Abstract
Background
To evaluate the management and outcomes of blunt pancreatic injuries based on the integrity of the major pancreatic duct (MPD).
Methods
Between August 1996 and August 2015, 35 patients with blunt pancreatic injuries underwent endoscopic retrograde pancreatography (ERP). Medical charts were retrospectively reviewed for demography, ERP timing, imaging findings, management, and outcome.
Results
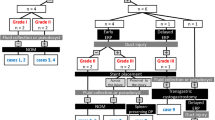
Of the 35 patients, 21 were men and 14 were women, with ages ranging from 11 to 70 years. On the basis of the ERP findings, we propose a MPD injury classification as follows: class 1 indicates normal MPD; class 2, partial injury with intact MPD continuity; and class 3, complete injury with disrupted MPD continuity. Both classes 2 and 3 are subdivided into classes a, b, and c, which represent the pancreatic tail, body, and head, respectively. In this report, 14 cases belonged to class 1, 10 belonged to class 2, and 11 belonged to class 3. Of the 14 patients with class 1 injuries, 10 underwent nonsurgical treatment and 4 underwent pancreatic duct stenting. Of the 10 patients with class 2 injuries, 4 underwent nonsurgical treatment and 6 underwent pancreatic duct stenting. Two of the 11 patients with class 3 injuries underwent pancreatic duct stenting; one in the acute stage developed sepsis that led to death even after converting to distal pancreatectomy plus splenectomy. Of the 11 patients with class 3 injuries, spleen-preserving distal pancreatectomy was performed in 6, distal pancreatectomy plus splenectomy in 2, and Roux-en-Y pancreaticojejunostomy after central pancreatectomy in 2. The overall pancreatic-related morbidity rate was 60% and the mortality rate was 2.8%.
Conclusion
Based on our experience, class 1 and 2 injuries could be treated by nonsurgical means and pancreatic duct stenting could be an adjunctive therapy in class 2b and 2c injuries. Operation is warranted in class 3 injuries.






Similar content being viewed by others
References
Jurkovich GJ, Carrico CJ (1990) Pancreatic trauma. Surg Clin North Am 70:575–593
Lin BC, Chen RJ, Fang JF, Hsu YP, Kao YC, Kao JL (2004) Management of blunt major pancreatic injury. J Trauma 56:774–778
Moore EE, Cogbill T, Malangoni MA, Jurkovich GJ, Champion HR, Gennarelli TA, McAninch JW, Pachter HL, Shackford SR, Trafton PG (1990) Organ injury scale II: pancreas, duodenum, small bowel, colon, and rectum. J Trauma 30:1427–1429
Wisner DH, Wold RL, Frey CF (1990) Diagnosis and treatment of pancreatic injuries: an analysis of management principles. Arch Surg 125:1109–1113
Patton JH Jr, Lyden SP, Croce MA, Pritchard FE, Minard G, Kudsk KA, Fabian TC (1997) Pancreatic trauma: a simplified management guideline. J Trauma 43:234–241
Biffl WL, Moore EE, Croce M, Davis JW, Coimbra R, Karmy-Jones R, McIntyre RC Jr, Moore FA, Sperry J, Malhotra A, Feliciano D (2013) Western Trauma Association critical decisions in trauma: management of pancreatic injuries. J Trauma Acute Care Surg 75:941–946
Wong YC, Wang LJ, Fang JF, Lin BC, Ng CJ, Chen RJ (2008) Multidetector-row computed tomography (CT) of blunt pancreatic injuries: can contrast-enhanced multiphasic CT detect pancreatic duct injuries? J Trauma 64:666–672
Belohlavek D, Merkle P, Probst M (1978) Identification of traumatic rupture of the pancreatic duct by endoscopic retrograde pancreatography. Gastrointest Endosc 24:255–256
Barkin JS, Ferstenburg RM, Panullo W, Manten HD, Davis RC Jr (1988) Endoscopic retrograde cholangiopancreatography in pancreatic trauma. Gastrointest Endosc 34:102–105
Bhasin DK, Rana SS, Rao C, Gupta R, Verma GR, Kang M, Nagi B, Singh K (2012) Endoscopic management of pancreatic injury due to abdominal trauma. J Pancreas 13:187–192
Takishima T, Hirata M, Kataoka Y, Asari Y, Sato K, Ohwada T, Kakita A (2000) Pancreatographic classification of pancreatic ductal injuries caused by blunt injury to the pancreas. J Trauma 48:745–752
Thomson DA, Krige JE, Thomson SR, Bornman PC (2014) The role of endoscopic retrograde pancreatography in pancreatic trauma: a critical appraisal of 48 patients treated at a tertiary institution. J Trauma Acute Care Surg 76:1362–1366
Kim HS, Lee DK, Kim IW, Baik SK, Kwon SO, Park JW, Cho NC, Rhoe BS (2001) The role of endoscopic retrograde pancreatography in the treatment of traumatic pancreatic duct injury. Gastrointest Endosc 54:49–55
Whittwell AE, Gomez GA, Byers P, Kreis DJ Jr, Manten H, Casillas VJ (1989) Blunt pancreatic trauma: prospective evaluation of early endoscopic retrograde pancreatography. South Med 82:586–591
Delcenserie R, Barthet MA, Yzet T, Grimaud JC, Dupas JL (2001) Endoscopic retrograde pancreatography in diagnosis and treatment of pancreatic trauma. Gastrointest Endosc 53:AB138
Houben CH, Ade-Ajayi N, Patel S, Kane P, Karani J, Devlin J, Harrison P, Davenport M (2007) Traumatic pancreatic duct injury in children: minimally invasive approach to management. J Pediatr Surg 42:629–635
Wind P, Tiret E, Cunningham C, Frileux P, Cugnenc P, Parc R (1999) Contribution of endoscopic retrograde pancreatography in management of complications following distal pancreatic trauma. Am Surg 65:777–783
Wood JH, Partrick DA, Bruny JL, Sauaia A, Moulton SL (2010) Operative vs nonoperative management of blunt pancreatic trauma in children. J Pediatr Surg 45:401–406
Rogers SJ, Cello JP, Schecter WP (2010) Endoscopic retrograde cholangiography in patients with pancreatic trauma. J Trauma 68:538–544
Keil R, Drabek J, Lochmannova J, Stovicek J, Rygl M, Snajdauf J, Hlava S (2016) What is the role of endoscopic retrograde cholangiopancreatography in assessing traumatic rupture of the pancreatic in children? Scand J Gastroenterol 51:218–224
Coelho DE, Ardengh JC, Carbalo MT, de Lina-Filho ER, Baron TH, Coelho JF (2011) Clinicopathologic characteristics and endoscopic treatment of post-traumatic pancreatic pseudocysts. Pancreas 40:469–473
Cheon YK, Cho KB, Watkins JL, Mchenry L, Fogel EL, Sherman S, Lehman GA (2007) “Frequency and severity of post-ERCP pancreatitis correlated with extent of pancreatic ductal opacification. Gastrointest Endosc 65:385–393
Lin BC, Liu NJ, Fang JF, Kao YC (2006) Long-term results of endoscopic stent in the management of blunt major pancreatic duct injury. Surg Endosc 20:1551–1555
Lin BC, Fang JF, Wong YC, Liu NJ (2007) Blunt pancreatic trauma and pseudocyst: management of major pancreatic duct injury. Injury 38:588–593
Ikenberr SO, Sherman S, Hawes RH, Smith M, Lehman GA (1994) The occlusion rate of pancreatic stents. Gastrointest Endosc 40:611–613
Acknowledgements
The authors thank Miss Shu-Fang Huang for her statistical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs Being-Chuan Lin, Yon-Cheong Wong, Ray-Jade Chen, Nai-Jen Liu, Cheng-Hsien Wu, Tsann-Long Hwang, and Yu-Pao Hsu have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Lin, BC., Wong, YC., Chen, RJ. et al. Major pancreatic duct continuity is the crucial determinant in the management of blunt pancreatic injury: a pancreatographic classification. Surg Endosc 31, 4201–4210 (2017). https://doi.org/10.1007/s00464-017-5478-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5478-0