Abstract
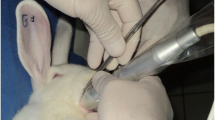
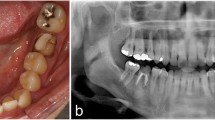
This study aimed to investigate the influence of low-power 830 nm gallium–aluminium–arsenide (GaAlAs) laser [continuous wave (CW) 40 mW and fluence 4 J/cm2, with total energy density of 16 J/cm2] on the healing of human infra-bony defects treated with bioactive glass graft material. Twenty patients with chronic periodontitis and bilateral infra-bony defects were included. Using a split mouth design, we treated 20 defects with bioactive glass plus laser irradiation during surgical procedures and on days 3, 5, 7 postoperatively; 20 contra-lateral defects were treated with bioactive glass only. Clinical probing pocket depths, clinical attachment levels and standardized periapical radiographs were recorded at baseline and at 3 months and 6 months postoperatively. At 3 months there was a statistically significant difference between the laser and non-laser sites in the parameters investigated. However, at 6 months, no difference was observed. Our results have confirmed the positive effect of soft laser in accelerating periodontal wound healing.






Similar content being viewed by others
References
Sculean A, Barbe G, Chiantella GC, Arweiler NB, Berakdar M, Brecx M (2002) Clinical evaluation of an enamel matrix protein derivative combined with a bioactive glass for the treatment of intrabony periodontal defects in humans. J Periodontol 73:401–408
Sculean A, Pietruska M, Schwars F, Willershausen B, Arweiler NB, Auuschill TM (2005) Healing of human intrabony defects following regenerative periodontal therapy with an enamel matrix protein derivative alone or combined with a bioactive glass. A controlled clinical study. J Clin Periodont 32:111–117
Keles GC, Cetinkaya BO, Albayrak D, Koprulu H, Acikgoz G (2006) Comparison of platelet pellet and bioactive glass in periodontal regenerative therapy. Acta Odont Scand 64:327–333
Pinheiro AL, Gerbi ME (2006) Photo engineering of bone repair processes. Photomed Laser Surg 24:169–178
Dortbudak O, Haas R, Mailath PG (2000) Biostimulation of bone marrow cells with a diode soft laser. Clin Oral Implants Res 11:540–545
Silva Junior AN, Pinherio ALB, Oliveira MG, Weismann R, Ramalho PLM, Nicolau RA (2002) Computerized morphometric assessment of the effect of low level laser therapy on bone repair: an experimental animal study. J Clin Laser Med Surg 20:83–87
Gerbi ME, Pinheiro ALB, Marzola C, Limera Junior FD, Ramalho LM, Ponzi EA, Soares AO (2005) Assessment of bone repair associated with the use of organic bovine bone and membrane irradiated at 830 nm. Photomed Laser Surg 23:382–388
Pinheiro AL, Nascimento SC, Vieira AL (2001) Effects of LLLT on malignant cells: study in vitro. In: Rechmann P, Fried D, Hennig T (eds) Lasers in dentistry VII. SPIE, Billingham, pp 56–60
Stein A, Benayahu D, Maltz L, Oron L (2005) Low level laser irradiation promotes proliferation and differentiation of human osteoblasts in vitro. Photomed Laser Surg 23:161–166
Lugar EJ, Rockhind S, Wollman Y, Kogan G, Dekel S (1998) Effect of low power laser irradiation on the mechanical properties of bone fracture healing in rats. Lasers Surg Med 22:97–102
Anneroth G, Hall G, Ryden H, Zetterqvist L (1998) The effect of low-energy infrared laser radiation on wound healing in rats. Br J Oral Maxillofac Surg 26:12–17
Romanos GE, Everts H, Nentwig GH (2000) Effects of diode and Nd: YAG laser irradiation on titanium discs: a scanning electron microscope examination. J Peridontol 71:810–815
Armitage GC (1999) Development of a classification system for periodontal diseases and conditions. Ann Periodontol 4:1–6
Benn DK (1992) A computer-assisted method for making linear radiographic measurements using stored regions of interest. J Clin Periodont 19:441–448
Eickholz P, Benn DK, Staehle HJ (1996) Radiographic evaluation of bone regeneration following periodontal surgery with or without ePTFE barriers. J Periodontol 67:379–385
Saito S, Shimizu N (1997) Stimulatory effects of low power laser irradiation on bone regeneration in mid-palatal suture during expansion in the rat. J Orthod Dentofac Orthop 111:525–532
De Souza Merli LA, Santos MTB, Genovese WJ, Faloppa F (2005) Effect of low-intensity laser irradiation on the process of bone repair. Photomed Laser Surg 23:212–215
Schneider NP, Soudry M, Remusat M, Franquim JC, Martin PM (1989) Modification of growth dynamics and ultrastructure after helium-neon laser treatment of human gingival fibroblasts. Quintessence Int 20:887–893
Guzzardella GA., Tigani D, Torricelli P, Fini M, Martini L, Morrone G, Giardino R (2001) Low-power diode laser stimulation of surgical osteochondral defects. Results after 24 weeks. Artif Cells Blood Substit Immobil Biotechnol 29:235–244
Pinheiro AL, Júnior LD, Gerbi ME, Ramalho LM, Marzola C (2003) Effect of low level laser therapy on the repair of bone defects grafted with inorganic bovine bone. Braz Dent J 14:177–181
Weber JB, Pinherio AL, De Oliveira MG, Oliveira FA, Ramalho LM (2006) Laser therapy improves healing of bone defects submitted to autologous bone graft. Photomed Laser Surg 24:38–44
Takeda Y (1988) Irradiation effect of low energy laser on alveolar bone after tooth extraction. Experimental study in rats. Int J Oral Maxillofac Surg 17:388–391
Ozawa Y, Shimizu N, Kariya G, Abiko Y (1998) Low energy laser irradiation stimulates bone nodule formation of early stage of cell culture in rat calvarial cells—a transmission electron microscopic study. Bone 22:347–354
Kreisler M, Kohnen W, Beck M, Al Haj H, Christoffers AB, Gotz H, Duschner H (2003) Efficacy of NaOCl/H2O2 irrigation and GaAlAs laser in decontamination of root canals in vitro. Lasers Surg Med 32:189–196
Lekovic V, Camargo PM, Weinlaender M, Vasilic N, Kenny EB (2003) Effectiveness of a combination of platelet-rich plasma, bovine porous bone mineral and guided tissue regeneration in the treatment of mandibular grade II molar furcations in humans. J Clin Periodont 30:746–751
Cortenllini P, Pini-Prato G, Tonetti MS (1996) Periodontal regeneration of human infrabony defects with bioresorbable membranes. A controlled clinical trial. J Periodontol 67:217–223
Hanna R, Trejo PM, Weltman PM (2004) Treatment of infrabony defects with bovine-derived xenograft alone and in combination with platelet-rich plasma: a randomized clinical trial. J Periodontol 75:1668–1677
Cortellini P, Pini-Prato G, Tonetti MS (1995) Periodontal regeneration of human infrabony defects with titanium reinforced membranes. A controlled clinical trial. J Periodontol 66:797–803
Laurell L, Gottolow J, Zybutz M, Persson R (1998) Treatment of infrabony defects by different surgical procedures. A literature review. J Periodontol 69:303–313
Zamet JS, Darbar UR, Griffiths GS (1997) Particulate bioglass as a grafting material in the treatment of periodontal infrabony defects. J Clin Periodont 24:410–418
Froum SJ, Weinberg MA, Tarnow D (1998) Comparison of bioactive glass synthetic bone graft particles and open debridement in the treatment of human periodontal defects. J Periodontol 69:698–709
Mengel R, Soffner M, Jacoby FL (2003) Bioabsorbable membrane and bioactive glass in the treatment of intrabony defects in patients with generalized aggressive periodontitis: results of a 12-month clinical and radiological study. J Periodontol 74:899–908
Anderegg CR, Alaxander DC, Friedman MA (1999) Bioactive glass particulate in the treatment of molar furcation invasions. J Periodontol 70:384–387
Low SB, King CJ, Krieger J (1997) An evaluation of bioactive ceramic in the treatment of periodontal osseous defects. Int J Periodont Rest Dent 17:358–367
Lovelace TB, Mellonig JT, Meffert RM, Jones AA, Cochran DL (1998) Clinical evaluation of bioactive glass in the treatment of periodontal osseous defects in humans. J Periodontol 69:1027–1035
Nevins ML, Camelo M, Nevins M, King CJ, Oringer RJ, Schenk RK, Fiorellini JP (2000) Human histologic evaluation of bioactive ceramic in the treatment of periodontal osseous defects. Int J Periodont Rest Dent 20:458–467
Ong MM, Eber RM, Korsnes ML (1998) Evaluation of a bioactive glass alloplast in treating periodontal intrabony defects. J Periodontol 69:1346–1354
Dybvik T, Leknes KN, Boe OE, Skavland RJ, Albandar JM (2007) Bioactive ceramic filler in the treatment of severe osseous defects: 12-month results. J Periodontol 78:403–410
Maegawa Y, Itoh T, Hosokawa T, Nishi M, Yaegashi K (2000) Effects of near infrared low-level laser irradiation on microcirculation. Lasers Surg Med 27:427–437
Lopes CB, Pinheriro ALB, Sathaiah S, Durate J, Martins MC (2005) Infrared laser light reduces loading time of dental implants: a Raman spectroscopic study. Photomed Laser Surg 23:27–31
Acknowledgements
The authors wish to acknowledge funding received for this study from the Egyptian Government for a Channel Link PhD Programme. The authors would also like to thank the Department of Radiology at King’s College Dental Hospital for its assistance with this project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
AboElsaad, N.S., Soory, M., Gadalla, L.M.A. et al. Effect of soft laser and bioactive glass on bone regeneration in the treatment of infra-bony defects (a clinical study). Lasers Med Sci 24, 387–395 (2009). https://doi.org/10.1007/s10103-008-0576-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-008-0576-9