Abstract
Purpose
To evaluate the causes of IOL explantation, techniques for secondary IOL implantation, visual outcomes and complications.
Methods
Setting: Department of Ophthalmology Complexo Hospitalario Universitario A Coruña, Spain. Design: Retrospective study. All explanted IOLs from January 2010 to June 2018 were included. Medical records were reviewed to determine the surgical indication for IOL explantation, type of IOL implanted, time between surgeries, visual outcomes and surgical complications.
Results
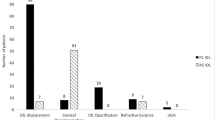
One hundred forty-one IOLs were explanted (134 patients). Mean time from original surgery to IOL explantation was 7.89 ± 5.81 years. Causes of IOL explantation were IOL dislocation (81.56%)—in-the-bag IOL dislocation (71.63%), out-of-the-bag IOL dislocation (9.9%)—corneal decompensation (12.05%), refractive surprise (3.5%), uveitis-glaucoma-hyphema syndrome (1.4%), IOL opacification (1.4%). Procedures for secondary IOL implantation were retropupillar iris-claw IOL (63.8%), flanged scleral fixated IOL (9.2%), three-piece IOL in ciliary sulcus (8.5%), angle-supported anterior chamber IOL (7.1%), in-the-bag IOL (3.5%), scleral fixated IOL with sutures (0.7%). Ten cases (7.1%) were left aphakic. Mean preoperative and postoperative logMAR CDVA were 1.34 ± 0.87 and 0.63 ± 0.69, respectively (p = 0.000). Mean preoperative IOP and postoperative IOP were 16.78 ± 4.49 and 15.53 ± 3.476 mmHg, respectively (p = 0.005). Complications include cystoid macular edema (7.8%), glaucoma (7.1%), IOL luxation (2.1%), retinal detachment (1.4%), trophic ulcer and leucoma (1.4%), corneal decompensation (1.4%).
Conclusions
In-the-bag IOL dislocation was the most frequent indication for IOL explantation, followed by pseudophakic bullous keratopathy. Simultaneous IOL exchange for a retropupillar iris-claw IOL was the most frequent procedure for secondary IOL implantation. Mean CDVA improved significantly and IOP decreased significantly after IOL explantation. The most frequent postoperative complication was cystoid macular edema.



Similar content being viewed by others
References
Chan TC, Lok JK, Jhanji V, Wong VW (2015) Intraocular lens explantation in Chinese patients: different patterns and different responses. Int Ophthalmol 35:679–684
Jones J, Jones YJ, ** GJC (2014) Indications and outcomes of intraocular lens exchange during a recent 5-year period. Am J Ophthalmol 157:154–162
Fernández-Buenaga R, Alió JL, Muñoz Negrete J, Barraquer RI, Alió del Barrio JL (2012) Causes of IOL explantation in Spain. Eur J Ophthalmol 22:762–768
** GJC, Crandall AS, Jones JJ (2005) Changing indications for and improving outcomes of intraocular lens exchange. Am J Ophthalmol 140:688–694
Doren GS, Stern GA, Driebe WT (1992) Indications for and results of intraocular lens explantation. J Cataract Refract Surg 18:79–85
Mamalis N, Crandall AS, Pulsipher MW, Follett S, Monson MC (1991) Intraocular lens explantation and exchange. A review of lens styles, clinical indications, clinical results, and visual outcome. J Cataract Refract Surg 17:811–818
Mamalis N, Davis B, Nilson CD, Hickman MS, Leboyer RM (2004) Complications of foldable intraocular lenses requiring explantation or secondary intervention—2003 survey update. J Cataract Refract Surg 30:2209–2218
Mamalis N, Brubaker J, Davis D, Espandar L, Werner L (2008) Complications of foldable intraocular lenses requiring explantation or secondary intervention—2007 survey update. J Cataract Refract Surg 34:1584–1591
Marques FF, Marques DM, Osher RH, Freitas LL (2007) Longitudinal study of intraocular lens exchange. J Cataract Refract Surg 33:254–257
Davies EC, Pineda R II (2016) Intraocular lens exchange surgery at a tertiary referral: indications, complications, and visual outcomes. J Cataract Refract Surg 42:1262–1267
Lyle WA, ** JCh (1992) An analysis of intraocular lens exchange. Ophthalmic Surgery 23:7
Leysen I, Bartholomeeusen E, Coeckelbergh T, Tassignon MJ (2009) Surgical outcomes of intraocular lens exchange five-year study. J Cataract Refract Surg 35:1013–1018
Jirásková N, Rozsíval P, Kohout A (2007) A survey of intraocular lens explantation: a retrospective analysis of 23 IOLs explanted during 2005. Eur J Ophthalmol 17:579–587
Oltulu R, Erşan I, Şatırtav G, Donbaloglu M, Kerimoğlu H, Özkağnıcı A (2015) Intraocular lens explantation or exchange: indications, postoperative interventions, and outcomes. Arq Bras Oftalmol 78:154–157
Chai F, Ma B, Yang XG, Li J, Chu MF (2017) A pilot study of intraocular lens explantation in 69 eyes in Chinese patients. Int J Ophthalmol 10:579–585
Dick HB, Augustin AJ (2001) Lens implant selection with absence of capsular support. Curr Opin Ophthalmol 12:47–57
Sorenson R, Scott IU, Tucker SH, Chinchilli UM, Papachristu GC (2016) Practice patterns of cataract surgeons at academic medical s for the management of inadequate capsular support for intracapsular or sulcus intraocular lens placement during cataract surgery. J Cataract Refract Surg 42:239–245
Lorente R, de Rojas V, Vázquez de Parga P, Moreno C, Landaluce ML, Domínguez R, Lorente B (2010) Management of late spontaneous in-the-bag intraocular lens dislocation: retrospective analysis of 45 cases. J Cataract Refract Surg 36:1270–1282
Govetto A, Lorente R, Vázquez de Parga P, Rojas L, Moreno C, Lagoa F, Lorente B (2015) Frequency of pseudoexfoliation among patients scheduled for cataract surgery. J Cataract Refract Surg 41:1224–1231
Jakobsson G, Zetterberg M, Lundström M, Stenevi U, Grenmark R, Sundelin K (2010) Late dislocation of in-the bag and out-of-the bag intraocular lenses: ocular and surgical characteristics and time to lens repositioning. J Cataract Refract Surg 36:1637–1644
Kim SS, Smiddy WE, Feuer W, Shi W (2008) Management of dislocated intraocular lenses. Ophthalmology 115:1699–1704
Hayashi K, Hirata A, Hayashi H (2007) Possible predisposing factors for in-the-bag and out-of-the-bag intraocular lens dislocation and outcomes of intraocular lens exchange surgery. Ophthalmology 114:969–975
Neuhann IM, Kleinmann G, Apple DJ (2008) A new classification of calcification of intraocular lenses. Ophthalmology 115:73–79
Chang DF, Masket S, Miller KM, Braga-Mele R, Little BC, Mamalis N, Oetting TA, Packer M (2009) Complications of sulcus placement of single-piece acrylic intraocular lenses Recommendations for backup IOL implantation following posterior capsule rupture for the ASCRS Cataract Clinical Committee. J Cataract Refract Surg 35:1445–1458
Forlini M, Soliman W, Bratu A, Rossini P, Cavallini GM, Forlini C (2015) Long-term follow-up of retropupillary iris-claw intraocular lens implantation: a retrospective analysis. BMC Ophthalmology 15:143
Yamane S, Sato S, Maruyama-Inoue M, Kadonosono K (2017) Flanged intrascleral intraocular lens fixation with double-needle technique. Ophthalmology 124:1136–1142
Wagoner MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL (2003) Intraocular lens implantation in the absence of capsular support. A report by the American Academy of Ophthalmology. Ophthalmology 110:840–859
D’Amico DJ (2016) Different preferences between United States and European vitreoretinal surgeons: personal observations. Curr Opin Ophthalmol 27:196–200
Lorente B, de Rojas MV, Lorente R (2019) Intraocular pressure changes before and after surgery for spontaneous in the bag intraocular lens dislocation. J Cataract Refract Surg 45:305–311
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights statement
Given the retrospective nature of the research design, informed consent and institutional review board approval were unnecessary.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Rojas, M., Viña, S., Gestoso, A. et al. Intraocular lens explantation in Spain: indications and outcomes at a tertiary referral center from 2010 to 2018. Int Ophthalmol 40, 313–323 (2020). https://doi.org/10.1007/s10792-019-01181-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-019-01181-x