Abstract
Introduction
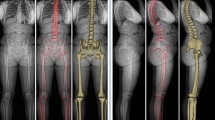
Sagittal balance of the coxofemoral joint in standing position and its extension capacity determine hip/spine adaptation, especially in relation to pelvic retroversion, which may be age-associated or follow either spinal arthrodesis or vertebral osteotomies. The concept of extension reserve is essential for assessing posterior hip im**ement. The global visualization of the lumbar–pelvic–femoral complex obtained by EOS® imaging enables this sagittal analysis of both the subpelvic region and lumbar spine by combining the reference standing position and the possibility of dynamic tests.
Materials and methods
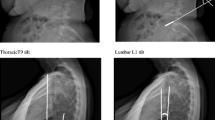
We studied 46 patients and their 92 hips. The EOS® radiography was performed in neutral standing position and with one foot on a step, alternately the right and left feet. Pelvic incidence, sacral slope, pelvic version, and femoral version were measured twice by two operators. The global extension reserve (GER) was defined by the sum of the intrinsic extension reserve (allowed by the hips, IER) and the extrinsic extension reserve (allowed by the spine, EER). The IER for each hip corresponds to the difference in the sacrofemoral angle (SFA) for each of the two positions. The EER was measured by the difference in the sacral slope. A descriptive study was performed, together with studies of inter- and intra-observer reproducibility, right/left symmetry, and an analysis according to age, sex, and BMI.
Results
The mean femoral version in the reference position was 11.7° (SD 14.3°). The reproducibility of the SFA measurement was statistically verified. The IER (mean 8.8°), EER (mean −0.7°), and GER (mean 8.2°) all differed significantly between the two sides for each patient and were not associated with age, sex, or BMI.
Discussion
The femoral axis is not perpendicular to the ground in neutral position, contrary to the conventional view of this position. The measurements proposed for dynamic sagittal analysis of the hip are reproducible and make it possible to identify the IER within the GER of the spinal–pelvic–femoral complex.
Conclusion
The assessment of the lumbar–pelvic–femoral complex by EOS imaging makes it possible to define the intrinsic and extrinsec extension reserves to describe the reciprocal adaptive capacities of the hips and spine.
Level of evidence
IV.





Similar content being viewed by others
References
Roussouly P, Pinheiro-Franco JL (2011) Biomechanical analysis of the spino-pelvic organization and adaptation in pathology. Eur Spine J 20(Suppl 5):609–618
Le Huec JC, Leijssen P, Duarte M, Aunoble S (2011) Thoracolumbar imbalance analysis for osteotomy planification using a new method: FBI technique. Eur Spine J 20(Suppl 5):669–680
Lazennec JY, Saillant G, Saidi K, Arafati N, Barabas D, Benazet JP, Laville C, Roy-Camille R, Ramare S (1997) Surgery of the deformities in ankylosing spondylitis: our experience of lumbar osteotomies in 31 patients. Eur Spine J 6:222–232
Lazennec JY, Charlot N, Gorin M, Roger B, Arafati N, Bissery A, Saillant G (2004) Hip–spine relationship: a radio-anatomical study for optimization in acetabular cup positioning. Surg Radiol Anat 26:136–144
Legaye J (2009) Influence of the sagittal balance of the spine on the anterior pelvic plane and on the acetabular orientation. Int Orthop 33:1695–1700
Rousseau MA, Lazennec JY, Boyer P, Mora N, Gorin M, Catonne Y (2009) Optimization of total hip arthroplasty implantation: is the anterior pelvic plane concept valid? J Arthroplasty 24:22–26
Laffargue P, Pinoit Y, Tabutin J, Giraud F, Puget J, Migaud H (2006) Computer-assisted positioning of the acetabular cup for total hip arthroplasty based on joint kinematics without prior imaging: preliminary results with computed tomographic assessment. Rev Chir Orthop Reparatrice Appar Mot 92:316–325
Lazennec JY, Brusson A, Rousseau MA (2013) Lumbar–pelvic–femoral balance on sitting and standing lateral radiographs. Orthop Traumatol Surg Res 99:S87–S103
Lazennec JY, Brusson A, Rousseau MA (2012) THA patients in standing and sitting positions: a prospective evaluation using the low-Dose “Full-Body” EOS® imaging system. Semin Arthroplasty 23:220–225
Barrey C, Roussouly P, Le Huec JC, D’Acunzi G, Perrin G (2013) Compensatory mechanisms contributing to keep the sagittal balance of the spine. Eur Spine J 22(Suppl 6):S834–S841
Lazennec JY, Brusson A, Rousseau MA (2011) Hip–spine relations and sagittal balance clinical consequences. Eur Spine J 20(Suppl 5):686–698
Lazennec JY, Riwan A, Gravez F, Rousseau MA, Mora N, Gorin M, Lasne A, Catonne Y, Saillant G (2007) Hip spine relationships: application to total hip arthroplasty. Hip Int 17(Suppl 5):S91–S104
Morvan G, Mathieu P, Vuillemin V, Guerini H, Bossard P, Zeitoun F, Wybier M (2011) Standardized way for imaging of the sagittal spinal balance. Eur Spine J 20(Suppl 5):602–608
Mangione P, Senegas J (1997) Sagittal balance of the spine. Rev Chir Orthop Reparatrice Appar Mot 83:22–32
Hovorka I, Rousseau P, Bronsard N, Chalali M, Julia M, Carles M, Amoretti N, Boileau P (2008) Extension reserve of the hip in relation to the spine: comparative study of two radiographic methods. Rev Chir Orthop Reparatrice Appar Mot 94:771–776
Dubousset J, Charpak G, Skalli W, Kalifa G, Lazennec JY (2007) EOS stereo-radiography system: whole-body simultaneous anteroposterior and lateral radiographs with very low radiation dose. Rev Chir Orthop Reparatrice Appar Mot 93:141–143
Marks M, Stanford C, Newton P (2009) Which lateral radiographic positioning technique provides the most reliable and functional representation of a patient’s sagittal balance? Spine (Phila Pa 1976) 34:949–954
Legaye J, Duval-Beaupere G (2005) Sagittal plane alignment of the spine and gravity: a radiological and clinical evaluation. Acta Orthop Belg 71:213–220
NF-ISO-5725-2 (1994) Application de la statistique - Exactitude (justesse et fidélité) des résultats et méthodes de mesure - Partie 2 : méthodes de base pour la détermination de la répétabilité et de la reproductibilité d'une méthode de mesure normalisée. Application des méthodes statistiques.
Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86:420–428
Offierski CM, MacNab I (1983) Hip–spine syndrome. Spine (Phila Pa 1976) 8:316–321
Dujardin F, Selva O, Mejjad O, Pasero D, Piraux JL, Thomine JM (1995) Intra and interindividual variations of pelvic mobility in normal adult walk. Rev Chir Orthop Reparatrice Appar Mot 81:592–600
Lee LW, Zavarei K, Evans J, Lelas JJ, Riley PO, Kerrigan DC (2005) Reduced hip extension in the elderly: dynamic or postural? Arch Phys Med Rehabil 86:1851–1854
James B, Parker AW (1989) Active and passive mobility of lower limb joints in elderly men and women. Am J Phys Med Rehabil 68:162–167
Roach KE, Miles TP (1991) Normal hip and knee active range of motion: the relationship to age. Phys Ther 71:656–665
Lazennec JY, Brusson A, Rousseau MA (2012) Hip-Spine Relations: an innovative paradigm in THR Surgery. In: Samo K Fokter (ed) Recent advances in arthroplasty. InTech
Conflict of interest
The authors report no conflicts of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lazennec, J.Y., Brusson, A., Folinais, D. et al. Measuring extension of the lumbar–pelvic–femoral complex with the EOS® system. Eur J Orthop Surg Traumatol 25, 1061–1068 (2015). https://doi.org/10.1007/s00590-015-1603-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-015-1603-8