Abstract
Background
The aim of this study was to assess the 3-year objective and subjective outcomes of patients with complex anorectal fistula treated with Video-Assisted Anal Fistula Treatment (VAAFT). Furthermore, we evaluated the risk factors associated with recurrence.
Methods
All consecutive patients with complex anorectal fistula who underwent VAAFT in Beata Vergine Hospital of Mendrisio, Switzerland, from January 2013 to January 2016, were enrolled. Patients with suspicion or diagnosis of Crohn’s disease, malignancy, previous history of radiotherapy or radical pelvic surgery were excluded. Preoperative clinical assessment based upon medical history, physical examination and endosonography, was performed in all patients. Data regarding subjective outcomes (the Patient Global Impression of Improvement, patient satisfaction scores and Wexner score), objective cure rate (absence of fistula at clinical examination), and adverse events were collected during follow-up. Uni and multivariate analysis were performed to investigate outcomes.
Results
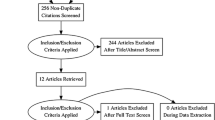
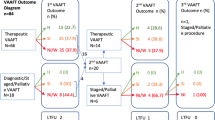
One hundred and four patients had VAAFT. At 3-year follow-up, 96 patients (92.3%) were available for the evaluation. At 3 years after surgery, 81 of 96 patients (84.4%) declared themselves cured (p = 0.60). Similarly, at 3-year evaluation, 80 of 96 patients (83.3%) were objectively cured (p = 0.52). No serious intraoperative or postoperative complications were reported. All recurrences were treated with a repeat VAAFT procedure resulting in a complete healing. Uni and multivariate analysis of variables potentially involved in the failure of VAAFT showed that age ≥ 50 years was the only factor associated at risk of recurrence.
Conclusions
VAAFT is a highly effective safe procedure for the treatment of anorectal fistula, with a low recurrence rate at 3-year follow-up. However, our study demonstrated that age ≥ 50 years is a risk factor for failure of VAAFT.


Similar content being viewed by others
References
Abcarian H (2011) Anorectal infection: abscess-fistula. Clin Colon Rectal Surg 24(1):14–21
Ramanujam PS et al (1984) Perianal abscesses and fistulas. A study of 1023 patients. Dis Colon Rectum 27(9):593
Amato A, Bottini C, De Nardi P et al (2020) Evaluation and management of perianal abscess and anal fistula: SICCR position statement. Tech Coloproctol 24:127–143. https://doi.org/10.1007/s10151-019-02144-1.0
Sangwan YP et al (1994) Is simple fistula-in-ano simple? Dis Colon Rectum 37:885–889
Meinero P, Mori L (2011) Video-assisted anal fistula treatment (VAAFT): a novel sphincter-saving procedure for treating complex anal fistulas. Tech Coloproctol 15(4):417–422
Rojanasakul A (2009) LIFT procedure: a simplified technique for fistula-in-ano. Tech Coloproctol 13:237–240
Lupinacci RM, Vallet C, Parc Y, Chafai N, Tiret E (2010) Treatment of fistula-in-ano with the Surgisis AFP(TM) anal fistula plug. Gastroenterol Clin Biol 34:549–553
Song KH (2012) New techniques for treating an anal fistula. J Korean Soc Coloproctol 28(1):7–12. https://doi.org/10.3393/jksc.2012.28.1.7
Garcia-Aguilar J, Belmonte C, Wong WD, Goldberg SM, Madoff RD (1996) Anal fistula surgery. Factors associated with recurrence and incontinence. Dis Colon Rectum 39(7):723–729
Emile SH, Elfeki H, Shalaby M, Sakr A (2018) A systematic review and meta-analysis of the efficacy and safety of video-assisted anal fistula treatment (VAAFT). Surg Endosc 32:2084–2093
Seow-En I, Seow-Choen F, Koh PK (2016) An experience with video-assisted anal fistula treatment (VAAFT) with new insights into the treatment of anal fistulae. Tech Coloproctol 20(6):389–393. https://doi.org/10.1007/s10151-016-1450-6
Parks AG et al (1976) A classification of fistula-in-ano. Br J Surg 63:1–12
Yalcin I, Bump RC (2003) Validation of two global impression questionnaires for incontinence. Am J Obstet Gynecol 189(1):98–101
Vaizey CJ, Carapeti E, Cahill JA, Kamm MA (1999) Prospective comparison of faecal incontinence grading systems. Gut 44:77–80
Takahashi-Monroy T, Morales M, Garcia-Osogobio S et al (2008) SECCA(R) procedure for the treatment of fecal incontinence: results of five-year follow-up. Dis Colon Rectum 51:355
Atkin GK et al (2011) For many high anal fistulas, lay open is still a good option. Tech Coloproctol 15:143–150
Mizrahi N, Wexner SD, Zmora O, Da Silva G, Efron J, Weiss EG, Vernava AM 3rd, Nogueras JJ (2002) Endorectal advancement flap: are there predictors of failure? Dis Colon Rectum 45(12):1616–1621
Sonoda T, Hull T, Piedmonte MR, Fazio VW (2002) Outcomes of primary repair of anorectal and rectovaginal fistulas using the endorectal advancement flap. Dis Colon Rectum 45:1622
Mentes BB et al (2004) Elastic one-stage cutting seton for the treatment of high anal fistulas: preliminary results. Tech Coloproctol 8(3):159–162
Shanwani A et al (2010) Ligation of the intersphincteric fistula tract (LIFT): a sphincter-saving technique for fistula-in-ano. Dis Colon Rectum 53:39–42
Lunniss PJ (2009) LIFT procedure: a simplified technique for fistula in ano. Tech Coloproctol 13(3):241–242
Sentovich SM (2003) Fibrin glue for anal fistulas: long-term results. Dis Colon Rectum 46(4):498–502
Christoforidis D et al (2008) Treatment of complex anal fistulas with the collagen fistula plug. Dis Colon Rectum 51(10):1482–1487
Wilhelm A (2011) A new technique for sphincter-preserving anal fistula repair using a novel radial emitting laser probe. Tech Coloproctol 15:445–449
Wang D et al (2014) Risk factors for anal fistula: a case–control study. Tech Coloproctol 18(7):635–639
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was conducted according to the tenets of the Declaration of Helsinki. No Institutional Review Board approval was required for this study because there was no deviation from normal clinical practice.
Informed consent
Preoperative written informed consent for VAAFT procedure was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Regusci, L., Fasolini, F., Meinero, P. et al. Video-Assisted Anal Fistula Treatment (VAAFT) for complex anorectal fistula: efficacy and risk factors for failure at 3-year follow-up. Tech Coloproctol 24, 741–746 (2020). https://doi.org/10.1007/s10151-020-02213-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-020-02213-w