Abstract
Purpose
Our aim was to establish a rodent model of nonarteritic ischemic optic neuropathy (rNAION).
Methods
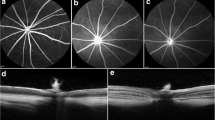
To induce rNAION, after administration of Rose Bengal (RB) (2.5 mM), the small vessels of the left optic nerve were photoactivated using a 514-nm argon green laser with about 500-μm spot size for 12 s (RB-laser induction). To evaluate the induction, funduscopic examination, fluorescein angiography (FA), visualization of capillaries within the optic disc, histologic evaluation, and electrophysiological testing were performed.
Results
In the RB-laser-induction eyes, the optic disc became swollen on day 3 followed by atrophy on week 8. FA showed filling defects in the choroid and optic disc at an early stage, followed by hyperfluorescence at a late stage. The capillaries within the optic disc were reduced markedly. Histopathologic examination showed acellular nerve fiber layer (NFL) swelling anterior to the optic disc. The morphologic retinal changes were apparent only in the retinal ganglion cell (RGC) layer, with a reduction in the number of cells. Visually evoked potential (VEP) amplitude decreased significantly, but electroretinography (ERG) showed no significant difference. The positive scotopic threshold response (pSTR) was not reduced on the 1st day but was significantly reduced 3 days after induction.
Conclusions
The findings are similar to human NAION. Therefore, RB-laser induction is well suited to establish the presence of rNAION.








Similar content being viewed by others
References
Arnold AC. Ischemic optic neuropathy. In: Miller NR, Newman NJ, editors. Walsh & Hoyt’s clinical neuro-ophthalmology. Philadelphia: Lippincott Williams &Wilkins; 2005. p. 349–84.
The Ischemic Optic Neuropathy Decompression Trial Research Group. Optic nerve decompression surgery for nonarteritic anterior ischemic optic neuropathy (NAION) is not effective and may be harmful. JAMA. 1995;273:625–32.
Kelman SE. Intravitral triamcinolone or bevacizumab for nonarteritic anterior ischemic optic neuropathy: do they merit further study? J Neuroophthalmol. 2007;3:161–3.
Bernstein SL, Guo Y, Kelman SE, Kelman SE, Flower RW, Johnson MA. Functional and cellular responses in a novel rodent model of anterior ischemic optic neuropathy. Invest Ophthalmol Vis Sci. 2003;44:4153–62.
Wang RS, Lv PL, Wang WJ, Wang XD, Zhang XJ, Li SN, et al. Establishing an experimental model of photodynamically induced anterior ischemic optic neuropathy. Vis Neurosci. 2011;28:155–62.
Bui BV, Fortune B. Ganglion cell contributions to the rat full-field electroretinogram. J Physiol. 2004;555:153–73.
Knox DL, Kerrison JB, Green WR. Histopathologic studies of ischemic optic neuropathy. Trans Am Ophthalmol Soc. 2000;98:203–22.
Masuzawa K, Jesmin S, Maeda S, Kaji Y, Oshika T, Zaedi S, et al. A model of retinal ischemia-reperfusion injury in rats by subconjunctival injection of endothelin-1. Exp Biol Med. 2006;231:1085–9.
Grozdanic SD, Sakaguchi DS, Kwon YH, Kardon RH, Sonea IM. Functional characterization of retina and optic nerve after acute ocular ischemia in rats. Invest Ophthalmol Vis Sci. 2003;44:2597–605.
Duvdevani R, Rosner M, Belkin M, Sautter J, Sabel BA, Schwartz M. Graded crash of the rat optic nerve as a brain injury model: combining electrophysiological and behavioral outcome. Rest Neurol Neurosci. 1990;2:31–8.
Berkrlaar M, Clarke DB, Wang YC, Bray GM, Aguayo AJ. Axotomy results in delayed death and apoptosis of retinal ganglion cells in adult rats. J Neurosci. 1994;14:4268–372.
Bernstein SL, Johnson MA, Miller NR. Nonarteritic anterior ischemic optic neuropathy (NAION) and its experimental models. Prog Retin Eye Res. 2011;30:167–87.
Watson BD, Dietrich WD, Busto R, Wachtel MS, Ginsberg MD. Induction of reproducible brain infarction by photochemically initiated thrombosis. Ann Neurol. 1985;17:497–504.
Zhao BQ, Suzuki Y, Kondo K, Kawano K, Ikeda Y, Umemura K. A novel MCA occulusion model of photothrombotic ischemia with cyclic flow reductions: development of cerebral hemorrhage induced by heparin. Brain Res Brain Res Protoc. 2002;9:85–92.
Mosinger JL, Olney JW. Photothrombosis-induced ischemic neuronal degeneration in the rat retina. Exp Neurol. 1989;105:110–3.
Fluhler EN, Hurley JK, Kochevar IE. Laser intensity and wavelength dependence of Rose Bengal- photosensitized inhibition of red blood cell acetylcholinesterase. Biochem Biophys Acta. 1994;990:269–75.
Rodgers MAJ. Light-induced generation of signet oxygen in solutions of Rose Bengal. Chem Phys Lett. 1981;78:509–14.
Acknowledgments
We Shigeki Machida from the University of Iwate for his technical support and invaluable comments on electrophysiology, and Yuichiro Sato from University of Miyazaki for his technical support and valuable comments on histopathology.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Chuman, H., Maekubo, T., Osako, T. et al. Rodent model of nonarteritic ischemic optic neuropathy and its electrophysiological evaluation. Jpn J Ophthalmol 56, 518–527 (2012). https://doi.org/10.1007/s10384-012-0167-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-012-0167-y