Abstract
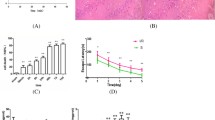
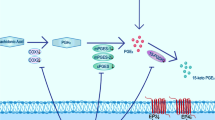
Stroke is an acute central nervous system disease with high morbidity and mortality rate. Cerebral ischemia reperfusion (I/R) injury is easily induced during the development or treatment of stroke and subsequently leads to more serious brain damage. Prostaglandin E2 (PGE2) is one of the most important inflammatory mediators in the brain and contributes to both physiological and pathophysiological functions. It may be upregulated and subsequently plays a key role in cerebral ischemia reperfusion injury. The synthesis and degradation of PGE2 is an extremely complex process, with multiple key stages and molecules. However, there are few comprehensive and systematic studies conducted to investigate the synthesis and degradation of PGE2 during cerebral I/R injury, which is what we want to demonstrate. In this study, qRT-PCR and immunoblotting demonstrated that the key enzymes in PGE2 synthesis, including COX-1, COX-2, mPGES-1 and mPGES-2, were upregulated during cerebral I/R injury, but 15-PGDH, the main PGE2 degradation enzyme, was downregulated. In addition, two of PGE2 receptors, EP3 and EP4, were also increased. Meanwhile, immunohistochemistry demonstrated the localization of these molecules in ischemic areas, including cortex, striatum and hippocampus, and reflected their expression patterns in different regions. Combining the results of PCR, Western blotting and immunohistochemistry, we can determine where the increase or decrease of these molecules occurs. Overall, these results further indicate a possible pathway that mediates enhanced production of PGE2, and thus that may impact production of inflammatory cytokines including IL-1β and TNF-α during cerebral I/R injury.







Similar content being viewed by others
References
Allen CL, Bayraktutan U (2009) Oxidative stress and its role in the pathogenesis of ischaemic stroke. Int J Stroke 4(6):461–470. https://doi.org/10.1111/j.1747-4949.2009.00387.x
Amantea D, Nappi G, Bernardi G, Bagetta G, Corasaniti MT (2009) Post-ischemic brain damage: pathophysiology and role of inflammatory mediators. Febs j 276(1):13–26. https://doi.org/10.1111/j.1742-4658.2008.06766.x
Anrather J, Iadecola C (2016) Inflammation and Stroke: An Overview. Neurotherapeutics 13(4):661–670. https://doi.org/10.1007/s13311-016-0483-x
Ashwal S, Tone B, Tian HR, Cole DJ, Pearce WJ (1998) Core and penumbral nitric oxide synthase activity during cerebral ischemia and reperfusion. Stroke 29 (5):1037–1046; discussion 1047
Basbaum AI, Bautista DM, Scherrer G, Julius D (2009) Cellular and molecular mechanisms of pain. Cell 139(2):267–284. https://doi.org/10.1016/j.cell.2009.09.028
Caggiano AO, Kraig RP (1999) Prostaglandin E receptor subtypes in cultured rat microglia and their role in reducing lipopolysaccharide-induced interleukin-1beta production. J Neurochem 72(2):565–575. https://doi.org/10.1046/j.1471-4159.1999.0720565.x
Calvello R, Panaro MA, Carbone ML, Cianciulli A, Perrone MG, Vitale P, Malerba P, Scilimati A (2012) Novel selective COX-1 inhibitors suppress neuroinflammatory mediators in LPS-stimulated N13 microglial cells. Pharmacol Res 65(1):137–148. https://doi.org/10.1016/j.phrs.2011.09.009
Cha YI, Solnica-Krezel L, DuBois RN (2006) Fishing for prostanoids: deciphering the developmental functions of cyclooxygenase-derived prostaglandins. Dev Biol 289(2):263–272. https://doi.org/10.1016/j.ydbio.2005.10.013
Chen LF, Tian YF, Lin CH, Huang LY, Niu KC, Lin MT (2014) Repetitive hyperbaric oxygen therapy provides better effects on brain inflammation and oxidative damage in rats with focal cerebral ischemia. J Formos Med Assoc 113(9):620–628. https://doi.org/10.1016/j.jfma.2014.03.012
Choi SH, Aid S, Bosetti F (2009) The distinct roles of cyclooxygenase-1 and -2 in neuroinflammation: implications for translational research. Trends Pharmacol Sci 30(4):174–181. https://doi.org/10.1016/j.tips.2009.01.002
Dalvi S, Nguyen HH, On N, Mitchell RW, Aukema HM, Miller DW, Hatch GM (2015) Exogenous arachidonic acid mediates permeability of human brain microvessel endothelial cells through prostaglandin E2 activation of EP3 and EP4 receptors. J Neurochem 135(5):867–879. https://doi.org/10.1111/jnc.13117
DeMars KM, McCrea AO, Siwarski DM, Sanz BD, Yang C, Candelario-Jalil E (2018) Protective Effects of L-902,688, a Prostanoid EP4 Receptor Agonist, against Acute Blood-Brain Barrier Damage in Experimental Ischemic Stroke. Front Neurosci 12:89. https://doi.org/10.3389/fnins.2018.00089
Eltzschig HK, Eckle T (2011) Ischemia and reperfusion–from mechanism to translation. Nat Med 17(11):1391–1401. https://doi.org/10.1038/nm.2507
Feigin VL, Abajobir AA, Abate KH, Abd-Allah F, Abdulle AM, Abera SF, Abyu GY, Ahmed MB, Aichour AN, Aichour I, Aichour MTE, Akinyemi RO, Alabed S, Al-Raddadi R, Alvis-Guzman N, Amare AT, Ansari H, Anwari P, Ärnlöv J, Asayesh H, Asgedom SW, Atey TM, Avila-Burgos L, Frinel E, Avokpaho GA, Azarpazhooh MR, Barac A, Barboza M, Barker-Collo SL, Bärnighausen T, Bedi N, Beghi E, Bennett DA, Bensenor IM, Berhane A, Betsu BD, Bhaumik S, Birlik SM, Biryukov S, Boneya DJ, Bulto LNB, Carabin H, Casey D, Castañeda-Orjuela CA, Catalá-López F, Chen H, Chitheer AA, Chowdhury R, Christensen H, Dandona L, Dandona R, de Veber GA, Dharmaratne SD, Do HP, Dokova K, Dorsey ER, Ellenbogen RG, Eskandarieh S, Farvid MS, Fereshtehnejad S-M, Fischer F, Foreman KJ, Geleijnse JM, Gillum RF, Giussani G, Goldberg EM, Gona PN, Goulart AC, Gugnani HC, Gupta R, Hachinski V, Gupta R, Hamadeh RR, Hambisa M, Hankey GJ, Hareri HA, Havmoeller R, Hay SI, Heydarpour P, Hotez PJ, Jakovljevic MB, Javanbakht M, Jeemon P, Jonas JB, Kalkonde Y, Kandel A, Karch A, Kasaeian A, Kastor A, Keiyoro PN, Khader YS, Khalil IA, Khan EA, Khang Y-H, Tawfih A, Khoja A, Khubchandani J, Kulkarni C, Kim D, Kim YJ, Kivimaki M, Kokubo Y, Kosen S, Kravchenko M, Krishnamurthi RV, Defo BK, Kumar GA, Kumar R, Kyu HH, Larsson A, Lavados PM, Li Y, Liang X, Liben ML, Lo WD, Logroscino G, Lotufo PA, Loy CT, Mackay MT, El Razek HMA, El Razek MMA, Majeed A, Malekzadeh R, Manhertz T, Mantovani LG, Massano J, Mazidi M, McAlinden C, Mehata S, Mehndiratta MM, Memish ZA, Mendoza W, Mengistie MA, Mensah GA, Meretoja A, Mezgebe HB, Miller TR, Mishra SR, Ibrahim NM, Mohammadi A, Mohammed KE, Mohammed S, Mokdad AH, Moradi-Lakeh M, Velasquez IM, Musa KI, Naghavi M, Ngunjiri JW, Nguyen CT, Nguyen G, Le Nguyen Q, Nguyen TH, Nichols E, Ningrum DNA, Nong VM, Norrving B, Noubiap JJN, Ogbo FA, Owolabi MO, Pandian JD, Parmar PG, Pereira DM, Petzold M, Phillips MR, Piradov MA, Poulton RG, Pourmalek F, Qorbani M, Rafay A, Rahman M, Rahman MH, Rai RK, Rajsic S, Ranta A, Rawaf S, Renzaho AMN, Rezai MS, Roth GA, Roshandel G, Rubagotti E, Sachdev P, Safiri S, Sahathevan R, Sahraian MA, Samy AM, Santalucia P, Santos IS, Sartorius B, Satpathy M, Sawhney M, Saylan MI, Sepanlou SG, Shaikh MA, Shakir R, Shamsizadeh M, Sheth KN, Shigematsu M, Shoman H, Silva DAS, Smith M, Sobngwi E, Sposato LA, Stanaway JD, Stein DJ, Steiner TJ, Stovner LJ, Abdulkader RS, Ei Szoeke C, Tabarés-Seisdedos R, Tanne D, Theadom AM, Thrift AG, Tirschwell DL, Topor-Madry R, Tran BX, Truelsen T, Tuem KB, Ukwaja KN, Uthman OA, Varakin YY, Vasankari T, Venketasubramanian N, Vlassov VV, Wadilo F, Wakayo T, Wallin MT, Weiderpass E, Westerman R, Wijeratne T, Wiysonge CS, Woldu MA, Wolfe CDA, Xavier D, Xu G, Yano Y, Yimam HH, Yonemoto N, Yu C, Zaidi Z, El Sayed ZM, Zunt JR, Murray CJL, Vos T (2017) Global, regional, and national burden of neurological disorders during 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. The Lancet Neurology 16(11):877–897. https://doi.org/10.1016/s1474-4422(17)30299-5
Goulet JL, Pace AJ, Key ML, Byrum RS, Nguyen M, Tilley SL, Morham SG, Langenbach R, Stock JL, McNeish JD, Smithies O, Coffman TM, Koller BH (2004) E-prostanoid-3 receptors mediate the proinflammatory actions of prostaglandin E2 in acute cutaneous inflammation. J Immunol 173(2):1321–1326. https://doi.org/10.4049/jimmunol.173.2.1321
Hankey GJ (2017) Stroke. The Lancet 389(10069):641–654. https://doi.org/10.1016/s0140-6736(16)30962-x
Iadecola C, Niwa K, Nogawa S, Zhao X, Nagayama M, Araki E, Morham S, Ross ME (2001) Reduced susceptibility to ischemic brain injury and N-methyl-D-aspartate-mediated neurotoxicity in cyclooxygenase-2-deficient mice. Proc Natl Acad Sci USA 98(3):1294–1299. https://doi.org/10.1073/pnas.98.3.1294
Ikeda-Matsuo Y, Ota A, Fukada T, Uematsu S, Akira S, Sasaki Y (2006) Microsomal prostaglandin E synthase-1 is a critical factor of stroke-reperfusion injury. Proc Natl Acad Sci USA 103(31):11790–11795. https://doi.org/10.1073/pnas.0604400103
Ikeda-Matsuo Y, Tanji H, Narumiya S, Sasaki Y (2011) Inhibition of prostaglandin E2 EP3 receptors improves stroke injury via anti-inflammatory and anti-apoptotic mechanisms. J Neuroimmunol 238(1–2):34–43. https://doi.org/10.1016/j.jneuroim.2011.06.014
Justin A, Sathishkumar M, Sudheer A, Shanthakumari S, Ramanathan M (2014) Non-hypotensive dose of telmisartan and nimodipine produced synergistic neuroprotective effect in cerebral ischemic model by attenuating brain cytokine levels. Pharmacol Biochem Behav 122:61–73. https://doi.org/10.1016/j.pbb.2014.03.009
Kang YJ, Mbonye UR, DeLong CJ, Wada M, Smith WL (2007) Regulation of intracellular cyclooxygenase levels by gene transcription and protein degradation. Prog Lipid Res 46(2):108–125. https://doi.org/10.1016/j.plipres.2007.01.001
Kapitanovic Vidak H, Catela Ivkovic T, Vidak Z, Kapitanovic S (2017) COX-1 and COX-2 polymorphisms in susceptibility to cerebral palsy in very preterm infants. Mol Neurobiol 54(2):930–938. https://doi.org/10.1007/s12035-016-9713-9
Kempski O, Shohami E, von Lubitz D, Hallenbeck JM, Feuerstein G (1987) Postischemic production of eicosanoids in gerbil brain. Stroke 18(1):111–119
Kumazawa T, Mizumura K, Koda H (1993) Involvement of EP3 subtype of prostaglandin E receptors in PGE2-induced enhancement of the bradykinin response of nociceptors. Brain Res 632(1–2):321–324
Legler DF, Bruckner M, Uetz-von Allmen E, Krause P (2010) Prostaglandin E2 at new glance: novel insights in functional diversity offer therapeutic chances. Int J Biochem Cell Biol 42(2):198–201. https://doi.org/10.1016/j.biocel.2009.09.015
Liu Y, Jia Z, Sun Y, Zhou L, Downton M, Chen R, Zhang A, Yang T (2014) Postnatal regulation of 15-hydroxyprostaglandin dehydrogenase in the rat kidney. Am J Physiol Renal Physiol 307(4):F388–395. https://doi.org/10.1152/ajprenal.00512.2013
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25(4):402–408. https://doi.org/10.1006/meth.2001.1262
McCullough L, Wu L, Haughey N, Liang X, Hand T, Wang Q, Breyer RM, Andreasson K (2004) Neuroprotective function of the PGE2 EP2 receptor in cerebral ischemia. J Neurosci 24(1):257–268. https://doi.org/10.1523/jneurosci.4485-03.2004
Minghetti L, Nicolini A, Polazzi E, Creminon C, Maclouf J, Levi G (1997) Inducible nitric oxide synthase expression in activated rat microglial cultures is downregulated by exogenous prostaglandin E2 and by cyclooxygenase inhibitors. Glia 19(2):152–160
Radi ZA, Khan NK (2006) Effects of cyclooxygenase inhibition on the gastrointestinal tract. Exp Toxicol Pathol 58(2–3):163–173. https://doi.org/10.1016/j.etp.2006.06.004
Saleem S, Kim YT, Maruyama T, Narumiya S, Dore S (2009) Reduced acute brain injury in PGE2 EP3 receptor-deficient mice after cerebral ischemia. J Neuroimmunol 208(1–2):87–93. https://doi.org/10.1016/j.jneuroim.2009.01.015
Shi J, Johansson J, Woodling NS, Wang Q, Montine TJ, Andreasson K (2010) The prostaglandin E2 E-prostanoid 4 receptor exerts anti-inflammatory effects in brain innate immunity. J Immunol 184(12):7207–7218. https://doi.org/10.4049/jimmunol.0903487
Shimizu T, Tanaka K, Nakamura K, Taniuchi K, Yawata T, Higashi Y, Ueba T, Dimitriadis F, Shimizu S, Yokotani K, Saito M (2014) Possible involvement of brain prostaglandin E2 and prostanoid EP3 receptors in prostaglandin E2 glycerol ester-induced activation of central sympathetic outflow in the rat. Neuropharmacology 82:19–27. https://doi.org/10.1016/j.neuropharm.2014.03.005
Sugimoto Y, Narumiya S (2007) Prostaglandin E receptors. The Journal of biological chemistry 282(16):11613–11617. https://doi.org/10.1074/jbc.R600038200
Tai HH, Cho H, Tong M, Ding Y (2006) NAD+-linked 15-hydroxyprostaglandin dehydrogenase: structure and biological functions. Curr Pharm Des 12(8):955–962
Tai HH, Ensor CM, Tong M, Zhou H, Yan F (2002) Prostaglandin catabolizing enzymes. Prostaglandins Other Lipid Mediat 68–69:483–493
Tanikawa N, Ohmiya Y, Ohkubo H, Hashimoto K, Kangawa K, Kojima M, Ito S, Watanabe K (2002) Identification and characterization of a novel type of membrane-associated prostaglandin E synthase. Biochem Biophys Res Commun 291(4):884–889. https://doi.org/10.1006/bbrc.2002.6531
Tanioka T, Nakatani Y, Semmyo N, Murakami M, Kudo I (2000) Molecular identification of cytosolic prostaglandin E2 synthase that is functionally coupled with cyclooxygenase-1 in immediate prostaglandin E2 biosynthesis. The Journal of biological chemistry 275(42):32775–32782. https://doi.org/10.1074/jbc.M003504200
Xu J, Xu Z, Yan A (2017) Prostaglandin E2 EP4 Receptor Activation Attenuates Neuroinflammation and Early Brain Injury Induced by Subarachnoid Hemorrhage in Rats. Neurochem Res 42(4):1267–1278. https://doi.org/10.1007/s11064-016-2168-6
Funding
This work was supported by the National Natural Science Foundation of China (No. 81571880, 81373147, 30901555, 30972870, 81360080, 81671895, 81471897 and 81671895) and Natural Science Foundation of Hunan Province (No. 2016JJ2157). All the funding bodies funded in the study design, collection, analysis, interpretation of data and writing the manuscript.
Author information
Authors and Affiliations
Contributions
YL and JZ designed and directed the project. YX and KL performed the experiments. YX, YL, KL, SM, CL and CW analyzed the data. All authors discussed the results and contributed to the final manuscript. Yunfei Xu wrote the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted by Experimental Animal Center of Central South University (Changsha, China), No: 2018sydw0222.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xu, Y., Liu, Y., Li, K. et al. Regulation of PGE2 Pathway During Cerebral Ischemia Reperfusion Injury in Rat. Cell Mol Neurobiol 41, 1483–1496 (2021). https://doi.org/10.1007/s10571-020-00911-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-020-00911-5