Abstract
Aims
The hyperglycemia and adverse pregnancy outcome study demonstrated a continuous association between fasting plasma glucose (FPG) levels below those diagnostic of diabetes and adverse neonatal outcomes. We aimed to investigate whether the same association was found in a Mediterranean population.
Methods
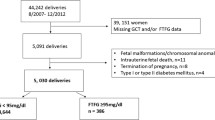
A retrospective analysis of singleton pregnancies attended at our Hospital between 2008 and 2015 (n = 5203). FPG was evaluated in the second trimester, and it was divided into 7 categories (1 < 75, 2 75–79, 3 80–84, 4 85–89, 5 90–94, 6 95–99 and 7 100–124 mg/dL). Pregnancy outcomes included elective cesarean delivery, gestational hypertensive disorders (GHD), large for gestational age (LGA), small for gestational age (SGA), macrosomia, prematurity, severe prematurity and APGAR at 1 min <7.
Results
Maternal age was 33.8 ± 3.8 years, and BMI at first antenatal visit was 22.9 ± 3.5 kg/m2; mean FPG was 79 ± 7 mg/dL. A positive association was observed between FPG and LGA (p < 0.001), GHD (p = 0.004) and prematurity both <37 and <34 weeks of gestation (p = 0.001 and p = 0.004). FPG and SGA were inversely related (p = 0,038). FPG was not significantly related to rate of C-section or APGAR. Adjusted odds ratios associated with 1 standard deviation increase in the fasting plasma glucose (7 mg/dL) were 1.26 (1.15 to 1.37) for LGA, 1.28 (1.09 to 1.49) for GHD and 0.83 (0.74–0.93) for SGA. In a multivariate analysis controlling for confounders, FPG remained associated with LGA.
Conclusions
We found an association between FPG levels, below those diagnostic of gestational diabetes according to our guidelines, and adverse maternal and neonatal outcomes in a Mediterranean population.

Similar content being viewed by others
References
Metzger BE, Lowe LP, Dyer AR et al (2008) Hyperglycemia and adverse pregnancy outcomes. N Engl J Med 358:1991–2002
Metzger BE, Gabbe SG, Persson B et al (2010) International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care 33:676–682
Professional Practice Committee for the Standards of Medical Care in Diabetes—2016 (2015). Diabetes Care 39:S107–S108
Vandorsten JP, Dodson WC, Espeland MA et al (2013) NIH consensus development conference: diagnosing gestational diabetes mellitus. NIH Consens State Sci Statements 29:1–31
Practice Bulletin No. 137 (2013) Gestational diabetes mellitus. Obstet Gynecol 122:406–416
National Institute for Health and Care Excellence (NICE) (2016) Diabetes in pregnancy: management of diabetes and its complications from preconception to the postnatal period. Clinical guideline NG3 2015. www.nice.org.uk/guidance/ng3/resources/diabetes-in-pregnancy-management-of-diabetes-and-its-complications-from-preconception-to-the-postnatal-period-51038446021. Accessed 26 Feb 2016
Corcoy R, Lumbreras B, Bartha JL, Ricart W (2010) New diagnostic criteria for gestational diabetes mellitus after the HAPO study are they valid in our environment? Endocrinol y Nutr 57:277–280
Spanish Group of Diabetes and Pregnancy (GEDE) (2015) Care of pregnancies complicated by diabetes. Clinical practice guidelines: 2014 update. Av Diabetol 31:45–59
Buckley BS, Harreiter J, Damm P et al (2012) Gestational diabetes mellitus in Europe: prevalence, current screening practice and barriers to screening. Diabet Med 29:844–854
Metzger BE, Coustan (1998) Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes Care 21:161–167
World Health Organisation (2013) Diagnostic criteria and classification of hyperglycaemia first detected in pregnancy. http://apps.who.int/iris/bitstream/10665/85975/1/WHO_NMH_MND_13.2_eng.pdf. Accessed 12 Mar 2016
Crowther CA, Hiller JE, Moss JR, McPhee AJ, Jeffries WS, Robinson JS (2005) Effect of treatment of gestational diabetes mellitus on pregnancy outcomes. N Engl J Med 352:2477–2486
Landon MB, Thom E, Spong CY et al (2007) The National Institute of Child Health and Human Development Maternal-Fetal Medicine Unit Network randomized clinical trial in progress: standard therapy versus no therapy for mild gestational diabetes. Diabetes Care 30(Suppl 2):S194–S199
Hartling L, Dryden DM, Guthrie A, Muise M, Vandermeer B, Donovan L (2013) Benefits and harms of treating gestational diabetes mellitus: a systematic review and meta-analysis for the U.S. Preventive Services Task Force and the National Institutes of Health Office of Medical Applications of Research. Ann Intern Med 159:123–129
Rubio JA, Ontañón M, Perea V, Megia A (2016) Asistencia sanitaria de la mujer gestante con diabetes en España: aproximación usando un cuestionario. Endocrinol y Nutr 63:113–120
Duran A, Sáenz S, Torrejón MJ et al (2014) Introduction of IADPSG criteria for the screening and diagnosis of gestational diabetes mellitus results in improved pregnancy outcomes at a lower cost in a large cohort of pregnant women: the St. Carlos Gestational Diabetes Study. Diabetes Care 37:2442–2450
Sacks DA, Hadden DR, Maresh M et al (2012) Frequency of gestational diabetes mellitus at collaborating centers based on IADPSG consensus panel-recommended criteria: the hyperglycemia and adverse pregnancy outcome (HAPO) Study. Diabetes Care 35:526–528
Hillier TA, Pedula KL, Vesco KK et al (2008) Excess gestational weight gain: modifying fetal macrosomia risk associated with maternal glucose. Obstet Gynecol 112:1007–1014
Ferraro ZM, Barrowman N, Prud’homme D et al (2012) Excessive gestational weight gain predicts large for gestational age neonates independent of maternal body mass index. J Matern Neonatal Med 25:538–542
Murphy DJ, Fahey T (2013) A retrospective cohort study of mode of delivery among public and private patients in an integrated maternity hospital setting. BMJ Open 3:e003865
Escuriet-Peiró R, Goberna-Tricas J, Pueyo-Sanchez MJ et al (2015) Impact of maternity care policy in Catalonia: a retrospective cross-sectional study of service delivery in public and private hospitals. BMC Pregnancy Childbirth 15:23
Mikesh LM, Bruns DE (2008) Stabilization of glucose in blood specimens: mechanism of delay in fluoride inhibition of glycolysis. Clin Chem 54:930–932
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant conflict of interest to disclose.
Ethical standard
The protocol was approved by the Hospital Ethical Committee.
Human and animal rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Declaration of Helsinki 1975, as revised in 2008 (5).
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Managed by Massimo Federici.
Rights and permissions
About this article
Cite this article
Sesmilo, G., Meler, E., Perea, V. et al. Maternal fasting glycemia and adverse pregnancy outcomes in a Mediterranean population. Acta Diabetol 54, 293–299 (2017). https://doi.org/10.1007/s00592-016-0952-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-016-0952-z