Abstract
Background
During esophagectomy, laparoscopy can be used together with thoracoscopy, but it is not known whether a combined thoracoscopic–laparoscopic procedure is associated with fewer postoperative complications than open esophagectomy, and without compromising oncological outcome.
Methods
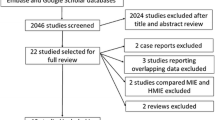
This was a longitudinal cohort study that included 185 esophageal cancer patients, including 72 who underwent combined thoracoscopic–laparoscopic esophagectomy (TLE), 34 who underwent thoracoscopic esophagectomy (TE), and 79 who underwent open esophagectomy (OE) between January 2002 and May 2010. The main outcome measures were postoperative respiratory and overall complications. The secondary outcome was 2-year relapse-free survival (RFS).
Results
Respiratory complications occurred in 9 patients who underwent TLE, 13 who underwent TE, and 31 who underwent OE. TLE was associated with fewer respiratory complications (TLE vs. OE: odds ratio [OR], 0.22; 95% confidence interval [CI], 0.09–0.53 and TE vs. OE: OR, 0.71; 95% CI 0.29–1.76). Overall complications occurred in 34 patients who underwent TLE, 20 who underwent TE, and 54 who underwent OE. TLE was associated with fewer overall complications (TLE vs. OE: OR, 0.47; 95% CI 0.23–0.94 and TE vs. OE: OR, 0.51; 95% CI 0.21–1.25). The 2-year RFS rates were similar among the three groups: 71.6% for TLE, 57.7% for TE, and 58.3% for OE (TLE vs. OE: hazard ratio, 0.65; 95% CI 0.35–1.20 and TE vs. OE: hazard ratio, 0.91; 95% CI 0.45–1.82).
Conclusion
Unlike TE, TLE was associated with fewer postoperative complications than was OE, with no compromise of 2-year RFS. A randomized controlled trial with longer follow-up is needed.


Similar content being viewed by others
Abbreviations
- ASA-PS:
-
American Society of Anesthesiologists Physical Status classification
- CI:
-
Confidence interval
- CTCAE:
-
Common Terminology Criteria for Adverse Events
- FEV1%:
-
Forced expiratory volume in 1 s as a percentage of the forced vital capacity
- MIE:
-
Minimally invasive esophagectomy
- OE:
-
Open esophagectomy
- OR:
-
Odds ratio
- RFS:
-
Relapse-free survival
- TNM:
-
Tumor Node Metastasis classification
References
Sgourakis G, Gockel I, Radtke A, Musholt TJ, Timm S, Rink A, Tsiamis A, Karaliotas C, Lang H (2010) Minimally invasive versus open esophagectomy: meta-analysis of outcomes. Dig Dis Sci 55:3031–3040
Nagpal K, Ahmed K, Vats A, Yakoub D, James D, Ashrafian H, Darzi A, Moorthy K, Athanasiou T (2010) Is minimally invasive surgery beneficial in the management of esophageal cancer? A meta-analysis. Surg Endosc 24:1621–1629
Biere SS, Cuesta MA, van der Peet DL (2009) Minimally invasive versus open esophagectomy for cancer: a systematic review and meta-analysis. Minerva Chir 64:121–133
Hamouda AH, Forshaw MJ, Tsigritis K, Jones GE, Noorani AS, Rohatgi A, Botha AJ (2010) Perioperative outcomes after transition from conventional to minimally invasive Ivor-Lewis esophagectomy in a specialized center. Surg Endosc 24:865–869
Pham TH, Perry KA, Dolan JP, Schipper P, Sukumar M, Sheppard BC, Hunter JG (2010) Comparison of perioperative outcomes after combined thoracoscopic-laparoscopic esophagectomy and open Ivor-Lewis esophagectomy. Am J Surg 199:594–598
Safranek PM, Cubitt J, Booth MI, Dehn TC (2010) Review of open and minimal access approaches to oesophagectomy for cancer. Br J Surg 97:1845–1853
Zingg U, McQuinn A, DiValentino D, Esterman AJ, Bessell JR, Thompson SK, Jamieson GG, Watson DI (2009) Minimally invasive versus open esophagectomy for patients with esophageal cancer. Ann Thorac Surg 87:911–919
Lee JM, Cheng JW, Lin MT, Huang PM, Chen JS, Lee YC (2011) Is there any benefit to incorporating a laparoscopic procedure into minimally invasive esophagectomy? the impact on perioperative results in patients with esophageal cancer. World J Surg 35(4):790–797
Smithers BM, Gotley DC, Martin I, Thomas JM (2007) Comparison of the outcomes between open and minimally invasive esophagectomy. Ann Surg 245:232–240
Noshiro H, Iwasaki H, Kobayashi K, Uchiyama A, Miyasaka Y, Masatsugu T, Koike K, Miyazaki K (2010) Lymphadenectomy along the left recurrent laryngeal nerve by a minimally invasive esophagectomy in the prone position for thoracic esophageal cancer. Surg Endosc 24:2965–2973
Itami A, Watanabe G, Tanaka E, Nakayama S, Fujimoto A, Kondo M, Nakau M, Okabe H, Satoh S, Sakai Y (2008) Multimedia article. Upper mediastinal lymph node dissection for esophageal cancer through a thoracoscopic approach. Surg Endosc 22:2741
Swanson SJ, Batirel HF, Bueno R, Jaklitsch MT, Lukanich JM, Allred E, Mentzer SJ, Sugarbaker DJ (2001) Transthoracic esophagectomy with radical mediastinal and abdominal lymph node dissection and cervical esophagogastrostomy for esophageal carcinoma. Ann Thorac Surg 72:1918–1924 discussion 1924-1915
Sato N, Koeda K, Ikeda K, Kimura Y, Aoki K, Iwaya T, Akiyama Y, Ishida K, Saito K, Endo S (2002) Randomized study of the benefits of preoperative corticosteroid administration on the postoperative morbidity and cytokine response in patients undergoing surgery for esophageal cancer. Ann Surg 236:184–190
Sobin LH, Wittekind C (2002) TNM classification of malignant tumours (UICC), 6th edn. Wiley-Liss, New York
Kitano S, Shiraishi N, Fujii K, Yasuda K, Inomata M, Adachi Y (2002) A randomized controlled trial comparing open vs laparoscopy-assisted distal gastrectomy for the treatment of early gastric cancer: an interim report. Surgery 131:S306–S311
Lee JH, Han HS (2005) A prospective randomized study comparing open vs laparoscopy-assisted distal gastrectomy in early gastric cancer: early results. Surg Endosc 19:168–173
Zingg U, Smithers BM, Gotley DC, Smith G, Aly A, Clough A, Esterman AJ, Jamieson GG, Watson DI (2011) Factors associated with postoperative pulmonary morbidity after esophagectomy for cancer. Ann Surg Oncol 18(5):1460–1468
Law S, Wong KH, Kwok KF, Chu KM, Wong J (2004) Predictive factors for postoperative pulmonary complications and mortality after esophagectomy for cancer. Ann Surg 240:791–800
Nagawa H, Kobori O, Muto T (1994) Prediction of pulmonary complications after transthoracic oesophagectomy. Br J Surg 81:860–862
Markar SR, Karthikesalingam A, Vyas S, Hashemi M, Winslet M (2011) Hand-sewn versus stapled oesophago-gastric anastomosis: systematic review and meta-analysis. J Gastrointest Surg 15(5):876–884
Mine S, Udagawa H, Tsutsumi K, Kinoshita Y, Ueno M, Ehara K, Haruta S (2009) Colon interposition after esophagectomy with extended lymphadenectomy for esophageal cancer. Ann Thorac Surg 88:1647–1653
Abate E, De Meester SR, Zehetner J, Oezcelik A, Ayazi S, Costales J, Banki F, Lipham JC, Hagen JA, De Meester TR (2010) Recurrence after esophagectomy for adenocarcinoma: defining optimal follow-up intervals and testing. J Am Coll Surg 210:428–435
Kunisaki C, Makino H, Takagawa R, Yamamoto N, Nagano Y, Fujii S, Kosaka T, Ono HA, Otsuka Y, Akiyama H, Ichikawa Y, Shimada H (2008) Surgical outcomes in esophageal cancer patients with tumor recurrence after curative esophagectomy. J Gastrointest Surg 12:802–810
Disclosures
Yousuke Kinjo, Noriaki Kurita, Fumiaki Nakamura, Hiroshi Okabe, Eiji Tanaka, Yoshiki Kataoka, Atsushi Itami, Yoshiharu Sakai, and Shunichi Fukuhara have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kinjo, Y., Kurita, N., Nakamura, F. et al. Effectiveness of combined thoracoscopic–laparoscopic esophagectomy: comparison of postoperative complications and midterm oncological outcomes in patients with esophageal cancer. Surg Endosc 26, 381–390 (2012). https://doi.org/10.1007/s00464-011-1883-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-1883-y