Abstract
Objectives
To evaluate the relationship between gingival biotypes and gingival thickness based on probe transparency through the gingival margin and to assess the sensitivity of a novel classification method.
Material and methods
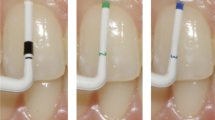
Sixty adult Caucasian subjects were stratified by their gingival biotype (GB) as defined by the transparency of a prototype double-ended periodontal probe through the buccal gingival margin into “thin” (30 subjects), “moderate” (15 subjects), and “thick” (15 subjects) GB. Three additional parameters were also assessed: gingival thickness (GT), probing depth (PD), and gingival width (GW).
Results
Median GT was 0.43 mm (P 25% 0.32; P 75% 0.58) for thin, 0.74 mm (P 25% 0.58; P 75% 0.81) for moderate, and 0.83 mm (P 25% 0.74; P 75% 0.95) for thick GB, respectively. GT was statistically significant different for thin versus moderate and thin versus thick, respectively (Kruskal-Wallis test, p < 0.05; Dunn’s test, thin versus moderate: p = 0.002; thin versus thick: p < 0.001; moderate versus thick: p = 0.089). GW was directly correlated with GT (Spearman correlation p < 0.01). The sensitivity of the new classification tool for diagnosing a thin GB was 91.3%. No adverse events or complications were reported.
Conclusion
GT differs significantly between the presented GB groups, hence, an alternative classification especially focusing on thin biotypes based on a modified periodontal probe might be advantageous. In addition, the presence of a thick gingiva is associated with a wide band of keratinized tissue.
Clinical relevance
This clinical setting might to be useful to identify high-risk patients with a very thin biotype and, consequently, higher risk for gingival recession after dental treatments.



Similar content being viewed by others
References
Fu JH, Lee A, Wang HL (2011) Influence of tissue biotype on implant esthetics. Int J Oral Maxillofac Implants 26:499–508
Cosyn J, Eghbali A, De Bruyn H, Collys K, Cleymaet R, De Rouck T (2011) Immediate single-tooth implants in the anterior maxilla: 3-year results of a case series on hard and soft tissue response and aesthetics. J Clin Periodontol 38:746–753. doi:10.1111/j.1600-051X.2011.01748.x
Kan JY, Rungcharassaeng K, Umezu K, Kois JC (2003) Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol 74:557–562. doi:10.1902/jop.2003.74.4.557
Nisapakultorn K, Suphanantachat S, Silkosessak O, Rattanamongkolgul S (2010) Factors affecting soft tissue level around anterior maxillary single-tooth implants. Clin Oral Implants Res 21:662–670. doi:10.1111/j.1600-0501.2009.01887.x
Chen ST, Buser D (2014) Esthetic outcomes following immediate and early implant placement in the anterior maxilla—a systematic review. Int J Oral Maxillofac Implants 29(Suppl):186–215. doi:10.11607/jomi.2014suppl.g3.3
Cosyn J, Hooghe N, De Bruyn H (2012) A systematic review on the frequency of advanced recession following single immediate implant treatment. J Clin Periodontol 39:582–589. doi:10.1111/j.1600-051X.2012.01888.x
Sailer I, Zembic A, Jung RE, Hammerle CH, Mattiola A (2007) Single-tooth implant reconstructions: esthetic factors influencing the decision between titanium and zirconia abutments in anterior regions. Eur J Esthet Dent 2:296–310
Jung RE, Sailer I, Hammerle CH, Attin T, Schmidlin P (2007) In vitro color changes of soft tissues caused by restorative materials. Int J Periodontics Restorative Dent 27:251–257
Linkevicius T, Apse P, Grybauskas S, Puisys A (2009) The influence of soft tissue thickness on crestal bone changes around implants: a 1-year prospective controlled clinical trial. Int J Oral Maxillofac Implants 24:712–719
Linkevicius T, Apse P, Grybauskas S, Puisys A (2010) Influence of thin mucosal tissues on crestal bone stability around implants with platform switching: a 1-year pilot study. Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial Surgeons 68:2272–2277. doi:10.1016/j.joms.2009.08.018
Eghbali A, De Rouck T, De Bruyn H, Cosyn J (2009) The gingival biotype assessed by experienced and inexperienced clinicians. J Clin Periodontol 36:958–963. doi:10.1111/j.1600-051X.2009.01479.x
Fischer KR, Grill E, Jockel-Schneider Y, Bechtold M, Schlagenhauf U, Fickl S (2013) On the relationship between gingival biotypes and supracrestal gingival height, crown form and papilla height. Clin Oral Implants Res. doi:10.1111/clr.12196
Fischer KR, Richter T, Friedmann A, Fickl S (2016) On the relationship between gingival morphotypes and different crown shape assessments in young Caucasians. Clinical oral investigations. doi:10.1007/s00784-016-1720-8
Fischer KR, Richter T, Kebschull M, Petersen N, Fickl S (2014) On the relationship between gingival biotypes and gingival thickness in young Caucasians. Clin Oral Implants Res. doi:10.1111/clr.12356
De Rouck T, Eghbali R, Collys K, De Bruyn H, Cosyn J (2009) The gingival biotype revisited: transparency of the periodontal probe through the gingival margin as a method to discriminate thin from thick gingiva. J Clin Periodontol 36:428–433. doi:10.1111/j.1600-051X.2009.01398.x
Olsson M, Lindhe J, Marinello CP (1993) On the relationship between crown form and clinical features of the gingiva in adolescents. J Clin Periodontol 20:570–577
Kan JY, Morimoto T, Rungcharassaeng K, Roe P, Smith DH (2010) Gingival biotype assessment in the esthetic zone: visual versus direct measurement. Int J Periodontics Restorative Dent 30:237–243
Ross SB, Pette GA, Parker WB, Hardigan P (2014) Gingival margin changes in maxillary anterior sites after single immediate implant placement and provisionalization: a 5-year retrospective study of 47 patients. Int J Oral Maxillofac Implants 29:127–134. doi:10.11607/jomi.3124
Kan JY, Rungcharassaeng K, Lozada JL, Zimmerman G (2011) Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. Int J Oral Maxillofac Implants 26:179–187
Dawson A, Chen S, Buser D, Cordaro L, Martin W, Belser U (2009) The SAC classification in implant dentistry. Quintessenz Publishing Co. Ltd., London
Rungcharassaeng K, Kan JY, Yoshino S, Morimoto T, Zimmerman G (2012) Immediate implant placement and provisionalization with and without a connective tissue graft: an analysis of facial gingival tissue thickness. Int J Periodontics Restorative Dent 32:657–663
Cosyn J, Eghbali A, Hermans A, Vervaeke S, De Bruyn H, Cleymaet R (2016) A 5-year prospective study on single immediate implants in the aesthetic zone. J Clin Periodontol 43:702–709. doi:10.1111/jcpe.12571
Rasperini G, Acunzo R, Cannalire P, Farronato G (2015) Influence of periodontal biotype on root surface exposure during orthodontic treatment: a preliminary study. Int J Periodontics Restorative Dent 35:665–675. doi:10.11607/prd.2239
Pontoriero R, Carnevale G (2001) Surgical crown lengthening: a 12-month clinical wound healing study. J Periodontol 72:841–848. doi:10.1902/jop.2001.72.7.841
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This study was solely funded by the authors’ institutions.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study protocol and consent form was approved by the Ethical Committee of the Medical Faculty, Witten/Herdecke University (34/2015).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Fischer, K.R., Künzlberger, A., Donos, N. et al. Gingival biotype revisited—novel classification and assessment tool. Clin Oral Invest 22, 443–448 (2018). https://doi.org/10.1007/s00784-017-2131-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2131-1