Abstract
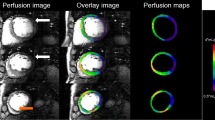
This study aims to quantify subendocardial and subepicardial myocardial blood flow (MBF) from dynamic contrast-enhanced MRI and to compare semi-quantitative and quantitative analysis methods. 17 healthy volunteers (9 males, mean age 34 ± 8) were scanned during adenosine stress and at rest. A “semi-quantitative” myocardial perfusion index (MPI) was calculated based on maximal upslopes of signal intensity-time profiles for a mid-ventricular myocardial slice. In addition, absolute MBF (ml/g/min) was estimated using Fermi-constrained deconvolution. On semi-quantitative analysis, the ratio of subendocardial to subepicardial MPI was 0.98 ± 0.1 at stress and 1.16 ± 0.09 at rest, P < 0.0001. The MPRI (i.e. the ratio of stress over rest MPI) for the subendocardium was 1.54 ± 0.3 versus 1.81 ± 0.35 for the subepicardium, P = 0.03. For quantitative analysis, the ratio of subendocardial to subepicardial MBF was 0.91 ± 0.11 at stress versus 1.17 ± 0.16 at rest, P < 0.0001. The subendocardial MBF reserve was also lower than in the subepicardium (2.6 ± 0.75 vs. 3.32 ± 0.93, P = 0.027). In conclusion, semi-quantitative and quantitative analysis of dynamic contrast-enhanced MRI shows higher subendocardial blood flow at rest and reduced subendocardial perfusion reserve compared to the subepicardium.







Similar content being viewed by others
Abbreviations
- CMR:
-
Cardiovascular magnetic resonance
- EF:
-
Ejection fraction
- MBF:
-
Myocardial blood flow
- MPRI:
-
Myocardial perfusion reserve index
- MPI:
-
Myocardial perfusion index
- BP:
-
Blood pressure
- LV-EDV:
-
Left ventricular end-diastolic volume
- LV-ESV:
-
Left ventricular end-systolic volume
- SI:
-
Signal intensity
- ROI:
-
Region of interest
References
Ball RM, Bache RJ, Cobb FR, Greenfield JC Jr (1975) Regional myocardial blood flow during graded treadmill exercise in the dog. J Clin Invest 55(1):43–49
Lee DC, Simonetti OP, Harris KR, Holly TA, Judd RM, Wu E, Klocke FJ (2004) Magnetic resonance versus radionuclide pharmacological stress perfusion imaging for flow-limiting stenoses of varying severity. Circulation 110(1):58–65
Christian TF, Rettmann DW, Aletras AH, Liao SL, Taylor JL, Balaban RS, Arai AE (2004) Absolute myocardial perfusion in canines measured by using dual-bolus first-pass MR imaging. Radiology 232(3):677–684
Muehling OM, Jerosch-Herold M, Panse P, Zenovich A, Wilson BV, Wilson RF, Wilke N (2004) Regional heterogeneity of myocardial perfusion in healthy human myocardium: assessment with magnetic resonance perfusion imaging. J Cardiovasc Magn Reson 6(2):499–507
Panting JR, Gatehouse PD, Yang G-Z, Grothues F, Firmin DN, Collins P, Pennell DJ (2002) Abnormal subendocardial perfusion in cardiac syndrome X detected by cardiovascular magnetic resonance imaging. N Engl J Med 346(25):1948–1953
Vermeltfoort IA, Bondarenko O, Raijmakers PG, Odekerken DA, Kuijper AF, Zwijnenburg A, van der Vis-Melsen MJ, Twisk JW, Beek AM, Teule GJ, van Rossum AC (2007) Is subendocardial ischaemia present in patients with chest pain and normal coronary angiograms? A cardiovascular MR study. Eur Heart J 28(13):1554–1558
Radjenovic A, Biglands JD, Larghat A, Ridgway JP, Ball SG, Greenwood JP, Jerosch-Herold M, Plein S (2010) Estimates of systolic and diastolic myocardial blood flow by dynamic contrast-enhanced MRI. Magn Reson Med 64(6):1696–1703
Alfakih K, Reid S, Jones T, Sivananthan M (2004) Assessment of ventricular function and mass by cardiac magnetic resonance imaging. Eur Radiol 14(10):1813–1822
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK, Pennell DJ, Rumberger JA, Ryan T, Verani MS (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart: a statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation 105(4):539–542
Jerosch-Herold M, Wilke N, Stillman A (1998) Magnetic resonance quantification of the myocardial perfusion reserve with a Fermi function model for constrained deconvolution. Med Phys 25(1):73–84
Larsson HBW, FritzHansen T, Rostrup E, Sondergaard L, Ring P, Henriksen O (1996) Myocardial perfusion modeling using MRI. Magn Reson Med 35(5):716–726
Fritz-Hansen T, Hove JD, Kofoed KF, Kelbaek H, Larsson HBW (2008) Quantification of MRI measured myocardial perfusion reserve in healthy humans: a comparison with positron emission tomography. J Magn Reson Imaging 27(4):818–824
Rohrer M, Bauer H, Mintorovitch J, Requardt M, Weinmann H-J (2005) Comparison of magnetic properties of MRI contrast media solutions at different magnetic field strengths. Invest Radiol 40(11):715–724
Fritsch FN, Carlson RE (1980) Monotone piecewise cubic interpolation. SIAM J Numer Anal 17(2):238–246
Cheong LH, Koh TS, Hou Z (2003) An automatic approach for estimating bolus arrival time in dynamic contrast MRI using piecewise continuous regression models. Phys Med Biol 48(5):N83–N88
Duncker DJ, Bache RJ (2008) Regulation of coronary blood flow during exercise. Physiol Rev 88(3):1009–1086
Duncker DJ, Ishibashi Y, Bache RJ (1998) Effect of treadmill exercise on transmural distribution of blood flow in hypertrophied left ventricle. Am J Physiol 275(4 Pt 2):H1274–H1282
Duncker DJ, Traverse JH, Ishibashi Y, Bache RJ (1999) Effect of NO on transmural distribution of blood flow in hypertrophied left ventricle during exercise. Am J Physiol 276(4 Pt 2):H1305–H1312
Parks CM, Manohar M (1983) Transmural coronary vasodilator reserve and flow distribution during severe exercise in ponies. J Appl Physiol 54(6):1641–1652
Knaapen P, Germans T, Camici PG, Rimoldi OE, ten Cate FJ, ten Berg JM, Dijkmans PA, Boellaard R, van Dockum WG, Gotte MJW, Twisk JWR, van Rossum AC, Lammertsma AA, Visser FC (2008) Determinants of coronary microvascular dysfunction in symptomatic hypertrophic cardiomyopathy. Am J Physiol Heart Circ Physiol 294(2):H986–H993
Kawecka-Jaszcz K, Czarnecka D, Olszanecka A, Klecha A, Kwiecien-Sobstel A, Stolarz-Skrzypek K, Pennell DJ, Pasowicz M, Klimeczek P, Banys RP (2008) Myocardial perfusion in hypertensive patients with normal coronary angiograms. J Hypertens 26(8):1686–1694
Deussen A, Lauer T, Loncar R, Kropp J (2001) Heterogeneity of metabolic parameters in the left ventricular myocardium and its relation to local blood flow. Basic Res Cardiol 96(6):564–574
Zwanenburg JJ, Gotte MJ, Kuijer JP, Hofman MB, Knaapen P, Heethaar RM, van Rossum AC, Marcus JT (2005) Regional timing of myocardial shortening is related to prestretch from atrial contraction: assessment by high temporal resolution MRI tagging in humans. Am J Physiol Heart Circ Physiol 288(2):H787–H794
Gebker R, Schwitter J, Fleck E, Nagel E (2007) How we perform myocardial perfusion with cardiovascular magnetic resonance. J Cardiovasc Magn Reson 9(3):539–547
Kellman P, Arai AE (2007) Imaging sequences for first pass perfusion–a review. J Cardiovasc Magn Reson 9(3):525–537
Gerber BL, Raman SV, Nayak K, Epstein FH, Ferreira P, Axel L, Kraitchman DL (2008) Myocardial first-pass perfusion cardiovascular magnetic resonance: history, theory, and current state of the art. J Cardiovasc Magn Reson 10(1):18
Schwitter J (2006) Myocardial perfusion. J Magn Reson Imaging 24:953–963
Biglands JD, Larghat A, Plein S, Buckley DL, Jerosch-Herold M, Magee D, Boyle R, Radjenovic A (2010) Saturation correction of dynamic contrast enhanced MRI uptake curves for quantitative myocardial blood flow measurements using an assumed T1 for blood. Proc Intl Soc Magn Reson Med 19
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Larghat, A., Biglands, J., Maredia, N. et al. Endocardial and epicardial myocardial perfusion determined by semi-quantitative and quantitative myocardial perfusion magnetic resonance. Int J Cardiovasc Imaging 28, 1499–1511 (2012). https://doi.org/10.1007/s10554-011-9982-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-011-9982-3