Singla, N., & Gupta, R. (2003). Community meidated domicilliary DOTS execution: A study from New Delhi. Indian Journal of Tuberculosis, 50, 143.
Akkslip, S., Rasmithat, S., Maher, D., et al. (1999). Direct observation of TB treatment by supervised family members in Yasothorn Province Thailand. The International Journal of Tuberculosis and Lung Disease, 2(12), 1061–1065.
Becx-Bleumink, M., Djamaluddin, S., Loprang, Z. F., de Soldenhoff, R., Wibowo, H., & Aryono, M. (1999). High cure rates in smear positive TB patients using ambulatory treatment with once-weekly supervision during the intensive phase in Sulawesi, Republic of Indonesia. The International Journal of Tuberculosis and Lung Disease, 3, 1066–1072.
Becx-Bleumink, M., Wibowo, H., Apriani, W., & Vrakking, H. (2001). High TB notification and treatment success rates through community participation in central Sulawesi, Republic of Indonesia. The International Journal of Tuberculosis and Lung Disease, 5, 920–925.
Adatu, F., Odeke, R., Mugenyi, M., et al. (2003). Implementation of the DOTS strategy for tuberculosis control in rural Kiboga District, Uganda, offering patients the option of treatment supervision in the community, 1998–1999. The International Journal of Tuberculosis and Lung Disease, 7(9), S63–S71.
Okello, D., Floyd, K., Adatu, F., et al. (2003). Cost and cost-effectiveness of community-based care for tuberculosis patients in rural Uganda. The International Journal of Tuberculosis and Lung Disease, 7(9), S72–S79.
Manalo, F., Tan, F., Sbarbaro, J. A., et al. (1990). Community-based short-course treatment of pulmonary TB in a develo** nation. The American Review of Respiratory Disease, 142, 1301–1305.
Clarke, M., Dick, J., Zwarenstein, M., et al. (2004). Lay health worker intervention with choice of DOT superior to standard TB care for farm dwellers in South Africa: A cluster randomized control trial. The International Journal of Tuberculosis and Lung Disease, 9(6), 673–679.
Chowdhury, A. M., Chowdhury, S., Islam, M. D. N., et al. (1997). Control of tuberculosis by community health workers in Bangladesh. Lancet, 350, 169–172.
Chowdhury, A. M. R., Alam, A., Chowdhury, S. A., & Ahmed, J. (1992). Tuberculosis control in Bangladesh. Lancet, 339, 1181–1182.
Chowdhury, A. M. (1999). Success with the DOTS strategy. Lancet, 353, 1003–1004.
Chowdhury, A. M. (2003). Health workforce for TB control by DOTS: The BRAC case. Joint learning initiative: Human resources for health and development 2003.
Kamolratanakul, P., Sawert, H., Lertmaharit, S., et al. (1999). Randomized controlled DOT with pulmonary TB in Thailand. Transactions of the Royal Society of Tropical Medicine and Hygiene, 93, 552–557.
China Tuberculosis Control Collaboration. (1996). Results of directly observed short-course chemotherapy in 112,842 Chinese patients with smear-positive tuberculosis. Lancet, 347, 358–362.
Singh, A. A., Parasher, D., Shekhavat, G. S., Sahu, S., Wares, D. F., & Granich, R. (2004). Effectiveness of urban community volunteers in directly observed treatment of tuberculosis patients: A field report from Haryana, North India. The International Journal of Tuberculosis and Lung Disease, 8(6), 800–802.
Moalosi, G., Floyd, K., Phatshwane, J., et al. (2003). Cost-effectiveness of home-based care versus hospital care for chronically ill tuberculosis patients, Francistown, Botswana. The International Journal of Tuberculosis and Lung Disease, 7(9), S80–S85.
Miti, S., Mfungwe, V., Reijer, P., et al. (2003). Integration of tuberculosis treatment in a community-based home care program for persons living with HIV/AIDS in Ndola, Zambia. The International Journal of Tuberculosis and Lung Disease, 7(9), S92–S98.
Nsutebu, E. F., Walley, J., Mataka, E., et al. (2001). Scaling up HIV/AIDS and TB Home-based care: Lessons from Zambia. Health Policy and Planning, 16(3), 240–247.
Wright, J., Walley, J., Philip, A., Pushpanathan, S., Dlamini, E., Dlamini, S., et al. (2004). Direct Observation of treatment for tuberculosis: A randomized controlled trial of community health workers versus family members. Tropical Medicine & International Health, 9(4), 559–565.
Escott, S., Walley, J. (2005). Listening to those on the frontline: Lessons for community-based tuberculosis programs from a qualitative study in Swaziland. Social Science and Medicine, 61(8), 1701–1710.
Olle-Goig, J. E., & Alvarez, J. (2001). Treatment of tuberculosis in a rural area of Haiti: Directly observed and non-observed regiments. The experience of Hopital Albert Schweitzer. The International Journal of Tuberculosis and Lung Disease, 5(2), 137–141.
Kironde, S., & Kahirimbanyi, M. (2002). Community participation in primary health care (PHC) programmes: Lessons from tuberculosis treatment delivery in South Africa. African Health Sciences, 2(1), 16–23.
Kironde, S., & Neil, S. (2004). Indigenous NGO involvement in TB treatment programmes in high-burden settings: Experiences from the Northern Cape province, South Africa. The International Journal of Tuberculosis and Lung Disease, 8(4), 504–508.
Garner, P., & Volmink, J. (1997). Directly observed therapy. Lancet, 350, 666.
Garner, P., & Volmink, J. (2000). Directly observed therapy and treatment adherence. Lancet, 355, 1345–1349.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kangovi, S., Mukherjee, J., Bohmer, R. et al. A Classification and Meta-analysis of Community-based Directly Observed Therapy Programs for Tuberculosis Treatment in Develo** Countries. J Community Health 34, 506–513 (2009). https://doi.org/10.1007/s10900-009-9174-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-009-9174-4