Abstract
Objective
Clinical outcomes of the stand-alone cage have been encouraging when used in anterior cervical discectomy and fusion (ACDF), but concerns remain regarding its complications, especially cage subsidence. This retrospective study was undertaken to investigate the long-term radiological and clinical outcomes of the stand-alone titanium cage and to evaluate the incidence of cage subsidence in relation to the clinical outcome in the surgical treatment of degenerative cervical disc disease.
Methods
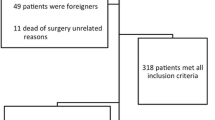
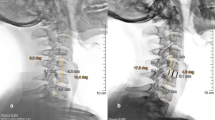
A total of 57 consecutive patients (68 levels) who underwent ACDF using a titanium box cage for the treatment of cervical radiculopathy and/or myelopathy were reviewed for the radiological and clinical outcomes. They were followed for at least 5 years. Radiographs were obtained before and after surgery, 3 months postoperatively, and at the final follow-up to determine the presence of fusion and cage subsidence. The Cobb angle of C2–C7 and the vertebral bodies adjacent to the treated disc were measured to evaluate the cervical sagittal alignment and local lordosis. The disc height was measured as well. The clinical outcomes were evaluated using the Japanese Orthopaedic Association (JOA) score for cervical myelopathy, before and after surgery, and at the final follow-up. The recovery rate of JOA score was also calculated. The Visual Analogue Scale (VAS) score of neck and radicular pain were evaluated as well. The fusion rate was 95.6% (65/68) 3 months after surgery.
Results
Successful bone fusion was achieved in all patients at the final follow-up. Cage subsidence occurred in 13 cages (19.1%) at 3-month follow-up; however, there was no relation between fusion and cage subsidence. Cervical and local lordosis improved after surgery, with the improvement preserved at the final follow-up. The preoperative disc height of both subsidence and non-subsidence patients was similar; however, postoperative posterior disc height (PDH) of subsidence group was significantly greater than of non-subsidence group. Significant improvement of the JOA score was noted immediately after surgery and at the final follow-up. There was no significant difference of the recovery rate of JOA score between subsidence and non-subsidence groups. The recovery rate of JOA score was significantly related to the improvement of the C2–C7 Cobb angle. The VAS score regarding neck and radicular pain was significantly improved after surgery and at the final follow-up. There was no significant difference of the neck and radicular pain between both subsidence and non-subsidence groups.
Conclusions
The results suggest that the clinical and radiological outcomes of the stand-alone titanium box cage for the surgical treatment of one- or two-level degenerative cervical disc disease are satisfactory. Cage subsidence does not exert significant impact upon the long-term clinical outcome although it is common for the stand-alone cages. The cervical lordosis may be more important for the long-term clinical outcome than cage subsidence



Similar content being viewed by others
References
Abd-Alrahman N, Dokmak AS, Abou-Madawi A (1999) Anterior cervical discectomy (ACD) versus anterior cervical fusion (ACF), clinical and radiological outcome study. Acta Neurochir 141:1089–1092
Barsa P, Suchomel P (2007) Factors affecting sagittal malalignment due to cage subsidence in standalone cage assisted anterior cervical fusion. Eur Spine J 16:1395–1400
Bartels RH, Donk RD, Feuth T (2006) Subsidence of stand-alone cervical carbon fiber cages. Neurosurgery 58:502–508
Cho DY, Liau WR, Lee WY, Liu JT, Chiu CL, Sheu PC (2002) Preliminary experience using a polyetheretherketone (PEEK) cage in the treatment of cervical disc disease. Neurosurgery 51:1343–1349
Dai LY, Jiang LS (2008) Anterior cervical fusion with interbody cage containing beta-tricalcium phosphate augmented with plate fixation: a prospective randomized study with 2-year follow-up. Eur Spine J 17:698–705
Demircan MN, Kutlay AM, Colak A, Kaya S, Tekin T, Kibici K, Ungoren K (2007) Multilevel cervical fusion without plates, screws or autogenous iliac crest bone graft. J Clin Neurosci 14:723–728
Ferch RD, Shad A, Cadoux-Hudson TA, Teddy PJ (2004) Anterior correction of cervical kyphotic deformity: effects on myelopathy, neck pain, and sagittal alignment. J Neurosurg 100:13–19
Fraser JF, Hartl R (2007) Anterior approaches to fusion of the cervical spine: a metaanalysis of fusion rates. J Neurosurg Spine 6:298–303
Galbusera F, Bellini CM, Costa F, Assietti R, Fornari M (2008) Anterior cervical fusion: a biomechanical comparison of 4 techniques. Laboratory investigation. J Neurosurg Spine 9:444–449
Gercek E, Arlet V, Delisle J, Marchesi D (2003) Subsidence of stand-alone cervical cages in anterior interbody fusion: warning. Eur Spine J 12:513–516
Hacker RJ, Cauthen JC, Gilbert TJ, Griffith SL (2000) A prospective randomized multicenter clinical evaluation of an anterior cervical fusion cage. Spine 25:2646–2654
Harrison DD, Harrison DE, Janik TJ, Cailliet R, Ferrantelli JR, Haas JW, Holland B (2004) Modeling of the sagittal cervical spine as a method to discriminate hypolordosis: results of elliptical and circular modeling in 72 asymptomatic subjects, 52 acute neck pain subjects, and 70 chronic neck pain subjects. Spine 29:2485–2492
Heidecke V, Rainov NG, Burkert W (1998) Anterior cervical fusion with the Orion locking plate system. Spine 23:1796–1802
Hida K, Iwasaki Y, Yano S, Akino M, Seki T (2008) Long-term follow-up results in patients with cervical disk disease treated by cervical anterior fusion using titanium cage implants. Neurol Med Chir 48:440–446
Hwang SL, Hwang YF, Lieu AS, Lin CL, Kuo TH, Su YF, Howng SL, Lee KS (2005) Outcome analyses of interbody titanium cage fusion used in the anterior discectomy for cervical degenerative disc disease. J Spinal Disord Tech 18:326–331
Hwang SL, Lin CL, Lieu AS, Lee KS, Kuo TH, Hwang YF, Su YF, Howng SL (2004) Three-level and four-level anterior cervical discectomies and titanium cage-augmented fusion with and without plate fixation. J Neurosurg Spine 1:160–167. doi:10.3171/spi.2004.1.2.0160
Kast E, Derakhshani S, Bothmann M, Oberle J (2009) Subsidence after anterior cervical inter-body fusion. A randomized prospective clinical trial. Neurosurg Rev 32:207–214
Katsuura A, Hukuda S, Saruhashi Y, Mori K (2001) Kyphotic malalignment after anterior cervical fusion is one of the factors promoting the degenerative process in adjacent intervertebral levels. Eur Spine J 10:320–324
Lied B, Roenning PA, Sundseth J, Helseth E (2011) Anterior cervical discectomy with fusion in patients with cervical disc degeneration: a prospective outcome study of 258 patients (181 fused with autologous bone graft and 77 fused with a PEEK cage). BMC Surg 10:10
Lowery GL, McDonough RF (1998) The significance of hardware failure in anterior cervical plate fixation: patients with 2- to 7-year follow-up. Spine 23:181–186
Samartzis D, Shen FH, Lyon C, Phillips M, Goldberg EJ, An HS (2004) Does rigid instrumentation increase the fusion rate in one-level anterior cervical discectomy and fusion? Spine J 4:636–643
Schmieder K, Wolzik-Grossmann M, Pechlivanis I, Engelhardt M, Scholz M, Harders A (2006) Subsidence of the wing titanium cage after anterior cervical interbody fusion: 2-year follow-up study. J Neurosurg Spine 4:447–453
Silber JS, Anderson DG, Daffner SD, Brislin BT, Leland JM, Hilibrand AS, Vaccaro AR, Albert TJ (2003) Donor site morbidity after anterior iliac crest bone harvest for single-level anterior cervical discectomy and fusion. Spine 28:134–139
Smith GW, Robinson RA (1958) The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Am 40:607–624
Sonntag VK, Klara P (1996) Is fusion necessary after anterior cervical discectomy? Spine 21:1111–1113
Thome C, Krauss JK, Zevgaridis D (2004) A prospective clinical comparison of rectangular titanium cages and iliac crest autografts in anterior cervical discectomy and fusion. Neurosurg Rev 27:34–41
Thorell W, Cooper J, Hellbusch L, Leibrock L (1998) The long-term clinical outcome of patients undergoing anterior cervical discectomy with and without intervertebral bone graft placement. Neurosurgery 43:268–273
Troyanovich SJ, Stroink AR, Kattner KA, Dornan WA, Gubina I (2002) Does anterior plating maintain cervical lordosis versus conventional fusion techniques? A retrospective analysis of patients receiving single-level fusions. J Spinal Disord Tech 15:69–74
Villavicencio AT, Babuska JM, Ashton A, Busch E, Roeca C, Nelson EL, Mason A, Burneikiene S (2009) Prospective, randomized, double-blind clinical study evaluating the correlation of clinical outcomes and cervical sagittal alignment. Neurosurgery 68:1309–1316
Watters WC III, Levinthal R (1994) Anterior cervical discectomy with and without fusion: results, complications, and long-term follow-up. Spine 19:2343–2347
Wigfield CC, Nelson RJ (2001) Nonautologous interbody fusion materials in cervical spine surgery: how strong is the evidence to justify their use? Spine 26:687–694
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Wu, WJ., Jiang, LS., Liang, Y. et al. Cage subsidence does not, but cervical lordosis improvement does affect the long-term results of anterior cervical fusion with stand-alone cage for degenerative cervical disc disease: a retrospective study. Eur Spine J 21, 1374–1382 (2012). https://doi.org/10.1007/s00586-011-2131-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-2131-9