Abstract
Airway abnormalities are frequently associated with congenital heart disease in infants and children. Respiratory distress in these children frequently requires prolonged respiratory support. Wide-detector dynamic pulmonary computed tomography angiography (DP-CTA) is a non-invasive technique that completely evaluates vascular and airway abnormalities during a single breathe. Our purpose was to evaluate the efficacy of DP-CTA to provide unique actionable information for patient care in newborns and infants with congenital heart disease and persistent respiratory distress. 23 infants with congenital heart disease and persistent respiratory distress underwent DP-CTA. All were intubated at the time of the examinations. The most common cardiac anomalies were tetralogy of Fallot (6) and hypoplastic left heart syndrome variants (5). The most common cardiac surgeries prior to DP-CTA were Norwood (4) and hybrid (3) procedures. The protocol for DP-CTA for intubated infants is four gantry rotations in 1.4 s after intravenous contrast injection. 3D and multiplanar reconstruction with cine loops were created for combined cardiopulmonary imaging. Tracheobronchomalacia was present in 17 children. Lobar bronchomalacia was identified in six children. Branch pulmonary artery stenosis was the most common vascular finding (10 children). Medical management was changed or a surgical procedure performed based on the information resulting from DP-CTA in 16 of the 23 patients (70 %). DP-CTA is non-invasive, fast and provides unique information for the management of infants with congenital heart disease and persistent respiratory distress. DP-CTA is uniquely suited for comprehensive and simultaneous evaluation of airway and vascular abnormalities in infants.




Similar content being viewed by others
References
Lee EY, Boiselle PM (2009) Tracheobronchial malacia in infants and children: multidetector CT evaluation. Radiology 252:7–22
Healy F, Hanna BD, Zinman R (2012) Pulmonary complications of congenital heart disease. Paediatr Respir Rev 13(1):10–15. doi:10.1016/j.prrv.2011.01.007
Mok Q, Negus S, McLaren CA, Rajka T, Elliott MJ, Roebuck DJ, McHugh K (2005) Computed tomography versus bronchography in the diagnosis and management of tracheobronchomalacia in ventilator dependent infants. Arch Dis Child Fetal Neonatal Ed 90:F290–F293
Lee EY, Greenberg SB, Boiselle PM (2011) Multidetector computed tomography of pediatric large airway diseases: state-of-the-art. Radiol Clin North Am 49:869–893
Lee EY, Litmanovich D, Boiselle PM (2009) Multidetector CT evaluation of tracheobronchomalacia. Radiol Clin North Am 47:261–269
Goo HW, Kim HJ (2006) Detection of air trap** on inspiratory and expiratory phase images obtained by 0.3-second cine CT in the lungs of free-breathing young children. AJR 187:1019–1023
Greenberg SB (2012) Dynamic pulmonary CT of children. Am J Roentgenol 199:435–440
Thomas EK, Wang B (2008) Age-specific effective doses for pediatric MSCT examinations at a large children’s hospital using DLP conversion coefficients: a simple estimation method. Pediatr Radiol 38:645–656
Aquino SL, Shepard JA, Ginns LC, Moore RH, Halpern E, Grillo HC, McLoud TC (2001) Acquired tracheomalacia: detection by expiratory CT scan. J Comput Assist Tomogr 25:394–399
Watanabe N, Hayabuchi Y, Inoue M, Sakata M, Nabo MM, Nakagawa R, Saijo T, Kagami S (2009) Tracheal compression due to an elongated aortic arch in patients with congenital heart disease: evaluation using multidetector-row CT. Pediatr Radiol 39:1048–1053
Hainstock M, Bardo D, Rice M, Langley S (2010) Hypoplastic left heart syndrome associated with large omphalocele and hypoplastic left bronchus. Pediatr Cardiol 31:878–880
Wang CC, Chen SJ, Wu ET, Chen CA, Chiu SN, Lin MT, Lu F, Huang SC, Wu MH, Wang JK (2013) Lower airway anomalies in children with CATCH 22 syndrome and congenital heart disease. Pediatr Pulmonol 48(6):587–591. doi:10.1002/ppul.22674
Nayak PP, Sheth J, Cox PN, Davidson L, Forte V, Manlhiot C, McCrindle BW, Schwartz SM, Solomon M, Van Arsdell GS, Sivarajan VB (2012) Predictive value of bronchoscopy after infant cardiac surgery: a prospective study. Intensive Care Med 38:1851–1857
Ferandos C, El-Said H, Hamzeh R, Moore JW (2009) Adverse impact of vascular stent “mass effect” on airways. Catheter Cardiovasc Interv 74:132–136
Prodhan P, Fiser RT, Cenac S, Bhutta AT, Fontenot E, Moss M, Schexnayder S, Seib S, Chipman C, Weygandt L, Immamura M, Jaquiss RD, Dyamenahalli U (2010) Intrahospital transport of children on extracorporeal membrane oxygenation: indications, process, interventions, and effectiveness. Pediatr Crit Care Med 11:227–233
Greenberg SB (2011) Rebalancing the risks of computed tomography and magnetic resonance imaging. Pediatr Radiol 41:951–952
Lee EY, Zurakowski D, Waltz DA (2008) MDCT evaluation of the prevalence of tracheomalacia in children with mediastinal aortic vascular anomalies. J Thorac Imaging 23:258–265
Lee EY (2013) Interstitial lung disease in infants: new classification system, imaging technique, clinical presentation and imaging findings. Pediatr Radiol 43:3–13
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
10554_2013_344_MOESM1_ESM.avi
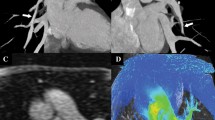
Figure 2 supplemental: The color lit cine loop shows dynamic narrowing of the left bronchus during expiration as the left bronchus passes anterior to the descending aorta. (AVI 6146 kb)
10554_2013_344_MOESM2_ESM.avi
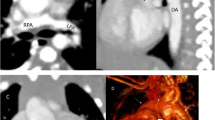
Figure 3 supplemental: The 3D volume rendering cine loop shows severe right upper lobe bronchomalacia resulting from the PDA stent. (AVI 6146 kb)
10554_2013_344_MOESM3_ESM.avi
Figure 4 supplemental: The3D volume rendering shows severe left bronchomalacia associated with the left PDA stent. (AVI 6146 kb)
Rights and permissions
About this article
Cite this article
Greenberg, S.B., Dyamenahalli, U. Dynamic pulmonary computed tomography angiography: a new standard for evaluation of combined airway and vascular abnormalities in infants. Int J Cardiovasc Imaging 30, 407–414 (2014). https://doi.org/10.1007/s10554-013-0344-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-013-0344-1