Abstract
Background
Chronic intestinal inflammation alters host physiology and could lead to colorectal cancer (CRC). We have previously reported beneficial effects of the probiotic strain of Lactobacillus casei BL23 in different murine models of intestinal inflammation. In addition, there is an emerging interest on the potential beneficial effects of probiotics to treat CRC. We thus explored whether L. casei BL23 displays protective effects on CRC.
Methods
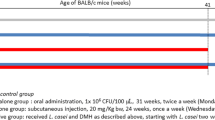
Mice were subcutaneously injected with 1,2-dimethylhydrazine (DMH) weekly during 10 weeks and orally administered with L. casei BL23 in the drinking water until the 10th week. Multiple plaque lesions in the large intestine were observed macroscopically and counted and intestinal tissues were also histologically analyzed. Finally, T-cell populations and cytokine production were evaluated after co-incubation of L. casei BL23 with spleen cells from non-treated mice to determine the immuno-modulatory effects of this bacterium.
Results
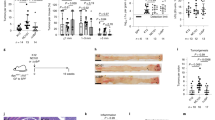
Our results show that oral treatment with this probiotic bacterium modulates host immune responses and significantly protect mice against DMH-induced CRC. This protection may be associated with the modulation of regulatory T-cells towards a Th17-biased immune response accompanied by the expression of regulatory cytokines (IL-6, IL-17, IL-10 and TGF-β), as demonstrated in L. casei BL23-treated splenocytes, but also with the colonic expression of IL-22 observed in vivo on L. casei BL23-treated mice; suggesting the induction of a fine-tune Th17-biased response.
Conclusions
Altogether our results reveal the high potential of L. casei BL23 to treat CRC and opens new frontiers for the study of immunomodulatory functions of probiotics.








Similar content being viewed by others
Change history
08 September 2020
This article has been retracted. Please see the retraction notice for more detail: https://doi.org/10.1007/s00535-015-1158-9.
References
Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin. 2013;63(1):11–30.
Viaud S, Saccheri F, Mignot G, Yamazaki T, Daillere R, Hannani D, et al. The intestinal microbiota modulates the anticancer immune effects of cyclophosphamide. Science. 2013;342(6161):971–6.
Uccello M, Malaguarnera G, Basile F, D’Agata V, Malaguarnera M, Bertino G, et al. Potential role of probiotics on colorectal cancer prevention. BMC Surg. 2012;12(Suppl 1):S35.
Kahouli I, Tomaro-Duchesneau C, Prakash S. Probiotics in colorectal cancer (CRC) with emphasis on mechanisms of action and current perspectives. J Med Microbiol. 2013;62(Pt 8):1107–23.
Joint FAO/WHO Working Group report on drafting guidelines for the evaluation of probiotics in food. London: Food and Agriculture Organization. 2002. http://www.who.int/foodsafety/fs_management/en/probiotic_guidelines.pdf. Accessed 04 Jan 2016.
Bernardeau M, Vernoux JP, Henri-Dubernet S, Gueguen M. Safety assessment of dairy microorganisms: the Lactobacillus genus. Int J Food Microbiol. 2008;126(3):278–85.
Madsen KL, Doyle JS, Jewell LD, Tavernini MM, Fedorak RN. Lactobacillus species prevents colitis in interleukin 10 gene-deficient mice. Gastroenterology. 1999;116(5):1107–14.
Khazaie K, Zadeh M, Khan MW, Bere P, Gounari F, Dennis K, et al. Abating colon cancer polyposis by Lactobacillus acidophilus deficient in lipoteichoic acid. Proc Natl Acad Sci USA. 2012;109(26):10462–7.
Kato I, Endo K, Yokokura T. Effects of oral-administration of Lactobacillus casei on antitumor responses induced by tumor resection in mice. Int J Immunopharmacol. 1994;16(1):29–36.
Aragon F, Carino S, Perdigon G, de Moreno de LeBlanc A. Inhibition of growth and metastasis of breast cancer in mice by milk fermented with Lactobacillus casei CRL 431. J Immunother. 2015;38(5):185–96.
Hu J, Wang C, Ye L, Yang W, Huang H, Meng F, et al. Anti-tumour immune effect of oral administration of Lactobacillus plantarum to CT26 tumour-bearing mice. J Biosci. 2015;40(2):269–79.
Aragon F, Carino S, Perdigon G, de Moreno de LeBlanc A. The administration of milk fermented by the probiotic Lactobacillus casei CRL 431 exerts an immunomodulatory effect against a breast tumour in a mouse model. Immunobiology. 2014;219(6):457–64.
Martin R, Miquel S, Ulmer J, Kechaou N, Langella P, Bermudez-Humaran LG. Role of commensal and probiotic bacteria in human health: a focus on inflammatory bowel disease. Microb Cell Fact. 2013;12:71.
de Moreno de LeBlanc A, LeBlanc JG. Effect of probiotic administration on the intestinal microbiota, current knowledge and potential applications. World J Gastroenterol. 2014;20(44):16518–28.
O’Mahony L, Feeney M, O’Halloran S, Murphy L, Kiely B, Fitzgibbon J, et al. Probiotic impact on microbial flora, inflammation and tumour development in IL-10 knockout mice. Aliment Pharmacol Ther. 2001;15(8):1219–25.
Lankaputhra WE, Shah NP. Antimutagenic properties of probiotic bacteria and of organic acids. Mutat Res. 1998;397(2):169–82.
Reddy BS. Prevention of colon cancer by pre- and probiotics: evidence from laboratory studies. Br J Nutr. 1998;80(4):S219–23.
Brady LJ, Gallaher DD, Busta FF. The role of probiotic cultures in the prevention of colon cancer. J Nutr. 2000;130(2S Suppl):410S–4S.
Burns AJ, Rowland IR. Anti-carcinogenicity of probiotics and prebiotics. Curr Issues intest Microbiol. 2000;1(1):13–24.
de Moreno de LeBlanc A, Perdigon G. The application of probiotic fermented milks in cancer and intestinal inflammation. Proc Nutr Soc. 2010;69(3):421–8.
Reddy BS, Rivenson A. Inhibitory effect of Bifidobacterium longum on colon, mammary, and liver carcinogenesis induced by 2-amino-3-methylimidazo[4,5-f]quinoline, a food mutagen. Cancer Res. 1993;53(17):3914–8.
Hirayama K, Rafter J. The role of probiotic bacteria in cancer prevention. Microbes Infect. 2000;2(6):681–6.
Commane D, Hughes R, Shortt C, Rowland I. The potential mechanisms involved in the anti-carcinogenic action of probiotics. Mutat Res. 2005;591(1–2):276–89.
Rochat T, Bermudez-Humaran L, Gratadoux JJ, Fourage C, Hoebler C, Corthier G, et al. Anti-inflammatory effects of Lactobacillus casei BL23 producing or not a manganese-dependant catalase on DSS-induced colitis in mice. Microb Cell Fact. 2007;6:22.
de Moreno de LeBlanc A, LeBlanc JG, Perdigon G, Miyoshi A, Langella P, Azevedo V, et al. Oral administration of a catalase-producing Lactococcus lactis can prevent a chemically induced colon cancer in mice. J Med Microbiol. 2008;57(1):100–5.
Ribelles P, Benbouziane B, Langella P, Suarez JE, Bermudez-Humaran LG. Protection against human papillomavirus type 16-induced tumors in mice using non-genetically modified lactic acid bacteria displaying E7 antigen at its surface. Appl Microbiol Biotechnol. 2013;97(3):1231–9.
Maze A, Boel G, Zuniga M, Bourand A, Loux V, Yebra MJ, et al. Complete genome sequence of the probiotic Lactobacillus casei strain BL23. J Bacteriol. 2010;192(10):2647–8.
Gasson MJ. Plasmid complements of Streptococcus lactis NCDO 712 and other lactic streptococci after protoplast-induced curing. J Bacteriol. 1983;154(1):1–9.
Bermudez-Humaran LG, Cortes-Perez NG, Lefevre F, Guimaraes V, Rabot S, Alcocer-Gonzalez JM, et al. A novel mucosal vaccine based on live Lactococci expressing E7 antigen and IL-12 induces systemic and mucosal immune responses and protects mice against human papillomavirus type 16-induced tumors. J Immunol. 2005;175(11):7297–302.
Lin KY, Guarnieri FG, StaveleyOCarroll KF, Levitsky HI, August JT, Pardoll DM, et al. Treatment of established tumors with a novel vaccine that enhances major histocompatibility class II presentation of tumor antigen. Cancer Res. 1996;56(1):21–6.
Santiago C, Pagan B, Isidro AA, Appleyard CB. Prolonged chronic inflammation progresses to dysplasia in a novel rat model of colitis-associated colon cancer. Cancer Res. 2007;67(22):10766–73.
Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976;72:248–54.
Mason KM, Bigley NJ, Fink PS. Development of a novel in vitro co-culture system for studying host response to native bacterial antigens. J Immunol Methods. 1998;211(1–2):147–58.
Hazebrouck S, Przybylski-Nicaise L, Ah-Leung S, Adel-Patient K, Corthier G, Langella P, et al. Influence of the route of administration on immunomodulatory properties of bovine beta-lactoglobulin-producing Lactobacillus casei. Vaccine. 2009;27(42):5800–5.
Yang M, Yang C, Mine Y. Multiple T cell epitope peptides suppress allergic responses in an egg allergy mouse model by the elicitation of forkhead box transcription factor 3- and transforming growth factor-beta-associated mechanisms. Clin Exp Allergy. 2010;40(4):668–78.
Cha HR, Chang SY, Chang JH, Kim JO, Yang JY, Kim CH, et al. Downregulation of Th17 cells in the small intestine by disruption of gut flora in the absence of retinoic acid. J Immunol. 2010;184(12):6799–806.
Cardoso CR, Provinciatto PR, Godoi DF, Ferreira BR, Teixeira G, Rossi MA, et al. IL-4 regulates susceptibility to intestinal inflammation in murine food allergy. Am J Physiol Gastrointest Liver Physiol. 2009;296(3):G593–600.
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2−ΔΔCT method. Methods. 2001;25(4):402–8.
De Simone V, Franze E, Ronchetti G, Colantoni A, Fantini MC, Di Fusco D, et al. Th17-type cytokines, IL-6 and TNF-alpha synergistically activate STAT3 and NF-kB to promote colorectal cancer cell growth. Oncog. 2015;34(27):3493–503.
Murugaiyan G, Saha B. Protumor vs antitumor functions of IL-17. J Immunol. 2009;183(7):4169–75.
Gounaris E, Blatner NR, Dennis K, Magnusson F, Gurish MF, Strom TB, et al. T-regulatory cells shift from a protective anti-inflammatory to a cancer-promoting proinflammatory phenotype in polyposis. Cancer Res. 2009;69(13):5490–7.
Tosolini M, Kirilovsky A, Mlecnik B, Fredriksen T, Mauger S, Bindea G, et al. Clinical impact of different classes of infiltrating T cytotoxic and helper cells (Th1, th2, treg, th17) in patients with colorectal cancer. Cancer Res. 2011;71(4):1263–71.
Liu Y, Wang L, Predina J, Han R, Beier UH, Wang LC, et al. Inhibition of p300 impairs Foxp3(+) T regulatory cell function and promotes antitumor immunity. Nat Med. 2013;19(9):1173–7.
Lee YK, Mukasa R, Hatton RD, Weaver CT. Developmental plasticity of Th17 and Treg cells. Curr Opin Immunol. 2009;21(3):274–80.
Ohnmacht C, Park JH, Cording S, Wing JB, Atarashi K, Obata Y, et al. The microbiota regulates type 2 immunity through RORγt+ T cells. Science. 2015;349(6251):989–93.
Sawa S, Lochner M, Satoh-Takayama N, Dulauroy S, Berard M, Kleinschek M, et al. RORgammat+ innate lymphoid cells regulate intestinal homeostasis by integrating negative signals from the symbiotic microbiota. Nat Immunol. 2011;12(4):320–6.
Acknowledgments
Marion Lenoir was a recipient of an ABIES Grant. Diego Muñoz-Provencio was the recipient of a fellowship from the “Fundación Alfonso Martín Escudero, Spain”. Daniel Lozano-Ojalvo acknowledges his FPU Grant (MECD) and financial support through AGL2014-59771R project. This work was partially funded by ECOS-Sud Program (Action No. A11S02).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Marion Lenoir, Silvina del Carmen and Alejandra de Moreno de LeBlanc have contributed equally to this work.
About this article
Cite this article
Lenoir, M., del Carmen, S., Cortes-Perez, N.G. et al. RETRACTED ARTICLE: Lactobacillus casei BL23 regulates Treg and Th17 T-cell populations and reduces DMH-associated colorectal cancer. J Gastroenterol 51, 862–873 (2016). https://doi.org/10.1007/s00535-015-1158-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-015-1158-9